Abstract
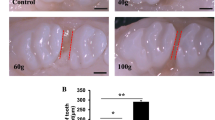
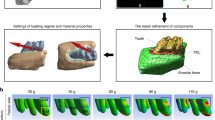
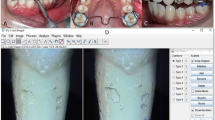
Root resorption is a common complication during orthodontic treatment. Microcracks occur on the root surface after an orthodontic force is applied and may be related to the root resorption caused by the orthodontic process. However, the mechanisms underlying root resorption induced by microcracks remain unclear. In this study, a rat orthodontic model was used to investigate the biological mechanisms of root resorption caused by microcracks. First, the first molar was loaded with 0.5-N orthodontic force for 7 days, and microcracks were observed on the root apex surface using a scanning electron microscope. Second, to describe the mechanical principle resulting in microcracks, a finite element model of rat orthodontics was established, which showed that a maximum stress on the root apex can cause microcrack extension. Third, after 7 days of loading in vivo, histological observation revealed that root resorption occurred in the stress concentration area and cementoclasts appeared in the resorption cavity. Finally, proteomics analysis of the root apex area, excluding the periodontal ligament, revealed that the NOX2, Aifm1, and MAPK signaling pathways were involved in the root resorption process. Microcrack extension on the root surface increases calcium ion concentrations, alters the proteins related to root resorption, and promotes cementoclast formation.








Similar content being viewed by others
References
Abass, S. K., and J. K. Hartsfield. Orthodontics and external apical root resorption. Semin. Orthod. 13:246–256, 2007.
Alvares, K., C. J. DeHart, P. M. Thomas, N. L. Kelleher, and A. Veis. The unique biomineralization transcriptome and proteome of Lytechinus variegatus teeth. Connect. Tissue Res. 59:20–29, 2018.
Bhattacharjee, N., S. Barma, N. Konwar, S. Dewanjee, and P. Manna. Mechanistic insight of diabetic nephropathy and its pharmacotherapeutic targets: an update. Eur. J. Pharmacol. 791:8–24, 2016.
Brudvik, P., and P. Rygh. Multi-nucleated cells remove the main hyalinized tissue and start resorption of adjacent root surfaces. Eur. J. Orthod. 16:265–273, 1994.
Brudvik, P., and P. Rygh. Root resorption beneath the main hyalinized zone. Eur. J. Orthod. 16:249–263, 1994.
Cardoso, L., B. C. Herman, O. Verborgt, D. Laudier, R. J. Majeska, and M. B. Schaffler. Osteocyte apoptosis controls activation of intracortical resorption in response to bone fatigue. J Bone Miner Res 24:597–605, 2009.
Cohn, Z. A., and B. Benson. The in vitro differentiation of mononuclear phagocytes: II. The influence of serum on granule granule formation, hydrolase production, and pinocytosis. J. Exp. Med. 121:835–848, 1965.
Conesa, A., S. Götz, J. M. García-Gómez, J. Terol, M. Talón, and M. Robles. Blast2GO: a universal tool for annotation, visualization and analysis in functional genomics research. Bioinformatics 21:3674–3676, 2005.
DeLaurier, A., A. Boyde, M. A. Horton, and J. S. Price. Analysis of the surface characteristics and mineralization status of feline teeth using scanning electron microscopy. J. Anat. 209:655–669, 2006.
Dimayacyac-Esleta, B. R. T., C.-F. Tsai, R. B. Kitata, P.-Y. Lin, W.-K. Choong, T.-D. Lin, Y.-T. Wang, S.-H. Weng, P.-C. Yang, S. D. Arco, T.-Y. Sung, and Y.-J. Chen. Rapid high-pH reverse phase StageTip for sensitive small-scale membrane proteomic profiling. Anal. Chem. 87:12016–12023, 2015.
Donaldson, F., D. Ruffoni, P. Schneider, A. Levchuk, A. Zwahlen, P. Pankaj, and R. Müller. Modeling microdamage behavior of cortical bone. Biomech. Model. Mechanobiol. 13:1227–1242, 2014.
El-Benna, J., P. M.-C. Dang, M.-A. Gougerot-Pocidalo, J.-C. Marie, and F. Braut-Boucher. p47phox, the phagocyte NADPH oxidase/NOX2 organizer: structure, phosphorylation and implication in diseases. Exp. Mol. Med. 41:217–225, 2009.
Giuliani, N., M. Ferretti, M. Bolzoni, P. Storti, M. Lazzaretti, B. Dalla Palma, S. Bonomini, E. Martella, L. Agnelli, A. Neri, F. Ceccarelli, and C. Palumbo. Increased osteocyte death in multiple myeloma patients: role in myeloma-induced osteoclast formation. Leukemia 26:1391–1401, 2012.
Gonzales, C., H. Hotokezaka, Y. Arai, T. Ninomiya, J. Tominaga, I. Jang, Y. Hotokezaka, M. Tanaka, and N. Yoshida. An in vivo 3D micro-CT evaluation of tooth movement after the application of different force magnitudes in rat molar. Angle Orthod. 79:703–714, 2009.
Görlach, A., K. Bertram, S. Hudecova, and O. Krizanova. Calcium and ROS: a mutual interplay. Redox Biol. 6:260–271, 2015.
Götz, S., J. M. García-Gómez, J. Terol, T. D. Williams, S. H. Nagaraj, M. J. Nueda, M. Robles, M. Talón, J. Dopazo, and A. Conesa. High-throughput functional annotation and data mining with the Blast2GO suite. Nucleic Acids Res. 36:3420–3435, 2008.
Gu, G., M. Mulari, Z. Peng, T. A. Hentunen, and H. K. Väänänen. Death of osteocytes turns off the inhibition of osteoclasts and triggers local bone resorption. Biochem. Biophys. Res. Commun. 335:1095–1101, 2005.
Guan, L., S. Lin, W. Yan, L. Chen, and X. Wang. Effects of calcitonin on orthodontic tooth movement and associated root resorption in rats. Acta Odontol. Scand. 75:595–602, 2017.
Herman, B. C., L. Cardoso, R. J. Majeska, K. J. Jepsen, and M. B. Schaffler. Activation of bone remodeling after fatigue: differential response to linear microcracks and diffuse damage. Bone 47:766–772, 2010.
Hichijo, N., E. Tanaka, N. Kawai, L. J. van Ruijven, and G. E. J. Langenbach. Effects of decreased occlusal loading during growth on the mandibular bone characteristics. PLoS ONE 10:e0129290, 2015.
Ibrahim, A. Y., S. Gudhimella, S. N. Pandruvada, and S. S. Huja. Resolving differences between animal models for expedited orthodontic tooth movement. Orthod. Craniofac. Res. 20:72–76, 2017.
Iglesias-Linares, A., and J. J. K. Hartsfield. Cellular and molecular pathways leading to external root resorption. J. Dent. Res. 96:145–152, 2017.
Inubushi, T., E. Tanaka, E. B. Rego, J. Ohtani, A. Kawazoe, K. Tanne, M. Miyauchi, and T. Takata. Ultrasound stimulation attenuates resorption of tooth root induced by experimental force application. Bone 53:497–506, 2013.
Jiang, H., Y. Ren, Z. Liu, and S. Zhang. Microscale finite element analysis for predicting effects of air voids on mechanical properties of single fiber bundle in composites. J. Mater. Sci. 54:1363–1381, 2019.
Jung, H., and O. Akkus. Activation of intracellular calcium signaling in osteoblasts colocalizes with the formation of post-yield diffuse microdamage in bone matrix. Bonekey Rep. 5:778, 2016.
Kawarizadeh, A., C. Bourauel, and A. Jäger. Experimental and numerical determination of initial tooth mobility and material properties of the periodontal ligament in rat molar specimens. Eur. J. Orthod. 25:569–578, 2003.
Kilkenny, C., W. J. Browne, I. C. Cuthill, M. Emerson, and D. G. Altman. Improving bioscience research reporting: the ARRIVE guidelines for reporting animal research. PLoS Biol. 8:e1000412, 2010.
Lee, D. G., S.-H. Kim, S. Kim, J. H. Yu, and S. W. Cho. Prediction of material properties of ceramic composite material by porous structure and porosity using the finite element method. Int. J. Precis. Eng. Manuf. 20:805–814, 2019.
Levine, J., E. Kwon, P. Paez, W. Yan, G. Czerwieniec, J. A. Loo, M. V. Sofroniew, and I.-B. Wanner. Traumatically injured astrocytes release a proteomic signature modulated by STAT3-dependent cell survival. Glia 64:668–694, 2016.
Lim, J.-A., L. Li, O. Kakhlon, R. Myerowitz, and N. Raben. Defects in calcium homeostasis and mitochondria can be reversed in Pompe disease. Autophagy 11:385–402, 2015.
Lü, L.-W., G.-W. Meng, and Z.-H. Liu. Finite element analysis of multi-piece post-crown restoration using different types of adhesives. Int. J. Oral Sci. 5:162–166, 2013.
Lyu, C., L. Zhang, and S. Zou. The effectiveness of supplemental vibrational force on enhancing orthodontic treatment. A systematic review. Eur. J. Orthod. 41:502–512, 2019.
Marco, M., E. Giner, R. Larraínzar-Garijo, J. R. Caeiro, and M. H. Miguélez. Numerical modelling of femur fracture and experimental validation using bone simulant. Ann. Biomed. Eng. 45:2395–2408, 2017.
Matsumoto, Y., S. Sringkarnboriboon, and T. Ono. Proinflammatory mediators related to orthodontically induced periapical root resorption in rat mandibular molars. Eur. J. Orthod. 39:686–691, 2017.
Mentaverri, R., S. Yano, N. Chattopadhyay, L. Petit, O. Kifor, S. Kamel, E. F. Terwilliger, M. Brazier, and E. M. Brown. The calcium sensing receptor is directly involved in both osteoclast differentiation and apoptosis. FASEB J. 20:2562–2564, 2006.
Michelogiannakis, D., D. Al-Shammery, Z. Akram, P. E. Rossouw, F. Javed, and G. E. Romanos. Influence of low-level laser therapy on orthodontically-induced inflammatory root resorption. A systematic review. Arch. Oral Biol. 100:1–13, 2019.
Milne, T. J., I. Ichim, B. Patel, A. McNaughton, and M. C. Meikle. Induction of osteopenia during experimental tooth movement in the rat: alveolar bone remodelling and the mechanostat theory. Eur. J. Orthod. 31:221–231, 2009.
Miyake, N., N. I. Wolf, F. K. Cayami, J. Crawford, A. Bley, D. Bulas, A. Conant, S. J. Bent, K. W. Gripp, A. Hahn, S. Humphray, S. Kimura-Ohba, Z. Kingsbury, B. R. Lajoie, D. Lal, D. Micha, A. Pizzino, R. J. Sinke, D. Sival, I. Stolte-Dijkstra, A. Superti-Furga, N. Ulrick, R. J. Taft, T. Ogata, K. Ozono, N. Matsumoto, B. A. Neubauer, C. Simons, and A. Vanderver. X-linked hypomyelination with spondylometaphyseal dysplasia (H-SMD) associated with mutations in AIFM1. Neurogenetics 18:185–194, 2017.
Nayyer, N., T. Tripathi, P. Rai, and R. Gopal. Effect of photobiomodulation on external root resorption during orthodontic tooth movement—a scoping review. Lasers Dent. Sci. 3:219–226, 2019.
Ochiai, N., Y. Nakachi, T. Yokoo, T. Ichihara, T. Eriksson, Y. Yonemoto, T. Kato, H. Ogata, N. Fujimoto, Y. Kobayashi, N. Udagawa, S. Kaku, T. Ueki, Y. Okazaki, N. Takahashi, and T. Suda. Murine osteoclasts secrete serine protease HtrA1 capable of degrading osteoprotegerin in the bone microenvironment. Commun. Biol. 2:86, 2019.
Ouyang, S., Z. Deng, and X. Hou. Stress concentration in octagonal honeycombs due to defects. Compos. Struct. 204:814–821, 2018.
Parker, R. J., and E. F. Harris. Directions of orthodontic tooth movements associated with external apical root resorption of the maxillary central incisor. Am. J. Orthod. Dentofac. Orthop. 114:677–683, 1998.
Rahimi, A., L. Keilig, G. Bendels, R. Klein, T. M. Buzug, I. Abdelgader, M. Abboud, and C. Bourauel. 3D Reconstruction of dental specimens from 2D histological images and μCT-Scans. Comput. Methods Biomech. Biomed. Eng. 8:167–176, 2005.
Ru, N., S. S.-Y. Liu, Y. Bai, S. Li, Y. Liu, and X. Wei. BoneCeramic graft regenerates alveolar defects but slows orthodontic tooth movement with less root resorption. Am. J. Orthod. Dentofac. Orthop. 149:523–532, 2016.
Sato, M., K. Nagata, S. Kuroda, S. Horiuchi, T. Nakamura, M. Karima, T. Inubushi, and E. Tanaka. Low-intensity pulsed ultrasound activates integrin-mediated mechanotransduction pathway in synovial cells. Ann. Biomed. Eng. 42:2156–2163, 2014.
Schileo, E., F. Taddei, L. Cristofolini, and M. Viceconti. Subject-specific finite element models implementing a maximum principal strain criterion are able to estimate failure risk and fracture location on human femurs tested in vitro. J. Biomech. 41:356–367, 2008.
Schwarz, A. M. Tissue changes incidental to orthodontic tooth movement. Int. J. Orthod. Oral Surg. Radiogr. 18:331–352, 1932.
Shah, A., D. Lee, M. Song, S. Kim, M. K. Kang, and R. H. Kim. Clastic cells are absent around the root surface in pulp-exposed periapical periodontitis lesions in mice. Oral Dis. 24:57–62, 2018.
Shirokova, N., and E. Niggli. Cardiac phenotype of duchenne muscular dystrophy: insights from cellular studies. J. Mol. Cell. Cardiol. 58:217–224, 2013.
Shu, Y., M. J. Baumann, E. D. Case, R. K. Irwin, S. E. Meyer, C. S. Pearson, and L. R. McCabe. Surface microcracks signal osteoblasts to regulate alignment and bone formation. Mater. Sci. Eng. C 44:191–200, 2014.
Simon, A. R., U. Rai, B. L. Fanburg, and B. H. Cochran. Activation of the JAK-STAT pathway by reactive oxygen species. Am. J. Physiol. Physiol. 275:C1640–C1652, 1998.
Spivak, M., J. Weston, L. Bottou, L. Käll, and W. S. Noble. Improvements to the percolator algorithm for peptide identification from shotgun proteomics data sets. J. Proteome Res. 8:3737–3745, 2009.
Sringkarnboriboon, S., Y. Matsumoto, and K. Soma. Root resorption related to hypofunctional periodontium in experimental tooth movement. J. Dent. Res. 82:486–490, 2003.
Tami, A. E., P. Nasser, O. Verborgt, M. B. Schaffler, and M. L. K. Tate. The role of interstitial fluid flow in the remodeling response to fatigue loading. J. Bone Miner. Res. 17:2030–2037, 2002.
Taylor, D., J. G. Hazenberg, and T. C. Lee. Living with cracks: damage and repair in human bone. Nat. Mater. 6:263–268, 2007.
Vasquez-Sancho, F., A. Abdollahi, D. Damjanovic, and G. Catalan. Flexoelectricity in bones. Adv. Mater. 30:1705316, 2018.
Verborgt, O., G. J. Gibson, and M. B. Schaffler. Loss of osteocyte integrity in association with microdamage and bone remodeling after fatigue in vivo. J. Bone Miner. Res. 15:60–67, 2000.
Verna, C., P. M. Cattaneo, and M. Dalstra. Corticotomy affects both the modus and magnitude of orthodontic tooth movement. Eur. J. Orthod. 40:107–112, 2018.
Viecilli, R. F., M. H. Kar-kuri, J. Varriale, A. Budiman, and M. Janal. Effects of initial stresses and time on orthodontic external root resorption. J. Dent. Res. 92:346–351, 2013.
Wiśniewski, J. R., A. Zougman, N. Nagaraj, and M. Mann. Universal sample preparation method for proteome analysis. Nat. Methods 6:359–362, 2009.
Xiao, S., L. Li, L. Wang, Y. Wang, M. Zhang, J. Yao, and Y. Fan. Root surface microcracks induced by orthodontic force as a potential primary indicator of root resorption. J. Biomech. 110:109938, 2020.
Yamaguchi, M., N. Aihara, T. Kojima, and K. Kasai. RANKL increase in compressed periodontal ligament cells from root resorption. J. Dent. Res. 85:751–756, 2006.
Yu, C., D. Huang, K. Wang, B. Lin, Y. Liu, S. Liu, W. Wu, and H. Zhang. Advanced oxidation protein products induce apoptosis, and upregulate sclerostin and RANKL expression, in osteocytic MLO-Y4 cells via JNK/p38 MAPK activation. Mol. Med. Rep. 15:543–550, 2017.
Yuan, S., Z. Yang, and G. Chen. 3D microstructure model and thermal shock failure mechanism of a Si3N4-bonded SiC ceramic refractory with SiC high volume ratio particles. Ceram. Int. 45:4219–4229, 2019.
Zhao, N., B. L. Foster, and L. F. Bonewald. The cementocyte—an osteocyte relative? J. Dent. Res. 95:734–741, 2016.
Zhao, Y., A. Sarkar, and X. Wang. Peptide nucleic acid based tension sensor for cellular force imaging with strong DNase resistance. Biosens. Bioelectron. 150:111959, 2020.
Acknowledgments
This work was supported by the National Natural Science Foundation of China (Nos. U20A20390 and 11827803). We thank Dr. Peng Xu and Dr. Tianyun Jiang for their assistance in guiding the use of related finite element softwares. We thank the Beijing Fangtailun Medical Technology Co., Ltd. for providing the laser transmitter.
Conflict of interest
The authors declare no competing interests.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Associate Editor Eiji Tanaka oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Xiao, S., Li, L., Yao, J. et al. Microcracks on the Rat Root Surface Induced by Orthodontic Force, Crack Extension Simulation, and Proteomics Study. Ann Biomed Eng 49, 2228–2242 (2021). https://doi.org/10.1007/s10439-021-02733-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-021-02733-y