Abstract
Purpose
To investigate the prevalence of treatment-emergent central sleep apnea (TECSA) in individuals with obstructive sleep apnea syndrome (OSAS) during continuous positive airway pressure (CPAP) titration and assess their polysomnographic characteristics.
Methods
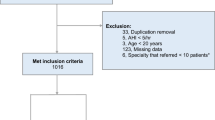
A total of 116 patients with OSAS who underwent full-night CPAP titration at the Sleep Laboratory of Adana City Research and Education Hospital from September 2017 to January 2018 were recruited for the study. The patients’ polysomnographic data related to respiratory events and sleep stages were reviewed in a retrospective manner.
Results
While on CPAP titration, 20 of the 116 patients developed central sleep apnea (CSA). The prevalence of TECSA in the patients with OSAS was 17.2%, being separately determined as 16.3% and 2.2% for the male and female patients, respectively. In the baseline PSG, the groups did not statistically significantly differ in relation to the apnea hypopnea index (AHI), central apnea index (CAI), arousal index (AI), or oxygen desaturation index (ODI). However, the TECSA group had a significantly higher mean oxygen saturation value compared to the non-TECSA group (p = 0.01). The total AHI, CAI, and AI values of the TECSA group were significantly higher during the whole CPAP titration compared to the non-TECSA group. No significant difference was observed in the comparison of the two groups in relation to the titration pressure and ODI.
Conclusion
TECSA is a phenomenon that can occur with obstructive sleep apnea treatment and mostly regress spontaneously following appropriate CPAP treatment. TECSA is observed at different rates of prevalence. In this study, the prevalence of TECSA was higher than previously reported.

Similar content being viewed by others
Data availability
Due to privacy and ethical concerns, neither the data nor its source code can be made available to the public.
References
Sateia MJ (2014) International classification of sleep disorders-third edition: highlights and modifications. Chest 146(5):1387–1394. https://doi.org/10.1378/chest.14-0970
Ruehland WR, Rochford PD, O’Donoghue FJ, Pierce RJ, Singh P, Thornton AT (2009) The new AASM criteria for scoring hypopneas: impact on the apnea hypopnea index. Sleep 32(2):150–157. https://doi.org/10.1093/sleep/32.2.150
Bradley TD, Phillipson EA (1992) Central sleep apnea. Clin Chest Med 13(3):493–505
Rana AM, Sankari A (2023) Central sleep apnea. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. Available from https://www.ncbi.nlm.nih.gov/books/NBK578199/
Randerath W, Verbraecken J, Andreas S, Arzt M, Bloch KE, Brack T et al (2017) Definition, discrimination, diagnosis and treatment of central breathing disturbances during sleep. Eur Respir J 49(1):1600959. https://doi.org/10.1183/13993003.00959-2016
Liu D, Armitstead J, Benjafield A, Shao S, Malhotra A, Cistulli PA et al (2017) Trajectories of emergent central sleep apnea during CPAP therapy. Chest 152(4):751–760
Selim B, Ramar K (2021) Sleep-related breathing disorders: when CPAP is not enough. Neurotherapeutics 18(1):81–90. https://doi.org/10.1007/s13311-020-00955-x
Zhang J, Wang L, Guo HJ, Wang Y, Cao J, Chen BY (2020) Treatment-emergent central sleep apnea: a unique sleep-disordered breathing. Chin Med J (Engl) 133(22):2721–2730. https://doi.org/10.1097/CM9.0000000000001125
Gay PC (2008) Complex sleep apnea: it really is a disease. J Clin Sleep Med 4(5):403–5
Malhotra A, Bertisch S, Wellman A (2008) Complex sleep apnea: it isn’t really a disease. J Clin Sleep Med 4(5):406–8
Younes M, Ostrowski M, Thompson W, Leslie C, Shewchuk W (2001) Chemical control stability in patients with obstructive sleep apnea. Am J Respir Crit Care Med 163:1181–1190. https://doi.org/10.1164/ajrccm.163.5.2007013
Salloum A, Rowley JA, Mateika JH, Chowdhuri S, Omran Q, Badr MS (2010) Increased propensity for central apnea in patients with obstructive sleep apnea: effect of nasal continuous positive airway pressure. Am J Respir Crit Care Med 181:189–193
Stanchina M, Robinson K, Corrao W, Donat W, Sands S, Malhotra A (2014) Clinical use of loop gain measures to determine continuous positive airway pressure efficacy in patients with complex sleep apnea. A pilot study. Ann Am Thorac Soc 12(9):1351–1357. https://doi.org/10.1513/AnnalsATS.201410-469BC
Cassel W, Canisius S, Becker HF, Leistner S, Ploch T, Jerrentrup A et al (2011) A prospective polysomnographic study on the evolution of complex sleep apnoea. Eur Respir J 38(2):329–337. https://doi.org/10.1183/09031936.00162009
Nakazaki C, Noda A, Yasuda Y, Nakata S, Koike Y, Yasuma F et al (2012) Continuous positive airway pressure intolerance associated with elevated nasal resistance is possible mechanism of complex sleep apnea syndrome. Sleep Breath 16(3):747–752. https://doi.org/10.1007/s11325-011-0570-5
Kuźniar TJ, Morgenthaler TI (2008) Treatment of complex sleep apnea syndrome. Curr Treat Options Neurol 10(5):336–341. https://doi.org/10.1007/s11940-008-0036-7
Dernaika T, Tawk M, Nazir S, Younis W, Kinasewitz GT (2007) The significance and outcome of continuous positive airway pressure-related central sleep apnea during split-night sleep studies. Chest 132(1):81–87. https://doi.org/10.1378/chest.06-2562
Brown LK, Casey KR (2007) Complex sleep apnea: the hedgehog and the fox. Curr Opin Pulm Med 13(6):473–478. https://doi.org/10.1097/MCP.0b013e3282f1479b
Montesi SB, Bakker JP, Macdonald M, Hueser L, Pittman S, White DP et al (2013) Leak during CPAP titration as a risk factor for central apnea. J Clin Sleep Med 9(11):1187–1191. https://doi.org/10.5664/jcsm.3166
Morgenthaler TI, Kagramanov V, Hanak V, Decker PA (2006) Complex sleep apnea syndrome: is it a unique clinical syndrome? Sleep 29(9):1203–1209. https://doi.org/10.1093/sleep/29.9.1203
Javaheri S, Smith J, Chung E (2009) The prevalence and natural history of complex sleep apnea. J Clin Sleep Med 5(3):205–211
Aurora RN, Chowdhuri S, Ramar K, Bista SR, Casey KR, Lamm CI et al (2012) The treatment of central sleep apnea syndromes in adults: practice parameters with an evidence-based literature review and meta-analyses. Sleep 35(1):17–40. https://doi.org/10.5665/sleep.1580
Kushida CA, Chediak A, Berry RB, Brown LK, Gozal D, Iber C et al (2008) Positive Airway Pressure Titration Task Force; American Academy of Sleep Medicine. Clinical guidelines for the manual titration of positive airway pressure in patients with obstructive sleep apnea. J Clin Sleep Med. 4(2):157–71
Lehman S, Antic NA, Thompson C, Catcheside PG, Mercer J, McEvoy RD (2007) Central sleep apnea on commencement of continuous positive airway pressure in patients with a primary diagnosis of obstructive sleep apnea-hypopnea. J Clin Sleep Med 3(5):462–6
Verbraecken J, Schoonis L, Verplancke B (2009) Prevalence of complex sleep apnea (CompSAS) during manual CPAP titration for obstructive sleep apnea. Eur Respir J 34(53):649s. https://doi.org/10.1183/20734735.042412
Endo Y, Suzuki M, Inoue Y, Sato M, Namba K, Hasegawa M et al (2008) Prevalence of complex sleep apnea among Japanese patients with sleep apnea syndrome. Tohoku J Exp Med 15(4):349–354. https://doi.org/10.1620/tjem.215.349
Thomas RJ, Terzano MG, Parrino L, Weiss JW (2004) Obstructive sleep-disordered breathing with a dominant cyclic alternating pattern–a recognizable polysomnographic variant with practical clinical implications. Sleep 27(2):229–234. https://doi.org/10.1093/sleep/27.2.229
Yaegashi H, Fujimoto K, Abe H, Orii K, Eda S, Kubo K (2009) Characteristics of Japanese patients with complex sleep apnea syndrome: a retrospective comparison with obstructive sleep apnea syndrome. Intern Med 48(6):427–432. https://doi.org/10.2169/internalmedicine.48.1459
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants adhered to the ethical standards set by the institutional and/or national research committee (Adana Research and Education Hospital, Clinical Research Ethics Committee), as well as those specified by the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Consent to participate
Formal consent was not required for this type of study.
Conflict of interest
The author declares no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Berik Safçi, S. The prevalence and polysomnographic characteristics of treatment-emergent central sleep apnea with obstructive sleep apnea. Sleep Breath (2024). https://doi.org/10.1007/s11325-024-02999-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11325-024-02999-1