Abstract
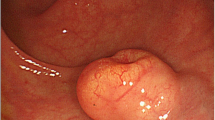
The presence of extramural tumor deposits without lymph node structure (EX) is an important prognostic factor in patients with colorectal carcinoma. However, there is no English literature on neuroendocrine tumor (NET) with EX. We report a patient with rectal NET with extracapsular metastasis of a regional lymph node that was considered to be EX. A 51-year-old Japanese woman with diabetes was referred to our hospital for further examination of a submucosal tumor in the lower rectum. She was diagnosed as having rectal NET by immunohistochemical analysis of a biopsy, and underwent laparoscopic low anterior resection with lymph node dissection and covering ileostomy. Pathological findings of the resected specimen showed that the primary tumor was NET-G1 without any lymphatic or venous invasion. A single metastatic deposit was found near the capsule of a NET-negative regional lymph node. She has been free from recurrence for nine months without adjuvant treatments. Extracapsular metastasis of NET on a dissected lymph node in our case was considered to correspond to EX as defined for colorectal carcinoma. This rare case suggests that NET can disseminate to form EX in a similar manner to colorectal carcinoma.






Similar content being viewed by others
References
Öberg K, Knigge U, Kwekkeboom D, et al. Neuroendocrine gastro-entero-pancreatic tumors: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2012;23:VII124–30.
Modlin IM, Lye KD, Kidd M. A 5-decade analysis of 13,715 carcinoid tumors. Cancer. 2003;97:934–59.
Ito T, Sasano H, Tanaka M, et al. Epidemiological study of gastroenteropancreatic neuroendocrine tumors in Japan. J Gastroenterol. 2010;45:234–43.
Masui T, Ito T, Komoto I, et al. Recent epidemiology of patients with gastro-entero-pancreatic neuroendocrine neoplasms (GEP-NEN) in Japan: a population-based study. BMC Cancer. 2020;20:1104.
NCCN Clinical Practice Guidelines in Oncology. Neuroendocrine tumor of the gastrointestinal tract, lung and thymus. Version 2; 2020.
Japan NeuroEndocrine Tumor Society (JNETS). Clinical Practice Guidelines for Gastroenteropancreatic Neuroendocrine Neoplasms (GEP-NEN) 2019. 2nd ed. Tokyo: KANEHARA & Co., LTD; 2019.
Konishi T, Watanabe T, Kishimoto J, et al. Prognosis and risk factors of metastasis in colorectal carcinoids: results of a nationwide registry over 15 years. Gut. 2007;56:863–8.
Zhou X, Xie H, Xie L, et al. Factors associated with lymph node metastasis in radically resected rectal carcinoids: a systematic review and meta-analysis. J Gastrointest Surg. 2013;17:1689–97.
Shields CJ, Tiret E, Winter DC, International Rectal Carcinoid Study Group. Carcinoid tumors of the rectum: a multi-institutional international collaboration. Ann Surg. 2010;252:750–5.
Sohn B, Kwon Y, Ryoo SB, et al. Predictive factors for lymph node metastasis and prognostic factors for survival in rectal neuroendocrine tumors. J Gastrointest Surg. 2017;21:2066–74.
Brierley JD, Gospodarowicz M, Wittekind C. TNM classification of malignant tumours. 8th ed. Oxford: Wiley-Blackwell; 2017.
Ueno H, Mochizuki H, Shirouzu K, et al. Actual status of distribution and prognostic impact of extramural discontinuous cancer spread in colorectal cancer. J Clin Oncol. 2011;29:2550–6.
Japanese Society for Cancer of the Colon and Rectum. Japanese classification of colorectal, appendiceal and anal carcinoma: the 3d English Edition. J Anus Rectum Colon. 2019;3:175–95.
Nagtegaal ID, Odze RD, Klimstra D, et al. The 2019 WHO classification of tumours of the digestive system. Histopathology. 2020;76:182–8.
Soga J. Carcinoids of the rectum: an evaluation of 1271 reported cases. Surg Today. 1997;27:112–9.
Prabhudesai A, Arif S, Finlayson CJ, Kumar D. Impact of microscopic extranodal tumor deposits on the outcome of patients with rectal cancer. Dis Colon Rectum. 2003;46:1531–7.
Kimura K, Yamano T, Matsuda I, et al. Multiple rectal neuroendocrine tumors with recurrence of inguinal lymph nodes. Jpn J Gastroenterol Surg. 2018;51:170–7.
Klöppel G, Couvelard A, Perren A, et al. ENETS consensus guidelines for the standard care in neuroendocrine tumors: towards a standardized approach to the diagnosis of gastroenteropancreatic neuroendocrine tumors and their prognostic stratification. Neuroendocrinology. 2009;90:162–6.
Ramage JK, De Herder WW, Delle Fave G, et al. ENETS consensus guidelines update for colorectal neuroendocrine neoplasms. Neuroendocrinology. 2016;103:139–43.
Frilling A, Clift AK. Therapeutic strategies for neuroendocrine liver metastasis. Cancer. 2015;121:1172–86.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors contributed to this work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Consent to participate
Informed consent was obtained from the participant included in the study.
Consent for publication
The patient has consented to the submission of the case report for submission to the journal.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sakamoto, A., Nozawa, H., Sonoda, H. et al. Rectal neuroendocrine tumor with extracapsular lymph node metastasis: a case report. Clin J Gastroenterol 14, 1426–1430 (2021). https://doi.org/10.1007/s12328-021-01447-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-021-01447-x