Abstract
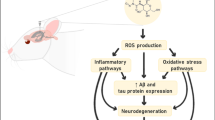
Dementia is the most common age-related problem due predominantly to Alzheimer’s disease (AD) and vascular dementia (VaD). It has been shown that these contributors are associated with a high amount of oxidative stress that leads to changes in neurological function and cognitive impairment. The aim of study was to explore the mechanism by which hexahydrocurcumin (HHC) attenuates oxidative stress, amyloidogenesis, phosphorylated Tau (pTau) expression, neuron synaptic function, and cognitive impairment and also the potential mechanisms involved in induced permanent occlusion of bilateral common carotid arteries occlusion (BCCAO) or 2-vessel occlusion (2VO) in rats. After surgery, rats were treated with HHC (40 mg/kg) or piracetam (600 mg/kg) by oral gavage daily for 4 weeks. The results showed that HHC or piracetam attenuated oxidative stress by promoting nuclear factor erythroid 2-related factor 2 (Nrf2) activity, and alleviated expression of synaptic proteins (pre- and post-synaptic proteins) mediated by the Wingless/Integrated (Wnt)/β-catenin signaling pathway. Moreover, HHC or piracetam also improved synaptic plasticity via the brain-derived neurotrophic factor (BDNF)/Tyrosine receptor kinase B (TrkB)/cAMP responsive element binding protein (CREB) signaling pathway. In addition, HHC reduced amyloid beta (Aβ) production and pTau expression and improved memory impairment as evidenced by the Morris water maze. In conclusion, HHC exerted remarkable improvement in cognitive function in the 2VO rats possibly via the attenuation of oxidative stress, improvement in synaptic function, attenuation of amyloidogenesis, pTau, and neuronal injury, thereby improving cognitive performance.
Graphical Abstract








Similar content being viewed by others
Data Availability
The datasets generated and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Abbreviations
- 2VO:
-
The 2-vessel occlusion
- 4-HNE:
-
4-Hydroxynonenal
- Aβ:
-
Amyloid-beta
- AChE:
-
Acetylcholinesterase
- AD:
-
Alzheimer’s disease
- BCCAO:
-
Bilateral common carotid artery occlusion
- BDNF:
-
Brain-derived neurotrophic factor
- BuChE:
-
Butyrylcholinesterase
- BW:
-
Body weight
- CBF:
-
Cerebral blood flow
- CCA:
-
Common carotid arteries
- CCH:
-
Chronic cerebral hypoperfusion
- CREB:
-
CAMP responsive element binding protein
- GAP43:
-
Growth Associated Protein 43
- GLUTs:
-
Glucose transporter
- GSK3β:
-
Glycogen synthase kinase-3 beta
- HHC:
-
Hexahydrocurcumin
- HIFs:
-
Hypoxia-inducible factor 1
- MWM:
-
Morris water maze test
- Nrf2:
-
Nuclear factor erythroid 2-related factor 2
- PARP1:
-
Poly (ADP-ribose) polymerase-1
- PSD95:
-
Postsynaptic protein density 95
- SOD:
-
Superoxide dismutase
- SYN:
-
Synaptophysin
- TrkB:
-
Tyrosine receptor kinase B
- VaD:
-
Vascular dementia
- Wnts:
-
Wingless/Integrated
References
Arvanitakis Z, Shah RC, Bennett DA (2019) Diagnosis and management of dementia. JAMA 322(16):1589–1599. https://doi.org/10.1001/jama.2019.4782
Majdi A, Sadigh-Eteghad S, Aghsan SR, Farajdokht F, Vatandoust SM, Namvaran A, Mahmoudi J (2020) Amyloid-β, tau, and the cholinergic system in Alzheimer’s disease: seeking direction in a tangle of clues. Rev Neurosci 31(4):391–413. https://doi.org/10.1515/revneuro-2019-0089
Attems J, Jellinger KA (2014) The overlap between vascular disease and Alzheimer’s disease-lessons from pathology. BMC Med 12(1):1–12. https://doi.org/10.1186/s12916-014-0206-2
Tayler H, Miners JS, Güzel Ö, MacLachlan R, Love S (2021) Mediators of cerebral hypoperfusion and blood-brain barrier leakiness in Alzheimer’s disease, vascular dementia and mixed dementia. Brain Pathol 31(4):e12935. https://doi.org/10.1111/bpa.12935
Román GC (2022) Vascular dementia revisited: diagnosis, pathogenesis, treatment, and prevention. Med Clin North Am 86(3):477–499. https://doi.org/10.1016/s0025-7125(02)00008-1
Wang X, Xing A, Xu C, Cai Q, Liu H, Li L (2010) Cerebrovascular hypoperfusion induces spatial memory impairment, synaptic changes, and amyloid-β oligomerization in rats. J Alzheimers Dis 21(3):813–822. https://doi.org/10.3233/JAD-2010-100216
Sigfridsson E, Marangoni M, Hardingham GE, Horsburgh K, Fowler JH (2020) Deficiency of Nrf2 exacerbates white matter damage and microglia/macrophage levels in a mouse model of vascular cognitive impairment. J Neuroinflammation 17(1):1–15. https://doi.org/10.1186/s12974-020-02038-2
Yan N, Xu Z, Qu C, Zhang J (2021) Dimethyl fumarate improves cognitive deficits in chronic cerebral hypoperfusion rats by alleviating inflammation, oxidative stress, and ferroptosis via NRF2/ARE/NF-κB signal pathway. Int Immunopharmacol 98:107844. https://doi.org/10.1016/j.intimp.2021.107844
Yang Y, Zhang J, Liu H, Wang J, Xin J, Deng M (2013) Changes in levels of hypoxia-induced mediators in rat hippocampus during chronic cerebral hypoperfusion. Neurochem Res 38(11):2433–2439. https://doi.org/10.1007/s11064-013-1158-1
Zhao Y, Gu J-h, Dai C-l, Liu Q, Iqbal K, Liu F, Gong C-X (2014) Chronic cerebral hypoperfusion causes decrease of O-GlcNAcylation, hyperphosphorylation of tau and behavioral deficits in mice. Front Aging Neurosci 6:10. https://doi.org/10.3389/fnagi.2014.00010
Zhao Y, Gong C-X (2015) From chronic cerebral hypoperfusion to Alzheimer-like brain pathology and neurodegeneration. Cell Mol Neurobiol 35(1):101–110. https://doi.org/10.1007/s10571-014-0127-9
Martinez M, Torres VI, Vio CP, Inestrosa NC (2020) Canonical Wnt signaling modulates the expression of pre-and postsynaptic components in different temporal patterns. Mol Neurobiol 57(3):1389–1404. https://doi.org/10.1007/s12035-019-01785-5
Sun F-L, Wang W, Zuo W, Xue J-L, Xu J-d, Ai H-X, Zhang L, Wang X-M et al (2014) Promoting neurogenesis via Wnt/β-catenin signaling pathway accounts for the neurorestorative effects of morroniside against cerebral ischemia injury. Eur J Pharmacol 738:214–221. https://doi.org/10.1016/j.ejphar.2014.05.019
Shruster A, Ben-Zur T, Melamed E, Offen D (2012) Wnt signaling enhances neurogenesis and improves neurological function after focal ischemic injury. PLoS ONE 7(7):e40843. https://doi.org/10.1371/journal.pone.0040843
Inestrosa NC, Varela-Nallar L (2014) Wnt signaling in the nervous system and in Alzheimer’s disease. J Mol Cell Biol 6(1):64–74. https://doi.org/10.1093/jmcb/mjt051
Kim M-S, Bang J, Jeon WK (2020) The involvement of canonical Wnt signaling in memory impairment induced by chronic cerebral hypoperfusion in mice. Transl Stroke Res 11(4):734–746. https://doi.org/10.1007/s12975-019-00748-1
Somparn P, Phisalaphong C, Nakornchai S, Unchern S, Morales NP (2007) Comparative antioxidant activities of curcumin and its demethoxy and hydrogenated derivatives. Biol Pharm Bull 30(1):74–78. https://doi.org/10.1248/bpb.30.74
Kocaadam B, Şanlier N (2017) Curcumin, an active component of turmeric (Curcuma longa), and its effects on health. Crit Rev Food Sci Nutr 57(13):2889–95. https://doi.org/10.1080/10408398.2015.1077195
Huang Y, Cao S, Zhang Q, Zhang H, Fan Y, Qiu F, Kang N (2018) Biological and pharmacological effects of hexahydrocurcumin, a metabolite of curcumin. Arch Biochem Biophys 646:31–37. https://doi.org/10.1016/j.abb.2018.03.030
Thangwong P, Jearjaroen P, Govitrapong P, Tocharus C, Tocharus J (2022) Melatonin improves cognitive function by suppressing endoplasmic reticulum stress and promoting synaptic plasticity during chronic cerebral hypoperfusion in rats. Biochem Pharmacol 198:114980. https://doi.org/10.1016/j.bcp.2022.114980
Bartorelli L, Giraldi C, Saccardo M, Cammarata S, Bottini G, Fasanaro A, Trequattrini A (2005) Effects of switching from an AChE inhibitor to a dual AChE-BuChE inhibitor in patients with Alzheimer’s disease. Curr Med Res Opin 21(11):1809–1817. https://doi.org/10.1185/030079905X65655
Changtam C, de Koning HP, Ibrahim H, Sajid MS, Gould MK, Suksamrarn A (2010) Curcuminoid analogs with potent activity against Trypanosoma and Leishmania species. Eur J Med Chem 45(3):941–56. https://doi.org/10.1016/j.ejmech.2009.11.035
Lee S-L, Huang W-J, Lin WW, Lee S-S, Chen C-H (2005) Preparation and anti-inflammatory activities of diarylheptanoid and diarylheptylamine analogs. Bioorg Med Chem 13(22):6175–6181. https://doi.org/10.1016/j.bmc.2005.06.058
Vorhees CV, Williams MT (2006) Morris water maze: procedures for assessing spatial and related forms of learning and memory. Nat Protoc 1(2):848–858. https://doi.org/10.1038/nprot.2006.116
Ellman GL, Courtney KD, Andres V Jr, Featherstone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7(2):88–95. https://doi.org/10.1016/0006-2952(61)90145-9
Ciacciarelli A, Sette G, Giubilei F, Orzi F (2020) Chronic cerebral hypoperfusion: an undefined, relevant entity. J Clin Neurosci 73:8–12. https://doi.org/10.1016/j.jocn.2020.01.026
Liu Z, Hu M, Lu P, Wang H, Qi Q, Xu J, Xiao Y, Fan M et al (2017) Cerebrolysin alleviates cognitive deficits induced by chronic cerebral hypoperfusion by increasing the levels of plasticity-related proteins and decreasing the levels of apoptosis-related proteins in the rat hippocampus. Neurosci Lett 651:72–78. https://doi.org/10.1016/j.neulet.2017.04.022
Zhang N, Song C, Zhao B, Xing M, Luo L, Gordon ML, Cheng Y (2017) Neovascularization and synaptic function regulation with memantine and rosuvastatin in a rat model of chronic cerebral hypoperfusion. J Mol Neurosci 63(2):223–232. https://doi.org/10.1007/s12031-017-0974-1
Jearjaroen P, Pakdeepak K, Tocharus C, Chaichompoo W, Suksamrarn A, Tocharus J (2021) Inhibitory effect of hexahydrocurcumin on memory impairment and amyloidogenesis in dexamethasone-treated mice. Neurotox Res 39(2):266–276. https://doi.org/10.1007/s12640-020-00269-y
Wicha P, Tocharus J, Janyou A, Jittiwat J, Chaichompoo W, Suksamrarn A, Tocharus C (2020) Hexahydrocurcumin alleviated blood–brain barrier dysfunction in cerebral ischemia/reperfusion rats. Pharmacol Rep 72:659–671. https://doi.org/10.1007/s43440-019-00050-9
Orsucci D, Mancuso M, CaldarazzoIenco E, Simoncini C, Siciliano G, Bonuccelli U (2013) Vascular factors and mitochondrial dysfunction: a central role in the pathogenesis of Alzheimer’s disease. Curr Neurovasc Res 10(1):76–80. https://doi.org/10.2174/156720213804805972
Lee J-W, Bae S-H, Jeong J-W, Kim S-H, Kim K-W (2004) Hypoxia-inducible factor (HIF-1) α: its protein stability and biological functions. Exp Mol Med 36(1):1–12. https://doi.org/10.1038/emm.2004.1
Ren C, Liu Y, Stone C, Li N, Li S, Li H, Cheng Z, Hu J et al (2021) Limb remote ischemic conditioning ameliorates cognitive impairment in rats with chronic cerebral hypoperfusion by regulating glucose transport. Aging Dis 12(5):1197. https://doi.org/10.14336/AD.2020.1125
Singh N, Sharma G, Mishra V, Raghubir R (2012) Hypoxia inducible factor-1: its potential role in cerebral ischemia. Cell Mol Neurobiol 32(4):491–507. https://doi.org/10.1007/s10571-012-9803-9
Du S-Q, Wang X-R, Xiao L-Y, Tu J-F, Zhu W, He T, Liu C-Z (2017) Molecular mechanisms of vascular dementia: what can be learned from animal models of chronic cerebral hypoperfusion? Mol Neurobiol 54(5):3670–3682. https://doi.org/10.1007/s12035-016-9915-1
Wicha P, Tocharus J, Janyou A, Jittiwat J, Changtam C, Suksamrarn A, Tocharus C (2017) Hexahydrocurcumin protects against cerebral ischemia/reperfusion injury, attenuates inflammation, and improves antioxidant defenses in a rat stroke model. PLoS ONE 12(12):e0189211. https://doi.org/10.1371/journal.pone.0189211
Zhang R, Zhang Z, Chopp M (2016) Function of neural stem cells in ischemic brain repair processes. J Cereb Blood Flow Metab 36(12):2034–2043. https://doi.org/10.1177/0271678X16674487
Zhang X, Shi X, Wang J, Xu Z, He J (2021) Enriched environment remedies cognitive dysfunctions and synaptic plasticity through NMDAR-Ca2+-activin A circuit in chronic cerebral hypoperfusion rats. Aging (Albany NY) 13(16):20748. https://doi.org/10.18632/aging.203462
Strittmatter SM, Vartanian T, Fishman MC (1992) GAP-43 as a plasticity protein in neuronal form and repair. J Neurobiol 23(5):507–520. https://doi.org/10.1002/neu.480230506
Liu HX, Zhang JJ, Zheng P, Zhang Y (2005) Altered expression of MAP-2, GAP-43, and synaptophysin in the hippocampus of rats with chronic cerebral hypoperfusion correlates with cognitive impairment. Brain Res Mol Brain Res 139(1):169–177. https://doi.org/10.1016/j.molbrainres.2005.05.014
Smith SE, Figley SA, Schreyer DJ, Paterson PG (2014) Protein-energy malnutrition developing after global brain ischemia induces an atypical acute-phase response and hinders expression of GAP-43. PLoS ONE 9(9):e107570. https://doi.org/10.1371/journal.pone.0107570
Zuliani G, Trentini A, Rosta V, Guerrini R, Pacifico S, Bonazzi S, Guiotto A, Passaro A et al (2020) Increased blood BACE1 activity as a potential common pathogenic factor of vascular dementia and late onset Alzheimer’s disease. Sci Rep 10(1):1–8. https://doi.org/10.1038/s41598-020-72168-3
Zhiyou C, Yong Y, Shanquan S, Jun Z, Liangguo H, Ling Y, Jieyin L (2009) Upregulation of BACE1 and β-amyloid protein mediated by chronic cerebral hypoperfusion contributes to cognitive impairment and pathogenesis of Alzheimer’s disease. Neurochem Res 34(7):1226–1235. https://doi.org/10.1007/s11064-008-9899-y
Li J-F, Wang Z, Sun Q-J, Du Y-F (2015) Expression of tau protein in rats with cognitive dysfunction induced by cerebral hypoperfusion. Int J Clin Exp Med 8(10):19682
Zhang X, Zhou K, Wang R, Cui J, Lipton SA, Liao F-F, Xu H, Zhang Y-w (2007) Hypoxia-inducible factor 1α (HIF-1α)-mediated hypoxia increases BACE1 expression and β-amyloid generation. J Biol Chem 282(15):10873–80. https://doi.org/10.1074/jbc.M608856200
Liu F, Shi J, Tanimukai H, Gu J, Gu J, Grundke-Iqbal I, Iqbal K, Gong C-X (2009) Reduced O-GlcNAcylation links lower brain glucose metabolism and tau pathology in Alzheimer’s disease. Brain 132(7):1820–1832. https://doi.org/10.1093/brain/awp099
Ray Chaudhuri A, Nussenzweig A (2017) The multifaceted roles of PARP1 in DNA repair and chromatin remodelling. Nat Rev Mol Cell Biol 18(10):610–621. https://doi.org/10.1038/nrm.2017.53
Chaitanya GV, Alexander JS, Babu PP (2010) PARP-1 cleavage fragments: signatures of cell-death proteases in neurodegeneration. Cell Commun Signal 8(1):1–11. https://doi.org/10.1186/1478-811X-8-31
McAllister AK, Katz LC, Lo DC (1999) Neurotrophins and synaptic plasticity. Annu Rev Neurosci 22(1):295–318. https://doi.org/10.1146/annurev.neuro.22.1.295
Yamada K, Nabeshima T (2003) Brain-derived neurotrophic factor/TrkB signaling in memory processes. J Pharmacol Sci 91(4):267–270. https://doi.org/10.1254/jphs.91.267
Ohira K, Hayashi M (2009) A new aspect of the TrkB signaling pathway in neural plasticity. Curr Neuropharmacol 7(4):276–285. https://doi.org/10.2174/157015909790031210
Yin C, Deng Y, Liu Y, Gao J, Yan L, Gong Q (2018) Icariside II ameliorates cognitive impairments induced by chronic cerebral hypoperfusion by inhibiting the amyloidogenic pathway: involvement of BDNF/TrkB/CREB signaling and up-regulation of PPARα and PPARγ in rats. Front Pharmacol 9:1211. https://doi.org/10.3389/fphar.2018.01211
Wang J, Zhang HY, Tang XC (2009) Cholinergic deficiency involved in vascular dementia: possible mechanism and strategy of treatment. Acta Pharmacol Sin 30(7):879–888. https://doi.org/10.1038/aps.2009.82
Damodaran T, Müller CP, Hassan Z (2019) Chronic cerebral hypoperfusion-induced memory impairment and hippocampal long-term potentiation deficits are improved by cholinergic stimulation in rats. Pharmacol Rep 71(3):443–448. https://doi.org/10.1016/j.pharep.2019.01.012
Funding
This work was supported by the Royal Golden Jubilee Ph.D. program (NRCT5-RGJ63004-076) and Thailand Science Research and Innovation (TSRI) (RUG6290031), Thailand. Partial support from the Center of Excellence for Innovation in Chemistry (PERCH-CIC), Ministry of Higher Education, Science, Research and Innovation is gratefully acknowledged.
Author information
Authors and Affiliations
Contributions
Pranglada Jearjaroen: Conducted the experiments, performed data analysis, writing – original draft, review & editing. Phakkawat Thangwong: conducted the experiments. Chainarong Tocharus: Performed data analysis, writing – original draft, review & editing. Anusorn Lungkaphin: writing – review & editing. Waraluck Chaichompoo: Preparation of hexahydrocurcumin. Jaranwit Srijun: Preparation of hexahydrocurcumin. Apichart Suksamrarn: Preparation of hexahydrocurcumin, writing – review & editing. Jiraporn Tocharus: Conceived and designed the experiments, performed data analysis, writing – original draft, review & editing, project administration.
Corresponding author
Ethics declarations
Ethical Approval
The experimental procedures were approved by the Institutional Animal Care and Use Committee of the Faculty of Medicine, Chiang Mai University (31/2563) corresponding to the guidelines established by National Institutes of Health (NIH).
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Conflict of Interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jearjaroen, P., Thangwong, P., Tocharus, C. et al. Hexahydrocurcumin Attenuates Neuronal Injury and Modulates Synaptic Plasticity in Chronic Cerebral Hypoperfusion in Rats. Mol Neurobiol (2023). https://doi.org/10.1007/s12035-023-03821-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12035-023-03821-x