Abstract
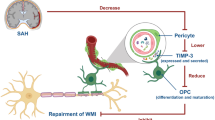
Myelin sheath injury contributes to cognitive deficits following subarachnoid hemorrhage (SAH). G protein-coupled receptor 17 (GPR17), a membrane receptor, negatively regulates oligodendrocyte precursor cell (OPC) differentiation in both developmental and pathological contexts. Nonetheless, GPR17's role in modulating OPC differentiation, facilitating remyelination post SAH, and its interaction with downstream molecules remain elusive. In a rat SAH model induced by arterial puncture, OPCs expressing GPR17 proliferated prominently by day 14 post-onset, coinciding with compromised myelin sheath integrity and cognitive deficits. Selective Gpr17 knockdown in oligodendrocytes (OLs) via adeno-associated virus (AAV) administration revealed that reduced GPR17 levels promoted OPC differentiation, restored myelin sheath integrity, and improved cognitive deficits by day 14 post-SAH. Moreover, GPR17 knockdown attenuated the elevated expression of the inhibitor of DNA binding 2 (ID2) post-SAH, suggesting a GPR17-ID2 regulatory axis. Bi-directional modulation of ID2 expression in OLs using AAV unveiled that elevated ID2 counteracted the restorative effects of GPR17 knockdown. This resulted in hindered differentiation, exacerbated myelin sheath impairment, and worsened cognitive deficits. These findings highlight the pivotal roles of GPR17 and ID2 in governing OPC differentiation and axonal remyelination post-SAH. This study positions GPR17 as a potential therapeutic target for SAH intervention. The interplay between GPR17 and ID2 introduces a novel avenue for ameliorating cognitive deficits post-SAH.







Similar content being viewed by others
Data Availability
The data that were used to support the findings of this study are not openly available to maintain privacy protection. However, the data can be made available from the corresponding author upon reasonable request. Researchers who are interested in accessing the data for scientific purposes can contact the corresponding author to request access.
Abbreviations
- aSAH:
-
Aneurysmal subarachnoid hemorrhage
- AAV:
-
Adeno-associated virus
- ACA:
-
Anterior cerebral artery
- AUC:
-
Area under the curve
- BrdU:
-
Bromodeoxyuridine
- CBF:
-
Cerebral blood flow
- CC:
-
Corpus callosum
- CCA:
-
Common carotid artery
- CNS:
-
Central nervous system
- EAE:
-
Experimental autoimmune encephalomyelitis
- ECA:
-
External carotid artery
- DCI:
-
Delayed cerebral ischemia
- GPR17:
-
G protein-coupled receptor 17 (for protein)
- Gpr17:
-
Gpr17 gene
- ICA:
-
Internal carotid artery
- IF:
-
Immunofluorescence
- LFP:
-
Local field potential
- MWM:
-
Morris water maze
- MS:
-
Multiple sclerosis
- NC:
-
Normal control
- OGD:
-
Oxygen-glucose deprivation
- OL:
-
Oligodendrocyte OPColigodendrocyte precursor cell
- OPC:
-
Oligodendrocyte precursor cell
- PSD:
-
Power spectral density
- ROI:
-
Region of interest
- ShG-V:
-
AAV2/9-control shRNA
- ShG:
-
AAV2/9-Gpr17 shRNA
- SGOI-V:
-
AAV2/9-Gpr17 shRNA + AAV2/9-NC control
- SGOI:
-
AAV2/9-Gpr17 shRNA + AAV2/9-Id2 overexpression RNA
- SGSI-V:
-
AAV2/9-Gpr17 shRNA + AAV2/9-control shRNA
- SGSI:
-
AAV2/9-Gpr17 shRNA + AAV2/9-Id2 shRNA
- TEM:
-
Transmission electron microscope
- WB:
-
Western blotting
References
Feigin VL, Lawes CMM, Bennett DA, Barker-Collo SL, Parag V. Worldwide stroke incidence and early case fatality reported in 56 population-based studies: a systematic review. Lancet Neurol. 2009;8:355–69.
Macdonald RL, Schweizer TA. Spontaneous subarachnoid haemorrhage. Lancet. 2017;389:655–66.
Hu X, Yan J, Huang L, Araujo C, Peng J, Gao L, et al. INT-777 attenuates NLRP3-ASC inflammasome-mediated neuroinflammation via TGR5/cAMP/PKA signaling pathway after subarachnoid hemorrhage in rats. Brain Behav Immun. 2021;91:587–600.
Chen S, Feng H, Sherchan P, Klebe D, Zhao G, Sun X, et al. Controversies and evolving new mechanisms in subarachnoid hemorrhage. Prog Neurobiol. 2014;115:64–91.
Shen H, Chen Z, Wang Y, Gao A, Li H, Cui Y, et al. Role of Neurexin-1β and Neuroligin-1 in Cognitive Dysfunction After Subarachnoid Hemorrhage in Rats. Stroke. 2015;46:2607–15.
van Donkelaar CE, Bakker NA, Birks J, Veeger NJGM, Metzemaekers JDM, Molyneux AJ, et al. Prediction of Outcome After Aneurysmal Subarachnoid Hemorrhage. Stroke. 2019;50:837–44.
Minhas JS, Moullaali TJ, Rinkel GJE, Anderson CS. Blood Pressure Management After Intracerebral and Subarachnoid Hemorrhage: The Knowns and Known Unknowns. Stroke. 2022;53:1065–73.
Reijmer YD, van den Heerik MS, Heinen R, Leemans A, Hendrikse J, de Vis JB, et al. Microstructural White Matter Abnormalities and Cognitive Impairment After Aneurysmal Subarachnoid Hemorrhage. Stroke. 2018;49:2040–5.
Xu S, Lu J, Shao A, Zhang JH, Zhang J. Glial Cells: Role of the Immune Response in Ischemic Stroke. Front Immunol. 2020;11:294.
Monje M. Myelin Plasticity and Nervous System Function. Annu Rev Neurosci. 2018;41:61–76.
Rost NS, Brodtmann A, Pase MP, van Veluw SJ, Biffi A, Duering M, et al. Post-Stroke Cognitive Impairment and Dementia. Circ Res. 2022;130:1252–71.
Wu Y, Peng J, Pang J, Sun X, Jiang Y. Potential mechanisms of white matter injury in the acute phase of experimental subarachnoid haemorrhage. Brain. 2017;140:e36.
Peng J, Pang J, Huang L, Enkhjargal B, Zhang T, Mo J, et al. LRP1 activation attenuates white matter injury by modulating microglial polarization through Shc1/PI3K/Akt pathway after subarachnoid hemorrhage in rats. Redox Biol. 2019;21:101121.
Egashira Y, Zhao H, Hua Y, Keep RF, Xi G. White Matter Injury After Subarachnoid Hemorrhage: Role of Blood-Brain Barrier Disruption and Matrix Metalloproteinase-9. Stroke. 2015;46:2909–15.
Wu X, Wang Z, Li H, Xie X, Wu J, Shen H, et al. Loss of monocarboxylate transporter 1 aggravates white matter injury after experimental subarachnoid hemorrhage in rats. Front Med. 2021;15:887–902.
Xin W, Chan JR. Myelin plasticity: sculpting circuits in learning and memory. Nat Rev Neurosci. 2020;21:682–94.
Jäkel S, Agirre E, MendanhaFalcão A, van Bruggen D, Lee KW, Knuesel I, et al. Altered human oligodendrocyte heterogeneity in multiple sclerosis. Nature. 2019;566:543–7.
Ou Z, Sun Y, Lin L, You N, Liu X, Li H, et al. Olig2-Targeted G-Protein-Coupled Receptor Gpr17 Regulates Oligodendrocyte Survival in Response to Lysolecithin-Induced Demyelination. J Neurosci. 2016;36:10560–73.
Wang J, He X, Meng H, et al. Robust myelination of regenerated axons induced by combined manipulations of GPR17 and microglia. Neuron. 2020;108(5):876-886.e4. https://doi.org/10.1016/j.neuron.2020.09.016.
Wang Y, Yang X, Cao Y, et al. Electroacupuncture promotes remyelination and alleviates cognitive deficit via promoting OPC differentiation in a rat model of subarachnoid hemorrhage. Metab Brain Dis. 2023;38(2):687–98. https://doi.org/10.1007/s11011-022-01102-5.
Merten N, Fischer J, Simon K, et al. Repurposing HAMI3379 to Block GPR17 and promote rodent and human oligodendrocyte differentiation. Cell Chem Biol. 2018;25(6):775-786.e5. https://doi.org/10.1016/j.chembiol.2018.03.012.
Rivera AD, Pieropan F, Chacon-De-La-Rocha I, Lecca D, Abbracchio MP, Azim K, et al. Functional genomic analyses highlight a shift in Gpr17-regulated cellular processes in oligodendrocyte progenitor cells and underlying myelin dysregulation in the aged mouse cerebrum. Aging Cell. 2021;20:e13335.
Lecca D, Raffaele S, Abbracchio MP, Fumagalli M. Regulation and signaling of the GPR17 receptor in oligodendroglial cells. Glia. 2020;68:1957–67.
Chen Y, Wu H, Wang S, Koito H, Li J, Ye F, et al. The oligodendrocyte-specific G protein-coupled receptor GPR17 is a cell-intrinsic timer of myelination. Nat Neurosci. 2009;12:1398–406.
Simon K, Hennen S, Merten N, Blättermann S, Gillard M, Kostenis E, et al. The Orphan G Protein-coupled Receptor GPR17 Negatively Regulates Oligodendrocyte Differentiation via Gαi/o and Its Downstream Effector Molecules. J Biol Chem. 2016;291:705–18.
Wang S, Sdrulla A, Johnson JE, Yokota Y, Barres BA. A role for the helix-loop-helix protein Id2 in the control of oligodendrocyte development. Neuron. 2001;29:603–14.
Samanta J, Kessler JA. Interactions between ID and OLIG proteins mediate the inhibitory effects of BMP4 on oligodendroglial differentiation. Development. 2004;131:4131–42.
Jessen KR, Mirsky R. Negative regulation of myelination: relevance for development, injury, and demyelinating disease. Glia. 2008;56:1552–65.
Havrda MC, Paolella BR, Ran C, Jering KS, Wray CM, Sullivan JM, et al. Id2 mediates oligodendrocyte precursor cell maturation arrest and is tumorigenic in a PDGF-rich microenvironment. Cancer Res. 2014;74:1822–32.
Hesp ZC, Goldstein EZ, Goldstein EA, Miranda CJ, Kaspar BK, Kaspar BK, et al. Chronic oligodendrogenesis and remyelination after spinal cord injury in mice and rats. J Neurosci. 2015;35:1274–90.
Plemel JR, Manesh SB, Sparling JS, Tetzlaff W. Myelin inhibits oligodendroglial maturation and regulates oligodendrocytic transcription factor expression. Glia. 2013;61:1471–87.
Wu K-J, Chen Y-H, Bae E-K, Song Y, Min W, Yu S-J. Human Milk Oligosaccharide 2’-Fucosyllactose Reduces Neurodegeneration in Stroke Brain. Transl Stroke Res. 2020;11:1001–11.
Zhu Q, Enkhjargal B, Huang L, Zhang T, Sun C, Xie Z, et al. Aggf1 attenuates neuroinflammation and BBB disruption via PI3K/Akt/NF-κB pathway after subarachnoid hemorrhage in rats. J Neuroinflammation. 2018;15:178.
Liu X, Zhao S, Liu F, Kang J, Xiao A, Li F, et al. Remote ischemic postconditioning alleviates cerebral ischemic injury by attenuating endoplasmic reticulum stress-mediated apoptosis. Transl Stroke Res. 2014;5:692–700.
Zhu W, Saw D, Weiss M, Sun Z, Wei M, Shaligram S, et al. Induction of Brain Arteriovenous Malformation Through CRISPR/Cas9-Mediated Somatic Alk1 Gene Mutations in Adult Mice. Transl Stroke Res. 2019;10:557–65.
Zhang T, Wu P, Budbazar E, Zhu Q, Sun C, Mo J, et al. Mitophagy Reduces Oxidative Stress Via Keap1 (Kelch-Like Epichlorohydrin-Associated Protein 1)/Nrf2 (Nuclear Factor-E2-Related Factor 2)/PHB2 (Prohibitin 2) Pathway After Subarachnoid Hemorrhage in Rats. Stroke. 2019;50:978–88.
Yang J, Jing J, Chen S, Liu X, Tang Y, Pan C, et al. Changes in Cerebral Blood Flow and Diffusion-Weighted Imaging Lesions After Intracerebral Hemorrhage. Transl Stroke Res. 2022;13:686–706.
Zhang Y, Zhu M, Sun Y, et al. Environmental noise degrades hippocampus-related learning and memory. Proc Natl Acad Sci U S A. 2021;118(1):e2017841117. https://doi.org/10.1073/pnas.2017841117.
Chen D, Li J, Huang Y, Wei P, Miao W, Yang Y, et al. Interleukin 13 promotes long-term recovery after ischemic stroke by inhibiting the activation of STAT3. J Neuroinflammation. 2022;19:112.
Yan J, Li W, Zhou C, et al. Dynamic Measurements of cerebral blood flow responses to cortical spreading depolarization in the murine endovascular perforation subarachnoid hemorrhage model. Transl Stroke Res. 2023;14(4):530–44. https://doi.org/10.1007/s12975-022-01052-1.
Goshi N, Morgan RK, Lein PJ, Seker E. A primary neural cell culture model to study neuron, astrocyte, and microglia interactions in neuroinflammation. J Neuroinflammation. 2020;17:155.
Narayanan SV, Dave KR, Perez-Pinzon MA. Ischemic Preconditioning Protects Astrocytes against Oxygen Glucose Deprivation Via the Nuclear Erythroid 2-Related Factor 2 Pathway. Transl Stroke Res. 2018;9(2):99–109. https://doi.org/10.1007/s12975-017-0574-y.
Girdhar K, Huang Q, Chow IT, Vatanen T, Brady C, Raisingani A, et al. A gut microbial peptide and molecular mimicry in the pathogenesis of type 1 diabetes. Proc Natl Acad Sci USA. 2022;119:e2120028119.
Zhang YN, Wu Q, Zhang NN, Chen HS. Ischemic Preconditioning Alleviates Cerebral Ischemia-Reperfusion Injury by Interfering With Glycocalyx. Transl Stroke Res. 2022. https://doi.org/10.1007/s12975-022-01081-w.
Zhang P, Kishimoto Y, Grammatikakis I, Gottimukkala K, Cutler RG, Zhang S, et al. Senolytic therapy alleviates Aβ-associated oligodendrocyte progenitor cell senescence and cognitive deficits in an Alzheimer’s disease model. Nat Neurosci. 2019;22:719–28.
Zhang L, He X, Liu X, et al. Single-Cell Transcriptomics in Medulloblastoma Reveals Tumor-Initiating Progenitors and Oncogenic Cascades during Tumorigenesis and Relapse. Cancer Cell. 2019;36(3):302-318.e7. https://doi.org/10.1016/j.ccell.2019.07.009.
Sherafat A, Pfeiffer F, Reiss AM, Wood WM, Nishiyama A. Microglial neuropilin-1 promotes oligodendrocyte expansion during development and remyelination by trans-activating platelet-derived growth factor receptor. Nat Commun. 2021;12:2265.
Sturm D, Witt H, Hovestadt V, Khuong-Quang D-A, Jones DTW, Konermann C, et al. Hotspot mutations in H3F3A and IDH1 define distinct epigenetic and biological subgroups of glioblastoma. Cancer Cell. 2012;22:425–37.
Dugas JC, Cuellar TL, Scholze A, Ason B, Ibrahim A, Emery B, et al. Dicer1 and miR-219 Are required for normal oligodendrocyte differentiation and myelination. Neuron. 2010;65:597–611.
Jiang L, Shen F, Degos V, Schonemann M, Pleasure SJ, Mellon SH, et al. Oligogenesis and oligodendrocyte progenitor maturation vary in different brain regions and partially correlate with local angiogenesis after ischemic stroke. Transl Stroke Res. 2011;2:366–75.
Meijer DH, Kane MF, Mehta S, Liu H, Harrington E, Taylor CM, et al. Separated at birth? The functional and molecular divergence of OLIG1 and OLIG2. Nat Rev Neurosci. 2012;13:819–31.
Ramos-Cejudo J, Gutiérrez-Fernández M, Otero-Ortega L, Rodríguez-Frutos B, Fuentes B, Vallejo-Cremades MT, et al. Brain-derived neurotrophic factor administration mediated oligodendrocyte differentiation and myelin formation in subcortical ischemic stroke. Stroke. 2015;46:221–8.
Xu W, Li T, Gao L, Zheng J, Yan J, Zhang J, et al. Apelin-13/APJ system attenuates early brain injury via suppression of endoplasmic reticulum stress-associated TXNIP/NLRP3 inflammasome activation and oxidative stress in a AMPK-dependent manner after subarachnoid hemorrhage in rats. J Neuroinflammation. 2019;16:247.
Fan H, Ding R, Liu W, Zhang X, Li R, Wei B, et al. Heat shock protein 22 modulates NRF1/TFAM-dependent mitochondrial biogenesis and DRP1-sparked mitochondrial apoptosis through AMPK-PGC1α signaling pathway to alleviate the early brain injury of subarachnoid hemorrhage in rats. Redox Biol. 2021;40:101856.
Xu W, Yan J, Ocak U, Lenahan C, Shao A, Tang J, et al. Melanocortin 1 receptor attenuates early brain injury following subarachnoid hemorrhage by controlling mitochondrial metabolism AMPK/SIRT1/PGC-1α pathway in rats. Theranostics. 2021;11:522–39.
Macdonald RL. Delayed neurological deterioration after subarachnoid haemorrhage. Nat Rev Neurol. 2014;10:44–58.
Geraghty JR, Testai FD. Delayed Cerebral Ischemia after Subarachnoid Hemorrhage: Beyond Vasospasm and Towards a Multifactorial Pathophysiology. Curr Atheroscler Rep. 2017;19:50.
Savarraj JPJ, Hergenroeder GW, Zhu L, Chang T, Park S, Megjhani M, et al. Machine Learning to Predict Delayed Cerebral Ischemia and Outcomes in Subarachnoid Hemorrhage. Neurology. 2021;96:e553–62.
Neifert SN, Chapman EK, Martini ML, Shuman WH, Schupper AJ, Oermann EK, et al. Aneurysmal Subarachnoid Hemorrhage: the Last Decade. Transl Stroke Res. 2021;12:428–46.
Egashira Y, Hua Y, Keep RF, Xi G. Acute white matter injury after experimental subarachnoid hemorrhage: potential role of lipocalin 2. Stroke. 2014;45:2141–3.
Toyota Y, Wei J, Xi G, Keep RF, Hua Y. White matter T2 hyperintensities and blood-brain barrier disruption in the hyperacute stage of subarachnoid hemorrhage in male mice: The role of lipocalin-2. CNS Neurosci Ther. 2019;25:1207–14.
Wang F, Ren SY, Chen JF, Liu K, Li RX, Li ZF, et al. Myelin degeneration and diminished myelin renewal contribute to age-related deficits in memory. Nat Neurosci. 2020;23:481–6.
Klebe D, Krafft PR, Hoffmann C, Lekic T, Flores JJ, Rolland W, et al. Acute and delayed deferoxamine treatment attenuates long-term sequelae after germinal matrix hemorrhage in neonatal rats. Stroke. 2014;45:2475–9.
Campbell JSW, Leppert IR, Narayanan S, Boudreau M, Duval T, Cohen-Adad J, et al. Promise and pitfalls of g-ratio estimation with MRI. Neuroimage. 2018;182:80–96.
Young KM, Psachoulia K, Tripathi RB, Dunn S-J, Cossell L, Attwell D, et al. Oligodendrocyte dynamics in the healthy adult CNS: evidence for myelin remodeling. Neuron. 2013;77:873–85.
Eijlers AJC, Meijer KA, van Geest Q, Geurts JJG, Schoonheim MM. Determinants of Cognitive Impairment in Patients with Multiple Sclerosis with and without Atrophy. Radiology. 2018;288:544–51.
Bouhrara M, Reiter DA, Bergeron CM, Zukley LM, Ferrucci L, Resnick SM, et al. Evidence of demyelination in mild cognitive impairment and dementia using a direct and specific magnetic resonance imaging measure of myelin content. Alzheimer’s Dementia. 2018;14:998–1004.
Chen JF, Liu K, Hu B, Li RR, Xin W, Chen H, et al. Enhancing myelin renewal reverses cognitive dysfunction in a murine model of Alzheimer’s disease. Neuron. 2021;109:2292-2307.e2295.
Piao J, Major T, Auyeung G, Policarpio E, Menon J, Droms L, et al. Human embryonic stem cell-derived oligodendrocyte progenitors remyelinate the brain and rescue behavioral deficits following radiation. Cell Stem Cell. 2015;16:198–210.
Lim TC, Mandeville E, Weng D, Wang L-S, Kurisawa M, Leite-Morris K, et al. Hydrogel-Based Therapy for Brain Repair After Intracerebral Hemorrhage. Transl Stroke Res. 2020;11:412–7.
Kantarci K, Senjem ML, Avula R, Zhang B, Samikoglu AR, Weigand SD, et al. Diffusion tensor imaging and cognitive function in older adults with no dementia. Neurology. 2011;77:26–34.
Yan J, Zhang Y, Wang L, Li Z, Tang S, Wang Y, et al. TREM2 activation alleviates neural damage via Akt/CREB/BDNF signalling after traumatic brain injury in mice. J Neuroinflammation. 2022;19:289.
Raffaele S, Gelosa P, Bonfanti E, Lombardi M, Castiglioni L, Cimino M, et al. Microglial vesicles improve post-stroke recovery by preventing immune cell senescence and favoring oligodendrogenesis. Mol Ther. 2021;29:1439–58.
Meraviglia V, Ulivi AF, Boccazzi M, Valenza F, Fratangeli A, Passafaro M, et al. SNX27, a protein involved in down syndrome, regulates GPR17 trafficking and oligodendrocyte differentiation. Glia. 2016;64:1437–60.
Tiane A, Schepers M, Riemens R, Rombaut B, Vandormael P, Somers V, et al. DNA methylation regulates the expression of the negative transcriptional regulators ID2 and ID4 during OPC differentiation. Cell Mol Life Sci. 2021;78:6631–44.
Acknowledgements
The authors acknowledge the financial support provided by the National Natural Science Foundation of China, Chongqing Science and Health Joint Medical Research Project and the Science and Technology Research Program of Chongqing Municipal Education Commission.
Funding
• the National Natural Science Foundation of China (No.81901210 No.82071332 and No.82071397).
• the Key Project of Chongqing Science and Health Joint Medical Research Project (No.2020GDRC024).
• the Science and Technology Research Program of Chongqing Municipal Education Commission (No.KJQN202000428 and No.CYS22342).
Author information
Authors and Affiliations
Contributions
• Yue Wu, Zongduo Guo and Xiaochuan Sun designed the experimental protocol.
• Yingwen Wang and Anan Jiang conducted the experiments.
• Jin Yan, Daochen Wen, Nina Gu, Zhao Li, participated in various experiment steps, including data collection and analysis.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Ethical Approval
All procedures involving animals were approved by the Institutional Animal Care and Use Committee at Chongqing Medical University. All animal procedures complied with the regulations of the Institutional Animal Care and Use Committee at Chongqing Medical University.
Conflict of Interest
The authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Y., Jiang, A., Yan, J. et al. Inhibition of GPR17/ID2 Axis Improve Remyelination and Cognitive Recovery after SAH by Mediating OPC Differentiation in Rat Model. Transl. Stroke Res. (2023). https://doi.org/10.1007/s12975-023-01201-0
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12975-023-01201-0