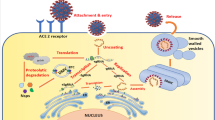
Abstract
Respiratory infections are quite challenging due to their complexity in ailments and composition of viral genetic material and their rate of proliferation. In particular, the eradication of viral illness is still a concern, irrespective of advancements in prevention and remedial procedures. The nature of the viral particle with the possibility of rapid transmission is prone to attach on the deposited surface for days together. This antigen expulses due to sneezing or coughing resulted in multiphase turbulent flow, contaminates the surroundings and is carried away by simple touch or inhalation and find newer hosts for instance, SARSCoV-2 aerosols remain viable for about an hour leading to infection. The present review focuses on the remedial aspects of respiratory infections through a knowledge-based approach towards nanosystems. The complete understanding of standard antiviral drugs and the remodelling of these drugs through nanosystems still is the need of the hour. The genetic material and epidemiology of viral antigen, help in redefining standard drugs along with nanocarriers to achieve more feasible and hour-based approach. The main goal of this review is to elaborate on the repurposing of existing standard antiviral drugs and ways to accelerate their mode of action to promote a feasible and hour-based approach. The consolidated three-dimensional approaches aimed at sustained, targeted and optimized levels of drug concentration in the circulating system along with bioactive nanocarriers which could effectively pass the cell membrane were reported. The platforms for nanomaterial evolution depend on nature of source, size, structure, and their unique functionalities (Stable, speedy, and long-lasting recovery procedure). However, the research activities and literature on coronavirus have been overwhelming but the information on the sustainability of nanotherapy in SARS-CoV-2 is still in the developmental stage. Hereby, the clinical aspects of SARS-CoV-2 and the eradication strategy developed for antiviral infections through nanotechnology will pave the way ahead for treating upcoming new variants or other pandemics.




Similar content being viewed by others
References
Agrawal G (2021) On pins and needles: tracking COVID-19 vaccines and therapeutics
Baas J, Senninger N, Elser H (1994) Das retikuloendotheliale System. Eine Ubersicht über Funktion, Pathologie und neuere Messmethoden [The reticuloendothelial system. An overview of function, pathology and recent methods of measurement]. Zeitschrift fur Gastroenterologie 32(2):117–123
Banerjee A, Qi J, Gogoi R, Wong J, Mitragotri S (2016) Role of nanoparticle size, shape and surface chemistry in oral drug delivery. J Control Release 238:176–185. https://doi.org/10.1016/j.jconrel.2016.07.051
Barbaro G, Scozzafava A, Mastrolorenzo A, Supuran CT (2005) Highly active antiretroviral therapy: current state of the art, new agents and their pharmacological interactions useful for improving therapeutic outcome. Curr Pharm Des 11(14):1805–43
Bharti C, Nagaich U, Pal AK, Gulati N (2015) Mesoporous silica nanoparticles in target drug delivery system: a review. Int J Pharma Investig 5(3):124–133. https://doi.org/10.4103/2230-973X.160844
Bolhassani A (2023) Lipid-based delivery systems in development of genetic and subunit vaccines. Mol Biotechnol 65(5):669–698. https://doi.org/10.1007/s12033-022-00624-8
Chenthamara D, Subramaniam S, Ramakrishnan SG, Krishnaswamy S, Essa MM, Lin FH, Qoronfleh MW (2019) Therapeutic efficacy of nanoparticles and routes of administration. Biomater Res 23:20. https://doi.org/10.1186/s40824-019-0166-x
Cortegiani A, Ingoglia G, Ippolito M, Giarratano A, Einav S (2020) A systematic review on the efficacy and safety of chloroquine for the treatment of COVID-19. J Crit Care 57:279–83
Courrier HM, Butz N, Vandamme TF (2002) Pulmonary drug delivery systems: recent developments and prospects. Crit Rev Ther Drug Carrier Syst 19(4–5):425–498. https://doi.org/10.1615/critrevtherdrugcarriersyst.v19.i45.40
Davis ME, Chen Z, Shin DM (2008) Nanoparticle therapeutics: an emerging treatment modality for cancer. Nat Rev Drug Discovery 7(9):771–782
Desai AD, Lavelle M, Boursiquot BC, Wan EY (2022) Long-term complications of COVID-19. Am J Physiol Cell Physiol 322(1):C1–C11. https://doi.org/10.1152/ajpcell.00375.2021
Diebold SS, Kursa M, Wagner E, Cotten M, Zenke M (1999) Mannose polyethylenimine conjugates for targeted DNA delivery into dendritic cells. J Biol Chem 274(27):19087–19094. https://doi.org/10.1074/jbc.274.27.19087
Drożdżal S, Rosik J, Lechowicz K, Machaj F, Kotfis K, Ghavami S, Łos MJ (2020) FDA approved drugs with pharmacotherapeutic potential for SARS-CoV-2 (COVID-19) therapy. Drug Resist Updat 53:100719. https://doi.org/10.1016/j.drup.2020.100719
Fang E, Liu X, Li M, Zhang Z, Song L, Zhu B, Wu X, Liu J, Zhao D, Li Y (2022) Advances in COVID-19 mRNA vaccine development. Sig Transduct Target Ther 7(1):94. https://doi.org/10.1038/s41392-022-00950-y
Gautret P, Lagier JC, Parola P, Meddeb L, Sevestre J, Mailhe M, Doudier B, Aubry C, Amrane S, Seng P, Hocquart M (2020) Clinical and microbiological effect of a combination of hydroxychloroquine and azithromycin in 80 COVID-19 patients with at least a six-day follow up: a pilot observational study. Travel Med Infect Dis 34:101663
Grenha A, Seijo B, Remunán-López C (2005) Microencapsulated chitosan nanoparticles for lung protein delivery. Eur J Pharm Sci 25(4–5):427–37
Grove J, Marsh M (2011) Host-pathogen interactions: the cell biology of receptor-mediated virus entry. J Cell Biol 195(7):1071–1082
Gunathilake TMSU, Ching YC, Uyama H, Chuah CH (2021) Nanotherapeutics for treating coronavirus diseases. J Drug Deliv Sci Technol 64:102634. https://doi.org/10.1016/j.jddst.2021.102634
Haasnoot J, Westerhout EM, Berkhout B (2007) RNA interference against viruses: strike and counterstrike. Nat Biotechnol 25(12):1435–43
Han J, Zhao D, Li D, Wang X, Jin Z, Zhao K (2018) Polymer-based nanomaterials and applications for vaccines and drugs. Polymers 10:31. https://doi.org/10.3390/polym10010031
Ioerger TR, O’Malley T, Liao R, Guinn KM, Hickey MJ, Mohaideen N, Murphy KC, Boshoff HIM, Mizrahi V, Rubin EJ, Sassetti CM, Barry CE, Sherman DR, Parish T, Sacchettini JC (2013) Identification of new drug targets and resistance mechanisms in mycobacterium tuberculosis. PLoS One 8:1–13. https://doi.org/10.1371/journal.pone.0075245
Jain AK, Khar RK, Ahmed FJ, Diwan PV (2008) Effective insulin delivery using starch nanoparticles as a potential trans-nasal mucoadhesive carrier. Eur J Pharm Biopharm 69(2):426–35
Kamal MA, Jusko WJ (2004) Interactions of prednisolone and other immunosuppressants used in dual treatment of systemic lupus erythematosus in lymphocyte proliferation assays. J Clin Pharmacol 44(9):1034–1045
Kamaly N, Yameen B, Wu J, Farokhzad OC (2016) Degradable controlled-release polymers and polymeric nanoparticles: mechanisms of controlling drug release. Chem Rev 116(4):2602–2663. https://doi.org/10.1021/acs.chemrev.5b00346
Kumar V, Sharma N, Maitra SS (2017) In vitro and in vivo toxicity assessment of nanoparticles. Int Nano Lett 7:243–256. https://doi.org/10.1007/s40089-017-0221-3
Kumar Malik D, Baboota S, Ahuja A, Hasan S, Ali J (2007) Recent advances in protein and peptide drug delivery systems. Curr Drug Deliv 4(2):141–51
Lawrence MJ, Rees GD (2000) Microemulsion-based media as novel drug delivery systems. Adv Drug Deliv Rev 45(1):89–121. https://doi.org/10.1016/s0169-409x(00)00103-4
Ledford H (2020) Chloroquine hype derails coronavirus drug trials. Nature 580(7805):573
Ledford H (2020b) Coronavirus breakthrough: dexamethasone is first drug shown to save lives. Nature 582(7813):469. https://doi.org/10.1038/d41586-020-01824-5
Lembo D, Cavalli R (2010) Nanoparticulate delivery systems for antiviral drugs. Antivir Chem Chemother 21(2):53–70
Li ZZ, Wen LX, Shao L, Chen JF (2004) Fabrication of porous hollow silica nanoparticles and their applications in drug release control. J Control Release 98(2):245–254. https://doi.org/10.1016/j.jconrel.2004.04.019
Li L, Li R, Wu Z, Yang X, Zhao M, Liu J, Chen D (2020) Therapeutic strategies for critically ill patients with COVID-19. Ann Intensive Care 10:1–9
Li J, Zhang K, Wu D, Ren L, Chu X, Qin C, Han X, Hang T, Xu Y, Yang L, Yin L (2021) Liposomal remdesivir inhalation solution for targeted lung delivery as a novel therapeutic approach for COVID-19. Asian J Pharm Sci 16(6):772–783. https://doi.org/10.1016/j.ajps.2021.09.002
Liu J, Liao X, Qian S et al (2020) Community transmission of severe acute respiratory syndrome coronavirus 2, Shenzhen China. Emerg Infect Dis 26(6):1320. https://doi.org/10.3201/eid2606.200239
Lu R, Zhao X, Li J, Niu P, Yang B, Wu H, Wang W, Song H, Huang B, Zhu N, Bi Y (2020) Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. The lancet 395(10224):565–74
Lythgoe MP, Middleton P (2020) Ongoing clinical trials for the management of the COVID-19 pandemic. Trends Pharmacol Sci 41(6):363–382
Maideen NM (2021) Therapeutic efficacy of kabasura kudineer (siddha formulation), in covid-19–a review of clinical and molecular docking studies. Asian J Adv Res 14:817–824
Malmsten M (2006) Soft drug delivery systems. Soft Matter 2(9):760–769
Mamo T, Moseman EA, Kolishetti N, Salvador-Morales C, Shi J, Kuritzkes DR, Langer R, von Andrian U, Farokhzad OC (2010) Emerging nanotechnology approaches for HIV/AIDS treatment and prevention. Nanomedicine (Lond) 5(2):269–85. https://doi.org/10.2217/nnm.10.1
Maus A, Strait L, Zhu D (2021) Nanoparticles as delivery vehicles for antiviral therapeutic drugs. Eng Regen 2:31–46. https://doi.org/10.1016/j.engreg.2021.03.001
Meuleman P, Catanese MT, Verhoye L, Desombere I, Farhoudi A, Jones CT, Sheahan T, Grzyb K, Cortese R, Rice CM, Leroux-Roels G (2012) A human monoclonal antibody targeting scavenger receptor class B type I precludes hepatitis C virus infection and viral spreadin vitroandin vivo. Hepatology 55(2):364–372
Milovanovic M, Arsenijevic A, Milovanovic J, Kanjevac T, Arsenijevic N (2017) Nanoparticles in antiviral therapy. Antimicrobial nanoarchitectonics. Elsevier, Amsterdam, pp 383–410
Mitchell MJ, Billingsley MM, Haley RM et al (2021) Engineering precision nanoparticles for drug delivery. Nat Rev Drug Discov 20:101–124. https://doi.org/10.1038/s41573-020-0090-8
Modrow S, Falke D, Truyen U, Schätzl H (2013) Viruses with single-stranded, positive-sense RNA genomes. Mol Virol 12:185
Molina JM, Delaugerre C, Le Goff J, Mela-Lima B, Ponscarme D, Goldwirt L, de Castro N (2020) No evidence of rapid antiviral clearance or clinical benefit with the combination of hydroxychloroquine and azithromycin in patients with severe COVID-19 infection. Medecine et Maladies Infectieuses 50(4):384
Müller RH, Mäder K, Gohla S (2000) Solid lipid nanoparticles (SLN) for controlled drug delivery - a review of the state of the art. Eur J Pharm Biopharm 50(1):161–177. https://doi.org/10.1016/s0939-6411(00)00087-4
Natarajan S, Anbarasi C, Sathiyarajeswaran P, Manickam P, Geetha S, Kathiravan R, Prathiba P, Pitchiahkumar M, Parthiban P, Kanakavalli K, Balaji P (2021) Kabasura Kudineer (KSK), a poly-herbal Siddha medicine, reduced SARS-CoV-2 viral load in asymptomatic COVID-19 individuals as compared to vitamin C and zinc supplementation: findings from a prospective, exploratory, open-labeled, comparative, randomized controlled trial, Tamil Nadu, India. Trials 22(1):1–1
Pang J (2015) Fabrication of mesoporous silica nanospheres with radially oriented meso channels by microemulsion templating for adsorption and controlled release of aspirin. RSC Adv 5(9):6599–6606
Panyam J, Labhasetwar V (2003) Biodegradable nanoparticles for drug and gene delivery to cells and tissue. Adv Drug Deliv Rev 55(3):329–347. https://doi.org/10.1016/s0169-409x(02)00228-4
Patil YB, Toti US, Khdair A, Ma L, Panyam J (2009) Single-step surface functionalization of polymeric nanoparticles for targeted drug delivery. Biomaterials 30(5):859–866. https://doi.org/10.1016/j.biomaterials.2008.09.05635
Patra JK, Das G, Fraceto LF, Campos EV, Rodriguez-Torres MD, Acosta-Torres LS, Diaz-Torres LA, Grillo R, Swamy MK, Sharma S, Habtemariam S (2018) Nano based drug delivery systems: recent developments and future prospects. J Nanobiotechnol 16(1):1–33
Sarkar I, Garg R, van Littel-van den Hurk S (2019) Selection of adjuvants for vaccines targeting specific pathogens. Expert Rev Vaccines 18(5):505–521. https://doi.org/10.1080/14760584.2019.1604231
Schwendener RA (2014) Liposomes as vaccine delivery systems: a review of the recent advances. Ther Adv Vaccines 2(6):159–182. https://doi.org/10.1177/2051013614541440
Seminara G, Carli B, Forni G et al (2020) Biological fluid dynamics of airborne COVID-19 infection. Rend Fis Acc Lincei 31:505–537. https://doi.org/10.1007/s12210-020-00938-2
Sharma N, Ojha H, Bharadwaj A, Pathak DP, Sharma RK (2015) Preparation and catalytic applications of nanomaterials: a review. RSC Adv 5:53381–53403
Sharma T, Gerstman B, Chapagain P (2023) Distinctive features of the XBB.1.5 and XBB.1.16 spike protein receptor-binding domains and their roles in conformational changes and angiotensin-converting enzyme 2 binding. Int J Mol Sci 24(16):12586. https://doi.org/10.3390/ijms241612586
Shi L, Plumley CJ, Berkland C (2007) Biodegradable nanoparticle flocculates for dry powder aerosol formulation. Langmuir 23(22):10897–901
Shi L, Plumley CJ, Berkland C (2007b) Biodegradable nanoparticle flocculates for dry powder aerosol formulation. Langmuir 23(22):10897–10901. https://doi.org/10.1021/la7020098
Singh L, Kruger HG, Maguire GEM, Govender T, Parboosing R (2017) The role of nanotechnology in the treatment of viral infections. Ther Adv Infect Dis 4(4):105–131. https://doi.org/10.1177/2049936117713593
Song SW, Hidajat K, Kawi S (2005) Functionalized SBA-15 materials as carriers for controlled drug delivery: influence of surface properties on matrix-drug interactions. Langmuir 21(21):9568–75. https://doi.org/10.1021/la051167e
Teixeira MZ (2020) Clinical research protocol to evaluate the effectiveness and safety of individualized homeopathic medicine in the treatment and prevention of the COVID-19 epidemic. Rev Assoc Med Bras 66(4):405–406. https://doi.org/10.1590/1806-9282.66.4.405
Teixeira MZ (2021) Homeopathy: a preventive approach to medicine? Int J High Dilution Res 8(29):155–172. https://doi.org/10.51910/ijhdr.v8i29.36015
Wang M, Cao R, Zhang L, Yang X, Liu J, Xu M, Shi Z, Hu Z, Zhong W, Xiao G (2020) Remdesivir and chloroquine effectively inhibit the recently emerged novel coronavirus (2019-nCoV) in vitro. Cell Res 30(3):269–271
Wilson B, Geetha KM (2022) Lipid nanoparticles in the development of mRNA vaccines for COVID-19. J Drug Deliv Sci Technol 74:103553. https://doi.org/10.1016/j.jddst.2022.103553
World Health Organization (2014) Infection prevention and control of epidemic- and pandemic-prone acute respiratory infections in health care. Geneva: World Health Organization; https://apps.who.int/iris/bitstream/handle/10665/112656/9789241507134_eng.pdf?sequence=1
World Health Organization (2023) COVID-19 weekly epidemiological update, edition 158, 29 September 2023. World Health Organization
Wu R, Wang L, Kuo HD, Shannar A, Peter R, Chou PJ, Li S, Hudlikar R, Liu X, Liu Z, Poiani GJ, Amorosa L, Brunetti L, Kong AN (2020) An update on current therapeutic drugs treating COVID-19. Curr Pharmacol Rep 6(3):56–70. https://doi.org/10.1007/s40495-020-00216-7
Xue Y, Liu C, Andrews G, Wang J, Ge Y (2022) Recent advances in carbon quantum dots for virus detection, as well as inhibition and treatment of viral infection. Nano Converg 9(1):15. https://doi.org/10.1186/s40580-022-00307-9
Yang SNY, Atkinson SC, Wang C, Lee A, Bogoyevitch MA, Borg NA, Jans DA (2020) The broad spectrum antiviral ivermectin targets the host nuclear transport importin α/β1 heterodimer. Antiviral Res 177:104760. https://doi.org/10.1016/j.antiviral.2020.104760
Yao X, Ye F, Zhang M, Cui C, Huang B, Niu P, Liu X, Zhao L, Dong E, Song C, Zhan S (2020) In vitro antiviral activity and projection of optimized dosing design of hydroxychloroquine for the treatment of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Clin Infect Dis 71(15):732–9
Yarlagadda H, Patel MA, Gupta V, Bansal T, Upadhyay S, Shaheen N, Jain R (2022) COVID-19 vaccine challenges in developing and developed countries. Cureus 14(4):e23951. https://doi.org/10.7759/cureus.23951
Yoo J, Park C, Yi G, Lee D, Koo H (2019) Active targeting strategies using biological ligands for nanoparticle drug delivery systems. Cancers 11(5):640
Zhang L, Gu FX, Chan JM, Wang AZ, Langer RS, Farokhzad OC (2008) Nanoparticles in medicine: therapeutic applications and developments. Clin Pharmacol Ther 83(5):761–769. https://doi.org/10.1038/sj.clpt.6100400. (Epub 2007 Oct 24 PMID: 17957183)
Acknowledgements
Dr NU and Dr NS acknowledge the support of the Director, ICMR-National Institute for Research in Tuberculosis, and the approval from ICMR. Dr NU and Dr SVK acknowledge Director, CSIR-Central Leather Research Institute. A/2021/CHR/NWP100/1514 is the communication number obtained from CLRI.
Author information
Authors and Affiliations
Contributions
All authors contributed to the work and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing financial interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Usharani, N., Kanth, S.V. & Saravanan, N. Biomimetic nanomaterials for pulmonary infections: A prospective view in drug delivery systems. Appl Nanosci 14, 363–373 (2024). https://doi.org/10.1007/s13204-023-02981-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13204-023-02981-5