Abstract
Purpose
We conducted a meta-analysis to determine the effect of hyperoxia on muscle sympathetic nerve activity in healthy individuals and those with cardio-metabolic diseases.
Methods
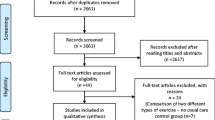
A comprehensive search of electronic databases was performed until August 2022. All study designs (except reviews) were included: population (humans; apparently healthy or with at least one chronic disease); exposures (muscle sympathetic nerve activity during hyperoxia or hyperbaria); comparators (hyperoxia or hyperbaria vs. normoxia); and outcomes (muscle sympathetic nerve activity, heart rate, blood pressure, minute ventilation). Forty-nine studies were ultimately included in the meta-analysis.
Results
In healthy individuals, hyperoxia had no effect on sympathetic burst frequency (mean difference [MD] − 1.07 bursts/min; 95% confidence interval [CI] − 2.17, 0.04bursts/min; P = 0.06), burst incidence (MD 0.27 bursts/100 heartbeats [hb]; 95% CI − 2.10, 2.64 bursts/100 hb; P = 0.82), burst amplitude (P = 0.85), or total activity (P = 0.31). In those with chronic diseases, hyperoxia decreased burst frequency (MD − 5.57 bursts/min; 95% CI − 7.48, − 3.67 bursts/min; P < 0.001) and burst incidence (MD − 4.44 bursts/100 hb; 95% CI − 7.94, − 0.94 bursts/100 hb; P = 0.01), but had no effect on burst amplitude (P = 0.36) or total activity (P = 0.90). Our meta-regression analyses identified an inverse relationship between normoxic burst frequency and change in burst frequency with hyperoxia. In both groups, hyperoxia decreased heart rate but had no effect on any measure of blood pressure.
Conclusion
Hyperoxia does not change sympathetic activity in healthy humans. Conversely, in those with chronic diseases, hyperoxia decreases sympathetic activity. Regardless of disease status, resting sympathetic burst frequency predicts the degree of change in burst frequency, with larger decreases for those with higher resting activity.











Similar content being viewed by others
Data availability
Data will be provided following a reasonable request to the corresponding author.
References:
Grou NO (1980) Continuous or nocturnal oxygen therapy in hypoxemic chronic obstructive lung disease. Ann Intern Med 93:391–398. https://doi.org/10.7326/0003-4819-93-3-391
Stuart-Harris C, Bishop JM, Clark TJH et al (1981) Long term domiciliary oxygen therapy in chronic hypoxic cor pulmonale complicating chronic bronchitis and emphysema. Lancet 317:681–686. https://doi.org/10.1016/S0140-6736(81)91970-X
Simpson LL, Busch SA, Oliver SJ et al (2019) Baroreflex control of sympathetic vasomotor activity and resting arterial pressure at high altitude: insight from Lowlanders and Sherpa. J Physiol 597:2379–2390. https://doi.org/10.1113/JP277663
Querido JS, Kennedy PM, Sheel AW (2010) Hyperoxia attenuates muscle sympathetic nerve activity following isocapnic hypoxia in humans. J Appl Physiol 108:906–912. https://doi.org/10.1152/japplphysiol.01228.2009
Hansen J, Sander M (2003) Sympathetic neural overactivity in healthy humans after prolonged exposure to hypobaric hypoxia. J Physiol 546:921–929. https://doi.org/10.1113/jphysiol.2002.031765
Duffin J (1990) The chemoreflex control of breathing and its measurement. Can J Anaesth 37:933–942. https://doi.org/10.1007/BF03006641
Lazović B, Zlatković ŠM, Durmić T et al (2016) The regulation role of carotid body peripheral chemoreceptors in physiological and pathophysiological conditions. Med Pregl 69:385–390. https://doi.org/10.2298/MPNS1612385L
Niewinski P, Janczak D, Rucinski A et al (2017) Carotid body resection for sympathetic modulation in systolic heart failure: results from first-in-man study. Eur J Heart Fail 19:391–400. https://doi.org/10.1002/ejhf.641
Narkiewicz K, Ratcliffe LEK, Hart EC et al (2016) Unilateral carotid body resection in resistant hypertension: a safety and feasibility trial. JACC Basic Transl Sci 1:313–324. https://doi.org/10.1016/j.jacbts.2016.06.004
Tymko MM, Young D, Vergel D et al (2023) The effect of hypoxemia on muscle sympathetic nerve activity and cardiovascular function—a systematic review and meta-analysis. Am J Physiol Regul Integr Comp Physiol. https://doi.org/10.1152/ajpregu.00021.2023
Steinback CD, Salzer D, Medeiros PJ et al (2009) Hypercapnic vs. hypoxic control of cardiovascular, cardiovagal, and sympathetic function. Am J Physiol Regul Integr Comp Physiol 296:R402–R410. https://doi.org/10.1152/ajpregu.90772.2008
Ott EP, Jacob DW, Baker SE et al (2020) Sympathetic neural recruitment strategies following acute intermittent hypoxia in humans. Am J Physiol Regul Integr Comp Physiol 318:R961–R971. https://doi.org/10.1152/ajpregu.00004.2020
Xie A, Skatrud JB, Puleo DS, Morgan BJ (2001) Exposure to hypoxia produces long-lasting sympathetic activation in humans. J Appl Physiol 91:1555–1562. https://doi.org/10.1152/jappl.2001.91.4.1555
Houssière A, Najem B, Cuylits N et al (2006) Hyperoxia enhances metaboreflex sensitivity during static exercise in humans. Am J Physiol Heart Circ Physiol 291:H210–H215. https://doi.org/10.1152/ajpheart.01168.2005
Seals DR, Johnson DG, Fregosi RF (1991) Hyperoxia lowers sympathetic activity at rest but not during exercise in humans. Am J Physiol 260:R873–R878. https://doi.org/10.1152/ajpregu.1991.260.5.R873
Moher D, Liberati A, Tetzlaff J et al (2009) Preferred Reporting Items for Systematic Reviews and Meta-Analyses: the PRISMA statement. Ann Inter Med 151:4. https://www.acpjournals.org/doi/full/10.7326/0003-4819-151-4-200908180-00135. Accessed 2 Mar 2023
Cramond F, O’Mara-Eves A, Doran-Constant L et al (2019) The development and evaluation of an online application to assist in the extraction of data from graphs for use in systematic reviews. Wellcome Open Res 3:157. https://doi.org/10.12688/wellcomeopenres.14738.3
Drevon D, Fursa SR, Malcolm AL (2017) Intercoder reliability and validity of webplotdigitizer in extracting graphed data. Behav Modif 41:323–339. https://doi.org/10.1177/0145445516673998
Moola S, Munn Z, Tufanaru C et al (2020) Chapter 7: systematic reviews of etiology and risk. In: Aromataris E, Munn Z (eds) JBI manual for evidence synthesis. JBI, Cham
Higgins JPT, Thomas J, Chandler J et al (2019) Cochrane handbook for systematic reviews of interventions. Wiley, Hoboken
Ciarka A, Najem B, Cuylits N et al (2005) Effects of peripheral chemoreceptors deactivation on sympathetic activity in heart transplant recipients. Hypertension 45:894–900. https://doi.org/10.1161/01.HYP.0000161875.32767.ac
Sinski M, Lewandowski J, Przybylski J et al (2012) Tonic activity of carotid body chemoreceptors contributes to the increased sympathetic drive in essential hypertension. Hypertens Res 35:487–491. https://doi.org/10.1038/hr.2011.209
Narkiewicz K, van de Borne PJH, Montano N et al (1998) Contribution of tonic chemoreflex activation to sympathetic activity and blood pressure in patients with obstructive sleep apnea. Circulation 97:943–945. https://doi.org/10.1161/01.CIR.97.10.943
Hering D, Zdrojewski Z, Król E et al (2007) Tonic chemoreflex activation contributes to the elevated muscle sympathetic nerve activity in patients with chronic renal failure. J Hypertens 25:157–161. https://doi.org/10.1097/HJH.0b013e3280102d92
Andreas S, Bingeli C, Mohacsi P et al (2003) Nasal oxygen and muscle sympathetic nerve activity in heart failure. Chest 123:366–371. https://doi.org/10.1378/chest.123.2.366
Binggeli C, Sudano I, Corti R et al (2010) Spontanous periodic breathing is associated with sympathetic hyperreactivity and baroreceptor dysfunction in hypertension. J Hypertens 28:985. https://doi.org/10.1097/HJH.0b013e3283370e3d
Ciarka A, Vachièry J-L, Houssière A et al (2007) Atrial septostomy decreases sympathetic overactivity in pulmonary arterial hypertension. Chest 131:1831–1837. https://doi.org/10.1378/chest.06-2903
Davy KP, Jones PP, Seals DR (1997) Influence of age on the sympathetic neural adjustments to alterations in systemic oxygen levels in humans. Am J Physiol 273:R690–R695. https://doi.org/10.1152/ajpregu.1997.273.2.R690
Despas F, Detis N, Dumonteil N et al (2009) Excessive sympathetic activation in heart failure with chronic renal failure: role of chemoreflex activation. J Hypertens 27:1849–1854. https://doi.org/10.1097/HJH.0b013e32832e8d0f
Despas F, Lambert E, Vaccaro A et al (2012) Peripheral chemoreflex activation contributes to sympathetic baroreflex impairment in chronic heart failure. J Hypertens 30:753–760. https://doi.org/10.1097/HJH.0b013e328350136c
Engelstein ED, Lerman BB, Somers VK, Rea RF (1994) Role of arterial chemoreceptors in mediating the effects of endogenous adenosine on sympathetic nerve activity. Circulation 90:2919–2926. https://doi.org/10.1161/01.CIR.90.6.2919
Franchitto N, Despas F, Labrunée M et al (2010) Tonic chemoreflex activation contributes to increased sympathetic nerve activity in heart failure-related anemia. Hypertension 55:1012–1017. https://doi.org/10.1161/HYPERTENSIONAHA.109.146779
Haque WA, Boehmer J, Clemson BS et al (1996) Hemodynamic effects of supplemental oxygen administration in congestive heart failure. J Am Coll Cardiol 27:353–357. https://doi.org/10.1016/0735-1097(95)00474-2
Hardy JC, Gray K, Whisler S, Leuenberger U (1994) Sympathetic and blood pressure responses to voluntary apnea are augmented by hypoxemia. J Appl Physiol 77:2360–2365. https://doi.org/10.1152/jappl.1994.77.5.2360
Heindl S, Lehnert M, Criée C-P et al (2001) Marked sympathetic activation in patients with chronic respiratory failure. Am J Respir Crit Care Med 164:597–601. https://doi.org/10.1164/ajrccm.164.4.2007085
Heusser K, Thöne A, Lipp A et al (2020) Efficacy of electrical baroreflex activation is independent of peripheral chemoreceptor modulation. Hypertension 75:257–264. https://doi.org/10.1161/HYPERTENSIONAHA.119.13925
Jendzjowsky NG, Steinback CD, Herman RJ et al (2019) Functional-optical coherence tomography: a non-invasive approach to assess the sympathetic nervous system and intrinsic vascular regulation. Front Physiol 10:1146
Jones PP, Davy S (1999) Influence of gender on the sympathetic neural adjustments to alterations in systemic oxygen levels in humans. Clin Physiol 19:153–160. https://doi.org/10.1046/j.1365-2281.1999.00158.x
Leuenberger U, Jacob E, Sweer L et al (1995) Surges of muscle sympathetic nerve activity during obstructive apnea are linked to hypoxemia. J Appl Physiol 79:581–588. https://doi.org/10.1152/jappl.1995.79.2.581
Leuenberger UA, Hardy JC, Herr MD et al (2001) Hypoxia augments apnea-induced peripheral vasoconstriction in humans. J Appl Physiol 90:1516–1522. https://doi.org/10.1152/jappl.2001.90.4.1516
Leuenberger UA, Hogeman CS, Quraishi S et al (2007) Short-term intermittent hypoxia enhances sympathetic responses to continuous hypoxia in humans. J Appl Physiol 103:835–842. https://doi.org/10.1152/japplphysiol.00036.2007
Limberg JK, Johnson BD, Mozer MT et al (2020) Role of the carotid chemoreceptors in insulin-mediated sympathoexcitation in humans. Am J Physiol Regul Integr Comp Physiol 318:R173–R181. https://doi.org/10.1152/ajpregu.00257.2019
Morgan BJ, Denahan T, Ebert TJ (1993) Neurocirculatory consequences of negative intrathoracic pressure vs. asphyxia during voluntary apnea. J Appl Physiol 74:2969–2975. https://doi.org/10.1152/jappl.1993.74.6.2969
Muller MD, Drew RC, Cui J et al (2013) Effect of oxidative stress on sympathetic and renal vascular responses to ischemic exercise. Physiol Rep. https://doi.org/10.1002/phy2.47
Notarius CF, Badrov MB, Tobushi T et al (2023) Cardiovascular reflex contributions to sympathetic inhibition during low intensity dynamic leg exercise in healthy middle-age. Physiol Rep 11:e15821. https://doi.org/10.14814/phy2.15821
Ott EP, Baker SE, Holbein WW et al (2019) Effect of varying chemoreflex stress on sympathetic neural recruitment strategies during apnea. J Neurophysiol 122:1386–1396. https://doi.org/10.1152/jn.00319.2019
Phillips DB, Steinback CD, Collins SÉ et al (2018) The carotid chemoreceptor contributes to the elevated arterial stiffness and vasoconstrictor outflow in chronic obstructive pulmonary disease. J Physiol 596:3233–3244. https://doi.org/10.1113/JP275762
Prasad B, Morgan BJ, Gupta A et al (2020) The need for specificity in quantifying neurocirculatory vs. respiratory effects of eucapnic hypoxia and transient hyperoxia. J Physiol 598:4803–4819. https://doi.org/10.1113/JP280515
Reed EL, Worley ML, Sackett J et al (2020) Muscle sympathetic nerve activity during thermoneutral head-out water immersion with and without hyperoxia. FASEB J 34:1–1. https://doi.org/10.1096/fasebj.2020.34.s1.06426
Rongen GA, Senn BL, Ando S et al (1997) Comparison of hemodynamic and sympathoneural responses to adenosine and lower body negative pressure in man. Can J Physiol Pharmacol 75:128–134
Sayegh ALC, Fan J-L, Vianna LC et al (2022) Sex differences in the sympathetic neurocirculatory responses to chemoreflex activation. J Physiol 600:2669–2689. https://doi.org/10.1113/JP282327
Siddiqi L, Oey PL, Blankestijn PJ (2010) Aliskiren reduces sympathetic nerve activity in chronic kidney disease patients: PP.24.467. J Hypertens 28:e386. https://doi.org/10.1097/01.hjh.0000379393.42415.72
Smorschok MP, Sobierajski FM, Purdy GM et al (2019) Peripheral chemoreceptor deactivation attenuates the sympathetic response to glucose ingestion. Appl Physiol Nutr Metab 44:389–396. https://doi.org/10.1139/apnm-2018-0062
Steele AR, Berthelsen LF, Fraser GM et al (2021) Blunted sympathetic neurovascular transduction is associated to the severity of obstructive sleep apnea. Clin Auton Res 31:443–451. https://doi.org/10.1007/s10286-021-00784-8
Stickland MK, Morgan BJ, Dempsey JA (2008) Carotid chemoreceptor modulation of sympathetic vasoconstrictor outflow during exercise in healthy humans: carotid chemoreceptor and sympathetic activation during exercise. J Physiol 586:1743–1754. https://doi.org/10.1113/jphysiol.2007.147421
Trzebski A, Smith ML, Beightol LA et al (1995) Modulation of human sympathetic periodicity by mild, brief hypoxia and hypercapnia. J Physiol Pharmacol 46:17–35
van de Borne P, Oren R, Anderson EA et al (1996) Tonic chemoreflex activation does not contribute to elevated muscle sympathetic nerve activity in heart failure. Circulation 94:1325–1328. https://doi.org/10.1161/01.CIR.94.6.1325
Velez-Roa S, Ciarka A, Najem B et al (2004) Increased sympathetic nerve activity in pulmonary artery hypertension. Circulation 110:1308–1312. https://doi.org/10.1161/01.CIR.0000140724.90898.D3
Yamauchi K, Tsutsui Y, Endo Y et al (2002) Sympathetic nervous and hemodynamic responses to lower body negative pressure in hyperbaria in men. Am J Physiol-Regul Integr Comp Physiol 282:R38–R45. https://doi.org/10.1152/ajpregu.2002.282.1.R38
Saboune J, Schwende B, Usselman CW, Davenport MH, Steinback CD (2023) Effect of sex on sympatho-inhibitors and non-inhibitors during acute hyperoxia. J Physiol (in press)
Franchitto N, Despas F, Labrunee M et al (2013) Cardiorenal anemia syndrome in chronic heart failure contributes to increased sympathetic nerve activity. Int J Cardiol 168:2352–2357. https://doi.org/10.1016/j.ijcard.2013.01.023
Reyes LM, Usselman CW, Khurana R et al (1985) (2021) Preeclampsia is not associated with elevated muscle sympathetic reactivity. J Appl Physiol 130:139–148. https://doi.org/10.1152/japplphysiol.00646.2020
Reyes LM, Khurana R, Usselman CW et al (2020) Sympathetic nervous system activity and reactivity in women with gestational diabetes mellitus. Physiol Rep 8:e14504. https://doi.org/10.14814/phy2.14504
Simmons GH, Manson JM, Halliwill JR (2007) Mild central chemoreflex activation does not alter arterial baroreflex function in healthy humans: central chemoreflex does not alter arterial baroreflex function. J Physiol 583:1155–1163. https://doi.org/10.1113/jphysiol.2007.137216
Notarius CF, Keir DA, Badrov MB et al (2020) Contrasting reflex neural modulation of muscle sympathetic nerve activity at rest and during one-leg dynamic exercise in subjects with and without heart failure. FASEB J 34:1–1. https://doi.org/10.1096/fasebj.2020.34.s1.06063
Andreas S, Haarmann H, Klarner S et al (2014) Increased sympathetic nerve activity in COPD is associated with morbidity and mortality. Lung 192:235–241. https://doi.org/10.1007/s00408-013-9544-7
Barretto ACP, Santos AC, Munhoz R et al (2009) Increased muscle sympathetic nerve activity predicts mortality in heart failure patients. Int J Cardiol 135:302–307. https://doi.org/10.1016/j.ijcard.2008.03.056
Ciarka A, Doan V, Velez-Roa S et al (2010) Prognostic significance of sympathetic nervous system activation in pulmonary arterial hypertension. Am J Respir Crit Care Med 181:1269–1275. https://doi.org/10.1164/rccm.200912-1856OC
Dejours P (1962) Chemoreflexes in breathing. Physiol Rev 42:335–358. https://doi.org/10.1152/physrev.1962.42.3.335
Grassi G, Pisano A, Bolignano D et al (2018) Sympathetic nerve traffic activation in essential hypertension and its correlates. Hypertension 72:483–491. https://doi.org/10.1161/HYPERTENSIONAHA.118.11038
Badrov MB, Keir DA, Tomlinson G et al (2023) Normal and excessive muscle sympathetic nerve activity in heart failure: implications for future trials of therapeutic autonomic modulation. Eur J Heart Fail 25:201–210. https://doi.org/10.1002/ejhf.2749
Smit B, Smulders YM, van der Wouden JC et al (2018) Hemodynamic effects of acute hyperoxia: systematic review and meta-analysis. Crit Care 22:45. https://doi.org/10.1186/s13054-018-1968-2
Mattos JD, Campos MO, Rocha MP et al (2019) Human brain blood flow and metabolism during isocapnic hyperoxia: the role of reactive oxygen species. J Physiol 597:741–755. https://doi.org/10.1113/JP277122
Fernandes IA, Mattos JD, Campos MO et al (2021) Reactive oxygen species play a modulatory role in the hyperventilatory response to poikilocapnic hyperoxia in humans. J Physiol 599:3993–4007. https://doi.org/10.1113/JP281635
Teboul J-L, Scheeren T (2017) Understanding the haldane effect. Intensive Care Med 43:91–93. https://doi.org/10.1007/s00134-016-4261-3
Dean JB, Mulkey DK, Henderson RA et al (2004) Hyperoxia, reactive oxygen species, and hyperventilation: oxygen sensitivity of brain stem neurons. J Appl Physiol 96:784–791. https://doi.org/10.1152/japplphysiol.00892.2003
Yamada Y, Miyajima E, Tochikubo O et al (1989) Age-related changes in muscle sympathetic nerve activity in essential hypertension. Hypertension 13:870–877. https://doi.org/10.1161/01.HYP.13.6.870
Abdala AP, McBryde FD, Marina N et al (2012) Hypertension is critically dependent on the carotid body input in the spontaneously hypertensive rat. J Physiol 590:4269–4277. https://doi.org/10.1113/jphysiol.2012.237800
Atanasova DY, Dandov AD, Lazarov NE (2023) Neurochemical plasticity of the carotid body in hypertension. Anat Rec 306:2366–2377. https://doi.org/10.1002/ar.24997
Paton JFR, Sobotka PA, Fudim M, et al (2013) The carotid body as a therapeutic target for the treatment of sympathetically mediated diseases. Hypertension 61(1):5-13. https://www.ahajournals.org/doi/epub/10.1161/HYPERTENSIONAHA.111.00064
Edwards BA, Sands SA, Owens RL et al (2014) Effects of hyperoxia and hypoxia on the physiological traits responsible for obstructive sleep apnoea. J Physiol 592:4523–4535. https://doi.org/10.1113/jphysiol.2014.277210
Niewinski P, Engelman ZJ, Fudim M et al (2013) Clinical predictors and hemodynamic consequences of elevated peripheral chemosensitivity in optimally treated men with chronic systolic heart failure. J Card Fail 19:408–415. https://doi.org/10.1016/j.cardfail.2013.03.013
Ponikowski P, Chua TP, Anker SD et al (2001) Peripheral chemoreceptor hypersensitivity: an ominous sign in patients with chronic heart failure. Circulation 104:544–549. https://doi.org/10.1161/hc3101.093699
Tubek S, Niewinski P, Paleczny B et al (2021) Acute hyperoxia reveals tonic influence of peripheral chemoreceptors on systemic vascular resistance in heart failure patients. Sci Rep 11:20823. https://doi.org/10.1038/s41598-021-99159-2
Hoeper MM, Benza RL, Corris P et al (2019) Intensive care, right ventricular support and lung transplantation in patients with pulmonary hypertension. Eur Respir J. https://doi.org/10.1183/13993003.01906-2018
Olsson KM, Frank A, Fuge J et al (2015) Acute hemodynamic effects of adaptive servoventilation in patients with pre-capillary and post-capillary pulmonary hypertension. Respir Res 16:137. https://doi.org/10.1186/s12931-015-0298-z
Acknowledgements
We would like to thank the authors who clarified aspects of their published data that were included in our meta-analysis.
Funding
This study was funded by a National Sciences and Engineering Research Council Discovery Grant (Craig Steinback: RGPIN–2020–05385). Margie Davenport is supported by the Christenson Professorship in Healthy Active Living.
Author information
Authors and Affiliations
Contributions
Desmond Young, Craig Steinback, and Margie Davenport conceptualized the project. Allison Sivak performed the literature search. Desmond Young, Paris Jones, Brittany Matenchuk, and Craig Steinback performed data analysis. Desmond Young drafted the manuscript, and all authors critically revised the work.
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethical approval
The manuscript does not contain clinical studies or patient data.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Young, D.A., Jones, P.A.T., Matenchuk, B.A. et al. The effect of hyperoxia on muscle sympathetic nerve activity: a systematic review and meta-analysis. Clin Auton Res 34, 233–252 (2024). https://doi.org/10.1007/s10286-024-01033-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10286-024-01033-4