Abstract
Ovarian aging reduced the quality of oocytes, resulting in age-related female infertility. It is reported that mesenchymal stem cells (MSCs) therapy can improve age-related ovarian function decline and the success rate of in vitro maturation (IVM) in assisted reproductive therapy. In order to investigate the effectiveness and mechanisms of MSCs to enhance oocyte quality of cumulus oocyte complexes (COCs) in advanced age, this study focus on the respective functional improvement of oocytes and granulosa cells (GCs) from aging mice and further to explore and verify the possible mechanisms. Here, we studied a popular but significant protein of follicular development, Forkhead box O-3a (FOXO3a), which is a transcription factor that mediates a variety of cellular processes, but the functions of which in regulating oocyte quality in MSCs therapy still remain inconclusive. In this study, the RNA-seq data of metaphase II (MII) oocytes and GCs isolated from COCs confirmed that, GCs of immature follicles show the most potential to be the targeted cells of bone marrow mesenchymal stem cells (BMSCs) by FOXO3a signaling pathway. Furthermore, we demonstrated the effectiveness of BMSCs co-culture with aging COCs to enhance oocyte quality and found its mechanism to function via ameliorating the biological function of GCs by alleviating FOXO3a levels. These results provide significant fundamental research on MSCs therapy on ovarian aging, as well as offering guidance for raising the success rate of assisted reproductive technology such IVM in clinical and non-clinical settings.
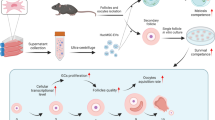
Graphical Abstract








Similar content being viewed by others
Data Availability
The data for this study are available by contacting the corresponding author upon reasonable request.
References
Wu J, Liu Y, Song Y, Wang L, Ai J, Li K. Aging conundrum: A perspective for ovarian aging. Front Endocrinol (Lausanne). 2022;13: 952471. https://doi.org/10.3389/fendo.2022.952471.
Bertoldo MJ, Listijono DR, Ho WJ, Riepsamen AH, Goss DM, Richani D, Jin XL, Mahbub S, Campbell JM, Habibalahi A, Loh WN, Youngson NA, Maniam J, Wong ASA, Selesniemi K, Bustamante S, Li C, Zhao Y, Marinova MB, Kim LJ, Lau L, Wu RM, Mikolaizak AS, Araki T, Le Couteur DG, Turner N, Morris MJ, Walters KA, Goldys E, O’Neill C, Gilchrist RB, Sinclair DA, Homer HA, Wu LE. NAD(+) Repletion Rescues Female Fertility during Reproductive Aging. Cell Rep. 2020;30:1670-1681.e1677. https://doi.org/10.1016/j.celrep.2020.01.058.
Gong Y, Zhang K, Xiong D, Wei J, Tan H, Qin S. Growth hormone alleviates oxidative stress and improves the IVF outcomes of poor ovarian responders: a randomized controlled trial. Reprod Biol Endocrinol. 2020;18:91. https://doi.org/10.1186/s12958-020-00648-2.
Navot D, Bergh PA, Williams MA, Garrisi GJ, Guzman I, Sandler B, Grunfeld L. Poor oocyte quality rather than implantation failure as a cause of age-related decline in female fertility. Lancet (London, England). 1991;337:1375–7. https://doi.org/10.1016/0140-6736(91)93060-m.
Edwards RG. Maturation in vitro of human ovarian oöcytes. Lancet (London, England). 1965;2:926–9. https://doi.org/10.1016/s0140-6736(65)92903-x.
Strowitzki T, Bruckner T, Roesner S. Maternal and neonatal outcome and children’s development after medically assisted reproduction with in-vitro matured oocytes-a systematic review and meta-analysis. Hum Reprod Update. 2021;27:460–73. https://doi.org/10.1093/humupd/dmaa056.
Li J, Chen J, Sun T, Zhang S, Jiao T, Chian RC, Li Y, Xu Y. Chromosome aneuploidy analysis in embryos derived from in vivo and in vitro matured human oocytes. J Transl Med. 2021;19:416. https://doi.org/10.1186/s12967-021-03080-1.
Gudimchuk NB, McIntosh JR. Regulation of microtubule dynamics, mechanics and function through the growing tip. Nat Rev Mol Cell Biol. 2021;22:777–95. https://doi.org/10.1038/s41580-021-00399-x.
van der Reest J, Nardini Cecchino G, Haigis MC, Kordowitzki P. Mitochondria: Their relevance during oocyte ageing. Ageing Res Rev. 2021;70:101378. https://doi.org/10.1016/j.arr.2021.101378.
Chiang JL, Shukla P, Pagidas K, Ahmed NS, Karri S, Gunn DD, Hurd WW, Singh KK. Mitochondria in Ovarian Aging and Reproductive Longevity. Ageing Res Rev. 2020;63: 101168. https://doi.org/10.1016/j.arr.2020.101168.
May-Panloup P, Boucret L, Chao de la Barca JM, Desquiret-Dumas V, Ferré-L’Hotellier V, Morinière C, Descamps P, Procaccio V, Reynier P. Ovarian ageing: the role of mitochondria in oocytes and follicles. Hum Reprod Update. 2016;22:725–43. https://doi.org/10.1093/humupd/dmw028.
Llonch S, Barragán M, Nieto P, Mallol A, Elosua-Bayes M, Lorden P, Ruiz S, Zambelli F, Heyn H, Vassena R, Payer B. Single human oocyte transcriptome analysis reveals distinct maturation stage-dependent pathways impacted by age. Aging Cell. 2021;20: e13360. https://doi.org/10.1111/acel.13360.
Hu W, Zeng H, Shi Y, Zhou C, Huang J, Jia L, Xu S, Feng X, Zeng Y, Xiong T, Huang W, Sun P, Chang Y, Li T, Fang C, Wu K, Cai L, Ni W, Li Y, Yang Z, Zhang QC, Chian R, Chen Z, Liang X, Kee K. Single-cell transcriptome and translatome dual-omics reveals potential mechanisms of human oocyte maturation. Nat Commun. 2022;13:5114. https://doi.org/10.1038/s41467-022-32791-2.
Reyes JM, Silva E, Chitwood JL, Schoolcraft WB, Krisher RL, Ross PJ. Differing molecular response of young and advanced maternal age human oocytes to IVM. Hum Reprod. 2017;32:2199–208. https://doi.org/10.1093/humrep/dex284.
Zhang Y, Yan Z, Qin Q, Nisenblat V, Chang HM, Yu Y, Wang T, Lu C, Yang M, Yang S, Yao Y, Zhu X, Xia X, Dang Y, Ren Y, Yuan P, Li R, Liu P, Guo H, Han J, He H, Zhang K, Wang Y, Wu Y, Li M, Qiao J, Yan J, Yan L. Transcriptome Landscape of Human Folliculogenesis Reveals Oocyte and Granulosa Cell Interactions. Mol Cell. 2018;72:1021-1034.e1024. https://doi.org/10.1016/j.molcel.2018.10.029.
Wang G, Zhang M, Zhang Y, Xie Y, Zou J, Zhong J, Zheng Z, Zhou X, Zheng Y, Chen B, Liu C. NAT10-mediated mRNA N4-acetylcytidine modification promotes bladder cancer progression. Clin Transl Med. 2022;12: e738. https://doi.org/10.1002/ctm2.738.
Richani D, Dunning KR, Thompson JG, Gilchrist RB. Metabolic co-dependence of the oocyte and cumulus cells: essential role in determining oocyte developmental competence. Hum Reprod Update. 2021;27:27–47. https://doi.org/10.1093/humupd/dmaa043.
Liu Y, Wang L, Ai J, Li K. Mitochondria in Mesenchymal Stem Cells: Key to Fate Determination and Therapeutic Potential. Stem Cell Rev Rep. 2024. https://doi.org/10.1007/s12015-024-10681-y.
Alberico HC, Woods DC. Role of Granulosa Cells in the Aging Ovarian Landscape: A Focus on Mitochondrial and Metabolic Function. Front Physiol. 2021;12: 800739. https://doi.org/10.3389/fphys.2021.800739.
Zhang D, Zhang X, Zeng M, Yuan J, Liu M, Yin Y, Wu X, Keefe DL, Liu L. Increased DNA damage and repair deficiency in granulosa cells are associated with ovarian aging in rhesus monkey. J Assist Reprod Genet. 2015;32:1069–78. https://doi.org/10.1007/s10815-015-0483-5.
Fragouli E, Lalioti MD, Wells D. The transcriptome of follicular cells: biological insights and clinical implications for the treatment of infertility. Hum Reprod Update. 2014;20:1–11. https://doi.org/10.1093/humupd/dmt044.
Jiang ZX, Wang YN, Li ZY, Dai ZH, He Y, Chu K, Gu JY, Ji YX, Sun NX, Yang F, Li W. The m6A mRNA demethylase FTO in granulosa cells retards FOS-dependent ovarian aging. Cell Death Dis. 2021;12:744. https://doi.org/10.1038/s41419-021-04016-9.
Piras AR, Ariu F, Maltana A, Leoni GG, Martino NA, Mastrorocco A, Dell’Aquila ME, Bogliolo L. Protective effect of resveratrol against cadmium-induced toxicity on ovine oocyte in vitro maturation and fertilization. J Anim Sci Biotechnol. 2022;13:83. https://doi.org/10.1186/s40104-022-00731-1.
Ma L, Cai L, Hu M, Wang J, Xie J, Xing Y, Shen J, Cui Y, Liu XJ, Liu J. Coenzyme Q10 supplementation of human oocyte in vitro maturation reduces postmeiotic aneuploidies. Fertil Steril. 2020;114:331–7. https://doi.org/10.1016/j.fertnstert.2020.04.002.
Wang L, Mei Q, Xie Q, Li H, Su P, Zhang L, Li K, Ma D, Chen G, Li J, Xiang W. A comparative study of Mesenchymal Stem Cells transplantation approach to antagonize age-associated ovarian hypofunction with consideration of safety and efficiency. J Adv Res. 2022;38:245–59. https://doi.org/10.1016/j.jare.2021.09.001.
Yan L, Wu Y, Li L, Wu J, Zhao F, Gao Z, Liu W, Li T, Fan Y, Hao J, Liu J, Wang H. Clinical analysis of human umbilical cord mesenchymal stem cell allotransplantation in patients with premature ovarian insufficiency. Cell Prolif. 2020;53: e12938. https://doi.org/10.1111/cpr.12938.
Zafardoust S, Kazemnejad S, Darzi M, Fathi-Kazerooni M, Rastegari H, Mohammadzadeh A. Improvement of Pregnancy Rate and Live Birth Rate in Poor Ovarian Responders by Intraovarian Administration of Autologous Menstrual Blood Derived- Mesenchymal Stromal Cells: Phase I/II Clinical Trial. Stem Cell Rev Rep. 2020;16:755–63. https://doi.org/10.1007/s12015-020-09969-6.
Maldonado M, Huang T, Chen J, Zhong Y. Differentiation Potential of Human Wharton’s Jelly-Derived Mesenchymal Stem Cells and Paracrine Signaling Interaction Contribute to Improve the In Vitro Maturation of Mouse Cumulus Oocyte Complexes. Stem Cells Int. 2018;2018:7609284. https://doi.org/10.1155/2018/7609284.
Nejabati HR, Nikzad S, Roshangar L. Therapeutic Potential of Mesenchymal Stem Cells in PCOS. Curr Stem Cell Res Ther. 2024;19:134–44. https://doi.org/10.2174/1574888x18666230517123256.
Lange-Consiglio A, Lazzari B, Pizzi F, Idda A, Cremonesi F, Capra E. Amniotic microvesicles impact hatching and pregnancy percentages of in vitro bovine embryos and blastocyst microRNA expression versus in vivo controls. Sci Rep. 2020;10:501. https://doi.org/10.1038/s41598-019-57060-z.
Hu J, Liu T, Fu F, Cui Z, Lai Q, Zhang Y, Yu B, Liu F, Kou J, Li F. Omentin1 ameliorates myocardial ischemia-induced heart failure via SIRT3/FOXO3a-dependent mitochondrial dynamical homeostasis and mitophagy. J Transl Med. 2022;20:447. https://doi.org/10.1186/s12967-022-03642-x.
Qin X, Dang W, Yang X, Wang K, Kebreab E, Lyu L. Neddylation inactivation affects cell cycle and apoptosis in sheep follicular granulosa cells. J Cell Physiol. 2022;237:3278–91. https://doi.org/10.1002/jcp.30777.
Liu H, Jiang C, La B, Cao M, Ning S, Zhou J, Yan Z, Li C, Cui Y, Ma X, Wang M, Chen L, Yu Y, Chen F, Zhang Y, Wu H, Liu J, Qin L. Human amnion-derived mesenchymal stem cells improved the reproductive function of age-related diminished ovarian reserve in mice through Ampk/FoxO3a signaling pathway. Stem Cell Res Ther. 2021;12:317. https://doi.org/10.1186/s13287-021-02382-x.
Rosario R, Stewart HL, Spears N, Telfer EE, Anderson RA. Anti-Mullerian hormone attenuates both cyclophosphamide-induced damage and PI3K signalling activation, while rapamycin attenuates only PI3K signalling activation, in human ovarian cortex in vitro. Hum Reprod. 2024;39:382–92. https://doi.org/10.1093/humrep/dead255.
Zhai J, Zhang J, Zhang L, Liu X, Deng W, Wang H, Zhang Z, Liu W, Chen B, Wu C, Long H, Xu B, Ying X, Zou H, He J, Li P, Hu T, Xiang W, Li J. Autotransplantation of the ovarian cortex after in-vitro activation for infertility treatment: a shortened procedure. Hum Reprod. 2021;36:2134–47. https://doi.org/10.1093/humrep/deab143.
Castrillon DH, Miao L, Kollipara R, Horner JW, DePinho RA. Suppression of ovarian follicle activation in mice by the transcription factor Foxo3a. Science. 2003;301:215–8. https://doi.org/10.1126/science.1086336.
Lv Y, Cao RC, Liu HB, Su XW, Lu G, Ma JL, Chan WY. Single-oocyte gene expression suggests that curcumin can protect the ovarian reserve by regulating the PTEN-AKT-FOXO3a pathway. Int J Mol Sci. 2021;22:6570. https://doi.org/10.3390/ijms22126570.
Mei NH, Guo SM, Zhou Q, Zhang YR, Liu XZ, Yin Y, He X, Yang J, Yin TL, Zhou LQ. H3K4 Methylation Promotes Expression of Mitochondrial Dynamics Regulators to Ensure Oocyte Quality in Mice. Adv Sci (Weinh). 2023;10: e2204794. https://doi.org/10.1002/advs.202204794.
Jiang X, Cheng Y, Zhu Y, Xu C, Li Q, Xing X, Li W, Zou J, Meng L, Azhar M, Cao Y, Tong X, Qin W, Zhu X, Bao J. Maternal NAT10 orchestrates oocyte meiotic cell-cycle progression and maturation in mice. Nat Commun. 2023;14:3729. https://doi.org/10.1038/s41467-023-39256-0.
Zhang T, Xi Q, Wang D, Li J, Wang M, Li D, Zhu L, Jin L. Mitochondrial dysfunction and endoplasmic reticulum stress involved in oocyte aging: an analysis using single-cell RNA-sequencing of mouse oocytes. J Ovarian Res. 2019;12:53. https://doi.org/10.1186/s13048-019-0529-x.
Zhao S, Heng N, Wang H, Wang H, Zhang H, Gong J, Hu Z, Zhu H. Mitofusins: from mitochondria to fertility. Cell Mol Life Sci. 2022;79:370. https://doi.org/10.1007/s00018-022-04386-z.
Cacciottola L, Vitale F, Donnez J, Dolmans MM. Use of mesenchymal stem cells to enhance or restore fertility potential: a systematic review of available experimental strategies. Hum Reprod Open. 2023;2023:hoad040. https://doi.org/10.1093/hropen/hoad040.
Wen T, Wang H, Li Y, Lin Y, Zhao S, Liu J, Chen B. Bone mesenchymal stem cell-derived extracellular vesicles promote the repair of intervertebral disc degeneration by transferring microRNA-199a. Cell Cycle. 2021;20:256–70. https://doi.org/10.1080/15384101.2020.1863682.
Yu G, Sun W, Wang W, Le C, Liang D, Shuai L. Overexpression of microRNA-202–3p in bone marrow mesenchymal stem cells improves cerebral ischemia-reperfusion injury by promoting angiogenesis and inhibiting inflammation. Aging (Albany NY). 2021;13:11877–88. https://doi.org/10.18632/aging.202889.
Zhang M, Liu D, Li S, Chang L, Zhang Y, Liu R, Sun F, Duan W, Du W, Wu Y, Zhao T, Xu C, Lu Y. Bone marrow mesenchymal stem cell transplantation retards the natural senescence of rat hearts. Stem Cells Transl Med. 2015;4:494–502. https://doi.org/10.5966/sctm.2014-0206.
Yu C, Chen J, Ma J, Zang L, Dong F, Sun J, Zheng M. Identification of Key Genes and Signaling Pathways Associated with the Progression of Gastric Cancer. Pathol Oncol Res. 2020;26:1903–19. https://doi.org/10.1007/s12253-019-00781-3.
Santo EE, Stroeken P, Sluis PV, Koster J, Versteeg R, Westerhout EM. FOXO3a is a major target of inactivation by PI3K/AKT signaling in aggressive neuroblastoma. Cancer Res. 2013;73:2189–98. https://doi.org/10.1158/0008-5472.Can-12-3767.
Tesarik J, Mendoza-Tesarik R. Mitochondria in human fertility and infertility. Int J Mol Sci. 2023;24:8950. https://doi.org/10.3390/ijms24108950.
Acknowledgements
We thanks to all authors for their contribution to this experiment. We would also thank Genergy Biotechnology Co., Ltd. (Shanghai, China) for RNA high-throughput sequencing and bioinformatic analysis, as well as SANGON BIOTECH for designing and synthesis of various primers (shanghai, China) and RiboBio Co., Ltd. (Guangzhou, China) for the silencing sequence design and synthesis of target gene.
Funding
This work has been supported by the National Key Research and Development Program of China (2017YFC1002002) and the National Natural Science Foundation of China (82101700).
Author information
Authors and Affiliations
Contributions
Conceptualization: Ling Zhang, Wenpei Xiang.
Formal analysis: Lingjuan Wang, Yang Liu.
Methodology: Qiaojuan Mei, Hongbei Mou, Jiachen Wu, Xinyu Tang.
Project administration: Houxiu Xiao, Xiaotao Han, Liqun Lv, Huaibiao Li.
Resources: Jihui Ai, Kezhen Li.
Writing – original draft: Yinhua Song.
Writing – review & editing: Lingjuan Wang, Wenpei Xiang.
Corresponding authors
Ethics declarations
Ethics Approval
The application of specific pathogen-free grade C57BL/6 mice was approved by the Animal Ethics Committee of Huazhong University of Science and Technology and all experiments were carried out in accordance with relevant guidelines and regulations.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, L., Liu, Y., Song, Y. et al. Enhancing Oocyte Quality in Aging Mice: Insights from Mesenchymal Stem Cell Therapy and FOXO3a Signaling Pathway Activation. Reprod. Sci. (2024). https://doi.org/10.1007/s43032-024-01509-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s43032-024-01509-8