Abstract
Objectives
Uric acid(UA) is related with cardiovascular disease, but the association of UA variability with all-cause mortality is rarely known. This study aimed to investigate the relationship between UA variability and all-cause mortality in Kailuan cohort study in northern China.
Design
Cohort study.
Setting
Kailuan community hospitals in Tangshan, Hebei province, Northern China.
Participants
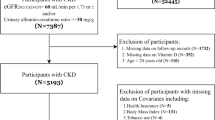
A total of 55717 participants from Kailuan Study were enrolled, and our study followed up biennially from 2006 to 2010.
Measurements
Clinical records of the participants enrolled were analyzed. UA variation independent of mean (UAVIM) values were calculated and all the participants were quartile grouped into four groups as: Q1(UAVIM<0.68), Q2(0.68≤UAVIM<1.10), Q3(1.10≤UAVIM<1.67) and Q4(UAVIM≥1.67). The endpoint event was all-cause death. Cox regression model was performed to evaluate the hazard ratios(HRs) of all-cause mortality based on UAVIM groups.
Results
During a median follow-up of 6.83 years, 2926 deaths occurred. The accumulated mortality rates were 4.6%, 4.8%, 5.4% and 6.1% in group Q1, Q2, Q3 and Q4 respectively. When adjusted potential confounders, the highest risk for all-cause mortality was in group Q4 and the adjusted HRs and 95% confidence intervals(CIs) of group Q2–Q4 for all-cause death were 1.044(0.937, 1.164), 1.182(1.064, 1.314) and 1.353(1.220, 1.501) compared with group Q1, respectively. Further analysis showed that the risk for all-cause death increased as UAVIM value increased. Sensitive analysis still showed the similar results when excluding participants with hyperuricemia or severe chronic kidney diseases. Sub-group analysis by age, gender, BMI or hypertension history also indicated analogous results.
Conclusion
Elevated UAVIM was related with increased all-cause mortality and UAVIM was an independent risk factor for all-cause mortality in the community cohort study.


Similar content being viewed by others
References
Johnson RJ, Bakris GL, Borghi C, et al. Hyperuricemia, Acute and Chronic Kidney Disease, Hypertension, and Cardiovascular Disease: Report of a Scientific Workshop Organized by the National Kidney Foundation. Am J Kidney Dis. 2018;71(6):851–865. doi:https://doi.org/10.1053/j.ajkd.2017.12.009.
Maruhashi T, Hisatome I, Kihara Y, Higashi Y. Hyperuricemia and endothelial function: From molecular background to clinical perspectives. Atherosclerosis. 2018;278:226–231.doi:https://doi.org/10.1016/j.atherosclerosis.2018.10.007.
Qin T, Zhou X, Wang J, et al. Hyperuricemia and the Prognosis of Hypertensive Patients: A Systematic Review and Meta-Analysis. J Clin Hypertens (Greenwich). 2016;18(12):1268–1278.doi:https://doi.org/10.1111/jch.12855.
Juraschek SP, McAdams-Demarco M, Miller ER, et al. Temporal relationship between uric acid concentration and risk of diabetes in a community-based study population. Am J Epidemiol. 2014;179(6):684–691.doi:https://doi.org/10.1093/aje/kwt320.
Kuwabara M, Borghi C, Cicero AFG, et al. Elevated serum uric acid increases risks for developing high LDL cholesterol and hypertriglyceridemia: A five-year cohort study in Japan. Int J Cardiol. 2018;261:183–188.doi:https://doi.org/10.1016/j.ijcard.2018.03.045.
Feig DI, Kang DH, Johnson RJ. Uric acid and cardiovascular risk. N Engl J Med. 2008;359(17):1811–1821.doi:https://doi.org/10.1056/NEJMra0800885.
Meisinger C, Koenig W, Baumert J, Doring A. Uric acid levels are associated with all-cause and cardiovascular disease mortality independent of systemic inflammation in men from the general population: the MONICA/KORA cohort study. Arterioscler Thromb Vasc Biol. 2008;28(6):1186–1192.doi:https://doi.org/10.1161/ATVBAHA.107.160184.
Konta T, Ichikawa K, Kawasaki R, et al. Association between serum uric acid levels and mortality: a nationwide community-based cohort study. Sci Rep. 2020;10(1):6066. doi:https://doi.org/10.1038/s41598-020-63134-0.
Kleber ME, Delgado G, Grammer TB, et al. Uric Acid and Cardiovascular Events: A Mendelian Randomization Study. J Am Soc Nephrol. 2015;26(11):2831–2838. doi:https://doi.org/10.1681/ASN.2014070660.
Tscharre M, Herman R, Rohla M, et al. Uric acid is associated with long-term adverse cardiovascular outcomes in patients with acute coronary syndrome undergoing percutaneous coronary intervention. Atherosclerosis. 2018;270:173–179.doi:https://doi.org/10.1016/j.atherosclerosis.2018.02.003.
Xia X, Luo Q, Li B, Lin Z, Yu X, Huang F. Serum uric acid and mortality in chronic kidney disease: A systematic review and meta-analysis. Metabolism. 2016;65(9):1326–1341.doi:https://doi.org/10.1016/j.metabol.2016.05.009.
Cho SK, Chang Y, Kim I, Ryu S. U-Shaped Association Between Serum Uric Acid Level and Risk of Mortality: A Cohort Study. Arthritis Rheumatol. 2018;70(7):1122–1132.doi:https://doi.org/10.1002/art.40472.
Hu L, Hu G, Xu BP, et al. U-Shaped Association of Serum Uric Acid With All-Cause and Cause-Specific Mortality in US Adults: A Cohort Study. J Clin Endocrinol Metab. 2020;105(1).doi:https://doi.org/10.1210/clinem/dgz068.
Cheong E, Ryu S, Lee JY, et al. Association between serum uric acid and cardiovascular mortality and all-cause mortality: a cohort study. J Hypertens. 2017;35 Suppl 1:S3–S9.doi:https://doi.org/10.1097/HJH.0000000000001330.
Grossman C, Grossman E, Goldbourt U. Uric acid variability at midlife as an independent predictor of coronary heart disease and all-cause mortality. PLoS One. 2019;14(8):e0220532.doi:https://doi.org/10.1371/journal.pone.0220532.
Loeffler LF, Navas-Acien A, Brady TM, Miller ER, 3rd, Fadrowski JJ. Uric acid level and elevated blood pressure in US adolescents: National Health and Nutrition Examination Survey, 1999–2006. Hypertension. 2012;59(4):811–817.doi:https://doi.org/10.1161/HYPERTENSIONAHA.111.183244.
Cagli K, Turak O, Canpolat U, et al. Association of Serum Uric Acid Level With Blood Pressure Variability in Newly Diagnosed Essential Hypertension. J Clin Hypertens (Greenwich). 2015;17(12):929–935.doi:https://doi.org/10.1111/jch.12641.
Stevens SL, Wood S, Koshiaris C, et al. Blood pressure variability and cardiovascular disease: systematic review and meta-analysis. BMJ. 2016;354:i4098.doi:https://doi.org/10.1136/bmj.i4098.
Wang J, Shi X, Ma C, et al. Visit-to-visit blood pressure variability is a risk factor for all-cause mortality and cardiovascular disease: a systematic review and meta-analysis. J Hypertens. 2017;35(1):10–17.doi:https://doi.org/10.1097/HJH.0000000000001159.
Wu S, Li Y, Jin C, et al. Intra-individual variability of high-sensitivity C-reactive protein in Chinese general population. Int J Cardiol. 2012;157(1):75–79.doi:https://doi.org/10.1016/j.ijcard.2010.12.019.
Wu Z, Jin C, Vaidya A, et al. Longitudinal Patterns of Blood Pressure, Incident Cardiovascular Events, and All-Cause Mortality in Normotensive Diabetic People. Hypertension. 2016;68(1):71–77.doi:https://doi.org/10.1161/HYPERTENSIONAHA.116.07381.
Wang G, Li N, Chang S, et al. A prospective follow-up study of the relationship between C-reactive protein and human cancer risk in the Chinese Kailuan Female Cohort. Cancer Epidemiol Biomarkers Prev. 2015;24(2):459–465.doi:https://doi.org/10.1158/1055-9965.EPI-14-1112.
Rognant N, Lemoine S, Laville M, Hadj-Aissa A, Dubourg L. Performance of the chronic kidney disease epidemiology collaboration equation to estimate glomerular filtration rate in diabetic patients. Diabetes Care. 2011;34(6):1320–1322.doi:https://doi.org/10.2337/dc11-0203.
Asayama K, Kikuya M, Schutte R, et al. Home blood pressure variability as cardiovascular risk factor in the population of Ohasama. Hypertension. 2013;61(1):61–69.doi:https://doi.org/10.1161/HYPERTENSIONAHA.111.00138.
Fukuda K, Kai H, Kamouchi M, et al. Day-by-Day Blood Pressure Variability and Functional Outcome After Acute Ischemic Stroke: Fukuoka Stroke Registry. Stroke. 2015;46(7):1832–1839.doi:https://doi.org/10.1161/STROKEAHA.115.009076.
Multidisciplinary Expert Task Force on H, Related D. Chinese Multidisciplinary Expert Consensus on the Diagnosis and Treatment of Hyperuricemia and Related Diseases. Chin Med J (Engl). 2017;130(20):2473–2488.doi:https://doi.org/10.4103/0366-6999.216416.
Brombo G, Bonetti F, Volpato S, et al. Uric acid within the “normal” range predict 9-year cardiovascular mortality in older individuals. The InCHIANTI study. Nutr Metab Cardiovasc Dis. 2019;29(10):1061–1067.doi:https://doi.org/10.1016/j.numecd.2019.06.018.
Virdis A, Masi S, Casiglia E, et al. Identification of the Uric Acid Thresholds Predicting an Increased Total and Cardiovascular Mortality Over 20 Years. Hypertension. 2020;75(2):302–308.doi:https://doi.org/10.1161/HYPERTENSIONAHA.119.13643.
Hoieggen A, Alderman MH, Kjeldsen SE, et al. The impact of serum uric acid on cardiovascular outcomes in the LIFE study. Kidney Int. 2004;65(3):1041–1049. doi:https://doi.org/10.1111/j.1523-1755.2004.00484.x.
Maiuolo J, Oppedisano F, Gratteri S, Muscoli C, Mollace V. Regulation of uric acid metabolism and excretion. Int J Cardiol. 2016;213:8–14.doi:https://doi.org/10.1016/j.ijcard.2015.08.109.
Dong ZX, Tian M, Li H, et al. Association of Serum Uric Acid Concentration and Its Change with Cardiovascular Death and All-Cause Mortality. Dis Markers. 2020;2020:7646384.doi:https://doi.org/10.1155/2020/7646384.
Lim SS, Yang YL, Chen SC, et al. Association of variability in uric acid and future clinical outcomes of patient with coronary artery disease undergoing percutaneous coronary intervention. Atherosclerosis. 2020;297:40–46.doi:https://doi.org/10.1016/j.atherosclerosis.2020.01.025.
Krzystek-Korpacka M, Patryn E, Kustrzeba-Wojcicka I, Chrzanowska J, Gamian A, Noczynska A. Gender-specific association of serum uric acid with metabolic syndrome and its components in juvenile obesity. Clin Chem Lab Med. 2011;49(1):129–136. doi:https://doi.org/10.1515/CCLM.2011.011.
McGorrian C, Yusuf S, Islam S, et al. Estimating modifiable coronary heart disease risk in multiple regions of the world: the INTERHEART Modifiable Risk Score. Eur Heart J. 2011;32(5):581–589.doi:https://doi.org/10.1093/eurheartj/ehq448.
Daiber A, Steven S, Weber A, et al. Targeting vascular (endothelial) dysfunction. Br J Pharmacol. 2017;174(12):1591–1619.doi:https://doi.org/10.1111/bph.13517.
Rizzo P, Miele L, Ferrari R. The Notch pathway: a crossroad between the life and death of the endothelium. Eur Heart J. 2013;34(32):2504–2509.doi:https://doi.org/10.1093/eurheartj/ehs141.
Esche J, Krupp D, Mensink GBM, Remer T. Dietary Potential Renal Acid Load Is Positively Associated with Serum Uric Acid and Odds of Hyperuricemia in the German Adult Population. J Nutr. 2018;148(1):49–55.doi:https://doi.org/10.1093/jn/nxx003.
Dolan E, O’Brien E. Blood pressure variability: clarity for clinical practice. Hypertension. 2010;56(2):179–181.doi:https://doi.org/10.1161/HYPERTENSIONAHA.110.154708.
Acknowledgement
The study was supported by the National Natural Science Foundation of China (No 8207020241). The authors thank all the contributions the staff of Kailuan Community Hospitals made to this study.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest: There was no conflict of interest to declare.
Ethical Standards: The Ethics Committee of the Kailuan hospital approved the study.
Rights and permissions
About this article
Cite this article
Wang, M., Wang, C., Zhao, M. et al. Uric Acid Variability and All-Cause Mortality: A Prospective Cohort Study in Northern China. J Nutr Health Aging 25, 1235–1240 (2021). https://doi.org/10.1007/s12603-021-1706-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-021-1706-3