Abstract
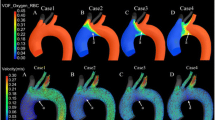
Interaction between native ventricular output and venoarterial extracorporeal membrane oxygenation (VA ECMO) flow may hinder oxygenated blood flow to the aortic arch branches, resulting in differential hypoxemia. Typically, the arterial cannula tip is placed in the iliac artery or abdominal aorta. However, the hemodynamics of a more proximal arterial cannula tip have not been studied before. This study investigated the effect of arterial cannula tip position on VA ECMO blood flow to the upper extremities using computational fluid dynamics simulations. Four arterial cannula tip positions (P1. common iliac, P2. abdominal aorta, P3. descending aorta and P4. aortic arch) were compared with different degrees of cardiac dysfunction and VA ECMO support (50%, 80% and 90% support). P4 was able to supply oxygenated blood to the arch vessels at all support levels, while P1 to P3 only supplied the arch vessels during the highest level (90%) of VA ECMO support. Even during the highest level of support, P1 to P3 could only provide oxygenated VA-ECMO flow at 0.11 L/min to the brachiocephalic artery, compared with 0.5 L/min at P4. This study suggests that cerebral perfusion of VA ECMO flow can be increased by advancing the arterial cannula tip towards the aortic arch.




Similar content being viewed by others
Abbreviations
- VA ECMO:
-
Venoarterial extracorporeal membrane oxygenation
- CFD:
-
Computational fluid dynamics
- P1, P2, P3 and P4:
-
Position 1, position 2, position 3 and position 4
- CT:
-
Computed tomography
- ECPR:
-
Extracorporeal cardiopulmonary resuscitation
- BCA:
-
Brachiocephalic artery
- LCCA:
-
Left common carotid artery
- LSCA:
-
Left subclavian artery
- SMA:
-
Superior mesenteric artery
- IMA:
-
Inferior mesenteric artery
- LCI:
-
Left common iliac
- RCI:
-
Right common iliac
- LV:
-
Left ventricle
- MAP:
-
Mean aortic pressure
References
Pavlushkov E, Berman M, Valchanov K (2017) Cannulation techniques for extracorporeal life support. Ann Transl Med. https://doi.org/10.21037/atm.2016.11.47
Strunina S, Hozman J, Ostadal P (2019) The peripheral cannulas in extracorporeal life support. Biomed Eng 64(2):127–133. https://doi.org/10.1515/bmt-2017-0107
Jayaraman AL, Cormican D, Shah P, Ramakrishna H (2017) Cannulation strategies in adult veno-arterial and veno-venous extracorporeal membrane oxygenation: techniques, limitations, and special considerations. Ann Card Anaesth 20(Suppl 1):S11. https://doi.org/10.4103/0971-9784.197791
Lorusso R, Barili F, Mauro MD, Gelsomino S, Parise O, Rycus PT, Maessen J, Mueller T, Muellenbach R, Belohlavek J (2016) In-hospital neurologic complications in adult patients undergoing venoarterial extracorporeal membrane oxygenation: results from the extracorporeal life support organization registry. Crit Care Med 44(10):e964–e972. https://doi.org/10.1097/CCM.0000000000001865
Rupprecht L, Lunz D, Philipp A, Lubnow M, Schmid C (2015) Pitfalls in percutaneous ECMO cannulation. Heart Lung Vessels 7(4):320
Contento C, Battisti A, Agrò B, De Marco M, Iaiza A, Pietraforte L, Pisani P, Proietti A, Vitalini E, Montalto A (2020) A novel veno-arteriovenous extracorporeal membrane oxygenation with double pump for the treatment of Harlequin syndrome. Perfusion 35(1suppl):65–72. https://doi.org/10.1177/0267659120908409
Pozzebon S, Blandino Ortiz A, Franchi F, Cristallini S, Belliato M, Lheureux O, Brasseur A, Vincent J-L, Scolletta S, Creteur J (2018) Cerebral near-infrared spectroscopy in adult patients undergoing veno-arterial extracorporeal membrane oxygenation. Neurocrit Care 29(1):94–104. https://doi.org/10.1007/s12028-018-0512-1
Javidfar J, Brodie D, Costa J, Miller J, Jurrado J, LaVelle M, Newmark A, Takayama H, Sonett JR, Bacchetta M (2012) Subclavian artery cannulation for venoarterial extracorporeal membrane oxygenation. ASAIO J 58(5):494–498
Chicotka S, Rosenzweig EB, Brodie D, Bacchetta M (2017) The “central sport model”: extracorporeal membrane oxygenation using the innominate artery for smaller patients as bridge to lung transplantation. ASAIO J 63(4):e39–e44
Kirker E, Korngold E, Hodson RW, Jones BM, McKay R, Cheema M, Heimansohn D, Moainie S, Hermiller J, Chatriwalla A (2020) Transcarotid versus subclavian/axillary access for transcatheter aortic valve replacement with SAPIEN 3. Ann Thorac Surg 110(6):1892–1897
Hou X, Yang X, Du Z, Xing J, Li H, Jiang C, Wang J, Xing Z, Li S, Li X (2015) Superior vena cava drainage improves upper body oxygenation during veno-arterial extracorporeal membrane oxygenation in sheep. Crit Care 19(1):1–10
Cai T, Li C, Xu B, Wang L, Du Z, Hao X, Guo D, Xing Z, Jiang C, Xin M (2021) Drainage from superior Vena Cava improves upper body oxygenation in patients on femoral veno-arterial extracorporeal membrane oxygenation. Front Cardiovasc Med 8
Falk L, Hultman J, Broman LM (2022) Differential hypoxemia and the clinical significance of venous drainage position during extracorporeal membrane oxygenation. Perfusion. https://doi.org/10.1177/02676591221090667
Falk L, Sallisalmi M, Lindholm JA, Lindfors M, Frenckner B, Broomé M, Broman LM (2019) Differential hypoxemia during venoarterial extracorporeal membrane oxygenation. Perfusion 34(1suppl):22–29
Nezami FR, Khodaee F, Edelman ER, Keller SP (2021) A computational fluid dynamics study of the extracorporeal membrane oxygenation-failing heart circulation. ASAIO J 67(3):276–283. https://doi.org/10.1097/MAT.0000000000001221
Stevens M, Callaghan F, Forrest P, Bannon P, Grieve S (2017) Flow mixing during peripheral veno-arterial extra corporeal membrane oxygenation–a simulation study. J Biomech 55:64–70. https://doi.org/10.1016/j.jbiomech.2017.02.009
Nezami FR, Ramezanpour M, Khodaee F, Goffer E, Edelman ER, Keller SP (2021) Simulation of fluid-structure interaction in extracorporeal membrane oxygenation circulatory support systems. J Cardiovasc Transl Res 1–9. https://doi.org/10.1007/s12265-021-10143-7
Zhang Q, Gao B, Chang Y (2018) The numerical study on the effects of cardiac function on the aortic oxygen distribution. Med Biol Eng Comput 56(7):1305–1313. https://doi.org/10.1007/s11517-017-1777-9
Prisco AR, Aguado-Sierra J, Butakoff C, Vazquez M, Houzeaux G, Eguzkitza B, Bartos JA, Yannopoulos D, Raveendran G, Holm M (2021) Concomitant respiratory failure can impair myocardial oxygenation in patients with Acute cardiogenic shock supported by VA-ECMO. J Cardiovasc Transl Res 1–10. https://doi.org/10.1007/s12265-021-10110-2
Rodriguez ML, Maharajh G (2018) Long venous cannula on the arterial position for VA-ECMO. Perfusion 33(6):423–425. https://doi.org/10.1177/0267659118765628
Alastruey J, Xiao N, Fok H, Schaeffter T, Figueroa CA (2016) On the impact of modelling assumptions in multi-scale, subject-specific models of aortic haemodynamics. J R Soc Interface 13(119):20160073. https://doi.org/10.1098/rsif.2016.0073
Xiao N, Alastruey J, Alberto Figueroa C (2014) A systematic comparison between 1-D and 3‐D hemodynamics in compliant arterial models. Int J Numer Methods Biomed Eng 30(2):204–231. https://doi.org/10.1002/cnm.2598
Cho YI, Kensey KR (1991) Effects of the non-newtonian viscosity of blood on flows in a diseased arterial vessel. Part 1: steady flows. Biorheology 28(3–4):241–262. https://doi.org/10.3233/bir-1991-283-415
Caballero A, Laín S (2015) Numerical simulation of non-newtonian blood flow dynamics in human thoracic aorta. Comput Methods Biomech BioMed Eng 18(11):1200–1216. https://doi.org/10.1080/10255842.2014.887698
Seetharaman A, Keramati H, Ramanathan K, Cove E, Kim M, Chua S, Leo HL (2021) Vortex dynamics of veno-arterial extracorporeal circulation: a computational fluid dynamics study. Phys Fluids 33(6):061908
Kato J, Seo T, Ando H, Takagi H, Ito T (1996) Coronary arterial perfusion during venoarterial extracorporeal membrane oxygenation. J Thorac Cardiovasc Surg 111(3):630–636. https://doi.org/10.1016/S0022-5223(96)70315-X
Hoeper MM, Tudorache I, Kühn C, Marsch G, Hartung D, Wiesner O, Boenisch O, Haverich A, Hinrichs J (2014) Extracorporeal membrane oxygenation watershed. Circulation 130(10):864–865. https://doi.org/10.1161/CIRCULATIONAHA.114.011677
Sakamoto T, Morimura N, Nagao K, Asai Y, Yokota H, Nara S, Hase M, Tahara Y, Atsumi T, Group S-JS (2014) Extracorporeal cardiopulmonary resuscitation versus conventional cardiopulmonary resuscitation in adults with out-of-hospital cardiac arrest: a prospective observational study. Resuscitation 85(6):762–768. https://doi.org/10.1016/j.resuscitation.2014.01.031
Bongert M, Gehron J, Geller M, Böning A, Grieshaber P (2019) Cannula position and Bernoulli effect contribute to leg malperfusion during extracorporeal life support with femoral arterial cannulation—an in silico simulation study. Interact Cardiovasc Thorac Surg 29(2):312–319. https://doi.org/10.1093/icvts/ivz048
Lehle K, Philipp A, Müller T, Schettler F, Bein T, Schmid C, Lubnow M (2014) Flow dynamics of different adult ECMO systems: a clinical evaluation. Artif Organs 38(5):391–398. https://doi.org/10.1111/aor.12180
Stephens AF, Wickramarachchi A, Burrell AJ, Bellomo R, Raman J, Gregory SD (2022) The hemodynamics of small arterial return cannulae for venoarterial extracorporeal membrane oxygenation. Artif Organs. https://doi.org/10.1111/aor.14179
Takayama H, Landes E, Truby L, Fujita K, Kirtane AJ, Mongero L, Yuzefpolskaya M, Colombo PC, Jorde UP, Kurlansky PA (2015) Feasibility of smaller arterial cannulas in venoarterial extracorporeal membrane oxygenation. J Thorac Cardiovasc Surg 149(5):1428–1433
Kim J, Cho YH, Sung K, Park TK, Lee GY, Lee JM, Song YB, Hahn J-Y, Choi J-H, Choi S-H (2019) Impact of cannula size on clinical outcomes in peripheral venoarterial extracorporeal membrane oxygenation. ASAIO J 65(6):573–579
Cui Y, Yang F, Hou X (2021) Echocardiographic image of a Cannula in the Inferior Vena Cava after Decannulation of Venoarterial extracorporeal membrane oxygenation. Chest 160(5):e527–e530
Acknowledgements
The authors wish to acknowledge Dr. Tim Joseph for their efforts in acquiring the computed tomography scans which were then used to generate the 3D model of the aorta.
Funding
This work was supported by Monash University. Shaun D Gregory is the recipient of a Fellowship (102062) from the National Heart Foundation of Australia.
Author information
Authors and Affiliations
Contributions
JR and RB proposed the idea of a long arterial cannula that could be positioned close to the arch of the aorta to maximize blood flow to the brain during ECMO; this was based on preliminary unpublished animal work. AW designed the study, developed the CFD model, conducted the CFD simulations and wrote the main draft of the manuscript. AB and MS designed the study and provided valuable clinical input towards the final draft of the manuscript. AS, MS, AV and MK aided in the interpretation of the data and provided vital contributions to the drafting of the manuscript. AV and MK also provided assistance with CFD modelling. JR and RB provided valuable clinical input and contributed towards the final draft of the manuscript contents. SG designed the study, aided in the interpretation of data and contributed towards the final draft of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval and consent to participate
Anonymized patient imaging and demographic data was used in this article in accordance with ethics approval from The Alfred Ethics Committee. Therefore, informed consent was not required.
Consent for publication
This manuscript has been approved for publication for this journal by all authors. Informed consent was not required from the patient as their imaging and demographic data was used in accordance with ethics approval from The Alfred Ethics Committee.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
13246_2022_1203_MOESM2_ESM.docx
Additional File 2: Description of the Windkessel outlet boundary condition and the respective resistance and compliance parameters for each aortic branch. Supplementary file2 (DOCX 34 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wickramarachchi, A., Burrell, A.J.C., Stephens, A.F. et al. The effect of arterial cannula tip position on differential hypoxemia during venoarterial extracorporeal membrane oxygenation. Phys Eng Sci Med 46, 119–129 (2023). https://doi.org/10.1007/s13246-022-01203-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13246-022-01203-6