Abstract
The objective was to develop a model to a priori identify the most suitable depot technology for a candidate based upon its therapeutic index (TI), pharmacokinetics (PK), and physical chemical properties. A depot map of release rates needed to achieve target PK in TI against release rates predicted based on intrinsic dissolution rate (IDR) and particle size (PS) clearly identified three zones: (a) products and candidates around the line of identity for which suspension is the appropriate depot technology, (b) area to the right of line of identity in which depot candidates would require a controlled release technology such as PLGA microspheres since in vivo release rate needed for PK in TI is significantly lower than predicted based on IDR and PS, and (c) area to the left of the line of identity where IDR is not sufficient to achieve target in vivo release rate for PK in TI and hence enhanced dissolution is needed such as with nanoparticles. Dose-solubility technology map of approved depot products and candidates showed clusters of products around a depot technology such as suspensions and microspheres, for drugs with high dose/low solubility and low dose/high solubility compounds, respectively. Novel PK-based computational tool showed how all combinations of depot doses and release rate constants for a candidate can be calculated to achieve plasma levels within the TI bounded by minimum effective and minimum toxic concentrations (MEC and MTC). The PK predictions for several drugs such as estradiol, risperidone, medroxyprogesterone acetate (MPA), and ziprasidone showed how these predictions can guide scientists to target specific depot doses and release rates into the depot formulation. In parallel, IDR of depot compounds clearly showed differentiation of compounds by successful depot technologies to achieve target dose and duration. For drugs with IDR between 0.1 and 1 mg/h/cm2, aqueous suspension has successfully delivered depot PK profile, while for candidates with IDRs greater than 1 mg/h/cm2, controlled release technology such as microsphere or in situ gel was required. The framework, prediction tools, and depot map will reduce the need for semi-empirical formulation work and preclinical studies to design depot formulations.

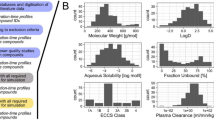
Graphical Abstract









Similar content being viewed by others
Abbreviations
- TI :
-
therapeutic index
- PK :
-
pharmacokinetics
- IDR :
-
intrinsic dissolution rate
- PS :
-
particle size
- PLGA :
-
poly-lactic-co-glycolic acid
- SC :
-
subcutaneous
- IM :
-
intramuscular
- MEC :
-
minimum effective concentration
- MTC :
-
minimum toxic concentration
- k a :
-
absorption rate constant
- t 1/2 :
-
elimination half-life
- Vd :
-
volume of distribution
- k e :
-
elimination rate constant
- k r :
-
release rate constant
- Tau:
-
depot duration
- Cmax:
-
maximum plasma or peak concentration during the dose
- Cmin:
-
minimum plasma or tough concentration during the dose
- F:
-
bioavailability of the active compound
- Log P:
-
log of octanol-water partition coefficient
- IR:
-
immediate release
References
Chien YW. Long-acting parenteral drug formulations. J Parenter Sci Technol. 1981;35(3):106–39.
Senior J. Insoluble salt forms and drug complexes. In: Senior J, Radomsky M, editors. Sustained release injectable products. Denver, CO: Interpharm Press; 2000. p. 41–70.
Murdan S, Florence A. Non-aqueous solutions and suspensions as sustained-release injectable formulations. In: Senior J, Radomsky M, editors. Sustained release injectable products. Denver, Co: Interpharm Press; 2000. p. 71–108.
Altamura AC, Sassella F, Santini A, Montresor C, Fumagalli F, Mundo E. Intramuscular preparations of antipsychotics. Drugs. 2003;63:493–512.
www.PDR.net. Prescriber’s Digital Reference, 2021 and Physician’s Desk Reference®-2004. 58th ed: Thomson Healthcare, The Medical Economics Company; 2003.
Luo J, Hubbard J, Midha K. Studies on the mechanism of absorption of depot neuroleptics: fluphenazine decanoate in sesame oil. Pharm Res. 1997;14(8):1079–984.
Shah JC. In: Stella V, Borchardt R, editors. Problems addressable by prodrugs: controlled release of small molecules; 2006) Chapter 9. p. 355–76.
Al-Hindawi M, James K, Nicholls P. The influence of the solvent on the availability of testosterone propionate from oily injections. J Pharm Pharmacol. 1981;81 65P.
Radd B, Newman A, Fegely B, Chrzanowski F, Lichten L, Walking W. Development of haloperidol in oil injection formulations. J Parenteral Sci Technol. 1985;39(1):48–50.
Tipton A, Dunn R. In situ gelling systems. In: Senior J, Radomsky M, editors. Sustained release injectable products. Denver, Co: Interpharm Press; 2000. p. 241–78.
Bao Q, Zhou Y, Wang Y, Choi S, Burgess D. Impact of formulation parameters on in vitro release from long acting injectable suspensions. AAPS J. 2021:23–42.
Shah J. Parenteral suspensions and nanosuspensions for NCE’s. In: Proceedings of the 42nd Arden House Pharmaceutical Technologies Conference-AAPS; 2007.
Wang EQ, Tseng E, Kendell LD, Inskeep PB, Shah J, Wisniecki P, Wagner D, Shah P. The effect of particle size on the pharmacokinetics of ziprasidone in Beagle dogs following intramuscular (IM) administration of aqueous depot formulations. AAPS J. 2006;9(S).
Shah J, Wisniecki P, Shah P, Wagner D. Injectable depot formulations and methods for providing sustained release of poorly soluble drugs comprising nanoparticles, US 2005671123 and WO 2006/191177, 2006;1–43.
Shah J. 2003 Novel injectable depot formulations of heterocyclic aryl compounds, US 20040138237, 2004;1–6.
Drug facts and comparisons. Lippincott Williams & Wilkins; 2017.
United States Pharmacopeia and National Formulary, USP 43 and NF 38. In: General Chapter on Physical Measurements, Description and Solubility, 1236, vol. 1-5; 2020.
Zhou M, Notari RE. A nomogram to predict the best biological half-life values for candidates for oral prolonged release formulations. J Pharm Sci. 1996;85(8):792–5.
Nara E, Masegi M, Hatono T, Hashida M. Pharmacokinetic analysis of drug absorption from muscle based on a physiological diffusion model: effect of molecular size on absorption. Pharm Res. 1992;9:161–9.
Hirano K, Ichihashi T, Yamada H. Studies on the absorption of practically water-insoluble drugs following injection. I. Intramuscular absorption from water-immiscible oil solutions in rats. Chem Pharm Bull. 1981;29(2):519–31.
Mishell D. Pharmacokinetics of Depo medroxyprogesterone acetate contraception. J Reprod Med. 1996;41(5):381–90.
Ramstack JM, Grandolfi GP, DHoore P, Mannaert E, Lasser RA. Risperdal Consta: prolonged release injectable delivery system using Medisorb microsphere technology. Proceedings of AAPS Annual Meeting. 2002;60:314.
Shah J, Chen JR, Chow D. Preformulation study of etoposide: possible physico-chemical characteristics responsible for the low and erratic oral bioavailability of etoposide. Pharm Res. 1989;6(5):407–12.
Paralkar VW, Borovecki H, Ke Z, Cameron KO, Lefker B, Grasser WA, Owen TA, Li M, DaSilva-Jardine P, Zhou M, Dunn RL, Dumont F, Korsmeyer R, Krasney P, Brown TA, Plowchalk D, Vukicevic S, Thompson DD. An EP2 receptor-selective prostaglandin E2 agonist induces bone healing. Proc Natl Acad Sci. 2003;100(11):6736–40.
Samtani MN, Vermeulen A, Stuyckens K. Population pharmacokinetics of intramuscular paliperidone palmitate in patients with schizophrenia. Clin Pharmacokinet. 2009;48(9):585–600.
Shah J, Sutton S, Way S, Brazeau G. Parenteral formulations: local injection site reactions and muscle toleration. In: Swarbrick J, editor. 4th Edition of Encyclopedia of Pharmaceutical Science and Technology. New York: Taylor & Francis; 2013. p. 2431–50.
Zuidema J, Kadir F, Titulaer HAC, Oussoren O. Release and absorption rates of intramuscularly and subcutaneously injected pharmaceuticals (II). Int J Pharm. 1994;104:189–207.
Sarisuta N, Parrott EL. Diffusivity and dissolution rate in polymeric solutions. Drug Dev Ind Pharm. 1983;9(5):861–75.
Rahnfeld L, Luciani P. Injectable Lipid-based depot formulations: where do we stand? Pharmaceutics. 2020;12(0567):1–28.
Rajoli RKR, Back DJ, Ramnard S, Maeyers CL, Flexner C, Owen A, Siccardi M. Physiologically based PK modeling to inform development of IM long-acting nanoformulations for HIV. Clin Pharmacokinet. 2015;54:639–50.
Ngyuen V, Bevernage J, Darville N, Tistaert C, Bocxlaer J, Rossenu V, Vereulen S, A. Linking in vitro intrinsic dissolution rate and thermodynamic solubility with pharmacokinetic profiles of bedaquiline long-acting aqueous microsuspensions in rats. Mol Pharm. 2021;18:952–65.
Acknowledgements
Christ Nieset for conducting the solubility and intrinsic dissolution rate measurements and Agnes Machate for collecting the physical chemical properties and PK parameters of approved depot drugs from various sources. We also appreciate editorial review and revisions made by Adesh Saxena of Pfizer Medical Writing Group and Thean Yeoh.
Author information
Authors and Affiliations
Contributions
Both JS and JH contributed to the concept of model for depot. JS designed the model and conducted the PK simulations while JH led the IDR measurements.
Corresponding author
Ethics declarations
Conflict of interest
None. JS and JH are Pfizer employees.
Additional information
This manuscript has not been published previously and not being considered for publication in any other journal currently.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(DOCX 21 kb)
Rights and permissions
About this article
Cite this article
Shah, J.C., Hong, J. Model for Long Acting Injectables (Depot Formulation) Based on Pharmacokinetics and Physical Chemical Properties. AAPS J 24, 44 (2022). https://doi.org/10.1208/s12248-022-00695-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12248-022-00695-0