Abstract
The worldwide emerging cases of various respiratory viral diseases and the current escalation of novel coronavirus disease (COVID‐19) make people considerably attentive to controlling these viruses through innovative methods. Most re-emerging respiratory diseases envelop RNA viruses that employ attachment between the virus and host cell to get an entry form using the host cell machinery. Emerging variants of COVD-19 also bring about a constant threat to public health as it has wide infectivity and can quickly spread to infect humans. This review focuses on insights into the current investigations to prevent the progression of incipient variants of Severe Acute Respiratory Syndrome Coronavirus (SARS-COV-2) along with similar enveloped RNA viruses that cause respiratory illness in humans and animals. Nanotheranostics is a trailblazing arena of nanomedicine that simultaneously helps prevent or treat diseases and diagnoses. Nanoparticle coating and nanofibers were extensively explored, preventing viral contaminations. Several studies have proven the virucidal activities of metal nanoparticles like copper, silver, and titanium against respiratory viral pathogens. Worldwide many researchers have shown surfaces coated with ionic nanoparticles like zinc or titanium act as potent antiviral agents against RNA viruses. Carbon nanotubes, quantum dots, silica nanoparticles (NPs), polymeric and metallic nanoparticles have also been explored in the field of nanotheranostics in viral detection. In this review, we have comprehensively discussed different types of metallic, ionic, organic nanoparticles and their hybrids showing substantial antiviral properties to stop the progression of the novel coronavirus disease focused on three key classes: prevention, diagnostics, and treatment.
Similar content being viewed by others
Introduction
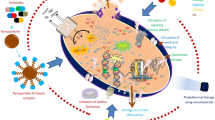
Enveloped viruses invade human cells by amalgamating cell membranes to make several copies of them. Worldwide different classes of coronaviruses, including the Middle East Respiratory Syndrome Coronavirus (MERS-CoV), Infectious Bronchitis Virus (IBV), and Severe Acute Respiratory Syndrome Coronavirus (SARS-COV) are attached at the cellular membrane or enters into the cell using tissue-specific receptor-mediated endocytosis and merged with endosomes [1]. To investigate the viral infectivity and the pathogenicity for identifying therapeutic targets, extensive studies were organized during the SARS-COV outbreak in 2003 and the MERS-CoV outbreak in 2012. Several studies determined that Abl kinase inhibitors can inhibit the virucidal activity of SARS-COV and MERS-CoV [2]. Abl kinases are located in the cytoplasm, a non-receptor tyrosine kinase [3, 4]. The spike (S) protein of the virus promotes host cell attachment. The coronavirus-induced disease 2019 or COVID-19 is caused by a new β‐coronavirus, named Severe Acute Respiratory Syndrome Coronavirus 2 (SARS‐COV‐2) [4]. It emerged in Wuhan, China, in December 2019. It has the most prominent known positive-sense single-strand RNA genome of 30–32 Kilobases. The disease has symptoms like high fever, dry cough, influenza-like illness, myalgia, lung infiltrates, and which ultimately lead to acute respiratory illness [5]. Coronavirus infection kicks off with viral attachment after recognizing the host cell-specific angiotensin-converting enzyme inhibitor receptor (ACE-2), fuses its cell membrane [6], and finishes off by egression from the host. Nucleocapsid (N), envelope (E), membrane (M), and spike (S) proteins are the four main structural proteins of the virus. Receptor-binding domain (RBD) of the S protein interacted with ACE-2 on the host cell membrane; the binding of RBD of S protein and ACE-2 brings about structural conformation on S protein (Fig. 1). In addition to SARS‐COV‐2, in the past 100 years, pandemics like SARS, H1N1 (1918), H2N2 (1956 − 1958) and H3N3 flu (1968), HIV (2005–2012), swine flu (2009) has occurred, so we can’t disavow the need of identifying novel and highly effective antivirals to combat with the different viruses [7, 8]. The worst was in 1918, which has taken way 40 million lives [9]. Since the commencement of the COVID-19 pandemic, multiple new variants of concern have appeared, associated with boosted transmissibility and enhanced virulence. Based on the epidemiological data provided by the WHO, of December 11th, 2021, since the onset of the pandemic, five new SARS-COV-2 variants have been identified as Variant of Concern (VOC). The first variant of concern was Alpha (B.1.1.7) in the United Kingdom (UK) in late December 2020. Then Beta (B.1.351) variant was reported in South Africa in December 2020, and Delta (B.1.617.2) was reported in India in December 2020 with the second wave of infection surge. In India, the delta lineage and Bengal variant (B.1.618.1) were mainly caused by a catastrophic condition in May 2021, resulting in over 400,000 daily infections [10]. Last year, Gamma (P.1) variant was reported in Brazil in early January, and finally, Omicron (B.1.1.529) was identified in South Africa in November with the third-wave surge. Though the Omicron variant has shown the highest transmissibility, it causes mild to moderate symptoms with low mortality. Recently the WHO has announced a new cautionary concerning a novel mutant variant of Omicron named XE. Concern has been raised over the rapid transmissibility, making it extraordinarily spreadable and might cause a new high-risk Covid wave. Effective infection control measures are essential to prevent these severe outbreaks because the loss of host protective immunity against such viruses and the outrageous pathogenicity of such strains continue to threaten lives. A previous study shows that SARS-COV-2 can remain infective on steel or plastic surfaces for 72 h; thus, it poses a significant challenge for infection control in hospitals and households, and food production facilities [11]. To be precise biomedical agents can block these potent pandemic viruses from spreading, alleviate patient conditions, or disinfect surfaces that are highly sought after. Along with disease prevention, early diagnosis can also reduce cross-contamination. Recently, many novel theranostic techniques have emerged to diagnose, prevent, and treat viral diseases. Nanotheranostics has evolved as the most capable nanotechnological application in the biomedical field in consequence of its antiviral efficacy. To prevent, diagnose and treat COVID-19 disease, nanotechnology plays a decisive role in mitigating infections [12]. On the whole, metal nanoparticles have less than one micrometer and have a higher surface area than their volume [13]. Nanoparticles have some unique features, including multifunctionality and enhanced solubility, efficiency for drug delivery, and interaction capturing molecules with the target analyte; they are ideal for sensor application [14]. Henceforth, recent nanomaterials studies have played a vital role in managing the current pandemic and combating the upcoming outbreak. The advancement of nanotechnology helps to streamline the sample collection, processing, and detection of viral pathogen and disease-specific antigens through the different implications of microchip-based unified sensing platforms and nanoparticles [15] In the arena of theranostics, nanotechnology proposed a ground-breaking solution, where a limited dosage of nanoparticles can selectively diagnose and kill the microorganisms [16].
Nanoparticle-Based Application in Infection Prevention
Metallic and Non-Metallic Nanocoating Preventing Viral Contamination
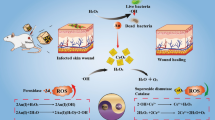
There are constant endeavors from the scientific community in response to this pandemic to develop some measures to reduce the chance of viral infection. A large surface area of the microporous structure of zeolites instigates a robust antiviral activity by an effective viral attachment with the Cu2+ on the zeolites assimilated in the cotton fibers. The synthesis of viral proteins from viral mRNA and virus assembly was eventually disrupted (Fig. 2a) [17]. Silver also has shown efficient antiviral activities. Against the influenza-A virus, the effect of silver hybrid coating implemented a reduction in virulence [18]. Silver nanoparticles achieved an antiviral impact at a high concentration against influenza-A (Fig. 2b). Blockage of the sialic acid receptor on the host cell surface can be done by functionalized gold nanoparticles. Sialic acid eventually eliminates glycerol dendron and thus blocks the fusion step of influenza [19]. There is also a report from a previous study that zinc can inhibit human rhinovirus by inhibiting the cleavage of viral polypeptides. Zinc interacts with HRV-1A capsid proteins, blocking the conversion of precursors & rapidly preventing the maturation of viral RNA capsid polypeptides (Fig. 2c). The zinc chloride had shown a 99% reduction in the number of plaques in plaque assay used after virus exposure [20]. Several transition materials like manganese and magnesium have shown evidence to wipe out the viral population when loaded into a light-induced photo-catalyst like TiO2 (Fig. 2d). This photo-catalyst is used to coat paint for antistatic application, and it can also minimize viral transmission via surface disinfection and aerosol [21]. Botequim et al. also reported immobilized SNP-DDAB (silica nanoparticle di-dodecyl dimethylammonium bromide) formulations on top of a substrate attached by a chemical adhesive pursue a long-term antiviral activity against influenza A without leaching. This antiviral activity is mediated by surface contact and can use as an antiviral coating [22]. Water-soluble metal ion, aluminium, copper, and mixtures showed an excellent antiviral effect, formulated in a tissue paper patented by Kelly et al. Due to the worldwide focus on using metal NPs (nanoparticles) as antiviral, many compounds have been developed that are effective against clinical isolate and pathogenic surrogates. Metallic nanoparticles have also shown a main antiviral activity against respiratory viruses like RSV and influenza [23, 24]. Besides some ionic compounds, several metallic compounds also showed practical virucidal activities. Copper in a solid-state or oxide state damages the genome of negative-sense RNA viruses [24]. Copper also can reduce the action of the hemagglutinin protein of Influenza A by structural deformation. Cu2O can also destroy protein structures by cleavage S-S bonds by employing a distortion of hydrogen binding latticework or ionic interactions in protein surfaces or by decreasing the thiol concentration [25]. Warnes et al. showed coronavirus 229E is inactivated in copper alloy and Cu/Zn brasses [26]. A previous study inferred that Cu2+ accessibility in a cell could be a limiting factor for viral viability as Cu2+ acts as a cofactor in viral, many viral proteins [27]. Copper has potent virucidal and bactericidal activity against various spectrums of the pathogen (Fig. 2a). The virucidal activity of copper is rendered by oxidative damage of various biomolecules, crosslinking with the nucleic acids of the virus. Free Cu can break down different cellular components generating Reactive Oxygen Species (ROS) through redox reactions. Copper alloys have been shown to inactivate enveloped viruses faster than non-enveloped viruses, probably by generating ROS on the outer alloy surface [26]. Several studies have exhibited the role of solid copper in inactivating novel coronavirus. In another study, after 2 hours under copper-coated surfaces, a significant drop (99%) of viral titter was observed [28]. Some studies have shown that the presence of ascorbic acid copper generates hydroxyl radicals and deactivates the virus [29]. Copper powder spray can kill viruses by disrupting lipid capsid and contact-killing due to its rough surface [30]. Applying metal NPs in personal protective equipment (PPE) can make a difference in stopping the transmission of the virus. The antiviral effect of silver nanoparticles was also evident by the destruction of surface proteins of the viral capsid composed of cysteine and methionine residues (Fig. 2b) [31]. Solid-state coating and Ag-doped solid-state coating of TiO2 manifest virucidal activity by photocatalysis. That TiO2 introduced ROS production through photo-stimulated redox reactions on the metal surface. The production of ROS induced virucidal activity by destroying organic compounds with strong oxidative activity. The photocatalysis may influence virucidal activity by changing the phospholipid content. Photocatalysis reaction damages the constituent proteins before degradation of nucleic acid, which eventually results in decreased infectability [31]. TiO2-coated Ag-doped solid-state releases silver ions into the aqueous environment, triggering the Inactivation of respiratory enzymes, interrupting electron transport, and altering the permeability of the viral membranes, causing cell death (Fig. 2c) [32]. However, these chemical entities could be used as disinfectants that can be much better than metallic compounds as nanoparticles release ions and aggregates, guiding to a magnification of the antiviral activity (Table 1).
Mechanisms of virucidal activity of some metallic & ionic particles schematic representation. a Antiviral activity of copper in both metallic & ionic form. Contact killing, genomic degradation by respiratory burst & destruction of viral proteins. b Destruction of viral lipid membrane & blocking of the sialic acid receptor by silver nanoparticles. c Zinc ions block membrane attachment as well as inhibit RNA-dependent RNA polymerase (RdRp), Reverse Transcriptase (RT), and DNA-dependent DNA polymerase (DdDp). d Titanium oxides show antiviral activity by both membrane dissociation and damaging genetic materials by ROS production after photocatalysis
Organic–Inorganic Nanocomposites Contending Viral Infection
Nanofibers fabricated by organic-inorganic nanocomposites provide an immense surface area that delays the efficiency of viral entry and attachment [33, 34]. It has a minute size, minimal weight, improved permeability, and outstanding interconnectivity [31]. The development of a Chitin-nanofiber sheet fabricated with silver nanoparticles (AgNPs) shows a 2-log decrease of negative-sense RNA virus particles at a 8.5 μL/cm concentration of AgNPs [35]. Chen et al. showed that Graphene-silver nanocomposites inhibited 24.8% of infectiveness by 4.7 × 104 TCID50/mL (Tissue Culture Infectious Dose 50%/mL) of feline coronavirus at a concentration of 0.1 mg/mL [36]. Based on an earlier study in 2007 [37], researchers showed the virucidal action of bismuth composites against SARS-COV. A recent survey by yuan et al. revealed that ranitidine bismuth citrate (RBC) application in human and animal cell lines manifested potent inhibitions of SARS-COV-2 replication by interfering with viral helicase activity [38]. The lethal effect of these polycations shown by Halder et al. achieved 100% virucidal activity against human and avian influenza in surfaces fabricated with N,N-dodecyl, methyl-polyethyleneimine, despite having oseltamivir-resistant [39]. N,N-dodecyl, methyl-polyurethane (Quat-12-PU) nanoparticle spoiling the viral envelope to breach the protection to RNA after being treated by spray coating on glass backbone [40]. Functionalizing the nanofibers with nucleating agents such as ß-cyclodextrin and o-iodosobenzoic acid decline the chance of breath in viral pathogens by neutralizing the contaminants [32]. Electrospinning is the standard method of synthesizing nanofiber-based material using electrical charge, enhancing its capability of capturing target particles [41,42,43]. Surface functionalized viral nanoparticles also have shown good preventative action against SARS-COV-2 through vaccine development [44, 45]
Nanotechnology-Dependent Viral Diagnosis
COVID-19 infection spreading can be constrained via early isolation and identification through disease detection and diagnosis. Irrespective of challenges in sensitive and quick diagnosis, some COVID detection techniques have been introduced. SARS-COV-2 infection can be detected through molecular diagnostic tests by targeting viral nucleic acids, having greater precision than radiographic imaging techniques. Viral infection can also be detected by targeting serological markers, i.e., immunoglobulin, against the specific viral antigen [46, 47]. Antigen and nucleic acid-based diagnostics systems are exceedingly reliant on the proteomics and genomics of viruses or variation in the genetic expression of host-specific inflammatory markers (Table 2).
Metal-Based Nanodiagnostics
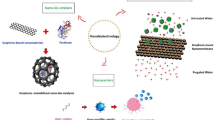
In the field of rapid diagnostics, some recent studies have reported gold nanoparticles (AuNPs) as one of the most frequently used nanomaterials [48]. Researchers have shown gold nanoparticles as a nanodiagnostic tool for detecting viral double-stranded DNA (dsDNA). The AuNP decorated with citrate ions can directly interact with single-stranded DNA (ssDNA) or ssRNA. This interaction between dsDNA of SARS-COV and AuNP can be detected by changing the color of the solution by salt addition through a simple colorimetric hybridization assay [49]. In another study, green fluorescent protein conjugated AuNPs have shown changes in absorbance interacting with specific complementary antibodies [50]. Another group has developed an AuNP-dependent electrochemical hybridization-based gene-sensor (Fig. 3b). This sensing system was designed to detect target viral DNA through hybridizing its biotinylated form with the AuNPs-based electrode decorated with the immobilized probe of thiolated-DNA. Researchers also developed Au-binding polypeptides, a strategy for restraining the target proteins on the exterior of AuNP. Using this strategy, a protein cocktail can be composed of streptavidin as core model proteins, surrounded by green fluorescent protein, and SARS-COV-E protein immobilized on AuNP. These protein compositions intermingle with the serum antibody, resulting in a change in absorbance, effectively diagnosing COVID-19 [51]. Zhao et al. reported the RNA isolation methods by synthesizing magnetic nanoparticles (pcMNPs) coated with poly amino ester with carboxyl groups (PC). Combining the lysis and binding phases, this extraction technique becomes time-efficient and user-friendly. Moreover, for performing the succeeding RT-PCR, this complex of pcMNPs-RNA can be fused directly into the reaction. With an identification limit of 10 copies of SARS-COV-2 viral particles, this detection system targeted the ORFlab and N region of viral RNA [52]. Based on Zhao et al. synthesis method, another group also has been presented with magnetic nanoparticles-based RNA isolation from a nasopharyngeal swab. Primarily, they have coated APTES on the magnetite nanoparticles (MNP) for developing the amino-magnetic nanoparticles complex (NH2-MNP) (Fig. 3a). Eventually, to obtain the Poly (amino-ester), they polymerized the Diacrylate-amine and coated the amino-magnetic nanoparticles (NH2-MNP) with Poly (amino-ester) to form the final product (Poly-NH2-MNP) [53]. Performing real-time RT-PCR tests for COVID-19, about 5000 RNA extraction/purification procedures can be achieved using only 100 mL of Poly-NH2-MNP. Precise detection of nucleic acid needs competent isolation and separation process allowing purification of target viral DNA or RNA. For instance, another study reported complementary probe conjugated superparamagnetic nanoparticles to detect the target sequence of a specific SARS-COV gene. The product of PCR performed by the extracted DNA has been tested using complementary sequence coupled silica-coated nanoparticles, producing fluorescence signals, detecting and calculating the yield of the target cDNA [54]. Somvanshi et al. conveyed the fabrication procedure of the surface-modified MNPs. They synthesized the zinc ferrite through combustion and eventually functionalized the exterior of the nanoparticle with silica and carboxyl-derivative polyvinyl alcohol. This system performed the viral RNA extraction from varied samples to potentially diagnose the COVID-19 disease [55].
Various strategies of nanotechnology-based viral diagnostics; a Schematic of Poly (amino-ester) linked amino-magnetic nanoparticles (NH2-MNP) synthesis through Michael addition methodology, used in viral RNA isolation. Reproduced from an open access journal [53]. b Diagram of detection kit of porcine epidemic diarrhea built on immunochromatographic assay using antibodies developed through AuNPs [50]. c Viral detection strategy using single-walled carbon nanotube (SWCNT)-based optical sensing approach [57]. Copyright © 2021, American Chemical Society
Carbon-Based Nanodiagnostics
Besides other metallic and non-metallic nanoparticles, carbon-based nanomaterials have also been widely used in COVID-specific nanodiagnostics. Different structural morphologies like graphene, carbon nanotubes (CNTs), and carbon nanodots (CNDs) can be used in detecting viral disease. In diagnosing SARS-COV-like respiratory viral diseases, the use of CNT has been reported in various journals. Yeh et al. [56] developed an innovative size-tunable enrichment microdevice (STEM) based on CNT that could augment and isolate viruses. Beside STEM-CNT, another group has prepared an optical sensing platforming based on single wall CNT (SWCNT) for detecting COVID-19 (Fig. 3c). That SWCNT-based nanosensor noncovalently coupled with ACE2 protein, having a high SARS-COV-2 spike protein specific binding affinity, showed improved sensitivity. As a result, the SWCNT has shown a twofold enhanced fluorescence signal in the existence of the target protein [57]. Likewise, another group of researchers has developed nano-printed reduced graphene oxide (rGO) coated 3D electrodes to rapidly detect COVID-19 antibodies [58]. For immobilizing the COVID-19-specific antigens, they have used nanoflakes. The antigen immobilization induced the binding of particular antibodies introduced into the device, deviating the impedance of the circuit. This device can detect target antigen at a limit of 2.8×10−15 M for spike S1 specific antibody and 16.9×10−15M for receptor-binding-domain (RBD) specific antibody [58]. In a different study, a group of researchers developed a chip-based SARS-COV detection kit. This device detects the N protein using Quantum Dot (QD) conjugated RNA aptamer-based system with high sensitivity and specificity [59]. In a nutshell, using fluorescent-based carbon nanoparticles and other carbon nanostructures may support scientists in evolving sensitive diagnostic methods to rapidly detect COVID-19 [60]. Recently researchers also have described the neutralizing mechanism of graphene-based nanocomposites for sensing COVID-19 [61] .
Antiviral Nanotherapeutic Strategies
Metallic Nanotherapeutics Combating Viral Diseases
Antiviral drugs have evolved recently and can be broadly segmentized depending on the mechanism of action, such as attachment and penetration inhibitors, reverse transcriptase inhibitors, DNA polymerase inhibitors, protein inhibitors, and neuraminidase inhibitors. In recent times for the treatment of viral infections, several new nanotherapeutic strategies have evolved (Table 3). Trogolo et al. claimed a combination of silver and copper ions to treat the disease incidental with SARS [15]. Auranofin (AF), a gold (Au) based metallodrug, inhibits the Intracellular viral RNA of SARS-COV-2, which decreased by 95% after 48 hours of administration [62]. AF can interfere with immune response pathways, interfering and blocking interleukin-6 signaling pathways through phosphorylation of JAK1 and STAT3. AF shows a potent inhibitory activity toward the cysteine proteases. AF inhibits potently SARS-COV-2 multiplication while attenuating infection in living human cells [62]. Synthetic virus-like particles (sVLPs) have been synthesized, exploiting the high surface energy of gold nanoparticles incubated with recombinant IBV spike protein as corona-specific model antigens. The avian coronavirus (AvCov) specific globular spike protein projected on the surface of the AuNP core-shell structure mimics the natural viral particles. This nano-formulation can improve the cell-mediated and humoral response against AvCov-IBV (Fig. 4a). The potent immune response of sVLPs against AvCov-IBV is attributed to diversified antigen display, improved antibody titers, and minimal inflammatory responses compared to the free antigens [13]. In the case of silver nanoparticles, different studies had shown the yield of AgNPs to obstruct viral entry. Uniform, spherical, and 15−20 nm silver-modified cerium oxide nanoparticles (AgCNPs) have been characterized and tested for antiviral efficacy. AgCNP reduced infectious human coronavirus OC43 titer to ∼103 TCID50/mL and completely inactivated contagious rhinovirus 14 (RV14) [63]. The infection and replication of transmissible gastroenteritis virus or transmissible gastroenteritis coronavirus (TGEV) can be interfered with by direct contact with Ag nanowires and nanoparticles, disrupting the viral attachment and entry (Fig. 4b) [64]. The Ag nanomaterials have shown virucidal activity through (i) inhibiting host cell apoptosis, increasing expression of p38/mitochondria-caspase-3 signaling proteins; (ii) initiating the inflammatory response interacting with the spike glycoprotein; and (iii) altering the surface protein structure, disrupting its capability to identify and adhere with porcine host-specific aminopeptidase N receptor. A metal nanocomposite, TPNT1, which contains Au-NP, Ag-NP, ZnO-NP, and ClO2 in an aqueous solution, was prepared and evaluated as a potent antiviral nanotherapeutic strategy. TPNT1 inhibits the viral entry by preventing the ACE2 receptor binding of the SARS-COV-2 spike antigen. Furthermore, both wild-type and oseltamivir-resistant human (H1N1) and avian (H5N1) influenza viruses also can be efficiently reduced by the cytopathic properties induced by TPNT1 [65]. Flexible and long entities of undecane sulfonic acid (MUS) treated gold nanoparticles (AuNPs) show virucidal activity counter to the viruses that bind to the heparan sulfate proteoglycan (HSPG). The high forces (~190 pN) generated by the nanoparticles irreversibly distort the virus structure [66].
Nanotherapeutic approaches against different strains of coronaviruses found in animals: a sVLPs-based immunization developed by gold nanoparticles incubated with IBV-specific antigen; b Virucidal activity of silver nanoparticles against infection introduced by TGEV‐induced host cell through disrupting p38‐MAPK signaling activation. Reproduced from an open access journal of Wiley (13) c Therapeutic activity of CQDs functionalized with boronic functions, on attaching to HCoV-229E virus: (i) restrict the interaction with S receptor, and (ii) inhibit the replication of viral RNA. Reproduced from an open-access journal of Wiley (14)
Organic Antiviral Nanotherapeutics
In recent years, organic nanostructures have also been widely used in antiviral nanotherapeutic applications. SARS-COV-2 can be counteracted by human lung epithelial type II cell membrane-derived nanosponges, displaying the stipulation of protein receptors for SARS-COV-2 host cell attachment and entry [67]. Triggering specific immunogenic reaction virus-mimetic nanovesicles can use as antiviral antigens delivery system and mimic the viral property [68]. Researchers also have found nanodecoys composed of gelatin nanoparticles and viral membranes of Zika virus, capturing the virus and disrupting the entry can inhibit the infectivity [69]. Lipid nanoparticles can be used as a transporter of an mRNA vaccine encoding the pre- membrane and envelope (prM- E) against the Zika virus [70]. Ting et al. [71] reported the curcumin-derived cationic carbon dot (CD) exhibiting a virucidal effect against the porcine epidemic diarrhea virus (PEDV). These CDs significantly subdue the viral entry, replication, and negative-strand RNA synthesis. Henceforth, this cationic carbon dot might act as potential therapeutics against other classes of coronaviruses such as SARS-COV-2. Decorating the carbon dot surface with 4-aminophenyl boronic acid and phenylboronic acid groups, Loczechin et al. have shown a tenfold improvement in the virucidal activity of the human coronavirus 229E (HCoV-229E) (Fig. 4c) [72]. The mechanism of action of these functionalized CDs is attributed to the interaction of the boronic acid functions with the S protein of HCoV-229E. A group of researchers has designed remdesivir-loaded PLGA nanoparticles (NPs) containing ACE inhibitor (ACEI) using a combined simulation of molecular docking and dissipative particle dynamics (DPD) for therapeutic application in COVID-19. Lisinopril, a classical ACEI, having a therapeutic and lung protecting activity, can be covalently embedded on top of PLGA (L–PLGA) and has been used to encapsulate remdesivir [73]. Drug nano-conjugates can also be an effective therapeutic option against viral diseases. Scientists have evaluated the antiviral activity of the nano-conjugates of two sitagliptin (SIT) and glatiramer acetate (GA), two FDA-approved drugs countering the SARS-COV-2 virus isolated from a human sample. Using the three-factor bilevel factorial design, SIT-GA nano-conjugates were developed, showing good virucidal activity against SARS-COV-2 with IC50 values of 8.52 μM for SIT-GA nano-conjugates, which is lesser than the individual drugs. Effectively high binding affinity have demonstrated for the COVID 3CL protease through molecular docking [74]. Nanoparticles derived from herbal sources like Azadirachta indica (neem plant) can be act as potential anti-SARS-COV-2 nanoformulation [75].
Conclusion
Though vaccination has successfully reduced the risk of COVID-19, relentless effort of continuous improvement in therapeutic or virucidal agents is persistent till date to efficiently mitigate further the threat of infection to minimize widespread outbreaks. In context of incidence of new variants, scientific community have acknowledged protecting the population by investigating therapeutic and diagnostic methods to be applied soon. Disinfection owing to infection control is a laboursome work in a different setting aiming to find other materials with good adaptability, relative preparatory facility, cost-effectiveness, and broad-spectrum of antimicrobial activity. This systemic review anticipates reducing the infectivity of respiratory viral diseases, including SARS-COV-2, using nanotheranostics approaches. We have comprehensively discussed different types of metallic, ionic, organic nanoparticles and their hybrids showing substantial antiviral properties to resist the progression of the disease focused on prevention, diagnostics, and treatment. A combination of materials with distinct antiviral mechanisms is expected to fabricate an intelligent surface that can eliminate many pathogens. This could help recognize the environmental pathogens and ultimately support the public health system in managing disease outbreaks. From a therapeutic point of view, we also explored enlisting a few organic and inorganic nanoparticles that might act as a potent antiviral hybrid against SARS-COV-2 infection. We have successfully identified a few of them that can be used as a viral diagnostic tool to reduce the spread of this pandemic. These antiviral materials need to be tested and validated before their intended application in personal protective equipment, such as masks, surgical drapes, high-touch surfaces, and others aiming at emancipation from the SARS-COV-2 pandemic. This systemic review will help medical professionals and scientists to get an idea regarding the nanotheranostic approach, to prevent any COVID-19 like respiratory viral diseases.
References
J.M. Sisk, M.B. Frieman, C.E. Machamer, Coronavirus S protein-induced fusion is blocked prior to hemifusion by Abl kinase inhibitors. J. Gen. Virol. 99, 619–630 (2018). https://doi.org/10.1099/jgv.0.001047
J. Dyall, C.M. Coleman, B.J. Hart, T. Venkataraman, M.R. Holbrook, J. Kindrachuk, R.F. Johnson, G.G. Olinger, P.B. Jahrling, M. Laidlaw, L.M. Johansen, C.M. Lear-Rooney, P.J. Glass, L.E. Hensley, M.B. Frieman, Repurposing of clinically developed drugs for treatment of Middle East respiratory syndrome coronavirus infection. Antimicrob Agents Chemother. 58, 4885–4893 (2014). https://doi.org/10.1128/AAC.03036-14
W.-H. Cheng, C. von Kobbe, P.L. Opresko, K.M. Fields, J. Ren, D. Kufe, V.A. Bohr, Werner syndrome protein phosphorylation by Abl Tyrosine kinase regulates its activity and distribution. Mol. Cell Biol. 23, 6385–6395 (2003). https://doi.org/10.1128/mcb.23.18.6385-6395.2003
E.M. Rogers, A.J. Spracklen, C.G. Bilancia, K.D. Sumigray, S.C. Allred, S.H. Nowotarski, K.N. Schaefer, B.J. Ritchie, M. Peifer, Abelson kinase acts as a robust, multifunctional scaffold in regulating embryonic morphogenesis. Mol. Biol. Cell. 27, 2613–2631 (2016). https://doi.org/10.1091/mbc.E16-05-0292
A. Banerjee, K. Kulcsar, V. Misra, M. Frieman, K. Mossman, Bats and coronaviruses. Viruses 11, 7–9 (2019). https://doi.org/10.3390/v11010041
E. de Clercq, Potential antivirals and antiviral strategies against SARS coronavirus infections. Expert Rev. Anti. Infect. Ther. 4, 291–302 (2006). https://doi.org/10.1586/14787210.4.2.291
S. Belouzard, V.C. Chu, G.R. Whittaker, Activation of the SARS coronavirus spike protein via sequential proteolytic cleavage at two distinct sites. Proc. Natl. Acad. Sci. U S A. 106, 5871–5876 (2009). https://doi.org/10.1073/pnas.0809524106
G. Reina, S. Peng, L. Jacquemin, A.F. Andrade, A. Bianco, Hard nanomaterials in time of viral pandemics. ACS Nano 14, 9364–9388 (2020). https://doi.org/10.1021/acsnano.0c04117
Organization, World Health: Evolution of a pandemic (2010)
B. Biswas, S. Chattopadhyay, S. Hazra, A.K. Hansda, R. Goswami, COVID-19 pandemic: the delta variant, T-cell responses, and the efficacy of developing vaccines. Inflamm. Res. 71, 377–396 (2022). https://doi.org/10.1007/s00011-022-01555-5
Patients L, Taylor D, Lindsay AC, Halcox JP (2020) Correspondence Niacin Compared with Ezetimibe. N Engl J Med
V.S. Sivasankarapillai, A.M. Pillai, A. Rahdar, A.P. Sobha, S.S. Das, A.C. Mitropoulos, M.H. Mokarrar, G.Z. Kyzas, On facing the SARS-COV-2 (COVID-19) with combination of nanomaterials and medicine: Possible strategies and first challenges. Nanomaterials 10, 1–23 (2020). https://doi.org/10.3390/nano10050852
A.P.A. Carvalho, C.A. Conte-Junior, Recent advances on nanomaterials to COVID-19 management: a systematic review on antiviral/virucidal agents and mechanisms of SARS-COV-2 inhibition/inactivation. Global Chall. 5, 2000115 (2021). https://doi.org/10.1002/gch2.202000115
E. Ruiz-Hitzky, M. Darder, B. Wicklein, C. Ruiz-Garcia, R. Martín-Sampedro, G. del Real, P. Aranda, Nanotechnology responses to COVID-19. Adv. Healthc. Mater. 9, 1–26 (2020). https://doi.org/10.1002/adhm.202000979
J.O. Noyce, H. Michels, C.W. Keevil, Inactivation of influenza A virus on copper versus stainless steel surfaces. Appl. Environ. Microbiol. 73, 2748–2750 (2007). https://doi.org/10.1128/AEM.01139-06
A.K. Ojha, R. Rajasekaran, A.K. Pandey, A. Dutta, V.S. Seesala, S.K. Das, K. Chaudhury, S. Dhara, Nanotheranostics: Nanoparticles Applications, Perspectives, and Challenges, in BioSensing, Theranostics, and Medical Devices: From Laboratory to Point-of-Care Testing. ed. by V. Borse, P. Chandra, R. Srivastava (Springer, Singapore, 2022), pp.345–376
Jan de Cubber, Z.: Patent Application Publication (10) Pub. No.: US 2007 / 0213831 A1. Us 2007 / 0213831 a1. 1, 19–21 (2007).
Q. He, J. Lu, N. Liu, W. Lu, Y. Li, C. Shang, X. Li, L. Hu, G. Jiang, Antiviral properties of silver nanoparticles against SARS-COV-2: effects of surface coating and particle size. Nanomaterials (2022). https://doi.org/10.3390/nano12060990
K. Imai, H. Ogawa, V.N. Bui, H. Inoue, J. Fukuda, M. Ohba, Y. Yamamoto, K. Nakamura, Inactivation of high and low pathogenic avian influenza virus H5 subtypes by copper ions incorporated in zeolite-textile materials. Antiviral Res. 93, 225–233 (2012). https://doi.org/10.1016/j.antiviral.2011.11.017
J. Hodek, V. Zajícová, I. Lovetinská-Šlamborová, I. Stibor, J. Müllerová, J. Weber, Protective hybrid coating containing silver, copper and zinc cations effective against human immunodeficiency virus and other enveloped viruses. BMC Microbiol. 16, 1–12 (2016). https://doi.org/10.1186/s12866-016-0675-x
Liss, P.S., Slater, P.G.: © 1974 Nature Publishing Group. (1974).
D. Botequim, J. Maia, M.M.F. Lino, L.M.F. Lopes, P.N. Simões, L.M. Ilharco, L. Ferreira, Nanoparticles and surfaces presenting antifungal, antibacterial and antiviral properties. Langmuir 28, 7646–7656 (2012). https://doi.org/10.1021/la300948n
I. Papp, C. Sieben, K. Ludwig, M. Roskamp, C. Böttcher, S. Schlecht, A. Herrmann, R. Haag, Inhibition of influenza virus infection by multivalent sialic-acid- functionalized gold nanoparticles. Small 6, 2900–2906 (2010). https://doi.org/10.1002/smll.201001349
S. Galdiero, A. Falanga, M. Vitiello, M. Cantisani, V. Marra, M. Galdiero, Silver nanoparticles as potential antiviral agents. Molecules 16, 8894–8918 (2011). https://doi.org/10.3390/molecules16108894
M. Minoshima, Y. Lu, T. Kimura, R. Nakano, H. Ishiguro, Y. Kubota, K. Hashimoto, K. Sunada, Comparison of the antiviral effect of solid-state copper and silver compounds. J. Hazard Mater. 312, 1–7 (2016). https://doi.org/10.1016/j.jhazmat.2016.03.023
S.L. Warnes, Z.R. Little, C.W. Keevil, Human coronavirus 229E remains infectious on common touch surface materials. MBio (2015). https://doi.org/10.1128/mBio.01697-15
T. Ishida, Antiviral activities of Cu2+ Ions in viral prevention, replication, RNA degradation, and for antiviral efficacies of lytic virus, ROS-mediated virus. Copper Chelation. World Sci. News 99, 149–168 (2018)
Luminore CopperTouch TM surface coating effectively inactivates SARS-COV-2, Ebola, and Marburg viruses in vitro Emily K. Mantlo. 1–18 (2020).
Y. Li, Q.M. Pi, H.H. You, J.Q. Li, P.C. Wang, X. Yang, Y. Wu, A smart multi-functional coating based on anti-pathogen micelles tethered with copper nanoparticles: via a biosynthesis method using l-vitamin C. RSC Adv. 8, 18272–18283 (2018). https://doi.org/10.1039/c8ra01985a
V. Champagne, K. Sundberg, D. Helfritch, Kinetically deposited copper antimicrobial surfaces. Coatings 9, 1–9 (2019). https://doi.org/10.3390/coatings9040223
R. Nakano, M. Hara, H. Ishiguro, Y. Yao, T. Ochiai, K. Nakata, T. Murakami, J. Kajioka, K. Sunada, K. Hashimoto, A. Fujishima, Y. Kubota, Broad spectrum microbicidal activity of photocatalysis by TiO2. Catalysts 3, 310–323 (2013). https://doi.org/10.3390/catal3010310
B. Moongraksathum, M.-Y. Chien, Y.-W. Chen, Antiviral and antibacterial effects of silver-doped TiO2 prepared by the peroxo Sol–Gel method. J Nanosci Nanotechnol. 19, 7356–7362 (2019). https://doi.org/10.1166/jnn.2019.16615
C. Akduman, E.P. Akcakoca Kumbasar, Nanofibers in face masks and respirators to provide better protection. IOP Conf. Ser. Mater. Sci. Eng. (2018). https://doi.org/10.1088/1757-899X/460/1/012013
D. Bisht, S.L. Rath, S. Roy, A. Jaiswal, MoS2 nanosheets effectively bind to the receptor binding domain of the SARS-COV-2 spike protein and destabilize the spike-human ACE2 receptor interactions. Soft Matter 18, 8961–8973 (2022). https://doi.org/10.1039/d2sm01181f
V.Q. Nguyen, M. Ishihara, J. Kinoda, H. Hattori, S. Nakamura, T. Ono, Y. Miyahira, T. Matsui, Development of antimicrobial biomaterials produced from chitin-nanofiber sheet/silver nanoparticle composites. J. Nanobiotechnol. 12, 1–9 (2014). https://doi.org/10.1186/s12951-014-0049-1
Y.N. Chen, Y.H. Hsueh, C. te Hsieh, D.Y. Tzou, P.L. Chang, Antiviral activity of graphene–silver nanocomposites against non-enveloped and enveloped viruses. Int. J. Environ. Res. Public Health 13, 4–6 (2016). https://doi.org/10.3390/ijerph13040430
N. Yang, J.A. Tanner, B.J. Zheng, R.M. Watt, M.L. He, L.Y. Lu, J.Q. Jiang, K.T. Shum, Y.P. Lin, K.L. Wong, M.C.M. Lin, H.F. Kung, H. Sun, J.D. Huang, Bismuth complexes inhibit the SARS coronavirus. Angew. Chem.—Int. Ed. 46, 6464–6468 (2007). https://doi.org/10.1002/anie.200701021
S. Yuan, R. Wang, J.F.W. Chan, A.J. Zhang, T. Cheng, K.K.H. Chik, Z.W. Ye, S. Wang, A.C.Y. Lee, L. Jin, H. Li, D.Y. Jin, K.Y. Yuen, H. Sun, Metallodrug ranitidine bismuth citrate suppresses SARS-COV-2 replication and relieves virus-associated pneumonia in Syrian hamsters. Nat. Microbiol. 5, 1439–1448 (2020). https://doi.org/10.1038/s41564-020-00802-x
J. Haldar, J. Chen, T.M. Tumpey, L.V. Gubareva, A.M. Klibanov, Hydrophobic polycationic coatings inactivate wild-type and zanamivir- and/or oseltamivir-resistant human and avian influenza viruses. Biotechnol. Lett. 30, 475–479 (2008). https://doi.org/10.1007/s10529-007-9565-5
D. Park, A.M. Larson, A.M. Klibanov, Y. Wang, Antiviral and antibacterial polyurethanes of various modalities. Appl. Biochem. Biotechnol. 169, 1134–1146 (2013). https://doi.org/10.1007/s12010-012-9999-7
D. Cirri, A. Pratesi, T. Marzo, L. Messori, Metallo therapeutics for COVID-19 Exploiting metal-based compounds for the discovery of new antiviral drugs. Expert Opin. Drug Discov. (2021). https://doi.org/10.1080/17460441.2020.1819236
E. Tuladhar, M.C. de Koning, I. Fundeanu, R. Beumer, E. Duizer, Different virucidal activities of hyperbranched quaternary ammonium coatings on poliovirus and influenza virus. Appl. Environ. Microbiol. 78, 2456–2458 (2012). https://doi.org/10.1128/AEM.07738-11
B.L. Carpenter, F. Scholle, H. Sadeghifar, A.J. Francis, J. Boltersdorf, W.W. Weare, D.S. Argyropoulos, P.A. Maggard, R.A. Ghiladi, Synthesis, characterization, and antimicrobial efficacy of photomicrobicidal cellulose paper. Biomacromol 16, 2482–2492 (2015). https://doi.org/10.1021/acs.biomac.5b00758
W. Sun, L. He, H. Zhang, X. Tian, Z. Bai, L. Sun, L. Yang, X. Jia, Y. Bi, T. Luo, G. Cheng, W. Fan, W. Liu, J. Li, The self-assembled nanoparticle-based trimeric RBD mRNA vaccine elicits robust and durable protective immunity against SARS-COV-2 in mice. Sig. Transduct. Target Ther. (2021). https://doi.org/10.1038/s41392-021-00750-w
S.M. Olivera-Ugarte, M. Bolduc, M.È. Laliberté-Gagné, L.J. Blanchette, C. Garneau, M. Fillion, P. Savard, I. Dubuc, L. Flamand, O. Farnòs, X. Xu, A. Kamen, M. Gilbert, H. Rabezanahary, M. Scarrone, C. Couture, M. Baz, D. Leclerc, A nanoparticle-based COVID-19 vaccine candidate elicits broad neutralizing antibodies and protects against SARS-COV-2 infection. Nanomedicine (2022). https://doi.org/10.1016/j.nano.2022.102584
E. Tuaillon, K. Bolloré, A. Pisoni, S. Debiesse, C. Renault, S. Marie, S. Groc, C. Niels, N. Pansu, A.M. Dupuy, D. Morquin, V. Foulongne, A. Bourdin, V. le Moing, P. van de Perre, Detection of SARS-CoV-2 antibodies using commercial assays and seroconversion patterns in hospitalized patients. J. Infect. 81, e39–e45 (2020). https://doi.org/10.1016/j.jinf.2020.05.077
R.A. Perera, C.K. Mok, O.T. Tsang, H. Lv, R.L. Ko, N.C. Wu, M. Yuan, W.S. Leung, J.M. Chan, T.S. Chik, C.Y. Choi, K. Leung, K.H. Chan, K.C. Chan, K.-C. Li, J.T. Wu, I.A. Wilson, A.S. Monto, L.L. Poon, M. Peiris, Serological assays for severe acute respiratory syndrome. Eurosurveillance 25, 1–9 (2020)
J.R. Choi, A. Nilghaz, L. Chen, K.C. Chou, X. Lu, Modification of thread-based microfluidic device with polysiloxanes for the development of a sensitive and selective immunoassay. Sens. Actuators B Chem. 260, 1043–1051 (2018). https://doi.org/10.1016/j.snb.2018.01.102
H. Li, L. Rothberg, Colorimetric detection of DNA sequences based on electrostatic interactions with unmodified gold nanoparticles. Proc. Natl. Acad. Sci. U S A. 101, 14036–14039 (2004). https://doi.org/10.1073/pnas.0406115101
H. Bian, F. Xu, Y. Jia, L. Wang, S. Deng, A. Jia, Y. Tang, A new immunochromatographic assay for on-site detection of porcine epidemic diarrhea virus based on monoclonal antibodies prepared by using cell surface fluorescence immunosorbent assay. BMC Vet. Res. 15, 1–10 (2019). https://doi.org/10.1186/s12917-019-1773-4
T.J. Park, S.Y. Lee, S.J. Lee, J.P. Park, K.S. Yang, K.B. Lee, S. Ko, J.B. Park, T. Kim, S.K. Kim, Y.B. Shin, B.H. Chung, S.J. Ku, D.H. Kim, I.S. Choi, Protein nanopatterns and biosensors using gold binding polypeptide as a fusion partner. Anal. Chem. 78, 7197–7205 (2006). https://doi.org/10.1021/ac060976f
Z. Zhao, H. Cui, W. Song, X. Ru, W. Zhou, X. Yu, A simple magnetic nanoparticles-based viral RNA extraction method for efficient detection of SARS-COV-2. BioRxiv 518055, 961268 (2020)
J.C. Chacón-Torres, C. Reinoso, D.G. Navas-León, S. Briceño, G. González, Optimized and scalable synthesis of magnetic nanoparticles for RNA extraction in response to developing countries’ needs in the detection and control of SARS-CoV-2. Sci. Rep. 10, 1–10 (2020). https://doi.org/10.1038/s41598-020-75798-9
V. Uskoković, Why have nanotechnologies been underutilized in the global uprising against the coronavirus pandemic? Nanomedicine 15, 1719–1734 (2020). https://doi.org/10.2217/nnm-2020-0163
S.B. Somvanshi, P.B. Kharat, T.S. Saraf, S.B. Somwanshi, S.B. Shejul, K.M. Jadhav, Multifunctional nano-magnetic particles assisted viral RNA-extraction protocol for potential detection of COVID19. Mater. Res. Innov. (2020). https://doi.org/10.1080/143289171769350
Q. Huang, Y. Chen, L. Liu, D. Tao, X. Li, On Combining biclustering mining and adaboost for breast tumor classification. IEEE Trans. Knowl. Data Eng. 32, 728–738 (2020). https://doi.org/10.1109/TKDE.2019.2891622
R.L. Pinals, F. Ledesma, D. Yang, N. Navarro, S. Jeong, J.E. Pak, L. Kuo, Y.C. Chuang, Y.W. Cheng, H.Y. Sun, M.P. Landry, Rapid SARS-COV-2 spike protein detection by carbon nanotube-based near-infrared nanosensors. Nano Lett. 21, 2272–2280 (2021). https://doi.org/10.1021/acs.nanolett.1c00118
M.A. Ali, C. Hu, S. Jahan, B. Yuan, M.S. Saleh, E. Ju, S.J. Gao, R. Panat, Sensing of COVID-19 antibodies in seconds via Aerosol Jet nanoprinted reduced-graphene-oxide-coated 3D electrodes. Adv. Mater. 33, 1–15 (2021). https://doi.org/10.1002/adma.202006647
C. Roh, S.K. Jo, Quantitative and sensitive detection of SARS coronavirus nucleocapsid protein using quantum dots-conjugated RNA aptamer on chip. J. Chem. Technol. Biotechnol. 86, 1475–1479 (2011). https://doi.org/10.1002/jctb.2721
Y. Rasmi, K.S. Saloua, M. Nemati, J.R. Choi, Recent progress in nanotechnology for covid-19 prevention, diagnostics and treatment. Nanomaterials 11, 1–25 (2021)
K.N. Fatema, S. Sagadevan, J.Y. Cho, W.K. Jang, W.C. Oh, Graphene-based nanocomposite using new modeling molecular dynamic simulations for proposed neutralizing mechanism and real-time sensing of COVID-19. Nanotechnol. Rev. (2022). https://doi.org/10.1515/ntrev-2022-0093
Rothan, H.A., Stone, S., Natekar, J., Kumari, P., Arora, K., Kumar, M.: Since January 2020 Elsevier has created a COVID-19 resource centre with free information in English and Mandarin on the novel coronavirus COVID- 19 . The COVID-19 resource centre is hosted on Elsevier Connect , the company ’ s public news and information . (2020).
C.J. Neal, C.R. Fox, T.S. Sakthivel, U. Kumar, Y. Fu, C. Drake, G.D. Parks, S. Seal, Metal-mediated nanoscale cerium oxide inactivates human coronavirus and rhinovirus by surface disruption. ACS Nano 15, 14544–14556 (2021). https://doi.org/10.1021/acsnano.1c04142
X. Lv, P. Wang, R. Bai, Y. Cong, S. Suo, X. Ren, C. Chen, Inhibitory effect of silver nanomaterials on transmissible virus-induced host cell infections. Biomaterials 35, 4195–4203 (2014). https://doi.org/10.1016/j.biomaterials.2014.01.054
S.Y. Chang, K.Y. Huang, T.L. Chao, H.C. Kao, Y.H. Pang, L. Lu, C.L. Chiu, H.C. Huang, T.J.R. Cheng, J.M. Fang, P.C. Yang, Nanoparticle composite TPNT1 is effective against SARS-COV-2 and influenza viruses. Sci. Rep. 11, 1–13 (2021). https://doi.org/10.1038/s41598-021-87254-3
V. Cagno, P. Andreozzi, M. D’Alicarnasso, P.J. Silva, M. Mueller, M. Galloux, R. le Goffic, S.T. Jones, M. Vallino, J. Hodek, J. Weber, S. Sen, E.R. Janecek, A. Bekdemir, B. Sanavio, C. Martinelli, M. Donalisio, M.A.R. Welti, J.F. Eleouet, Y. Han, L. Kaiser, L. Vukovic, C. Tapparel, P. Král, S. Krol, D. Lembo, F. Stellacci, Broad-spectrum non-toxic antiviral nanoparticles with a virucidal inhibition mechanism. Nat. Mater. 17, 195–203 (2018). https://doi.org/10.1038/NMAT5053
Q. Zhang, A. Honko, J. Zhou, H. Gong, S.N. Downs, J.H. Vasquez, R.H. Fang, W. Gao, A. Griffiths, L. Zhang, Cellular nanosponges inhibit SARS-COV-2 infectivity. Nano Lett. 20, 5570–5574 (2020). https://doi.org/10.1021/acs.nanolett.0c02278
P. Zhang, Y. Chen, Y. Zeng, C. Shen, R. Li, Z. Guo, S. Li, Q. Zheng, C. Chu, Z. Wang, Z. Zheng, R. Tian, S. Ge, X. Zhang, N.S. Xia, G. Liu, X. Chen, Virus-mimetic nanovesicles as a versatile antigen-delivery system. Proc. Natl. Acad. Sci. U. S. A. 112, E6129–E6138 (2015). https://doi.org/10.1073/pnas.1505799112
L. Rao, W. Wang, Q.F. Meng, M. Tian, B. Cai, Y. Wang, A. Li, M. Zan, F. Xiao, L.L. Bu, G. Li, A. Li, Y. Liu, S.S. Guo, X.Z. Zhao, T.H. Wang, W. Liu, J. Wu, A biomimetic nanodecoy traps Zika virus to prevent viral infection and fetal microcephaly development. Nano Lett. 19, 2215–2222 (2019). https://doi.org/10.1021/acs.nanolett.8b03913
J.M. Richner, S. Himansu, K.A. Dowd, S.L. Butler, V. Salazar, J.M. Fox, J.G. Julander, W.W. Tang, S. Shresta, T.C. Pierson, G. Ciaramella, M.S. Diamond, Modified mRNA vaccines protect against Zika Virus Infection. Cell 168, 1114-1125.e10 (2017). https://doi.org/10.1016/j.cell.2017.02.017
D. Ting, N. Dong, L. Fang, J. Lu, J. Bi, S. Xiao, H. Han, Erratum: multisite inhibitors for enteric coronavirus: antiviral cationic carbon dots based on curcumin. ACS Appl. Nano Mater. (2018). https://doi.org/10.1021/acsanm.0c00970
A. Łoczechin, K. Séron, A. Barras, E. Giovanelli, S. Belouzard, Y.T. Chen, N. Metzler-Nolte, R. Boukherroub, J. Dubuisson, S. Szunerits, Functional carbon quantum dots as medical countermeasures to human coronavirus. ACS Appl. Mater. Interfaces 11, 42964–42974 (2019). https://doi.org/10.1021/acsami.9b15032
J. Wu, H. Wang, B. Li, Structure-aided ACEI-capped remdesivir-loaded novel PLGA nanoparticles: toward a computational simulation design for anti-SARS-COV-2 therapy. Phys. Chem. Chem. Phys. 22, 28434–28439 (2020). https://doi.org/10.1039/d0cp04389c
N.A. Alhakamy, O.A.A. Ahmed, T.S. Ibrahim, H.M. Aldawsari, K. Eljaaly, U.A. Fahmy, A.L. Alaofi, F. Caraci, G. Caruso, Evaluation of the antiviral activity of Sitagliptin-Glatiramer acetate nano-conjugates against SARS-CoV-2 Virus. Pharmaceuticals (2021). https://doi.org/10.3390/ph14030178
F.E.T. Foka, N. Manamela, S.M. Mufamadi, H.T. Mufhandu, Potential of Azadirachta indica as a capping agent for antiviral nanoparticles against SARS-COV-2. BioMed. Res. Int. (2022). https://doi.org/10.1155/2022/5714035
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
SM and NS: provided data after an extensive literature review. SM: compiled all data and make tables and figures to find correlations between all data and drew the conclusion. Finally, SD: read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mukherjee, S., Manna, S., Som, N. et al. Organic–Inorganic Hybrid Nanocomposites for Nanotheranostics: Special Focus on Preventing Emerging Variants of SARS-COV-2. Biomedical Materials & Devices 1, 633–647 (2023). https://doi.org/10.1007/s44174-023-00077-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s44174-023-00077-w