Abstract
Purpose
Tumor infiltration by immunosuppressive myeloid cells or tumor-associated macrophages (TAMs) contributes to tumor progression and metastasis. In contrast to their adult counterparts, higher TAM signatures do not correlate with aggressive tumor behavior in pediatric brain tumors. While prominent TAM infiltrates exist before and after radiation, the degree to which irradiated macrophages and microglia support progression or leptomeningeal metastasis remains unclear. Patients with medulloblastoma often present with distant metastases and tumor recurrence is largely incurable, making them prime candidates for the study of novel approaches to prevent neuroaxis dissemination and recurrence.
Methods
Macrophage depletion was achieved using CSF-1 receptor inhibitors (CSF-1Ri), BLZ945 and AFS98, with or without whole brain radiation in a variety of medulloblastoma models, including patient-derived xenografts bearing Group 3 medulloblastoma and a transgenic Sonic Hedgehog (Ptch1+/−, Trp53−/−) medulloblastoma model.
Results
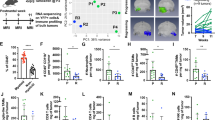
Effective reduction of microglia, TAM, and spinal cord macrophage with CSF-1Ri resulted in negligible effects on the rate of local and spinal recurrences or survival following radiation. Results were comparable between medulloblastoma subgroups. While notably few tumor-infiltrating lymphocytes (TILs) were detected, average numbers of CD3+ TILs and FoxP3+ Tregs did not differ between groups following treatment and tumor aggressiveness by Ki67 proliferation index was unaltered.
Conclusion
In the absence of other microenvironmental influences, medulloblastoma-educated macrophages do not operate as tumor-supportive cells or promote leptomeningeal recurrence in these models. Our data add to a growing body of literature describing a distinct immunophenotype amid the medulloblastoma microenvironment and highlight the importance of appropriate pediatric modeling prior to clinical translation.





Similar content being viewed by others
Availability of data and materials
All data generated or analyzed during this study are included in this published article [and its supplementary information files].
References
Chen JJW, Lin Y-C, Yao P-L, Yuan A, Chen H-Y, Shun C-T, Tsai M-F, Chen C-H, Yang P-C (2005) Tumor-associated macrophages: the double-edged sword in cancer progression. J Clin Oncol 23(5):953–964. https://doi.org/10.1200/jco.2005.12.172
Mantovani A, Marchesi F, Malesci A, Laghi L, Allavena P (2017) Tumour-associated macrophages as treatment targets in oncology. Nat Rev Clin Oncol 14(7):399–416. https://doi.org/10.1038/nrclinonc.2016.217
Stafford JH, Hirai T, Deng L, Chernikova SB, Urata K, West BL, Brown JM (2016) Colony stimulating factor 1 receptor inhibition delays recurrence of glioblastoma after radiation by altering myeloid cell recruitment and polarization. Neuro Oncol 18(6):797–806. https://doi.org/10.1093/neuonc/nov272
Yan D, Kowal J, Akkari L, Schuhmacher AJ, Huse JT, West BL, Joyce JA (2017) Inhibition of colony stimulating factor-1 receptor abrogates microenvironment-mediated therapeutic resistance in gliomas. Oncogene 36(43):6049–6058. https://doi.org/10.1038/onc.2017.261
Palma MD, Lewis CE (2013) Macrophage regulation of tumor responses to anticancer therapies. Cancer Cell 23(3):277–286. https://doi.org/10.1016/j.ccr.2013.02.013
Poon CC, Sarkar S, Yong VW, Kelly JJP (2017) Glioblastoma-associated microglia and macrophages: targets for therapies to improve prognosis. Brain 140(6):1548–1560. https://doi.org/10.1093/brain/aww355
Campbell MJ, Tonlaar NY, Garwood ER, Huo D, Moore DH, Khramtsov AI, Au A, Baehner F, Chen Y, Malaka DO, Lin A, Adeyanju OO, Li S, Gong C, McGrath M, Olopade OI, Esserman LJ (2011) Proliferating macrophages associated with high grade, hormone receptor negative breast cancer and poor clinical outcome. Breast Cancer Res Treat 128(3):703–711. https://doi.org/10.1007/s10549-010-1154-y
Steidl C, Diepstra A, Lee T, Chan FC, Farinha P, Tan K, Telenius A, Barclay L, Shah SP, Connors JM, Van Den Berg A, Gascoyne RD (2012) Gene expression profiling of microdissected Hodgkin Reed-Sternberg cells correlates with treatment outcome in classical Hodgkin lymphoma. Blood 120(17):3530–3540. https://doi.org/10.1182/blood-2012-06-439570
Zhu X-D, Zhang J-B, Zhuang P-Y, Zhu H-G, Zhang W, Xiong Y-Q, Wu W-Z, Wang L, Tang Z-Y, Sun H-C (2008) High expression of macrophage colony-stimulating factor in peritumoral liver tissue is associated with poor survival after curative resection of hepatocellular carcinoma. J Clin Oncol 26(16):2707–2716. https://doi.org/10.1200/jco.2007.15.6521
Jia JB, Wang WQ, Sun HC, Zhu XD, Liu L, Zhuang PY, Zhang JB, Zhang W, Xu HX, Kong LQ, Lu L, Wu WZ, Wang L, Tang ZY (2010) High expression of macrophage colony-stimulating factor-1 receptor in peritumoral liver tissue is associated with poor outcome in hepatocellular carcinoma after curative resection. Oncologist 15(7):732–743. https://doi.org/10.1634/theoncologist.2009-0170
Plant AS, Koyama S, Sinai C, Solomon IH, Griffin GK, Ligon KL, Bandopadhayay P, Betensky R, Emerson R, Dranoff G, Kieran MW, Ritz J (2018) Immunophenotyping of pediatric brain tumors: correlating immune infiltrate with histology, mutational load, and survival and assessing clonal T cell response. J Neurooncol. https://doi.org/10.1007/s11060-017-2737-9
Griesinger AM, Birks DK, Donson AM, Amani V, Hoffman LM, Waziri A, Wang M, Handler MH, Foreman NK (2013) Characterization of distinct immunophenotypes across pediatric brain tumor types. J Immunol 191(9):4880–4888. https://doi.org/10.4049/jimmunol.1301966
Mackay A, Burford A, Carvalho D, Izquierdo E, Fazal-Salom J, Taylor KR, Bjerke L, Clarke M, Vinci M, Nandhabalan M, Temelso S, Popov S, Molinari V, Raman P, Waanders AJ, Han HJ, Gupta S, Marshall L, Zacharoulis S, Vaidya S, Mandeville HC, Bridges LR, Martin AJ, Al-Sarraj S, Chandler C, Ng H-K, Li X, Mu K, Trabelsi S, Brahim DHM-B, Kisljakov AN, Konovalov DM, Moore AS, Carcaboso AM, Sunol M, De Torres C, Cruz O, Mora J, Shats LI, Stavale JN, Bidinotto LT, Reis RM, Entz-Werle N, Farrell M, Cryan J, Crimmins D, Caird J, Pears J, Monje M, Debily M-A, Castel D, Grill J, Hawkins C, Nikbakht H, Jabado N, Baker SJ, Pfister SM, Jones DTW, Fouladi M, Von Bueren AO, Baudis M, Resnick A, Jones C (2017) Integrated molecular meta-analysis of 1,000 pediatric high-grade and diffuse intrinsic pontine glioma. Cancer Cell 32(4):520-537.e525. https://doi.org/10.1016/j.ccell.2017.08.017
Mackay A, Burford A, Molinari V, Jones DTW, Izquierdo E, Brouwer-Visser J, Giangaspero F, Haberler C, Pietsch T, Jacques TS, Figarella-Branger D, Rodriguez D, Morgan PS, Raman P, Waanders AJ, Resnick AC, Massimino M, Garrè ML, Smith H, Capper D, Pfister SM, Würdinger T, Tam R, Garcia J, Thakur MD, Vassal G, Grill J, Jaspan T, Varlet P, Jones C (2018) Molecular, pathological, radiological, and immune profiling of non-brainstem pediatric high-grade glioma from the HERBY Phase II Randomized Trial. Cancer Cell 33(5):829-842.e825. https://doi.org/10.1016/j.ccell.2018.04.004
Koschmann C, Bloom K, Upadhyaya S, Geyer JR, Leary SE (2016) Survival after relapse of medulloblastoma. J Pediatr Hematol Oncol 38(4):269–273. https://doi.org/10.1097/mph.0000000000000547
Sabel M, Fleischhack G, Tippelt S, Gustafsson G, Doz F, Kortmann R, Massimino M, Navajas A, Von Hoff K, Rutkowski S, Warmuth-Metz M, Clifford SC, Pietsch T, Pizer B, Lannering B (2016) Relapse patterns and outcome after relapse in standard risk medulloblastoma: a report from the HIT-SIOP-PNET4 study. J Neurooncol 129(3):515–524. https://doi.org/10.1007/s11060-016-2202-1
Thomas PRM, Deutsch M, Kepner JL, Boyett JM, Krischer J, Aronin P, Albright L, Allen JC, Packer RJ, Linggood R, Mulhern R, Stehbens JA, Langston J, Stanley P, Duffner P, Rorke L, Cherlow J, Friedman HS, Finlay JL, Vietti TJ, Kun LE (2000) Low-stage medulloblastoma: final analysis of trial comparing standard-dose with reduced-dose neuraxis irradiation. J Clin Oncol 18(16):3004–3011. https://doi.org/10.1200/jco.2000.18.16.3004
Wang S-C, Yu C-F, Hong J-H, Tsai C-S, Chiang C-S (2013) Radiation therapy-induced tumor invasiveness is associated with SDF-1-regulated macrophage mobilization and vasculogenesis. PLoS ONE 8(8):e69182. https://doi.org/10.1371/journal.pone.0069182
Kioi M, Vogel H, Schultz G, Hoffman RM, Harsh GR, Brown JM (2010) Inhibition of vasculogenesis, but not angiogenesis, prevents the recurrence of glioblastoma after irradiation in mice. J Clin Invest 120(3):694–705. https://doi.org/10.1172/jci40283
Pyonteck SM, Akkari L, Schuhmacher AJ, Bowman RL, Sevenich L, Quail DF, Olson OC, Quick ML, Huse JT, Teijeiro V, Setty M, Leslie CS, Oei Y, Pedraza A, Zhang J, Brennan CW, Sutton JC, Holland EC, Daniel D, Joyce JA (2013) CSF-1R inhibition alters macrophage polarization and blocks glioma progression. Nat Med 19(10):1264–1272. https://doi.org/10.1038/nm.3337
Xu J, Escamilla J, Mok S, David J, Priceman S, West B, Bollag G, McBride W, Wu L (2013) CSF1R signaling blockade stanches tumor-infiltrating myeloid cells and improves the efficacy of radiotherapy in prostate cancer. Cancer Res 73(9):2782–2794. https://doi.org/10.1158/0008-5472.can-12-3981
Akkari L, Bowman RL, Tessier J, Klemm F, Handgraaf SM, De Groot M, Quail DF, Tillard L, Gadiot J, Huse JT, Brandsma D, Westerga J, Watts C, Joyce JA (2020) Dynamic changes in glioma macrophage populations after radiotherapy reveal CSF-1R inhibition as a strategy to overcome resistance. Sci Transl Med 12(552):eaaw7843. https://doi.org/10.1126/scitranslmed.aaw7843
Hume DA, Macdonald KPA (2012) Therapeutic applications of macrophage colony-stimulating factor-1 (CSF-1) and antagonists of CSF-1 receptor (CSF-1R) signaling. Blood 119(8):1810–1820. https://doi.org/10.1182/blood-2011-09-379214
Conway JG, McDonald B, Parham J, Keith B, Rusnak DW, Shaw E, Jansen M, Lin P, Payne A, Crosby RM, Johnson JH, Frick L, Lin MHJ, Depee S, Tadepalli S, Votta B, James I, Fuller K, Chambers TJ, Kull FC, Chamberlain SD, Hutchins JT (2005) Inhibition of colony-stimulating-factor-1 signaling in vivo with the orally bioavailable cFMS kinase inhibitor GW2580. PNAS 102(44):16078–16083. https://doi.org/10.1073/pnas.0502000102
Webb MW, Sun J, Sheard MA, Liu WY, Wu HW, Jackson JR, Malvar J, Sposto R, Daniel D, Seeger RC (2018) C olony stimulating factor 1 receptor blockade improves the efficacy of chemotherapy against human neuroblastoma in the absence of T lymphocytes. Int J Cancer 143(6):1483–1493. https://doi.org/10.1002/ijc.31532
Wesolowski R, Sharma N, Reebel L, Rodal MB, Peck A, West BL, Marimuthu A, Severson P, Karlin DA, Dowlati A, Le MH, Coussens LM, Rugo HS (2019) Phase Ib study of the combination of pexidartinib (PLX3397), a CSF-1R inhibitor, and paclitaxel in patients with advanced solid tumors. Ther Adv Med Oncol 11:175883591985423. https://doi.org/10.1177/1758835919854238
Carola M, Hoves S, Benz J, Wartha K, Runza V, Rey-Giraud F, Leon FF, Klaman I, Jones T, Jucknischke U, Scheiblich S, Kaluza K, Ingo WA, Abiraj K, Philippe SA, Gomez-Roca C, Karin IA, Christophe D-P, Levitsky H, Blay J-Y, Rüttinger D (2014) Targeting tumor-associated macrophages with anti-CSF-1R antibody reveals a strategy for cancer therapy. Cancer Cell 25(6):846–859. https://doi.org/10.1016/j.ccr.2014.05.016
Brabetz S, Leary SES, Gröbner SN, Nakamoto MW, Şeker-Cin H, Girard EJ, Cole B, Strand AD, Bloom KL, Hovestadt V, Mack NL, Pakiam F, Schwalm B, Korshunov A, Balasubramanian GP, Northcott PA, Pedro KD, Dey J, Hansen S, Ditzler S, Lichter P, Chavez L, Jones DTW, Koster J, Pfister SM, Kool M, Olson JM (2018) A biobank of patient-derived pediatric brain tumor models. Nat Med 24(11):1752–1761. https://doi.org/10.1038/s41591-018-0207-3
Romer JT, Kimura H, Magdaleno S, Sasai K, Fuller C, Baines H, Connelly M, Stewart CF, Gould S, Rubin LL, Curran T (2004) Suppression of the Shh pathway using a small molecule inhibitor eliminates medulloblastoma in Ptc1+/−p53−/− mice. Cancer Cell 6(3):229–240. https://doi.org/10.1016/j.ccr.2004.08.019
Chen Y-F, Fu L-W (2011) Mechanisms of acquired resistance to tyrosine kinase inhibitors. Acta Pharm 1(4):197–207. https://doi.org/10.1016/j.apsb.2011.10.007
Jiao Q, Bi L, Ren Y, Song S, Wang Q, Wang Y-S (2018) Advances in studies of tyrosine kinase inhibitors and their acquired resistance. Mol Cancer. https://doi.org/10.1186/s12943-018-0801-5
Wyckoff J, Wang W, Lin EY, Wang Y, Pixley F, Stanley ER, Graf T, Pollard JW, Segall J, Condeelis J (2004) A paracrine loop between tumor cells and macrophages is required for tumor cell migration in mammary tumors. Cancer Res 64(19):7022–7029. https://doi.org/10.1158/0008-5472.can-04-1449
Condeelis J, Pollard JW (2006) Macrophages: obligate partners for tumor cell migration, invasion, and metastasis. Cell 124(2):263–266. https://doi.org/10.1016/j.cell.2006.01.007
Coniglio SJ, Eugenin E, Dobrenis K, Stanley ER, West BL, Symons MH, Segall JE (2012) Microglial stimulation of glioblastoma invasion involves epidermal growth factor receptor (EGFR) and colony stimulating factor 1 receptor (CSF-1R) signaling. Mol Med 18(3):519–527. https://doi.org/10.2119/molmed.2011.00217
Northcott PA, Korshunov A, Witt H, Hielscher T, Eberhart CG, Mack S, Bouffet E, Clifford SC, Hawkins CE, French P, Rutka JT, Pfister S, Taylor MD (2011) Medulloblastoma comprises four distinct molecular variants. J Clin Oncol 29(11):1408–1414. https://doi.org/10.1200/jco.2009.27.4324
Margol AS, Robison NJ, Gnanachandran J, Hung LT, Kennedy RJ, Vali M, Dhall G, Finlay JL, Erdreich-Epstein A, Krieger MD, Drissi R, Fouladi M, Gilles FH, Judkins AR, Sposto R, Asgharzadeh S (2015) Tumor-associated macrophages in SHH subgroup of medulloblastomas. Clin Cancer Res 21(6):1457–1465. https://doi.org/10.1158/1078-0432.ccr-14-1144
Michele C (2013) Macrophage regulation of tumor responses to anticancer therapies. Cancer Cell 23(3):277–286. https://doi.org/10.1016/j.ccr.2013.02.013
Qian B-Z, Pollard JW (2010) Macrophage diversity enhances tumor progression and metastasis. Cell 141(1):39–51. https://doi.org/10.1016/j.cell.2010.03.014
Lieberman NAP, Degolier K, Kovar HM, Davis A, Hoglund V, Stevens J, Winter C, Deutsch G, Furlan SN, Vitanza NA, Leary SES, Crane CA (2019) Characterization of the immune microenvironment of diffuse intrinsic pontine glioma: implications for development of immunotherapy. Neuro Oncol 21(1):83–94. https://doi.org/10.1093/neuonc/noy145
Maximov V, Chen Z, Wei Y, Robinson MH, Herting CJ, Shanmugam NS, Rudneva VA, Goldsmith KC, Macdonald TJ, Northcott PA, Hambardzumyan D, Kenney AM (2019) Tumour-associated macrophages exhibit anti-tumoural properties in Sonic Hedgehog medulloblastoma. Nat Commun. https://doi.org/10.1038/s41467-019-10458-9
Wes PD, Holtman IR, Boddeke EWGM, Möller T, Eggen BJL (2016) Next generation transcriptomics and genomics elucidate biological complexity of microglia in health and disease. Glia 64(2):197–213. https://doi.org/10.1002/glia.22866
Peng X (2019) Preclinical evaluation of 3D185, a novel potent inhibitor of FGFR1/2/3 and CSF1-R, in FGFR-dependent and macrophage-dominant cancer models. J Exp Clin Cancer Res. https://doi.org/10.1186/s13046-019-1357-y
Quintana E, Schulze CJ, Myers DR, Choy TJ, Mordec K, Wildes D, Tobvis Shifrin N, Belwafa A, Koltun ES, Gill AL, Singh M, Kelsey S, Goldsmith MA, Nichols R, Smith JAM (2020) Allosteric inhibition of SHP2 stimulates anti-tumor immunity by transforming the immunosuppressive environment. Cancer Res. https://doi.org/10.1158/0008-5472.can-19-3038
Endersby R, Whitehouse J, Pribnow A, Kuchibhotla M, Hii H, Carline B, Gande S, Stripay J, Ancliffe M, Howlett M, Schoep T, George C, Andradas C, Dyer P, Schluck M, Patterson B, Tacheva-Gigorova SK, Cooper MN, Robinson G, Stewart C, Pfister SM, Kool M, Milde T, Gajjar A, Johns T, Wechsler-Reya RJ, Roussel MF, Gottardo NG (2021) Small-molecule screen reveals synergy of cell cycle checkpoint kinase inhibitors with DNA-damaging chemotherapies in medulloblastoma. Sci Transl Med 13(577):eaba7401. https://doi.org/10.1126/scitranslmed.aba7401
Shankarappa PS, Peer CJ, Odabas A, McCully CL, Garcia RC, Figg WD, Warren KE (2020) Cerebrospinal fluid penetration of the colony-stimulating factor-1 receptor (CSF-1R) inhibitor, pexidartinib. Cancer Chemother Pharmacol 85(5):1003–1007. https://doi.org/10.1007/s00280-020-04071-7
Monica A, Maya N, Elizabeth R, Kitazawa M, Matusow B, Nguyen H, Brian K (2014) Colony-stimulating factor 1 receptor signaling is necessary for microglia viability, unmasking a microglia progenitor cell in the adult brain. Neuron 82(2):380–397. https://doi.org/10.1016/j.neuron.2014.02.040
Rice RA, Pham J, Lee RJ, Najafi AR, West BL, Green KN (2017) Microglial repopulation resolves inflammation and promotes brain recovery after injury. Glia 65(6):931–944. https://doi.org/10.1002/glia.23135
Xu J, Erdreich-Epstein A, Gonzalez-Gomez I, Melendez EY, Smbatyan G, Moats RA, Rosol M, Biegel JA, Reynolds CP (2012) Novel cell lines established from pediatric brain tumors. J Neurooncol 107(2):269–280
Smith KS, Xu K, Mercer KS, Boop F, Klimo P, Decupyere M, Grenet J, Robinson S, Dunphy P, Baker SJ, Ellison DW, Merchant TE, Upadayaya SA, Gajjar A, Wu G, Orr BA, Robinson GW, Northcott PA, Roussel MF (2020) Patient-derived orthotopic xenografts of pediatric brain tumors: a St. Jude resource. Acta Neuropathol 140(2):209–225. https://doi.org/10.1007/s00401-020-02171-5
Acknowledgements
We thank the families who kindly donated tumor tissue to establish our repository of cell lines housed in the Brain Tumor Resource Lab (www.btrl.org). Special thanks to Peter Murray and all members of the Olson and Roussel-Sherr laboratories for technical support and mentorship.
Funding
This research was supported by the Ruth L. Kirschstein National Research Service Award (5T32CA009351; EEC) and NIH Grants, 2R01CA114567 (JMO), PO1CA96832, and Core Grant CA21765 (MFR). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. We are grateful for additional generous funding from the Seattle Run of Hope, the Pediatric Brain Tumor Research Fund Guild of Seattle Children’s Hospital, Unravel Pediatric Cancer and the American Lebanese-Syrian Associated Charities.
Author information
Authors and Affiliations
Contributions
EEC, YDC, SMCS, and EG performed and analyzed experiments. KB provided technical assistance. FP performed histopathological analyses. EEC, AM, MFR and JMO conceived, designed, and supervised the study. EEC wrote the manuscript with edits and final approval from all authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All human tissue procurement was in accordance with the ethical standards of our institution and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Crotty, E.E., Smith, S.M.C., Brasel, K. et al. Medulloblastoma recurrence and metastatic spread are independent of colony-stimulating factor 1 receptor signaling and macrophage survival. J Neurooncol 153, 225–237 (2021). https://doi.org/10.1007/s11060-021-03767-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-021-03767-x