Abstract
Purpose
The pharmaceutical bioequivalence of generic medicines must be confirmed with corresponding original drugs. Although the in vitro dissolution tests are required, results of the mandatory in vitro study do not necessarily reflect the in vivo performance after oral administration. Then, we have tried to develop the novel “Dissolution-Absorption Prediction (DAP) workflow” to evaluate the in vivo performance of generic medicines.
Methods
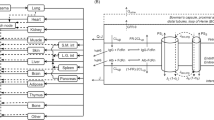
The DAP workflow consists of an “In vitro two-cell connected dissolution (TCCD) system” mimicking the changes in the luminal pH associated with gastrointestinal transit of medicines, “Evaluation of pharmacokinetics of active pharmaceutical ingredient (API)” and “Prediction of plasma concentration–time profile”. TCCD system-evaluated dissolution kinetics of APIs from generic formulations and pharmacokinetic parameters based on human data regarding the original drugs were used to calculate the plasma concentration–time profiles of APIs after the oral administration of generic medicines.
Results
The mandatory in vitro dissolution tests indicated that the dissolution properties of valsartan (BCS class II) and fexofenadine (BCS class III/IV) in generic formulations did not coincide with those in the corresponding original formulations. The TCCD system provided the very similar dissolution kinetics for the generic and original formulations for the two APIs. Plasma concentration–time profiles evaluated utilizing the dissolution profiles obtained by the TCCD system were in good agreement with the observed profiles for both the generic and original formulations for each API.
Conclusions
The DAP workflow would be valuable for estimating the in vivo performance of generic formulation and deducing their bioequivalence with the original formulation.









Similar content being viewed by others
References
Nayak AK, Maji R, Das B. Gastroretentive drug delivery systems: a review. Asian J Pharm Clin Res. 2010;3(1):2–10.
Lipinski AC. Drug-like properties and the causes of poor solubility and poor permeability. J Pharmacol Toxicol Methods. 2000;44(1):235–49. https://doi.org/10.1016/S1056-8719(00)00107-6.
Tanaka Y, Kubota A, Matsuo A, Kawakami A, Kamizi H, Mochigoe A, et al. Effect of absorption behavior of solubilizers on drug dissolution in the gastrointestinal tract: evaluation based on in vivo luminal concentration-time profile of cilostazol, a poorly soluble drug, and solubilizers. J Pharm Sci. 2016;105(9):2825–31. https://doi.org/10.1016/j.xphs.2016.02.026.
Bonferoni CM, Ferrari F, Rossi S, Caramella CM. The role of particle size in drug release and absorption. Particulate Products. 2014; p. 323–41. https://doi.org/10.1007/978-3-319-00714-4_11.
Jinno J, Kamada N, Miyake M, Yamada K, Mukai T, Odomi M, et al. Effect of particle size reduction on dissolution and oral absorption of a poorly water-soluble drug, cilostazol, in beagle dogs. J Control Release. 2006;111(1–2):56–64. https://doi.org/10.1016/j.jconrel.2005.11.013.
Himawan A, Djide NJN, Mardikasari SA, Utami RN, Arjuna A, Donnelly RF, et al. A novel in vitro approach to investigate the effect of food intake on release profile of valsartan in solid dispersion-floating gel in-situ delivery system. Eur J Pharm Sci. 2022;168:106057. https://doi.org/10.1016/j.ejps.2021.106057.
Beg S, Swain S, Singh HP, Patra CN, Rao MEB. Development, optimization, and characterization of solid self-nanoemulsifying drug delivery systems of valsartan using porous carriers. AAPS PharmSciTech. 2012;13(4):1416–27. https://doi.org/10.1208/s12249-012-9865-5.
Kushner J, Lamba M, Stock T, Ronnie W, Nemeth MA, Alvey C, et al. Development and validation of a level a in-vitro in-vivo correlation for tofacitinib modified-release tablets using extrudable core system osmotic delivery technology. Eur J Pharm Sci. 2020;147:105200. https://doi.org/10.1016/j.ejps.2019.105200.
Guideline for Bioequivalence Studies for Formulation Changes of Oral Solid Dosage Forms. https://www.nihs.go.jp/drug/index-E.thml#BE
Pharmaceuticals and Medical Devices Agency. Guideline for Bioequivalence Studies of Generic Products, Attachment 1 of PSEHB/PED Notification No. 0319–1, dated March 19, 2020. https://www.nihs.go.jp/drug/be-guide(e)/2020/GL1_BE_2020.pdf.
U.S. Department of Health and Human Services, Food and Drug Administration, Center for Drug Evaluation and Research (CDER). Dissolution testing of immediate release solid oral dosage forms. August 1997. https://www.fda.gov/regulatory-information/search-fda-guidance-documents/dissolution-testing-immediate-release-solid-oral-dosage-forms.
Haruta S, Kawai K, Nishii R, Jinnouchi S, Ogawara K, Higaki K, et al. Prediction of plasma concentration–time curve of orally administered theophylline based on a scintigraphic monitoring of gastrointestinal transit in human volunteers. Int J Pharm. 2002;233(1–2):179–90. https://doi.org/10.1016/S0378-5173(01)00942-5.
Yu XL, John R, Crison JR, Amidon GL. Compartmental transit and dispersion model analysis of small intestinal transit flow in humans. Int J Pharm. 1996;140(1):111–8. https://doi.org/10.1016/0378-5173(96)04592-9.
Dressman JB. Comparison of canine and human gastrointestinal physiology. Pharm Res. 1986;3(3):123–31.
Culen M, Rezacova A, Jampilek J, Dohnal J. Designing a dynamic dissolution method: a review of instrumental options and corresponding physiology of stomach and small intestine. J Pharm Sci. 2013;102(9):2995–3017. https://doi.org/10.1002/jps.23494.
Schiller C, Frohlich CP, Giessman T, Siegmund W, Monnikes H, Hostein N, Weitschies W. Intestinal fluid volumes and transit of dosage forms as assessed by magnetic resonance imaging. Aliment Pharmacol Ther. 2005;22:971–9.
Malthy JR, Sutherland AD, Sale JP, Shaffer EA. Preoperative oral fluids: is a five-hour fastjustified prior to elective surgery? Anesth Analg. 1986;65:1112–6.
Lydon A, Murray C, McGinley J, Plant R, Duggan F, Shorten G. Cisapride dose not alter gastric volume or pH in patients undergoing ambulatory surgery. Can J Anaesth. 1999;46:1181–4.
Placidi E, Hoad CL, Marciani L, Gowland PA, Spiller RC. Effects of an osmotic laxative on the distribution of water between the small and large intestine in humans. Gut. 2010;59:a141.
Jin C, Zhao C, Shen D, Dong W, Liu H, He Z. Evaluating bioequivalence of meloxicam tablets: is in-vitro dissolution test overdiscriminating? J Pharm Pharmacol. 2018;70(2):250–8. https://doi.org/10.1111/jphp.12859.
Picazo AR, Martinez-Martinez MT, Colón-Useche S, Iriarte R, Sánchez-Dengra B, González-Álvarez M, et al. In vitro dissolution as a tool for formulation selection: telmisartan two-step IVIVC. Mol Pharm. 2018;15(6):2307–15. https://doi.org/10.1021/acs.molpharmaceut.8b00153.
Alkhalidi BA, Al-Ghazawi M, AlKhatib HS, Sallam A. Development of a predictive in vitro dissolution for clarithromycin granular suspension based on in vitro-in vivo correlations. Pharm Dev Technol. 2010;15(3):286–95. https://doi.org/10.3109/10837450903188493.
Vuletić L, Khan MZI, Špoljarić D, Radić M, Cetina-Čižmek B, Filipović-Grčić J. Development of a clinically relevant dissolution method for metaxalone immediate release formulations based on an IVIVC model. Pharm Res. 2018;35(8):163. https://doi.org/10.1007/s11095-018-2434-1.
Kim TH, Shin S, Jeong SW, Lee JB, Shin BS. Physiologically relevant in vitro-in vivo correlation (IVIVC) approach for sildenafil with site-dependent dissolution. Pharmaceutics. 2019;11. https://doi.org/10.3390/pharmaceutics11060251.
Chen R, Blanchard A, Kushner J, Harrignton B, Liu J, DeMatteo V. Developing a biorelevant dissolution method for an extrudable core system (ECS) osmotic tablet. AAPS PharmSciTech. 2022;23:5. https://doi.org/10.1208/s12249-021-02110-x.
Okumu A, DiMaso M, Löbenberg R. Dynamic dissolution testing to establish in vitro/in vivo correlations for montelukast sodium, a poorly soluble drug. Pharm Res. 2008;25(12):2778–85.
Ruff A, Fiolka T, Kostewicz ES. Prediction of ketoconazole absorption using an updated in vitro transfer model coupled to physiologically based pharmacokinetic modelling. Eur J Pharm Sci. 2017;100:42–55.
Tsume Y, Takeuchi S, Matsui K, Amidon GE, Amidon GL. In vitro dissolution-methodology, mini-gastrointestinal simulator (mGIS), predicts better in vivo dissolution of weak base drug, dasatinib. Eur J Pharm Sci. 2015;76:203–12.
Patel S, Zhu W, Xia B, Sharma N, Hermans A, Ehrick JD, Kesisoglou F, Pennington J. Integration of precipitation kinetics from an in vitro, multicompartment transfer system and mechanistic oral absorption modeling for pharmacokinetic prediction of weakly basic drugs. J Pharm Sci. 2019;108:574–83.
Lopes de Castro LM, de Souza J, Caldeira TG, Mapa B, Soares AFM, Pegorelli BG, et al. The evaluation of valsartan biopharmaceutics properties. Curr Drug Res Rev. 2020;12(1):52–62. https://doi.org/10.2174/2589977511666191210151120.
Ono A, Sugano K. Application of the BCS biowaiver approach to assessing bioequivalence of orally disintegrating tablets with immediate release formulations. Eur J Pharm Sci. 2014;64:37–43. https://doi.org/10.1016/j.ejps.2014.08.003.
Rosa LS, Marques-Marinho FD, Braga SL, de Souza J. Equilibrium solubility study to determine fexofenadine hydrochloride bcs class and challenges in establishing conditions for dissolution profiles applied to suspension. Braz J Pharm Sci. 2020;56(1–10):e17737.
Johnson LR. Salivary secretion. In: Johnson LR, editor. Gastrointestinal physiology. St. Louis: Mosby; 1997. p. 59–68.
Evonik Industries AG. https://healthcare.evonik.com/en/pharmaceuticals/oral-drug-delivery/oral-excipients/eudragit-portfolio/immediate-release. Accessed 16 Jan 2022.
Steingoetter A, Fox M, Treier R, Weishaupt D, Marincek B, Boesiger P, et al. Effects of posture on the physiology of gastric emptying: a magnetic resonance imaging study. Scand J Gastroenterol. 2006;41(10):1155–64. https://doi.org/10.1080/00365520600610451.
Yamaoka K, Nakagawa T. A nonlinear least squares program based on differential equations, MULTI (RUNGE), for microcomputers. J Pharmacobio-Dyn. 1983;6(8):595–606. https://doi.org/10.1248/bpb1978.6.595.
Valsartan, 2013. Drug Information from the manufacture. https://www.pmda.go.jp/PmdaSearch/iyakuDetail/GeneralList/2149041F1. Accessed 16 Jan 2022.
Sester C, Ofridam F, Lebaz N, Gagniere E, Mangin D, Elaissari A. pH-sensitive methacrylic acid-methyl methacrylate copolymer Eudragit L100 and dimethylaminoethyl methacrylate, butyl methacrylate, and methyl methacrylate tri-copolymer Eudragit E100. Polymer Adv Technol. 2020;31:440–50.
Singh AP, Siddiqui J, Diosady LL. Characterizing the pH-dependent release kinetics of food-grade spray drying encapsulated iron microcapsules for food fortification. Food Bioprocess Technol. 2018;11:435–46.
Elder D, Symonds J. Dissolution testing in the modern world. Eur Pharm Rev. 2016; 29 Feb. https://www.europeanpharmaceuticalreview.com/article/39248/dissolution-test-ing-in-the-modern-world/.
Klein S. The mini paddle apparatus-a useful tool in the early developmental stage? Experiences with immediate-release dosage forms. Dissolution Tech. 2006; Nov. https://doi.org/10.14227/DT130406P6.
Acknowledgments
This study was performed as the joint research between Towa Pharmaceutical Co., Ltd. and Okayama University.
Author information
Authors and Affiliations
Contributions
Motoki Onishi; Conceptualization, Methodology, Writing, Acquisition, Analysis and interpretation of data: Kozo Tagawa; Conceptualization, Methodology: Maiko Jiko; Acquisition of data: Kayo Koike; Acquisition of data: Masato Maruyama; Interpretation of data: Hidetoshi Hashizume; Interpretation of data: Kazuhide Imagaki; Supervision: Kazutaka Higaki; Conceptualization, Methodology, Writing, Visualization, interpretation of data, Supervision.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing financial interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Onishi, M., Tagawa, K., Jiko, M. et al. Efficient Evaluation of In Vivo Performance in Human for Generic Formulation by Novel Dissolution-Absorption Prediction (DAP) Workflow. Pharm Res 39, 2203–2216 (2022). https://doi.org/10.1007/s11095-022-03337-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-022-03337-4