Abstract
Purpose
Anterior and posterior decompressions for cervical myelopathy and radiculopathy may lead to clinical improvements. However, patients with kyphotic cervical alignment have sometimes shown poor clinical outcomes with posterior decompression. There is a lack on report of mechanical analysis of the decompression procedures for kyphotic cervical alignment.
Methods
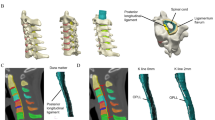
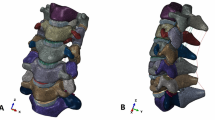
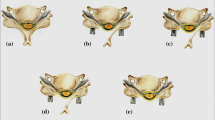
This study employed a three-dimensional finite element (FE) model of the cervical spine (C2-C7) with the pre-operative kyphotic alignment (Pre-OK) model and compared the biomechanical parameters (range of motion (ROM), annular stresses, nucleus stresses, and facet contact forces) for four decompression procedures at two levels (C3-C5); laminectomy (LN), laminoplasty (LP), posterior decompression with fusion (PDF), and anterior decompression with fusion (ADF). Pure moment with compressive follower load was applied to these models.
Results
PDF and ADF models’ global ROM were 40% at C2-C7 less than the Pre-OK, LN, and LP models. The annular and nucleus stresses decreased more than 10% at the surgery levels for ADF, and PDF, compared to the Pre-OK, LN, and LP models. However, the annular stresses at the adjacent cranial level (C2-C3) of ADF were 20% higher. The nucleus stresses of the caudal adjacent level (C5-C6) of PDF were 20% higher, compared to other models. The PDF and ADF models showed a less than 70% decrease in the facet forces at the surgery levels, compared to the Pre-OK, LN, and LP models.
Conclusion
The study concluded that posterior decompression, such as LN or LP, increases ROM, disc stress, and facet force and thus can lead to instability. Although there is the risk of adjacent segment disease (ASD), PDF and ADF can stabilize the cervical spine even for kyphotic alignments.






Similar content being viewed by others
References
Boody BS, Lendner M, Vaccaro AR (2019) Ossification of the posterior longitudinal ligament in the cervical spine: a review. Int Orthop 43(4):797–805
Yoshii T, Sakai K, Hirai T, Yamada T, Inose H, Kato T, Enomoto M, Tomizawa S, Kawabata S, Arai Y, Okawa A (2016) Anterior decompression with fusion versus posterior decompression with fusion for massive cervical ossification of the posterior longitudinal ligament with a ≥50% canal occupying ratio: a multicenter retrospective study. Spine J 16(11):1351–1357
Inose H, Hirai T, Yoshii T, Kimura A, Takeshita K, Inoue H, Maekawa A, Endo K, Furuya T, Nakamura A, Mori K, Kanbara S, Imagama S, Seki S, Matsunaga S, Takahashi K, Okawa A (2021) Predictors associated with neurological recovery after anterior decompression with fusion for degenerative cervical myelopathy. BMC Surg 21(1):144
Sakai K, Yoshii T, Hirai T, Arai Y, Torigoe I, Tomori M, Sato H, Okawa A (2016) Cervical sagittal imbalance is a predictor of kyphotic deformity after laminoplasty in cervical spondylotic myelopathy patients without preoperative kyphotic alignment. Spine (Phila Pa 1976) 41(4):299–305
Mayer M, Meier O, Auffarth A, Koller H (2015) Cervical laminectomy and instrumented lateral mass fusion: techniques, pearls and pitfalls. Eur Spine J 24(Suppl 2):168–185
Yoshii T, Egawa S, Chikuda H, Wakao N, Furuya T, Kanchiku T, Nagoshi N, Fujiwara Y, Yoshida M, Taguchi T, Watanabe M (2020) Comparison of anterior decompression with fusion and posterior decompression with fusion for cervical spondylotic myelopathy-A systematic review and meta-analysis. J Orthop Sci 25(6):938–945
Palepu V (2013) Biomechanical effects of initial occupant seated posture during rear end impact injury. OhioLINK electronic Theses and Dissertations Center. http://rave.ohiolink.edu/etdc/view?acc_num=toledo1376585027
Kallemeyn N, Gandhi A, Kode S, Shivanna K, Smucker J, Grosland N (2010) Validation of a C2-C7 cervical spine finite element model using specimen-specific flexibility data. Med Eng Phys 32(5):482–489
Venkataramana MP, Hans SA, Bawab SY, Keifer OP, Woodhouse ML, Layson PD (2005) Effects of initial seated position in low speed rear-end impacts: a comparison with the TNO rear impact dummy (TRID) model. Traffic Inj Prev 6(1):77–85
Pospiech J, Stolke D, Wilke HJ, Claes LE (1999) Intradiscal pressure recordings in the cervical spine. Neurosurgery 44(2):379–384
Finn MA, Brodke DS, Daubs M, Patel A, Bachus KN (2009) Local and global subaxial cervical spine biomechanics after single-level fusion or cervical arthroplasty. Eur Spine J 18(10):1520–1527
Goel VK, Clausen JD (1998) Prediction of load sharing among spinal components of a C5–C6 motion segment using the finite element approach. Spine (Phila Pa 1976) 23(6):684–691
Little JP, Adam CJ, Evans JH, Pettet GJ, Pearcy MJ (2007) Nonlinear finite element analysis of anular lesions in the L4/5 intervertebral disc. J Biomech 40(12):2744–2751
Godzik J, Pereira BA, Newcomb A, Lehrman JN, Mundis GM Jr, Hlubek RJ, Uribe JS, Kelly BP, Turner JD (2020) Optimizing biomechanics of anterior column realignment for minimally invasive deformity correction. Spine J 20(3):465–474
Nishida N, Mumtaz M, Tripathi S, Kelkar A, Sakai T, Goel VK (2021) Biomechanical analysis of posterior ligaments of cervical spine and laminoplasty. Appl Sci 11(16):7645
Scheer JK, Tang JA, Smith JS, Acosta FL Jr, Protopsaltis TS, Blondel B, Bess S, Shaffrey CI, Deviren V, Lafage V, Schwab F, Ames CP (2013) Cervical spine alignment, sagittal deformity, and clinical implications: a review. J Neurosurg Spine 19(2):141–159
Hayashi T, Daubs MD, Suzuki A, Phan K, Shiba K, Wang JC (2014) Effect of Modic changes on spinal canal stenosis and segmental motion in cervical spine. Eur Spine J 23(8):1737–1742
Hirabayashi S (2018) Recent surgical methods of double-door laminoplasty of the cervical spine (Kurokawa’s Method). Spine Surg Relat Res 2(2):154–158
Kumaran Y, Shah A, Katragadda A, Padgaonkar A, Zavatsky J, McGuire R, Serhan H, Elgafy H, Goel VK (2021) Iatrogenic muscle damage in transforaminal lumbar interbody fusion and adjacent segment degeneration: a comparative finite element analysis of open and minimally invasive surgeries. Eur Spine J 30(9):2622–2630
Quinn JC, Kiely PD, Lebl DR, Hughes AP (2015) Anterior surgical treatment of cervical spondylotic myelopathy: review article. Hss J 11(1):15–25
Patwardhan AG, Havey RM, Carandang G, Simonds J, Voronov LI, Ghanayem AJ, Meade KP, Gavin TM, Paxinos O (2003) Effect of compressive follower preload on the flexion-extension response of the human lumbar spine. J Orthop Res 21(3):540–546
Khuyagbaatar B, Kim K, Park WM, Lee S, Kim YH (2017) Increased stress and strain on the spinal cord due to ossification of the posterior longitudinal ligament in the cervical spine under flexion after laminectomy. Proc Inst Mech Eng H 231(9):898–906
Hirabayashi S, Kitagawa T, Yamamoto I, Yamada K, Kawano H (2020) Development and achievement of cervical laminoplasty and related studies on cervical myelopathy. Spine Surg Relat Res 4(1):8–17
Winestone JS, Farley CW, Curt BA, Chavanne A, Dollin N, Pettigrew DB, Ct K (2012) Laminectomy, durotomy, and piotomy effects on spinal cord intramedullary pressure in severe cervical and thoracic kyphotic deformity: a cadaveric study. J Neurosurg Spine 16(2):195–200
Qian S, Wang Z, Jiang G, Xu Z, Chen W (2018) Efficacy of laminoplasty in patients with cervical kyphosis. Med Sci Monit 24:1188–1195
Hashiguchi A, Kanchiku T, Nishida N, Taguchi T (2018) Biomechanical study of cervical posterior decompression. Asian Spine J 12(3):391–397
Subramaniam V, Chamberlain RH, Theodore N, Baek S, Safavi-Abbasi S, Senoğlu M, Sonntag VK, Crawford NR (2009) Biomechanical effects of laminoplasty versus laminectomy: stenosis and stability. Spine (Phila Pa 1976) 34(16):E573-578
Kim BS, Dhillon RS (2019) Cervical laminectomy with or without lateral mass instrumentation: a comparison of outcomes. Clin Spine Surg 32(6):226–232
Abumi K (2015) Cervical spondylotic myelopathy: posterior decompression and pedicle screw fixation. Eur Spine J 24(Suppl 2):186–196
Papagelopoulos PJ, Currier BL, Neale PG, Hokari Y, Berglund LJ, Larson DR, Fisher DR, An KN (2003) Biomechanical evaluation of posterior screw fixation in cadaveric cervical spines. Clin Orthop Relat Res. https://doi.org/10.1097/01.blo.0000068359.47147.bd(411):13-24
Karasin B, Grzelak M (2021) Anterior cervical discectomy and fusion: a surgical intervention for treating cervical disc disease. Aorn j 113(3):237–251
Deng Y, Li G, Liu H, Hong Y, Meng Y (2020) Mid- to long-term rates of symptomatic adjacent-level disease requiring surgery after cervical total disc replacement compared with anterior cervical discectomy and fusion: a meta-analysis of prospective randomized clinical trials. J Orthop Surg Res 15(1):468
Li Z, Liu H, Yang M, Zhang W (2021) A biomechanical analysis of four anterior cervical techniques to treating multilevel cervical spondylotic myelopathy: a finite element study. BMC Musculoskelet Disord 22(1):278
Siemionow K, Monsef JB, Janusz P (2016) Preliminary analysis of adjacent segment degeneration in patients treated with posterior cervical cages: 2-year follow-up. World Neurosurg 89:730.e731-737
Xia Y, Xu R, Kosztowski TA, Ramhmdani S, Ahmed AK, Lo SL, Bydon A (2019) Reoperation for proximal adjacent segment pathology in posterior cervical fusion constructs that fuse to C2 vs C3. Neurosurgery 85(3):E520-e526
Xia XP, Chen HL, Cheng HB (2013) Prevalence of adjacent segment degeneration after spine surgery: a systematic review and meta-analysis. Spine 38(7):597–608
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No benefits in any form have been received or will be acquired by a commercial party related directly or indirectly to the subject of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nishida, N., Mumtaz, M., Tripathi, S. et al. Biomechanical analysis of laminectomy, laminoplasty, posterior decompression with instrumented fusion, and anterior decompression with fusion for the kyphotic cervical spine. Int J CARS 17, 1531–1541 (2022). https://doi.org/10.1007/s11548-022-02692-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11548-022-02692-2