Abstract
Aims
Epidermal Neural Crest Stem Cells (EPI-NCSCs) have emerged as prospective ideal candidates to meet the fundamental requirements of cell-based therapies in neurodegenerative disorders. The present study aimed to identify the potential of metformin in driving EPI-NCSCs to neuronal/glial differentiation and express neurotrophic factors as well as assess their therapeutic potential for mitigating the main behavioral manifestations of chemotherapy-induced neurotoxicity (CIN).
Main Methods
EPI-NCSCs were extracted from the bulge region of hair follicle. Following expansion, transcript and protein expression profiles of key markers for stemness (Nestin, EGR-1, SOX-2 and 10), neurotrophic activity (BDNF, GDNF, NGF, FGF-2, and IL-6), and neuronal (TUB3, DCX, NRF and NeuN) and glial (PDGFRα, NG2, GFAP, and MBP) differentiation were determined on days 1 and 7 post-treatment with 10 and 100 μM metformin using real time-PCR and immunocytochemistry methods. Then, the in vivo function of metformin-treated stem cells was evaluated in the context of paclitaxel CIN. To do so, thermal hyperalgesia, mechanical allodynia, and spatial learning and memory tests were evaluated by Hotplate, Von Frey, and Morris water maze tests.
Key Findings
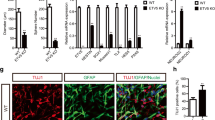
Our result indicated that exposure of EPI-NCSCs to metformin was associated with progressive decline in stemness markers and enhanced expression levels of several neurotrophic, neuron and oligodendrocyte-specific markers. Further, it was observed that intranasal metformin-treated EPI-NCSCs improved the cognitive impairment, and mechanical and thermal hypersensitivity induced by paclitaxel in rats.
Significance
Collectively, we reasoned that metformin pretreatment of EPI-NCSCs might further enhance their therapeutic benefits against CIN.
Graphical Abstract













Similar content being viewed by others
Data Availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Ahn, M. J., & Cho, G. W. (2017). Metformin promotes neuronal differentiation and neurite outgrowth through AMPK activation in human bone marrow–mesenchymal stem cells. Biotechnology and Applied Biochemistry, 64(6), 836–842.
Al-Massri, K. F., Ahmed, L. A., & El-Abhar, H. S. (2020). Mesenchymal stem cells in chemotherapy-induced peripheral neuropathy: A new challenging approach that requires further investigations. Journal of Tissue Engineering and Regenerative Medicine, 14(1), 108–122.
Albert, K., Niskanen, J., Kälvälä, S., & Lehtonen, Š. (2021). Utilising induced pluripotent stem cells in neurodegenerative disease research: Focus on glia. International Journal of Molecular Sciences, 22(9), 4334.
AsgariTaei, A., Dargahi, L., Khodabakhsh, P., Kadivar, M., & Farahmandfar, M. (2022). Hippocampal neuroprotection mediated by secretome of human mesenchymal stem cells against experimental stroke. CNS Neuroscience & Therapeutics, 28(9), 1425–1438.
AsgariTaei, A., Khodabakhsh, P., Nasoohi, S., Farahmandfar, M., & Dargahi, L. (2022). Paracrine effects of mesenchymal stem cells in ischemic stroke: Opportunities and challenges. Molecular Neurobiology, 59(10), 6281–6306.
Bahlakeh, G., Rahbarghazi, R., Mohammadnejad, D., Abedelahi, A., & Karimipour, M. (2021). Current knowledge and challenges associated with targeted delivery of neurotrophic factors into the central nervous system: Focus on available approaches. Cell & Bioscience, 11(1), 1–24.
Bergkvist, A., Rusnakova, V., Sindelka, R., Garda, J. M. A., Sjögreen, B., Lindh, D., Forootan, A., & Kubista, M. (2010). Gene expression profiling–clusters of possibilities. Methods, 50(4), 323–335.
Boukelmoune, N., Laumet, G., Tang, Y., Ma, J., Mahant, I., Singh, S. K., Nijboer, C., Benders, M., Kavelaars, A., & Heijnen, C. J. (2021). Nasal administration of mesenchymal stem cells reverses chemotherapy-induced peripheral neuropathy in mice. Brain, Behavior, and Immunity, 93, 43–54.
Chiang, M.-C., Cheng, Y.-C., Chen, S.-J., Yen, C.-H., & Huang, R.-N. (2016). Metformin activation of AMPK-dependent pathways is neuroprotective in human neural stem cells against amyloid-beta-induced mitochondrial dysfunction. Experimental Cell Research, 347(2), 322–331.
Chiu, G. S., Boukelmoune, N., Chiang, A. C., Peng, B., Rao, V., Kingsley, C., Liu, H.-L., Kavelaars, A., Kesler, S. R., & Heijnen, C. J. (2018). Nasal administration of mesenchymal stem cells restores cisplatin-induced cognitive impairment and brain damage in mice. Oncotarget, 9(85), 35581.
Chung, M.-M., Chen, Y.-L., Pei, D., Cheng, Y.-C., Sun, B., Nicol, C. J., Yen, C.-H., Chen, H.-M., Liang, Y.-J., & Chiang, M.-C. (2015). The neuroprotective role of metformin in advanced glycation end product treated human neural stem cells is AMPK-dependent. Biochimica et Biophysica Acta (BBA)-Molecular Basis of Disease, 1852(5), 720–731.
Dadwal, P., Mahmud, N., Sinai, L., Azimi, A., Fatt, M., Wondisford, F. E., Miller, F. D., & Morshead, C. M. (2015). Activating endogenous neural precursor cells using metformin leads to neural repair and functional recovery in a model of childhood brain injury. Stem Cell Reports, 5(2), 166–173.
Davies, M. J., D’Alessio, D. A., Fradkin, J., Kernan, W. N., Mathieu, C., Mingrone, G., Rossing, P., Tsapas, A., Wexler, D. J., & Buse, J. B. (2018). Management of hyperglycemia in type 2 diabetes, 2018. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care, 41(12), 2669–2701.
De Luca, M., Aiuti, A., Cossu, G., Parmar, M., Pellegrini, G., & Robey, P. G. (2019). Advances in stem cell research and therapeutic development. Nature Cell Biology, 21(7), 801–811.
Demaré, S., Kothari, A., Calcutt, N. A., & Fernyhough, P. (2021). Metformin as a potential therapeutic for neurological disease: Mobilizing AMPK to repair the nervous system. Expert Review of Neurotherapeutics, 21(1), 45–63.
Desforges, A. D., Hebert, C. M., Spence, A. L., Reid, B., Dhaibar, H. A., Cruz-Topete, D., Cornett, E. M., Kaye, A. D., Urits, I., & Viswanath, O. (2022). Treatment and diagnosis of chemotherapy-induced peripheral neuropathy: An update. Biomedicine & Pharmacotherapy, 147, 112671. https://doi.org/10.1016/j.biopha.2022.112671
Donega, V., van Velthoven, C. T., Nijboer, C. H., van Bel, F., Kas, M. J., Kavelaars, A., & Heijnen, C. J. (2013). Intranasal mesenchymal stem cell treatment for neonatal brain damage: Long-term cognitive and sensorimotor improvement. PLoS ONE, 8(1), e51253.
Eddy, N. B., & Leimbach, D. (1953). Synthetic analgesics. II. Dithienylbutenyl-and dithienylbutylamines. Journal of Pharmacology and Experimental Therapeutics, 107(3), 385–393.
El Ouaamari, Y., Van den Bos, J., Willekens, B., Cools, N., & Wens, I. (2023). Neurotrophic factors as regenerative therapy for neurodegenerative diseases: Current status, challenges and future perspectives. International Journal of Molecular Sciences, 24(4), 3866.
Erdő, F., Bors, L. A., Farkas, D., Bajza, Á., & Gizurarson, S. (2018). Evaluation of intranasal delivery route of drug administration for brain targeting. Brain Research Bulletin, 143, 155–170.
Erices, R., Bravo, M. L., Gonzalez, P., Oliva, B., Racordon, D., Garrido, M., Ibañez, C., Kato, S., Brañes, J., & Pizarro, J. (2013). Metformin, at concentrations corresponding to the treatment of diabetes, potentiates the cytotoxic effects of carboplatin in cultures of ovarian cancer cells. Reproductive Sciences, 20(12), 1433–1446.
Esmaeilzade, B., Nobakht, M., Joghataei, M. T., Roshandel, N. R., Rasouli, H., Kuchaksaraei, A. S., Hosseini, S. M., Najafzade, N., Asalgoo, S., & Hejazian, L. B. (2012). Delivery of epidermal neural crest stem cells (EPI-NCSC) to hippocamp in alzheimer’s disease rat model. Iranian Biomedical Journal, 16(1), 1.
Fang, W., Zhang, J., Hong, L., Huang, W., Dai, X., Ye, Q., & Chen, X. (2020). Metformin ameliorates stress-induced depression-like behaviors via enhancing the expression of BDNF by activating AMPK/CREB-mediated histone acetylation. Journal of Affective Disorders, 260, 302–313.
Fatt, M., Hsu, K., He, L., Wondisford, F., Miller, F. D., Kaplan, D. R., & Wang, J. (2015). Metformin acts on two different molecular pathways to enhance adult neural precursor proliferation/self-renewal and differentiation. Stem Cell Reports, 5(6), 988–995.
Hoogduijn, M. J., Roemeling-van Rhijn, M., Engela, A. U., Korevaar, S. S., Mensah, F. K., Franquesa, M., de Bruin, R. W., Betjes, M. G., Weimar, W., & Baan, C. C. (2013). Mesenchymal stem cells induce an inflammatory response after intravenous infusion. Stem Cells and Development, 22(21), 2825–2835.
Houshmand, F., Barati, M., Golab, F., Ramezani-Sefidar, S., Tanbakooie, S., Tabatabaei, M., Amiri, M., & Sanadgol, N. (2019). Metformin-induced AMPK activation stimulates remyelination through induction of neurotrophic factors, downregulation of NogoA and recruitment of Olig2+ precursor cells in the cuprizone murine model of multiple sclerosis. DARU Journal of Pharmaceutical Sciences, 27, 583–592.
Hu, Y. F., Zhang, Z. J., & Sieber-Blum, M. (2006). An epidermal neural crest stem cell (EPI-NCSC) molecular signature. Stem Cells, 24(12), 2692–2702.
Ikhsan, M., Palumbo, A., Rose, D., Zille, M., & Boltze, J. (2019). Neuronal stem cell and drug interactions: a systematic review and meta-analysis: Concise review. Stem Cells Translational Medicine, 8(11), 1202–1211. https://doi.org/10.1002/sctm.19-0020
Janelsins, M. C., Kesler, S. R., Ahles, T. A., & Morrow, G. R. (2014). Prevalence, mechanisms, and management of cancer-related cognitive impairment. International Review of Psychiatry, 26(1), 102–113.
Johnson, N. J., Hanson, L. R., & Frey, W. H. (2010). Trigeminal pathways deliver a low molecular weight drug from the nose to the brain and orofacial structures. Molecular Pharmaceutics, 7(3), 884–893.
Katila, N., Bhurtel, S., Park, P.-H., Hong, J. T., & Choi, D.-Y. (2020). Activation of AMPK/APKCΖ/CREB pathway by metformin is associated with upregulation of GDNF and dopamine. Biochemical Pharmacology, 180, 114193.
Khodabakhsh, P., Pournajaf, S., MohagheghShalmani, L., Ahmadiani, A., & Dargahi, L. (2021). Insulin promotes schwann-like cell differentiation of rat epidermal neural crest stem cells. Molecular Neurobiology, 58, 5327–5337.
Kim, J., Lo, L., Dormand, E., & Anderson, D. J. (2003). SOX10 maintains multipotency and inhibits neuronal differentiation of neural crest stem cells. Neuron, 38(1), 17–31.
Lalau, J. D., Kajbaf, F., Bennis, Y., Hurtel-Lemaire, A. S., Belpaire, F., & De Broe, M. E. (2018). Metformin treatment in patients with type 2 diabetes and chronic kidney disease stages 3A, 3B, or 4. Diabetes Care, 41(3), 547–553. https://doi.org/10.2337/dc17-2231
Li, Y., Yao, D., Zhang, J., Liu, B., Zhang, L., Feng, H., & Li, B. (2017). The effects of epidermal neural crest stem cells on local inflammation microenvironment in the defected sciatic nerve of rats. Frontiers in Molecular Neuroscience, 10, 133.
Lim, J. Y., Park, S. I., Oh, J. H., Kim, S. M., Jeong, C. H., Jun, J. A., Lee, K. S., Oh, W., Lee, J. K., & Jeun, S. S. (2008). Brain-derived neurotrophic factor stimulates the neural differentiation of human umbilical cord blood-derived mesenchymal stem cells and survival of differentiated cells through MAPK/ERK and PI3K/Akt-dependent signaling pathways. Journal of Neuroscience Research, 86(10), 2168–2178.
Liu, F., Xuan, A., Chen, Y., Zhang, J., Xu, L., Yan, Q., & Long, D. (2014). Combined effect of nerve growth factor and brain-derived neurotrophic factor on neuronal differentiation of neural stem cells and the potential molecular mechanisms. Molecular Medicine Reports, 10(4), 1739–1745.
Livak, K. J., & Schmittgen, T. D. (2001). Analysis of relative gene expression data using real-time quantitative PCR and the 2− ΔΔCT method. Methods, 25(4), 402–408.
Ma, J., Liu, J., Yu, H., Chen, Y., Wang, Q., & Xiang, L. (2015). Effect of metformin on schwann cells under hypoxia condition. International Journal of Clinical and Experimental Pathology, 8(6), 6748.
Marsh, S. E., & Blurton-Jones, M. (2017). Neural stem cell therapy for neurodegenerative disorders: The role of neurotrophic support. Neurochemistry International, 106, 94–100. https://doi.org/10.1016/j.neuint.2017.02.006
MohagheghShalmani, L., Valian, N., Pournajaf, S., Abbaszadeh, F., Dargahi, L., & Jorjani, M. (2020). Combination therapy with astaxanthin and epidermal neural crest stem cells improves motor impairments and activates mitochondrial biogenesis in a rat model of spinal cord injury. Mitochondrion, 52, 125–134. https://doi.org/10.1016/j.mito.2020.03.002
Mosmann, T. (1983). Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. Journal of immunological methods, 65(1–2), 55–63.
Narytnyk, A., Verdon, B., Loughney, A., Sweeney, M., Clewes, O., Taggart, M. J., & Sieber-Blum, M. (2014). Differentiation of human epidermal neural crest stem cells (hEPI-NCSC) into virtually homogenous populations of dopaminergic neurons. Stem cell reviews and reports, 10, 316–326.
Neirinckx, V., Coste, C., Rogister, B., & Wislet-Gendebien, S. (2013). Concise review: Adult mesenchymal stem cells, adult neural crest stem cells, and therapy of neurological pathologies: A state of play. Stem Cells Translational Medicine, 2(4), 284–296.
Ould-Brahim, F., Sarma, S. N., Syal, C., Lu, K. J., Seegobin, M., Carter, A., Jeffers, M. S., Doré, C., Stanford, W. L., Corbett, D. J. S. C., & development. (2018). Metformin preconditioning of human induced pluripotent stem cell-derived neural stem cells promotes their engraftment and improves post-stroke regeneration and recovery. 27(16), 1085–1096.
Pajtler, K., Bohrer, A., Maurer, J., Schorle, H., Schramm, A., Eggert, A., & Schulte, J. H. (2010). Production of chick embryo extract for the cultivation of murine neural crest stem cells. Journal of Visualized Experiments, (45). https://doi.org/10.3791/2380
Pournajaf, S., Valian, N., MohagheghShalmani, L., Khodabakhsh, P., Jorjani, M., & Dargahi, L. (2020). Fingolimod increases oligodendrocytes markers expression in epidermal neural crest stem cells. European Journal of Pharmacology, 885, 173502. https://doi.org/10.1016/j.ejphar.2020.173502
Präbst, K., Engelhardt, H., Ringgeler, S., & Hübner, H. (2017). Basic colorimetric proliferation assays: MTT, WST, and resazurin. Cell viability assays: methods and protocols, 1–17.
Ren, K. (1999). An improved method for assessing mechanical allodynia in the rat. Physiology & Behavior, 67(5), 711–716.
Ronaghi, M., Erceg, S., Moreno-Manzano, V., & Stojkovic, M. (2010). Challenges of stem cell therapy for spinal cord injury: human embryonic stem cells, endogenous neural stem cells, or induced pluripotent stem cells? Stem Cells, 28(1), 93–99. https://doi.org/10.1002/stem.253
Sakaue, M., & Sieber-Blum, M. (2015). Human epidermal neural crest stem cells as a source of Schwann cells. Development, 142(18), 3188–3197.
Salehi, M. S., Pandamooz, S., Safari, A., Jurek, B., Tamadon, A., Namavar, M. R., & Borhani-Haghighi, A. (2020). Epidermal neural crest stem cell transplantation as a promising therapeutic strategy for ischemic stroke. CNS Neuroscience & Therapeutics, 26(7), 670–681.
Sieber-Blum, M., & Hu, Y. (2008). Epidermal neural crest stem cells (EPI-NCSC) and pluripotency. Stem Cell Reviews, 4, 256–260.
Sieber-Blum, M., Schnell, L., Grim, M., Hu, Y. F., Schneider, R., & Schwab, M. E. (2006). Characterization of epidermal neural crest stem cell (EPI-NCSC) grafts in the lesioned spinal cord. Molecular and Cellular Neuroscience, 32(1–2), 67–81. https://doi.org/10.1016/j.mcn.2006.02.003
Stevenson, R., Samokhina, E., Rossetti, I., Morley, J. W., & Buskila, Y. (2020). Neuromodulation of glial function during neurodegeneration. Frontiers in Cellular Neuroscience, 14, 278.
Wang, J., Gallagher, D., DeVito, L. M., Cancino, G. I., Tsui, D., He, L., Keller, G. M., Frankland, P. W., Kaplan, D. R., & Miller, F. D. (2012). Metformin activates an atypical PKC-CBP pathway to promote neurogenesis and enhance spatial memory formation. Cell Stem Cell, 11(1), 23–35.
Wang, L. L., Janes, M. E., Kumbhojkar, N., Kapate, N., Clegg, J. R., Prakash, S., Heavey, M. K., Zhao, Z., Anselmo, A. C., & Mitragotri, S. (2021). Cell therapies in the clinic. Bioengineering & Translational Medicine, 6(2), e10214. https://doi.org/10.1002/btm2.10214
Zhang, L., Li, B., Liu, B., & Dong, Z. (2019). Co-transplantation of epidermal neural crest stem cells and olfactory ensheathing cells repairs sciatic nerve defects in rats. Frontiers in Cellular Neuroscience, 13, 253.
Zhang, P., Bu, J., Wu, X., Deng, L., Chi, M., Ma, C., Shi, X., & Wang, G. (2020). Upregulation of μ-opioid receptor in the rat spinal cord contributes to the α2-adrenoceptor agonist dexmedetomidine-induced attenuation of chronic morphine tolerance in cancer pain. Journal of Pain Research, 13, 2617.
Acknowledgements
The authors would like to express their gratitude to the dedicated staff of the Neuroscience Research Center at Shahid Beheshti University of Medical Sciences for their invaluable technical support. Special appreciation is extended to Dr. Farzin Kamari from the Institute of Physiology, Department of Neurophysiology, Eberhard Karls University of Tübingen, Tübingen, Germany, for his significant contributions, which enhanced both the visual and scientific aspects of this manuscript. The graphical abstract was produced using the tools provided by Biorender.com.
Funding
This study was funded by Research Affairs of Shahid Beheshti University of Medical Sciences, Tehran, Iran (grant No. 26873).
Author information
Authors and Affiliations
Contributions
Pariya Khodabakhsh and Afsaneh Asgari Taei: Investigation, Formal analysis, Writing – original draft, Writing – review & editing. Hamed Shafaroodi: Conceptualization, Supervision, Resources. Safura Pournajaf: Investigation, Writing – original draft, Writing – review & editing. Leila Dargahi: Conceptualization, Methodology, Supervision, Resources, Funding acquisition, Writing – review & editing. All authors have approved the manuscript.
Corresponding author
Ethics declarations
Conflicts of Interest
None.
Ethical Approval
All animal experiments were performed in accordance with the National Institute of Health Guide for the Care and Use of Laboratory Animals (NIH Publications No. 80–23, revised, 1996) and were approved by the Ethics Committee of Shahid Beheshti University of Medical Sciences (IR.SBMU.PHNS.REC.1399.164).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Pariya Khodabakhsh, Afsaneh Asgari Taei these authors contributed equally to this work and should be considered joint first authors.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Khodabakhsh, P., Asgari Taei, A., Shafaroodi, H. et al. Effect of Metformin on Epidermal Neural Crest Stem Cells and Their Potential Application in Ameliorating Paclitaxel-induced Neurotoxicity Phenotype. Stem Cell Rev and Rep 20, 394–412 (2024). https://doi.org/10.1007/s12015-023-10642-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-023-10642-x