Abstract
Background
Transmembrane protein 92 (TMEM92) has been implicated in the facilitation of tumor progression. Nevertheless, comprehensive analyses concerning the prognostic significance of TMEM92, as well as its role in immunological responses across diverse cancer types, remain to be elucidated.
Methods
In this study, data was sourced from a range of publicly accessible online platforms and databases, including TCGA, GTEx, UCSC Xena, CCLE, cBioPortal, HPA, TIMER2.0, GEPIA, CancerSEA, GDSC, exoRBase, and ImmuCellAI. We systematically analyzed the expression patterns of TMEM92 at both mRNA and protein levels across diverse human organs, tissues, extracellular vesicles (EVs), and cell lines associated with multiple cancer types. Subsequently, analyses were conducted to determine the relationship between TMEM92 and various parameters such as prognosis, DNA methylation, copy number variation (CNV), the tumor microenvironment (TME), immune cell infiltration, genes with immunological relevance, tumor mutational burden (TMB), microsatellite instability (MSI), mismatch repair (MMR), and half-maximal inhibitory concentration (IC50) values.
Results
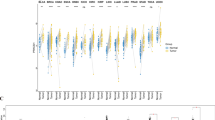
In the present study, we observed a pronounced overexpression of TMEM92 across a majority of cancer types, which was concomitantly associated with a less favorable prognosis. A notable association emerged between TMEM92 expression and both DNA methylation and CNV. Furthermore, a pronounced relationship was discerned between TMEM92 expression, the TME, and the degree of immune cell infiltration. Intriguingly, while TMEM92 expression displayed a positive correlation with macrophage presence, it inversely correlated with the infiltration level of CD8 + T cells. Concurrently, significant associations were identified between TMEM92 and the major histocompatibility complex, TMB, MSI, and MMR. Results derived from Gene Set Enrichment Analysis and Gene Set Variation Analysis further substantiated the nexus of TMEM92 with both immune and metabolic pathways within the oncogenic context.
Conclusions
These findings expanded the understanding of the roles of TMEM92 in tumorigenesis and progression and suggest that TMEM92 may have an immunoregulatory role in several malignancies.









Similar content being viewed by others
Data availability
All data generated or analysed during this study are included in this article. Further enquiries can be directed to the corresponding author.
Abbreviations
- ACC:
-
Adrenocortical carcinoma
- BLCA:
-
Bladder urothelial carcinoma
- BRCA:
-
Breast invasive carcinoma
- CESC:
-
Cervical squamous cell carcinoma and endocervical adenocarcinoma
- CHOL:
-
Cholangio carcinoma
- COAD:
-
Colon adenocarcinoma
- DLBC:
-
Lymphoid neoplasm diffuse large B-cell lymphoma
- ESCA:
-
Esophageal carcinoma
- ESCC:
-
Esophageal squamous cell carcinoma
- GBM:
-
Glioblastoma multiforme
- HNSC:
-
Head and neck squamous cell carcinoma
- KICH:
-
Kidney chromophobe
- KIRC:
-
Kidney renal clear cell carcinoma
- KIRP:
-
Kidney renal papillary cell carcinoma
- LAML:
-
Acute myeloid leukemia
- LGG:
-
Brain lower grade glioma
- LIHC:
-
Liver hepatocellular carcinoma
- LUAD:
-
Lung adenocarcinoma
- LUSC:
-
Lung squamous cell carcinoma
- MEL:
-
Melanoma
- MESO:
-
Mesothelioma
- OV:
-
Ovarian serous cystadenocarcinoma
- PAAD:
-
Pancreatic adenocarcinoma
- PCPG:
-
Pheochromocytoma and paraganglioma
- PRAD:
-
Prostate adenocarcinoma
- READ:
-
Rectum adenocarcinoma
- SKCM:
-
Skin cutaneous melanoma
- TGCT:
-
Testicular germ cell tumors
- THCA:
-
Thyroid carcinoma
- THYM:
-
Thymoma
- UCEC:
-
Uterine corpus endometrial carcinoma
- UCS:
-
Uterine carcinosarcoma
- UVM:
-
Uveal melanoma
References
Global Burden of Disease Cancer C, Kocarnik JM, Compton K, Dean FE, Fu W, Gaw BL, et al. Cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life years for 29 cancer groups from 2010 to 2019: a systematic analysis for the Global Burden of Disease Study 2019. JAMA Oncol. 2022;8(3):420–44. https://doi.org/10.1001/jamaoncol.2021.6987.
Saw PE, Chen J, Song E. Targeting CAFs to overcome anticancer therapeutic resistance. Trends Cancer. 2022;8(7):527–55. https://doi.org/10.1016/j.trecan.2022.03.001.
Schmit K, Michiels C. TMEM proteins in cancer: a review. Front Pharmacol. 2018;9:1345. https://doi.org/10.3389/fphar.2018.01345.
Zhao Y, Zhang K, Pan H, Wang Y, Zhou X, Xiang Y, et al. Genetic analysis of six transmembrane protein family genes in Parkinson’s disease in a large Chinese cohort. Front Aging Neurosci. 2022;14: 889057. https://doi.org/10.3389/fnagi.2022.889057.
Hayez A, Malaisse J, Roegiers E, Reynier M, Renard C, Haftek M, et al. High TMEM45A expression is correlated to epidermal keratinization. Exp Dermatol. 2014;23(5):339–44. https://doi.org/10.1111/exd.12403.
Lipinski P, Stepien KM, Ciara E, Tylki-Szymanska A, Jezela-Stanek A. Skeletal and bone mineral density features, genetic profile in congenital disorders of glycosylation: review. Diagnostics (Basel). 2021;11(8):1438. https://doi.org/10.3390/diagnostics11081438.
Deng H, Li T, Wei F, Han W, Xu X, Zhang Y. High expression of TMEM200A is associated with a poor prognosis and immune infiltration in gastric cancer. Pathol Oncol Res. 2023;29:1610893. https://doi.org/10.3389/pore.2023.1610893.
Rao J, Wu X, Zhou X, Deng R, Ma Y. TMEM205 Is an independent prognostic factor and is associated with immune cell infiltrates in hepatocellular carcinoma. Front Genet. 2020;11: 575776. https://doi.org/10.3389/fgene.2020.575776.
Du Y, Zeng X, Yu W, Xie W. A transmembrane protein family gene signature for overall survival prediction in osteosarcoma. Front Genet. 2022;13: 937300. https://doi.org/10.3389/fgene.2022.937300.
Pei J, Grishin NV. Unexpected diversity in Shisa-like proteins suggests the importance of their roles as transmembrane adaptors. Cell Signal. 2012;24(3):758–69. https://doi.org/10.1016/j.cellsig.2011.11.011.
Listing H, Mardin WA, Wohlfromm S, Mees ST, Haier J. MiR-23a/-24-induced gene silencing results in mesothelial cell integration of pancreatic cancer. Br J Cancer. 2015;112(1):131–9. https://doi.org/10.1038/bjc.2014.587.
Zhang S, Wan X, Lv M, Li C, Chu Q, Wang G. TMEM92 acts as an immune-resistance and prognostic marker in pancreatic cancer from the perspective of predictive, preventive, and personalized medicine. EPMA J. 2022;13(3):519–34. https://doi.org/10.1007/s13167-022-00287-0.
Lin MZ, Teng LL, Sun XL, Zhang LP, Chen F, Yu LJ. Transmembrane protein 92 performs a tumor-promoting function in breast carcinoma by contributing to the cell growth, invasion, migration and epithelial-mesenchymal transition. Tissue Cell. 2020;67: 101415. https://doi.org/10.1016/j.tice.2020.101415.
Zeng D, Li M, Zhou R, Zhang J, Sun H, Shi M, et al. Tumor microenvironment characterization in gastric cancer identifies prognostic and immunotherapeutically relevant gene signatures. Cancer Immunol Res. 2019;7(5):737–50. https://doi.org/10.1158/2326-6066.CIR-18-0436.
Yoshihara K, Shahmoradgoli M, Martinez E, Vegesna R, Kim H, Torres-Garcia W, et al. Inferring tumour purity and stromal and immune cell admixture from expression data. Nat Commun. 2013;4:2612. https://doi.org/10.1038/ncomms3612.
Thorsson V, Gibbs DL, Brown SD, Wolf D, Bortone DS, Ou Yang TH, et al. The immune landscape of cancer. Immunity. 2018;48(4):812–30e14. https://doi.org/10.1016/j.immuni.2018.03.023.
Bonneville R, Krook MA, Kautto EA, Miya J, Wing MR, Chen HZ, et al. Landscape of microsatellite instability across 39 cancer types. JCO Precis Oncol. 2017;2017: PO.17.00073. https://doi.org/10.1200/PO.17.00073.
Bilotta MT, Antignani A, Fitzgerald DJ. Managing the TME to improve the efficacy of cancer therapy. Front Immunol. 2022;13: 954992. https://doi.org/10.3389/fimmu.2022.954992.
Zhang Y, Zhang Z. The history and advances in cancer immunotherapy: understanding the characteristics of tumor-infiltrating immune cells and their therapeutic implications. Cell Mol Immunol. 2020;17(8):807–21. https://doi.org/10.1038/s41423-020-0488-6.
He Y, Zhang L, Zhou R, Wang Y, Chen H. The role of DNA mismatch repair in immunotherapy of human cancer. Int J Biol Sci. 2022;18(7):2821–32. https://doi.org/10.7150/ijbs.71714.
Yang W, Soares J, Greninger P, Edelman EJ, Lightfoot H, Forbes S, et al. Genomics of drug sensitivity in cancer (GDSC): a resource for therapeutic biomarker discovery in cancer cells. Nucleic Acids Res. 2013;41(Database issue):D955–61. https://doi.org/10.1093/nar/gks1111.
Ushijima T, Clark SJ, Tan P. Mapping genomic and epigenomic evolution in cancer ecosystems. Science. 2021;373(6562):1474–9. https://doi.org/10.1126/science.abh1645.
Huang W, Li H, Yu Q, Xiao W, Wang DO. LncRNA-mediated DNA methylation: an emerging mechanism in cancer and beyond. J Exp Clin Cancer Res. 2022;41(1):100. https://doi.org/10.1186/s13046-022-02319-z.
Anderson NM, Simon MC. The tumor microenvironment. Curr Biol. 2020;30(16):R921–5. https://doi.org/10.1016/j.cub.2020.06.081.
Dongre A, Weinberg RA. New insights into the mechanisms of epithelial-mesenchymal transition and implications for cancer. Nat Rev Mol Cell Biol. 2019;20(2):69–84. https://doi.org/10.1038/s41580-018-0080-4.
Wang Y, Li W, Jin X, Jiang X, Guo S, Xu F, et al. Identification of prognostic immune-related gene signature associated with tumor microenvironment of colorectal cancer. BMC Cancer. 2021;21(1):905. https://doi.org/10.1186/s12885-021-08629-3.
Halle S, Halle O, Forster R. Mechanisms and dynamics of T cell-mediated cytotoxicity in vivo. Trends Immunol. 2017;38(6):432–43. https://doi.org/10.1016/j.it.2017.04.002.
Oh DY, Fong L. Cytotoxic CD4(+) T cells in cancer: expanding the immune effector toolbox. Immunity. 2021;54(12):2701–11. https://doi.org/10.1016/j.immuni.2021.11.015.
Tie Y, Tang F, Wei YQ, Wei XW. Immunosuppressive cells in cancer: mechanisms and potential therapeutic targets. J Hematol Oncol. 2022;15(1):61. https://doi.org/10.1186/s13045-022-01282-8.
Palmeri M, Mehnert J, Silk AW, Jabbour SK, Ganesan S, Popli P, et al. Real-world application of tumor mutational burden-high (TMB-high) and microsatellite instability (MSI) confirms their utility as immunotherapy biomarkers. ESMO Open. 2022;7(1): 100336. https://doi.org/10.1016/j.esmoop.2021.100336.
Cristescu R, Aurora-Garg D, Albright A, Xu L, Liu XQ, Loboda A, et al. Tumor mutational burden predicts the efficacy of pembrolizumab monotherapy: a pan-tumor retrospective analysis of participants with advanced solid tumors. J Immunother Cancer. 2022;10(1): e003091. https://doi.org/10.1136/jitc-2021-003091.
Chakrabarti S, Bucheit L, Starr JS, Innis-Shelton R, Shergill A, Dada H, et al. Detection of microsatellite instability-high (MSI-H) by liquid biopsy predicts robust and durable response to immunotherapy in patients with pancreatic cancer. J Immunother Cancer. 2022;10(6): e004485. https://doi.org/10.1136/jitc-2021-004485.
Dawson JC, Serrels A, Stupack DG, Schlaepfer DD, Frame MC. Targeting FAK in anticancer combination therapies. Nat Rev Cancer. 2021;21(5):313–24. https://doi.org/10.1038/s41568-021-00340-6.
Acknowledgements
We would like to acknowledge the hard and dedicated work of all the staff that implemented the intervention and evaluation components of the study.
Funding
This study was funded by Natural Science Foundation of Hebei Province (No. H2022206221) Medical science research project of Hebei Province (No. 20240095)
Author information
Authors and Affiliations
Contributions
Conception and design of the research: Wu Z, Wang ZY. Acquisition of data: Zhang YH, Guo SH, Liu Y. Analysis and interpretation of the data: Liu Y, Zhang L, Li W. Statistical analysis: Guo SH, Liu Y. Obtaining financing: Wu Z. Writing of the manuscript: Wu Z, Pan T. Critical revision of the manuscript for intellectual content: Li W, Zhang YH, Wang ZY. All authors read and approved the final draft.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, Z., Pan, T., Li, W. et al. Comprehensive pan-cancer analysis reveals prognostic implications of TMEM92 in the tumor immune microenvironment. Clin Transl Oncol (2024). https://doi.org/10.1007/s12094-024-03477-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12094-024-03477-6