Abstract
Background
Currently used treatment algorithms were originally established based on the clinical outcomes of the initial treatment for primary hepatocellular carcinoma (HCC), and no strong evidence exists yet to suggest if these algorithms could also be applicable to patients with recurrent HCC after surgery. As such, this study sought to explore an optimal risk stratification method for cases of recurrent HCC for better clinical management.
Methods
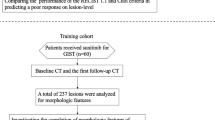
Among the 1616 patients who underwent curative resection for HCC, the clinical features and survival outcomes of 983 patients who developed recurrence were examined in detail.
Results
Multivariate analysis confirmed that both the disease-free interval (DFI) from the previous surgery and tumor stage at recurrence were significant prognostic factors. However, the prognostic impact of DFI seemed different according to the tumor stages at recurrence. While curative-intent treatment showed strong influence on survival [hazard ratio (HR), 0.61; P < 0.001] regardless of the DFI in patients with stage 0 or stage A disease at recurrence, early recurrence (< 6 months) was a poor prognostic marker in patients with stage B disease. The prognosis of patients with stage C disease was exclusively influenced by the tumor distribution or choice of treatment than by the DFI.
Conclusions
The DFI complementarily predicts the oncological behavior of recurrent HCC, with its predictive value differing depending on the tumor stage at recurrence. These factors should be considered for selection of the optimal treatment in patients with recurrent HCC after curative-intent surgery.



Similar content being viewed by others
References
Shindoh J, Kawamura Y, Kobayashi Y, et al. Time-to-interventional failure as a new surrogate measure for survival outcomes after resection of hepatocellular carcinoma. J Gastrointest Surg. 2019;24(1):50–7.
Kokudo N, Takemura N, Hasegawa K, et al. Clinical practice guidelines for hepatocellular carcinoma: the Japan Society of Hepatology 2017 (4th JSH-HCC guidelines) 2019 update. Hepatol Res. 2019;49:1109–13.
Reig M, Forner A, Rimola J, et al. BCLC strategy for prognosis prediction and treatment recommendation: the 2022 update. J Hepatol. 2022;76:681–93.
Shindoh J, Kawamura Y, Kobayashi Y, et al. Time-to-interventional failure as a new surrogate measure for survival outcomes after resection of hepatocellular carcinoma. J Gastrointest Surg. 2020;24:50–7.
Yoh T, Seo S, Taura K, et al. Surgery for recurrent hepatocellular carcinoma: achieving long-term survival. Ann Surg. 2021;273:792–9.
Liu YW, Yong CC, Lin CC, et al. Six months as a cutoff time point to define early recurrence after liver resection of hepatocellular carcinoma based on post-recurrence survival. Updates Surg. 2021;73:399–409.
Wei T, Zhang XF, Bagante F, et al. Early versus late recurrence of hepatocellular carcinoma after surgical resection based on post-recurrence survival: an international multi-institutional analysis. J Gastrointest Surg. 2021;25:125–33.
Tabrizian P, Jibara G, Shrager B, et al. Recurrence of hepatocellular cancer after resection: patterns, treatments, and prognosis. Ann Surg. 2015;261:947–55.
Lu X, Zhao H, Yang H, et al. A prospective clinical study on early recurrence of hepatocellular carcinoma after hepatectomy. J Surg Oncol. 2009;100:488–93.
Poon RT, Fan ST, Ng IO, et al. Different risk factors and prognosis for early and late intrahepatic recurrence after resection of hepatocellular carcinoma. Cancer. 2000;89:500–7.
Shah SA, Greig PD, Gallinger S, et al. Factors associated with early recurrence after resection for hepatocellular carcinoma and outcomes. J Am Coll Surg. 2006;202:275–83.
Imamura H, Matsuyama Y, Tanaka E, et al. Risk factors contributing to early and late phase intrahepatic recurrence of hepatocellular carcinoma after hepatectomy. J Hepatol. 2003;38:200–7.
Minagawa M, Makuuchi M, Takayama T, Kokudo N. Selection criteria for repeat hepatectomy in patients with recurrent hepatocellular carcinoma. Ann Surg. 2003;238:703–10.
He W, Peng B, Tang Y, et al. Nomogram to predict survival of patients with recurrence of hepatocellular carcinoma after surgery. Clin Gastroenterol Hepatol. 2018;16(756–764):e710.
Shindoh J, Kawamura Y, Kobayashi Y, et al. Platelet-albumin score as a sensitive measure for surgical risk prediction and survival outcomes of patients with hepatocellular carcinoma. J Gastrointest Surg. 2019;3:76–83.
Kudo M, Arizumi T, Ueshima K, et al. Subclassification of BCLC B stage hepatocellular carcinoma and treatment strategies: proposal of modified Bolondi’s subclassification (Kinki Criteria). Dig Dis. 2015;33:751–8.
Cucchetti A, Piscaglia F, Caturelli E, et al. Comparison of recurrence of hepatocellular carcinoma after resection in patients with cirrhosis to its occurrence in a surveilled cirrhotic population. Ann Surg Oncol. 2009;16:413–22.
Ding X, He M, Chan AWH, et al. Genomic and epigenomic features of primary and recurrent hepatocellular carcinomas. Gastroenterology. 2019;157(1630–1645):e1636.
Chan AWH, Zhong J, Berhane S, et al. Development of pre and post-operative models to predict early recurrence of hepatocellular carcinoma after surgical resection. J Hepatol. 2018;69:1284–93.
Jung SM, Kim JM, Choi GS, et al. Characteristics of early recurrence after curative liver resection for solitary hepatocellular carcinoma. J Gastrointest Surg. 2019;23:304–11.
Shinkawa H, Tanaka S, Takemura S, et al. Nomograms predicting extra- and early intrahepatic recurrence after hepatic resection of hepatocellular carcinoma. Surgery. 2021;169:922–8.
Yao LQ, Chen ZL, Feng ZH, et al. Clinical features of recurrence after hepatic resection for early-stage hepatocellular carcinoma and long-term survival outcomes of patients with recurrence: a multi-institutional analysis. Ann Surg Oncol. 2022. https://doi.org/10.1245/s10434-022-11454-y.
Mise Y, Hasegawa K, Shindoh J, et al. The feasibility of third or more repeat hepatectomy for recurrent hepatocellular carcinoma. Ann Surg. 2015;262:347–57.
Kudo M, Han KH, Ye SL, et al. A changing paradigm for the treatment of intermediate-stage hepatocellular carcinoma: Asia-Pacific primary liver cancer expert consensus statements. Liver Cancer. 2020;9:245–60.
Shindoh J, Kawamura Y, Kobayashi M, et al. Prognostic advantages of individual additional interventions after lenvatinib therapy in patients with advanced hepatocellular carcinoma. J Gastrointest Surg. 2022;26:1637–46.
Kudo M. Changing the treatment paradigm for hepatocellular carcinoma using atezolizumab plus bevacizumab combination therapy. Cancers. 2021;13:5475.
Kudo M, Izumi N, Kokudo N, et al. Report of the 21st nationwide follow-up survey of primary liver cancer in Japan (2010–2011). Hepatol Res. 2021;51:355–405.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
The authors have no conflicts of interest to disclose. This study was supported by a grant from Okinaka Memorial Institute for Medical Disease.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shindoh, J., Matsumura, M., Kobayashi, M. et al. Disease-Free Interval and Tumor Stage Complementarily Predict the Biological Behavior of Recurrent Hepatocellular Carcinoma. Ann Surg Oncol 30, 3402–3410 (2023). https://doi.org/10.1245/s10434-023-13228-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-13228-6