Opinion statement
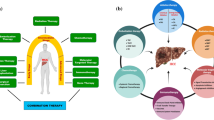
Hepatocellular carcinoma is the fourth leading cause of cancer-related deaths worldwide and its associated mortality rate is expected to rise within the next decade. The incidence rate of hepatocellular carcinoma varies significantly across countries and the latter can be attributed to the differences in risk factors that are prevalent across different countries. Some of the risk factors associated with hepatocellular carcinoma include hepatitis B and C infections, non-alcoholic fatty liver disease, and alcoholic liver disease. Regardless of the underlying aetiology, the end result is liver fibrosis and cirrhosis that ultimately progress into carcinoma. The treatment and management of hepatocellular carcinoma is complicated by treatment resistance and high tumor recurrence rates. Early stages of hepatocellular carcinoma are treated with liver resection and other forms of surgical therapy. Advanced stages of hepatocellular carcinoma can be treated with chemotherapy, immunotherapy, and the use of oncolytic viruses and these treatment options can be combined with nanotechnology to improve efficacy and reduce side effects. Moreover, chemotherapy and immunotherapy can be combined to further improve treatment efficacy and overcome resistance. Despite the treatment options available, the high mortality rates provide evidence that current treatment options for advanced-stage hepatocellular carcinoma are not achieving the desired therapeutic goals. Various clinical trials are ongoing to improve treatment efficacy, reduce recurrence rates, and ultimately prolong survival. This narrative review aims to provide an update on our current knowledge and future direction of research on hepatocellular carcinoma.

Similar content being viewed by others
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Philips CA, Rajesh S, Nair DC, Ahamed R, Abduljaleel JK, Augustine P. Hepatocellular carcinoma in 2021: an exhaustive update, Cureus. 2021. https://doi.org/10.7759/cureus.19274
Maurice J, Manousou P. Non-alcoholic fatty liver disease. Clin Med. 2018;18(3):245–50. https://doi.org/10.7861/clinmedicine.18-3-245.
Lotfollahzadeh S, Recio-Boiles A, Babiker H. Liver cancer, StatPearls Publishing, 2022. Available at: https://www.ncbi.nlm.nih.gov/books/NBK4. Accessed 20 Dec 2022
Nancy F. Primary liver cancer: surveillance, diagnosis, and treatment. 1st ed. Connecticut: Humana Press; 2012.
Kim E, Viatour P. Hepatocellular carcinoma: old friends and new tricks. Exp Mol Med. 2020;52(12):1898–907. https://doi.org/10.1038/s12276-020-00527-1.
Chidambaranathan-Reghupaty S, Fisher PB, Sarkar D. Hepatocellular carcinoma (HCC): epidemiology, etiology and molecular classification, Adv Cancer Res. 2021;1–61. doi: https://doi.org/10.1016/bs.acr.2020.10.001
Lurje I, Czigany Z, Bednarsch J, Roderburg C, Isfort P, Neumann UP, et al. Treatment strategies for hepatocellular carcinoma – a multidisciplinary approach. Int J Mol Sci. 2019;20(6):1465. https://doi.org/10.3390/ijms20061465.
Samant H, Amiri H, Zibari G. Addressing the worldwide hepatocellular carcinoma: epidemiology, prevention and management. J Gastrointest Oncol. 2021;12(S2):S361–73. https://doi.org/10.21037/jgo.2020.02.08.
Dasgupta P, Henshaw C, Youlden DR, Clark PJ, Aitken JF, and Baade PD. Global trends in incidence rates of primary adult liver cancers: a systematic review and meta-analysis. Front Oncol. 2020;10. https://doi.org/10.3389/fonc.2020.00171
• McGlynn K, Petrick J, El‐Serag H. Epidemiology of hepatocellular carcinoma. Hepatology. 2020;73(S1):4–13. https://doi.org/10.1002/hep.31288. This review demonstrated the impact of population’s demographic characteristics on the risk factors and incidence of HCC. In addition, it provided an overview on the epidemiology of HCC.
Jiang H, Chen J, Xia C, Cao L, Duan T, Song B. Non-invasive imaging of hepatocellular carcinoma: from diagnosis to prognosis. World J Gastroenterol. 2018;24(22):2348–62. https://doi.org/10.3748/wjg.v24.i22.2348.
Vogel A, Cervantes A, Chau I, Daniele B, Llovet JM, Meyer T, et al. Hepatocellular carcinoma: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2018;29:iv238–55. https://doi.org/10.1093/annonc/mdy308.
Fenton S, Burns M, Kalyan A. Epidemiology, mutational landscape and staging of hepatocellular carcinoma. Chin Clin Oncol. 2021;10(1):2–2. https://doi.org/10.21037/cco-20-162.
Bednarsch J, Czigany Z, Heise D, Joechle K, Luedde T, Heij L, et al. Prognostic evaluation of HCC patients undergoing surgical resection: an analysis of 8 different staging systems. Langenbeck’s Arch Surg. 2020;406(1):75–86. https://doi.org/10.1007/s00423-020-02052-1.
Pinter M, Trauner M, Peck-Radosavlijec M, Seighart W. Cancer and liver cirrhosis: implications on prognosis and management. ESMO Open. 2016;1(2):e000042. https://doi.org/10.1136/esmoopen-2016-000042.
Khemlina G, Ikeda S, Kurzrock R. The biology of hepatocellular carcinoma: implications for genomic and immune therapies. Mol Cancer. 2017;16(1). https://doi.org/10.1186/s12943-017-0712-x.
Goossens N, Hoshida Y. Hepatitis C virus-induced hepatocellular carcinoma. Clin Mol Hepatol. 2015;21(2):105. https://doi.org/10.3350/cmh.2015.21.2.105.
Nguyen MH, Wong G, Gane E, Kao J, Dushkeiko G. Hepatitis B virus: advances in prevention, diagnosis, and therapy. Clin Microbiol Rev. 2020;33(2). https://doi.org/10.1128/cmr.00046-19
D’souza S, Lau KC, Coffin CS, Patel TR. Molecular mechanisms of viral hepatitis induced hepatocellular carcinoma. World J Gastroenterol. 2020;26(38):5759–83. https://doi.org/10.3748/wjg.v26.i38.5759.
Rocco A, Compare D, Angrisani D, SanduzziZamparelli M, Nardone G. Alcoholic disease: liver and beyond. World J Gastroenterol. 2014;20(40):14652. https://doi.org/10.3748/wjg.v20.i40.14652.
Neuschwander-Tetri B. Non-alcoholic fatty liver disease. BMC Med. 2017;15(1). https://doi.org/10.1186/s12916-017-0806-8.
Affo S, Yu L, Schwabe R. The role of cancer-associated fibroblasts and fibrosis in liver cancer. Annu Rev Pathol. 2017;12(1):153–86. https://doi.org/10.1146/annurev-pathol-052016-100322.
Dhar D, Baglieri J, Kisseleva T, Brenner DA. Mechanisms of liver fibrosis and its role in liver cancer. Exp Biol Med. 2020;245(2):96–108. https://doi.org/10.1177/1535370219898141.
Anwanwan D, Singh SK, Singh S, Saikam V, Singh R. Challenges in liver cancer and possible treatment approaches. Biochimica et Biophysica Acta (BBA) - Rev Cancer. 2020;1873(1),188314. https://doi.org/10.1016/j.bbcan.2019.188314.
Chen Z, Xie H, Hu M, Huang T, Hu Y, Sang N, and Zhao Y. Recent progress in treatment of hepatocellular carcinoma. Am J Cancer Res. 2020;10(9):2993. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7539784/ (Accessed: 31 October 2022).
Petruzzi P, Crocetti L, Lencioni R. Chemoembolization of hepatocellular carcinoma. Semin Interv Radiol. 2013;30(01):003–11. https://doi.org/10.1055/s-0033-1333648.
Qiu Z, Li H, Zhang Z, Zhu Z, He S, Wang X, et al. A Pharmacogenomic landscape in human liver cancers. Cancer Cell. 2019;36(2):179-193.e11. https://doi.org/10.1016/j.ccell.2019.07.001.
•• Kong FH, Ye QF, Miao XY, Liu X, Haung SQ, Xiong L, et al. Current status of sorafenib nanoparticle delivery systems in the treatment of hepatocellular carcinoma. Theranostics. 2021;11(11):5464–90. https://doi.org/10.7150/thno.54822. This review illustrates the constituents of nanoparticles and how they influence drug delivery. In addition, this paper provided insight into the different drug delivery systems with regard to sorafenib in the treatment of HCC.
• Huang A, Yang XR, Chung WY, Dennison AR, and Zhou J. Targeted therapy for hepatocellular carcinoma. Sig Transduct Target Ther. 2020;5(1). https://doi.org/10.1038/s41392-020-00264-x. This paper provides an overview on different chemotherapy and immunotherapy agents available for the treatment of HCC and provides examples of chemotherapy agents used as sequential treatment to sorafenib
•• Zhao Y, Zhang YN, Wang KT, and Chen L. Lenvatinib for hepatocellular carcinoma: from preclinical mechanisms to anti-cancer therapy, Biochimica et Biophysica Acta (BBA) Rev Cancer. 2020;1874(1):188391. https://doi.org/10.1016/j.bbcan.2020.188391. This paper provides a summary of the mechanism of action of lenvatinib and describes clinical trials comparing lenvatinib with standard chemotherapy treatment. Additionally, this paper describes the results of clinical trials in which different combination therapy regimens are compared.
Sangro B, Sarobe P, Herves-Stubbs, and Melero I. Advances in immunotherapy for hepatocellular carcinoma. Nat Rev Gastroenterol Hepatol. 2021;18(8), 525-543. https://doi.org/10.1038/s41575-021-00438-0.
•• Luo, X., Wu, K. and He, X. Advances in drug development for hepatocellular carcinoma: clinical trials and potential therapeutic targets, J Exp Clin Cancer Res. 2021;40(1). https://doi.org/10.1186/s13046-021-01968-w. This review demonstrates the different therapy options available for HCC in terms of first-line and second-line treatments that are currently in use as well as therapy options that are at clinical trial stage.
Xu F, Jin T, Zhu Y, and Dai C. Immune checkpoint therapy in liver cancer. J Exp Clin Cancer Res. 2018;37(1). https://doi.org/10.1186/s13046-018-0777-4.
Sun JH, Luo Q, Liu LL. and Song GB Liver cancer stem cell markers: progression and therapeutic implications. World J Gastroenterol. 2016;22(13):3547. https://doi.org/10.3748/wjg.v22.i13.3547.
Cao L, Zhu YQ, Wu ZX, Wang GX, Cheng HW. Engineering nanotheranostic strategies for liver cancer. World J Gastrointest Oncol. 2021;13(10):1213–28. https://doi.org/10.4251/wjgo.v13.i10.1213.
Kaufman H, Kohlhapp F, Zloza A. Oncolytic viruses: a new class of immunotherapy drugs. Nat Rev Drug Discovery. 2015;4(9):642–62. https://doi.org/10.1038/nrd4663.
Li Y, Shen Y, Zhao R, Samudio I, Jia W, Bai X, et al. Oncolytic virotherapy in hepato-bilio-pancreatic cancer: the key to breaking the log jam? Cancer Med. 2020;9(9):2943–59. https://doi.org/10.1002/cam4.2949.
Li X, Sun X, Wang B, Li Y, Tong J. Oncolytic virus-based hepatocellular carcinoma treatment: current status, intravenous delivery strategies, and emerging combination therapeutic solutions. Asian J Pharm Sci. 2023;18(1):100771. https://doi.org/10.1016/j.ajps.2022.100771.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None of the authors has any potential conflicts of interest to disclose.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alawyia, B., Constantinou, C. Hepatocellular Carcinoma: a Narrative Review on Current Knowledge and Future Prospects. Curr. Treat. Options in Oncol. 24, 711–724 (2023). https://doi.org/10.1007/s11864-023-01098-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11864-023-01098-9