Abstract
A survey performed by the AAPS Drug Product Handling community revealed a general, mostly consensus, approach to the strategy for the selection of surfactant type and level for biopharmaceutical products. Discussing and building on the survey results, this article describes the common approach for surfactant selection and control strategy for protein-based therapeutics and focuses on key studies, common issues, mitigations, and rationale. Where relevant, each section is prefaced by survey responses from the 22 anonymized respondents. The article format consists of an overview of surfactant stabilization, followed by a strategy for the selection of surfactant level, and then discussions regarding risk identification, mitigation, and control strategy. Since surfactants that are commonly used in biologic formulations are known to undergo various forms of degradation, an effective control strategy for the chosen surfactant focuses on understanding and controlling the design space of the surfactant material attributes to ensure that the desired material quality is used consistently in DS/DP manufacturing. The material attributes of a surfactant added in the final DP formulation can influence DP performance (e.g., protein stability). Mitigation strategies are described that encompass risks from host cell proteins (HCP), DS/DP manufacturing processes, long-term storage, as well as during in-use conditions.
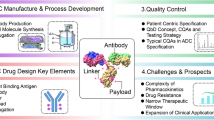
Graphical Abstract



Similar content being viewed by others
Change history
11 January 2023
A Correction to this paper has been published: https://doi.org/10.1208/s12248-023-00780-y
References
Number of products and pipeline count per modality for commonly used surfactants. 22 December 2021.
Bam NB, Randolph TW, Cleland JL. Stability of protein formulations: investigation of surfactant effects by a novel EPR spectroscopic technique. Pharm Res. 1995;12(1):2–11.
Misono T, et al. Surface adsorption and micelle formation of polyoxyethylene-type nonionic surfactants in mixtures of water and hydrophilic imidazolium-type ionic liquid. J Oleo Sci. 2016;65(6):499–506.
Khan T, Mahler H-C, Kishore R. Key interactions of surfactants in therapeutic protein formulations: a review. Eur J Pharm Biopharm. 2015;97.
Bam NB, et al. Tween protects recombinant human growth hormone against agitation-induced damage via hydrophobic interactions. J Pharm Sci. 1998;87(12):1554–9.
Chou DK, et al. Effects of Tween 20 and Tween 80 on the stability of albutropin during agitation. J Pharm Sci. 2005;94(6):1368–81.
Braun AC, et al. Predicting critical micelle concentration and micelle molecular weight of polysorbate 80 using compendial methods. Eur J Pharm Biopharm. 2015;94:559–68.
Garidel P, et al. Surface tension and self-association properties of aqueous polysorbate 20 HP and 80 HP solutions: insights into protein stabilisation mechanisms. J Pharm Innov. 2021;16(4):726–34.
Kreilgaard L, et al. Effects of additives on the stability of recombinant human factor XIII during freeze-drying and storage in the dried solid. Arch Biochem Biophys. 1998;360(1):121–34.
Bollenbach L, et al. Poloxamer 188 as surfactant in biological formulations – an alternative for polysorbate 20/80? Int J Pharm. 2022;620:121706.
Mustafi D, et al. Multi-block poloxamer surfactants suppress aggregation of denatured proteins. Biochim Biophys Acta (BBA) Gen Subj. 2008;1780(1):7–15.
Katakam M, Banga AK. Use of poloxamer polymers to stabilize recombinant human growth hormone against various processing stresses. Pharm Dev Technol. 1997;2(2):143–9.
Chang D, et al. Investigation of interfacial properties of pure and mixed poloxamers for surfactant-mediated shear protection of mammalian cells. Colloids Surf, B. 2017;156:358–65.
Gigout A, Buschmann MD, Jolicoeur M. The fate of Pluronic F-68 in chondrocytes and CHO cells. Biotechnol Bioeng. 2008;100(5):975–87.
Lee HJ, et al. Molecular origins of surfactant-mediated stabilization of protein drugs. Adv Drug Deliv Rev. 2011;63(13):1160–71.
LUXTERNA™ (voretigene neparvovec-rzyl) [package insert]. Spark Therapeutics, Inc., 2017.
Fichter C. Modular lentiviral vectors for highly efficient transgene expression in resting immune cells. Viruses. 2021;13. https://doi.org/10.3390/v13061170.
Bam NB, Cleland JL, Randolph TW. Molten globule intermediate of recombinant human growth hormone: stabilization with surfactants. Biotechnol Prog. 1996;12(6):801–9.
Merten OW, Hebben M, Bovolenta C. Production of lentiviral vectors. Mol Ther Methods Clin Dev. 2016;3:16017.
Gélinas J-F, et al. Assessment of selected media supplements to improve F/HN lentiviral vector production yields. Sci Rep. 2017;7(1):10198.
Vargo KB, et al. Surfactant impact on interfacial protein aggregation and utilization of surface tension to predict surfactant requirements for biological formulations. Mol Pharm. 2021;18(1):148–57.
Eppler A, et al. Relevant shaking stress conditions for antibody preformulation development. Eur J Pharm Biopharm. 2010;74(2):139–47.
Wang W, Wang YJ, Wang D. Dual effects of Tween 80 on protein stability. Int J Pharm. 2008;347(1–2):31–38.
Serno T, et al. Inhibition of agitation‐induced aggregation of an IgG‐antibody by hydroxypropyl‐β‐cyclodextrin. 2010;99(3):1193–1206.
Farjami A, et al. Evaluation of the physicochemical and biological stability of cetuximab under various stress condition. 2019;22:171–190.
He F, et al. High-throughput assessment of thermal and colloidal stability parameters for monoclonal antibody formulations. J Pharm Sci. 2011;100(12):5126–41.
Fesinmeyer RM, et al. Effect of ions on agitation- and temperature-induced aggregation reactions of antibodies. Pharm Res. 2009;26(4):903–13.
Fleischman ML, et al. Shipping-induced aggregation in therapeutic antibodies: utilization of a scale-down model to assess degradation in monoclonal antibodies. J Pharm Sci. 2017;106(4):994–1000.
Torisu T, et al. Synergistic effect of cavitation and agitation on protein aggregation. J Pharm Sci. 2017;106(2):521–9.
Telikepalli SN, et al. Structural characterization of IgG1 mAb aggregates and particles generated under various stress conditions. J Pharm Sci. 2014;103(3):796–809.
Kiese S, et al. Shaken, not stirred: mechanical stress testing of an IgG1 antibody. J Pharm Sci. 2008;97(10):4347–66.
Mahler HC, et al. Induction and analysis of aggregates in a liquid IgG1-antibody formulation. Eur J Pharm Biopharm. 2005;59(3):407–17.
Ishikawa T, et al. Prevention of stirring-induced microparticle formation in monoclonal antibody solutions. Biol Pharm Bull. 2010;33(6):1043–6.
Colombié S, Gaunand A, Lindet B. Lysozyme inactivation under mechanical stirring: effect of physical and molecular interfaces. Enzyme Microb Technol. 2001;28(9):820–6.
Hawe A, et al. Forced degradation of therapeutic proteins. J Pharm Sci. 2012;101(3):895–913.
Nowak C, et al. Forced degradation of recombinant monoclonal antibodies: a practical guide. mAbs. 2017;9(8):1217–1230.
Treuheit MJ, Kosky AA, Brems DN. Inverse relationship of protein concentration and aggregation. Pharm Res. 2002;19(4):511–6.
Kalonia CK, et al. Protein adsorption and layer formation at the stainless steel–solution interface mediates shear-induced particle formation for an IgG1 monoclonal antibody. Mol Pharm. 2018;15(3):1319–31.
Wang W, Roberts CJ. Protein aggregation - mechanisms, detection, and control. Int J Pharm. 2018;550(1–2):251–68.
Mahler HC, et al. Protein aggregation: pathways, induction factors and analysis. J Pharm Sci. 2009;98(9):2909–34.
Gikanga B, et al. Processing impact on monoclonal antibody drug products: protein subvisible particulate formation induced by grinding stress. PDA J Pharm Sci Technol. 2017;71(3):172.
Sediq AS, et al. No touching! Abrasion of adsorbed protein is the root cause of subvisible particle formation during stirring. J Pharm Sci. 2016;105(2):519–29.
Brückl L, et al. A systematic evaluation of mechanisms, material effects, and protein-dependent differences on friction-related protein particle formation in formulation and filling steps. Int J Pharm. 2016;511(2):931–45.
Gikanga B, Maa YF. A review on mixing-induced protein particle formation: the puzzle of bottom-mounted mixers. J Pharm Sci. 2020;109(8):2363–74.
Ladner T, et al. CFD supported investigation of shear induced by bottom-mounted magnetic stirrer in monoclonal antibody formulation. Pharm Res. 2018;35(11):215.
Toth SI, Smith LA, Ahmed SA. Extreme sensitivity of botulinum neurotoxin domains towards mild agitation. J Pharm Sci. 2009;98(9):3302–11.
Kiese S, et al. Equilibrium studies of protein aggregates and homogeneous nucleation in protein formulation. J Pharm Sci. 2010;99(2):632–44.
Cromwell MEM, Hilario E, Jacobson F. Protein aggregation and bioprocessing. AAPS J. 2006;8(3):E572–9.
Colombié S, Gaunand A, Lindet B. Lysozyme inactivation under mechanical stirring: effect of physical and molecular interfaces. Enzyme Microb Technol. 2001;28(9–10):820–6.
Li J, et al. Interfacial stress in the development of biologics: fundamental understanding, current practice, and future perspective. Aaps j. 2019;21(3):44.
Koepf E, et al. Notorious but not understood: How liquid-air interfacial stress triggers protein aggregation. Int J Pharm. 2018;537(1–2):202–12.
Randolph TW, et al. Do not drop: mechanical shock in vials causes cavitation, protein aggregation, and particle formation. J Pharm Sci. 2015;104(2):602–11.
den Engelsman J, et al. Strategies for the assessment of protein aggregates in pharmaceutical biotech product development. Pharm Res. 2011;28(4):920–33.
Xing Z, et al. Scale-up analysis for a CHO cell culture process in large-scale bioreactors. Biotechnol Bioeng. 2009;103(4):733–46.
Dengl S, et al. Aggregation and chemical modification of monoclonal antibodies under upstream processing conditions. Pharm Res. 2013;30(5):1380–99.
Nejadnik MR, et al. Postproduction handling and administration of protein pharmaceuticals and potential instability issues. J Pharm Sci. 2018;107(8):2013–9.
Snell JR, et al. Particle formation and aggregation of a therapeutic protein in nanobubble suspensions. J Pharm Sci. 2016;105(10):3057–63.
U.S. Food and Drug Administration, C.f.D.E.a.R.C., Center for Biologics Evaluation and Research (CBER), Guidance document Q1A(R2) stability testing of new drug substances and products. Vol. Revision 2. 2003, Rockville, MD.
(QWP), E.M.A.E.C.f.M.P.f.H.U.C.Q.W.P., Requirements to the chemical and pharmaceutical quality documentation concerning investigational medicinal products in clinical trials. Vol. Revision 2. 2022.
(QWP), E.M.A.E.C.f.M.P.f.H.U.C.Q.W.P., Guideline on strategies to identify and mitigate risks for first-in-human and early clinical trials with investigational medicinal products. Vol. Revision 1. 2017.
Kumru OS, et al. Compatibility, physical stability, and characterization of an IgG4 monoclonal antibody after dilution into different intravenous administration bags. J Pharm Sci. 2012;101(10):3636–50.
Morar-Mitrica S, et al. Development of a stable low-dose aglycosylated antibody formulation to minimize protein loss during intravenous administration. mAbs. 2015;7(4):792–803.
Kapp SJ, et al. Competitive adsorption of monoclonal antibodies and nonionic surfactants at solid hydrophobic surfaces. J Pharm Sci. 2015;104(2):593–601.
Sreedhara A, et al. Stability of IgG1 monoclonal antibodies in intravenous infusion bags under clinical in-use conditions. J Pharm Sci. 2012;101(1):21–30.
Brennan FR, Kiessling A. In vitro assays supporting the safety assessment of immunomodulatory monoclonal antibodies. Toxicol In Vitro. 2017;45(Pt 3):296–308.
Besheer A. Protein adsorption to in-line filters of intravenous administration sets. J Pharm Sci. 2017;106(10):2959–65.
Mahler HC, et al. Adsorption behavior of a surfactant and a monoclonal antibody to sterilizing-grade filters. J Pharm Sci. 2010;99(6):2620–7.
Schick AJ, et al. Understanding loss of soluble high molecular weight species during filtration of low concentration therapeutic monoclonal antibodies. J Pharm Sci. 2021;110(5):1997–2004.
Shieh IC, Patel AR. Predicting the agitation-induced aggregation of monoclonal antibodies using surface tensiometry. Mol Pharm. 2015;12(9):3184–93.
Kannan A, et al. In-use interfacial stability of monoclonal antibody formulations diluted in saline i.v. Bags. J Pharm Sci. 2021;110(4):1687–92.
Doshi N, et al. Evaluation of super refined™ polysorbate 20 with respect to polysorbate degradation, particle formation and protein stability. J Pharm Sci. 2020;109(10):2986–95.
Tomlinson A, Zarraga IE, Demeule B. Characterization of polysorbate ester fractions and implications in protein drug product stability. Mol Pharm. 2020;17(7):2345–53.
Doshi N, et al. A comprehensive assessment of all-oleate polysorbate 80: free fatty acid particle formation, interfacial protection and oxidative degradation. Pharm Res. 2021;38(3):531–48.
Doshi N, et al. Evaluating a modified high purity polysorbate 20 designed to reduce the risk of free fatty acid particle formation. 2021;38(9):1563–1583.
Kannan A, et al. A mechanistic understanding of monoclonal antibody interfacial protection by hydrolytically degraded polysorbate 20 and 80 under IV bag conditions. Pharm Res. 2022;39(3):563–75.
Gervasi V, et al. Parenteral protein formulations: an overview of approved products within the European Union. Eur J Pharm Biopharm. 2018;131:8–24.
(CHMP), E.M.A.E.C.f.M.P.f.H.U., Draft Information for the package leaflet regarding polysorbates used as excipients in medicinal products for human use 2018.
Katz JS, et al. Emerging challenges and innovations in surfactant-mediated stabilization of biologic formulations. J Pharm Sci. 2022;111(4):919–32.
Kriegel C, et al. Pediatric safety of polysorbates in drug formulations. Children (Basel). 2019. 7(1).
Hanawa T, et al. Investigation of the release behavior of diethylhexyl phthalate from the polyvinyl-chloride tubing for intravenous administration. Int J Pharm. 2000;210(1–2):109–15.
Pearson SD, Trissel LA. Leaching of diethylhexyl phthalate from polyvinyl chloride containers by selected drugs and formulation components. Am J Hosp Pharm. 1993;50(7):1405–9.
de Lemos ML, Hamata L, Vu T. Leaching of diethylhexyl phthalate from polyvinyl chloride materials into etoposide intravenous solutions. J Oncol Pharm Pract. 2005;11(4):155–7.
Kishore RS, et al. Degradation of polysorbates 20 and 80: studies on thermal autoxidation and hydrolysis. J Pharm Sci. 2011;100(2):721–31.
Maggio ET. Polysorbates, immunogenicity, and the totality of the evidence, in BioProcess International. 2012. p. 1–6.
Grabarek AD, et al. What makes polysorbate functional? Impact of polysorbate 80 grade and quality on IgG stability during mechanical stress. J Pharm Sci. 2020;109(1):871–80.
Maggio ET. Polysorbates, peroxides, protein aggregation, and immunogenicity - a growing concern. J Excip Food Chem. 2012;3(2):45–53.
Kranz W, et al. Factors influencing polysorbate’s sensitivity against enzymatic hydrolysis and oxidative degradation. J Pharm Sci. 2019;108(6):2022–32.
Brovč EV, et al. Rational design to biologics development: the polysorbates point of view. Int J Pharm. 2020;581:119285.
Gopalrathnam G, et al. Impact of stainless steel exposure on the oxidation of polysorbate 80 in histidine placebo and active monoclonal antibody formulation. PDA J Pharm Sci Technol. 2018;72(2):163–75.
Prajapati I, et al. Near UV and visible light photo-degradation mechanisms in citrate buffer: one-electron reduction of peptide and protein disulfides promotes oxidation and cis/trans isomerization of unsaturated fatty acids of polysorbate 80. J Pharm Sci. 2022;111(4):991–1003.
Brovč EV, et al. Degradation of polysorbates 20 and 80 catalysed by histidine chloride buffer. Eur J Pharm Biopharm. 2020;154:236–45.
Doyle Drbohlav LM, et al. A mechanistic understanding of polysorbate 80 oxidation in histidine and citrate buffer systems-part 2. PDA J Pharm Sci Technol. 2019;73(4):320–30.
Mason BD, et al. Oxidation of free L-histidine by tert-butylhydroperoxide. Pharm Res. 2010;27(3):447–56.
Wang T, et al. Solution stability of poloxamer 188 under stress conditions. J Pharm Sci. 2019;108(3):1264–71.
Abdul-Fattah AM, et al. Investigating factors leading to fogging of glass vials in lyophilized drug products. Eur J Pharm Biopharm. 2013;85(2):314–26.
Singh SN, et al. Unexplored benefits of controlled ice nucleation: lyophilization of a highly concentrated monoclonal antibody solution. Int J Pharm. 2018;552(1–2):171–9.
Soeda K, et al. Impact of poloxamer 188 material attributes on proteinaceous visible particle formation in liquid monoclonal antibody formulations. J Pharm Sci. 2022;111(8):2191–200.
Kannan A, Shieh IC, Fuller GG. Linking aggregation and interfacial properties in monoclonal antibody-surfactant formulations. J Colloid Interface Sci. 2019;550:128–38.
Kim HL, et al. Modulation of protein adsorption by poloxamer 188 in relation to polysorbates 80 and 20 at solid surfaces. J Pharm Sci. 2014;103(4):1043–9.
Dwivedi M, et al. Polysorbate degradation in biotherapeutic formulations: identification and discussion of current root causes. Int J Pharm. 2018;552(1–2):422–36.
Grapentin C, et al. Protein-polydimethylsiloxane particles in liquid vial monoclonal antibody formulations containing poloxamer 188. 2020;109(8):2393–2404.
Fang L, et al. Physicochemical excipient-container interactions in prefilled syringes and their impact on syringe functionality. PDA J Pharm Sci Technol. 2021;75(4):317–31.
Wang T, et al. Impact of surfactants on the functionality of prefilled syringes. J Pharm Sci. 2020;109(11):3413–22.
Wuchner K, et al. Industry perspective on the use and characterization of polysorbates for biopharmaceutical products part 1: survey report on current state and common practices for handling and control of polysorbates. J Pharm Sci. 2022;111(5):1280–91.
Santos MS, Tavares FW, Biscaia EC Jr. Molecular thermodynamics of micellization: micelle size distributions and geometry transitions. Braz J Chem Eng. 2016;33(3):515–23.
Yoshino N, et al. Critical micelle concentration and particle size determine adjuvanticity of cyclic lipopeptides. Scand J Immunol. 2018;88(2):e12698.
Savjani N, et al. Use of ferric thiocyanate derivatization for quantification of polysorbate 80 in high concentration protein formulations. Talanta. 2014;130:542–6.
Martos A, et al. Novel high-throughput assay for polysorbate quantification in biopharmaceutical products by using the fluorescent dye dii. J Pharm Sci. 2020;109(1):646–55.
About aura systems instruments designed for your needs. 2022; Available from: https://www.halolabs.com/aura-particle-analysis/. Accessed July 2022.
Gregoritza K, et al. Metal-induced fatty acid particle formation resulting from hydrolytic polysorbate degradation. J Pharm Sci. 2022;111(3):743–51.
Zhang L, et al. Dual effect of histidine on polysorbate 20 stability: mechanistic studies. Pharm Res. 2018;35(2):33.
Dixit N, et al. Residual host cell protein promotes polysorbate 20 degradation in a sulfatase drug product leading to free fatty acid particles. J Pharm Sci. 2016;105(5):1657–66.
Zhang S, et al. Rapid polysorbate 80 degradation by liver carboxylesterase in a monoclonal antibody formulated drug substance at early stage development. J Pharm Sci. 2020;109(11):3300–7.
Roy I, et al. Polysorbate degradation and particle formation in a high concentration mAb: formulation strategies to minimize effect of enzymatic polysorbate degradation. J Pharm Sci. 2021;110(9):3313–23.
United States Pharmacopeia (USP) 39 - national formulary (NF) 34. <1132> Residual host cell protein measurement in biopharmaceuticals. 2016, Rockville, MD: The United States Pharmacopeial Convention.
Shahrokh Z, Schmalzing D, Rawat R, Sluzky V, Ho K, Engelbergs J, Bishop J, Friedl E, Meiklejohn B, Ritter N. Science, risks, and regulations: current perspectives on host cell protein analysis and control in BioProcess International. 2016.
Bracewell DG, Francis R, Smales CM. The future of host cell protein (HCP) identification during process development and manufacturing linked to a risk-based management for their control. Biotechnol Bioeng. 2015;112(9):1727–37.
2.6.34. Host cell protein assays. Issue 27.2 ed, ed. E. Pharmacopoeia. 2015.
Chollangi S, et al. Development of robust antibody purification by optimizing protein-a chromatography in combination with precipitation methodologies. Biotechnol Bioeng. 2015;112(11):2292–304.
Pilely K, et al. Monitoring process-related impurities in biologics–host cell protein analysis. Anal Bioanal Chem. 2022;414(2):747–58.
Li X, et al. The measurement and control of high-risk host cell proteins for polysorbate degradation in biologics formulation. Antibody Therapeutics. 2022;5(1):42–54.
Prentice J, et al. Process characterization strategy for a precipitation step for host cell protein reduction. Biotechnol Prog. 2020;36(1):e2908.
Zhou JX, et al. Non-specific binding and saturation of polysorbate-20 with aseptic filter membranes for drug substance and drug product during mAb production. J Membr Sci. 2008;325(2):735–41.
Zhang Z, et al. Adsorption of non-ionic surfactant and monoclonal antibody on siliconized surface studied by neutron reflectometry. J Colloid Interface Sci. 2021;584:429–38.
Zheng S, Adams M, Mantri RV. An approach to mitigate particle formation on the dilution of a monoclonal antibody drug product in an IV administration fluid. J Pharm Sci. 2016;105(3):1349–50.
Vaclaw C, et al. Impact of polysorbate 80 grade on the interfacial properties and interfacial stress induced subvisible particle formation in monoclonal antibodies. J Pharm Sci. 2021;110(2):746–59.
Pegues MA, et al. Effect of fatty acid composition in polysorbate 80 on the stability of therapeutic protein formulations. Pharm Res. 2021;38(11):1961–75.
Doshi N, Martin J, Tomlinson A. Improving prediction of free fatty acid particle formation in biopharmaceutical drug products: incorporating ester distribution during polysorbate 20 degradation. Mol Pharm. 2020;17(11):4354–63.
Acknowledgements
The authors would like to acknowledge the AAPS Communities for providing the DP Handling Community with a space to meet and engage in scientific discussions. In addition, we want to thank Maria Nadeau from AAPS for setting up the electronic survey and providing the team with the responses.
Author information
Authors and Affiliations
Contributions
Annette Medina Morales and Sreedhara Alavattam designed and coordinated survey responses with AAPS, as well as collated and analyzed the responses. All of the authors contributed to the conception and design of the manuscript, as well as critical review and approval.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original article has been updated to correct the order of authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Morales, A.M., Sreedhara, A., Buecheler, J. et al. End-to-End Approach to Surfactant Selection, Risk Mitigation, and Control Strategies for Protein-Based Therapeutics. AAPS J 25, 6 (2023). https://doi.org/10.1208/s12248-022-00773-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12248-022-00773-3