Abstract
Background and aims
Specific mechanisms of lymph node (LN) metastasis in early-stage gastric cancer (GC) have not been elucidated. The role of anemia, a vital clinical feature of GC, in LN metastasis is also unclear. Since the number of erythroid progenitor cells (EPCs) is increased in chronic anemia, we investigated its association with LN metastasis in GC.
Methods
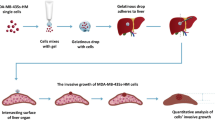
Flow cytometry and immunofluorescence analyses were performed to sort and study EPCs from the circulation and tumors of patients with stage I–III GC. The effect of these EPCs on the activation of T and B cells and on the functions of lymphatic endothelial cells (LECs) was determined, and their ability to promote LN metastasis was evaluated using a footpad‐popliteal LN metastasis model based on two human adenocarcinoma GC cell lines in nude mice. The prognostic value of EPCs was also analyzed.
Results
The proportion of CD45− EPCs was higher in the mononuclear cells in the circulation, tumors, and LNs of GC patients with LN metastasis (N+) than in those of GC patients without LN metastasis (N0). In N+ patients, CD45− EPCs were more abundant in metastatic LNs than in non-metastatic LNs. Lymphatic vessel endothelial hyaluronan receptor 1 immunoreactivity in tumors revealed that CD45− EPCs were positively associated with nodal stages and lymph vessel density. Furthermore, CD45− EPCs increased LEC proliferation and migration through their S100A8/A9 heterodimer-induced hybrid epithelial/mesenchymal (E/M) state; however, they did not influence the invasion and tubulogenesis of LECs or T and B cell proliferation. CD45− EPCs promoted LN metastasis in vivo; the S100A8/A9 heterodimer mimicked this phenomenon. Finally, CD45− EPCs predicted the overall and disease-free survival of stage I–III GC patients after radical resection.
Conclusions
The CD45− EPCs accumulated in GC tissues and metastatic LNs and promoted LN metastasis via the S100A8/9-induced hybrid E/M state of LECs, which was the specific mechanism of LN metastasis in the early stages of GC.







Similar content being viewed by others
Data availability
Data are available in a public, open-access repository. All data relevant to the study are included in the article or uploaded as supplementary information. Data are available in public, open-access repositories, directly included in the article, uploaded as supplementary information from first or last authors.
References
Kinami S, Nakamura N, Tomita Y, Miyata T, Fujita H, Ueda N, Kosaka T. Precision surgical approach with lymph-node dissection in early gastric cancer. World J Gastroenterol. 2019;25:1640–52.
Chen R, He Q, Cui J, Bian S, Chen L. Lymph node metastasis in early gastric cancer. Chin Med J (Engl). 2014;127:560–7.
Jana S, Muscarella RA Jr, Jones D. The multifaceted effects of breast cancer on tumor-draining lymph nodes. Am J Pathol. 2021;191:1353–63.
Rezzola S, Sigmund EC, Halin C, Ronca R. The lymphatic vasculature: an active and dynamic player in cancer progression. Med Res Rev. 2022;42:576–614.
Tammela T, Alitalo K. Lymphangiogenesis: molecular mechanisms and future promise. Cell. 2010;140:460–76.
Jalkanen S, Salmi M. Lymphatic endothelial cells of the lymph node. Nat Rev Immunol. 2020;20:566–78.
Dellinger MT, Witte MH. Lymphangiogenesis, lymphatic systemomics, and cancer: context, advances and unanswered questions. Clin Exp Metastasis. 2018;35:419–24.
Bieniasz-Krzywiec P, Martin-Perez R, Ehling M, Garcia-Caballero M, Pinioti S, Pretto S, Kroes R, et al. Podoplanin-expressing macrophages promote lymphangiogenesis and lymphoinvasion in breast cancer. Cell Metab. 2019;30(917–936): e910.
Tacconi C, Correale C, Gandelli A, Spinelli A, Dejana E, D’Alessio S, Danese S. Vascular endothelial growth factor C disrupts the endothelial lymphatic barrier to promote colorectal cancer invasion. Gastroenterology. 2015;148(1438–1451): e1438.
Weichand B, Popp R, Dziumbla S, Mora J, Strack E, Elwakeel E, Frank AC, et al. S1PR1 on tumor-associated macrophages promotes lymphangiogenesis and metastasis via NLRP3/IL-1beta. J Exp Med. 2017;214:2695–713.
Cadamuro M, Brivio S, Mertens J, Vismara M, Moncsek A, Milani C, Fingas C, et al. Platelet-derived growth factor-D enables liver myofibroblasts to promote tumor lymphangiogenesis in cholangiocarcinoma. J Hepatol. 2019;70:700–9.
Huang XZ, Yang YC, Chen Y, Wu CC, Lin RF, Wang ZN, Zhang X. Preoperative anemia or low hemoglobin predicts poor prognosis in gastric cancer patients: a meta-analysis. Dis Markers. 2019;2019:7606128.
Tang GH, Hart R, Sholzberg M, Brezden-Masley C. Iron deficiency anemia in gastric cancer: a Canadian retrospective review. Eur J Gastroenterol Hepatol. 2018;30:1497–501.
Elahi S, Ertelt JM, Kinder JM, Jiang TT, Zhang X, Xin L, Chaturvedi V, et al. Immunosuppressive CD71+ erythroid cells compromise neonatal host defence against infection. Nature. 2013;504:158–62.
Zhao L, He R, Long H, Guo B, Jia Q, Qin D, Liu SQ, et al. Late-stage tumors induce anemia and immunosuppressive extramedullary erythroid progenitor cells. Nat Med. 2018;24:1536–44.
Han Y, Liu Q, Hou J, Gu Y, Zhang Y, Chen Z, Fan J, et al. Tumor-induced generation of splenic erythroblast-like Ter-cells promotes tumor progression. Cell. 2018;173(634–648): e612.
Chen J, Qiao YD, Li X, Xu JL, Ye QJ, Jiang N, Zhang H, et al. Intratumoral CD45(+)CD71(+) erythroid cells induce immune tolerance and predict tumor recurrence in hepatocellular carcinoma. Cancer Lett. 2021;499:85–98.
Faustino SES, Tjioe KC, Assao A, Pereira MC, Carvalho AL, Kowalski LP, Oliveira DT. Association of lymph vessel density with occult lymph node metastasis and prognosis in oral squamous cell carcinoma. BMC Oral Health. 2021;21:114.
Niemiec JA, Adamczyk A, Ambicka A, Mucha-Malecka A, Wysocki WM, Biesaga B, Ziobro M, et al. Prognostic role of lymphatic vessel density and lymphovascular invasion in chemotherapy-naive and chemotherapy-treated patients with invasive breast cancer. Am J Transl Res. 2017;9:1435–47.
Zhang J, Dominguez-Sola D, Hussein S, Lee JE, Holmes AB, Bansal M, Vlasevska S, et al. Disruption of KMT2D perturbs germinal center B cell development and promotes lymphomagenesis. Nat Med. 2015;21:1190–8.
Nandi P, Girish GV, Majumder M, Xin X, Tutunea-Fatan E, Lala PK. PGE2 promotes breast cancer-associated lymphangiogenesis by activation of EP4 receptor on lymphatic endothelial cells. BMC Cancer. 2017;17:11.
Karnezis T, Farnsworth RH, Harris NC, Williams SP, Caesar C, Byrne DJ, Herle P, et al. CCL27/CCL28-CCR10 chemokine signaling mediates migration of lymphatic endothelial cells. Cancer Res. 2019;79:1558–72.
Liao TT, Yang MH. Hybrid epithelial/mesenchymal state in cancer metastasis: clinical significance and regulatory mechanisms. Cells. 2020;9(3):623.
Kroger C, Afeyan A, Mraz J, Eaton EN, Reinhardt F, Khodor YL, Thiru P, et al. Acquisition of a hybrid E/M state is essential for tumorigenicity of basal breast cancer cells. Proc Natl Acad Sci USA. 2019;116:7353–62.
He P, Qiu K, Jia Y. Modeling of mesenchymal hybrid epithelial state and phenotypic transitions in EMT and MET processes of cancer cells. Sci Rep. 2018;8:14323.
Shabani F, Farasat A, Mahdavi M, Gheibi N. Calprotectin (S100A8/S100A9): a key protein between inflammation and cancer. Inflamm Res. 2018;67:801–12.
Zhong X, Xie F, Chen L, Liu Z, Wang Q. S100A8 and S100A9 promote endothelial cell activation through the RAGEmediated mammalian target of rapamycin complex 2 pathway. Mol Med Rep. 2020;22:5293–303.
Dadashzadeh ER, Bou-Samra P, Huckaby LV, Nebbia G, Handzel RM, Varley PR, Wu S, et al. Leveraging decision curve analysis to improve clinical application of surgical risk calculators. J Surg Res. 2021;261:58–66.
Jiang Y, Tu R, Lu J, Zhang Y, Zhu J, Tang W, Gu M, et al. Proposed modification of the 8th edition of the AJCC staging system for gastric cancer. J Invest Surg. 2020;33:932–8.
Peng J, Liu X, Li C, Gao M, Wang H. Sema4C modulates the migration of primary tumor-associated lymphatic endothelial cells via an ERK-mediated pathway. Exp Ther Med. 2021;22:1102.
Grzywa TM, Justyniarska M, Nowis D, Golab J. Tumor immune evasion induced by dysregulation of erythroid progenitor cells development. Cancers (Basel). 2021;13:870.
Cormier K, Harquail J, Ouellette RJ, Tessier PA, Guerrette R, Robichaud GA. Intracellular expression of inflammatory proteins S100A8 and S100A9 leads to epithelial-mesenchymal transition and attenuated aggressivity of breast cancer cells. Anticancer Agents Med Chem. 2014;14:35–45.
Xu Z, Cheng C, Kong R, Liu Y, Wang S, Ma Y, Xing X. S100A8 and S100A9, both transcriptionally regulated by PU.1, promote epithelial-mesenchymal transformation (EMT) and invasive growth of dermal keratinocytes during scar formation post burn. Aging (Albany NY). 2021;13:15523–37.
Jo SH, Heo WH, Son HY, Quan M, Hong BS, Kim JH, Lee HB, et al. S100A8/A9 mediate the reprograming of normal mammary epithelial cells induced by dynamic cell-cell interactions with adjacent breast cancer cells. Sci Rep. 2021;11:1337.
Souilhol C, Harmsen MC, Evans PC, Krenning G. Endothelial-mesenchymal transition in atherosclerosis. Cardiovasc Res. 2018;114:565–77.
Wang SH, Chang JS, Hsiao JR, Yen YC, Jiang SS, Liu SH, Chen YL, et al. Tumour cell-derived WNT5B modulates in vitro lymphangiogenesis via induction of partial endothelial-mesenchymal transition of lymphatic endothelial cells. Oncogene. 2017;36:1503–15.
Deng JY, Liang H. Clinical significance of lymph node metastasis in gastric cancer. World J Gastroenterol. 2014;20:3967–75.
Li L, Yang F, Wang X, Hu J, Yang L, Tang C, Wu Y, et al. Effect of 15-hydroxyprostaglandin dehydrogenase gene on the proliferation of gastric cancer cell murine forestomach carcinoma. Exp Ther Med. 2014;7:290–4.
Hong S, Bi M, Yu H, Yan Z, Wang H. Radiation therapy enhanced therapeutic efficacy of anti-PD1 against gastric cancer. J Radiat Res. 2020;61:851–9.
Acknowledgements
We are grateful to the central laboratory of the Third Affiliated Hospital of Sun Yat-sen University for providing labs and technical guidance.
Funding
This study was supported by Guangdong Basic and Applied Basic Research Foundation (No. 2021A1515011022, 2023A1515012544, 2022A1515010547 and 2023A1515011803), Tip-top Scientific and Technical Innovative Youth Talents of the Third Affiliated Hospital of Sun Yat-sen University, and National Natural Science Foundation of China (82073397, 81972677, 82103331) and Science Foundation of Guang dong Provincial Bureau of traditional Chinese Medicine (20211090).
Author information
Authors and Affiliations
Contributions
W-J Y, J-N C and W-H Z acquired the animal data. W-J Y, J C, J-Y Z and Y D performed the in vitro cell experiments. W-J Y, Y-J C and J C acquired the RNA seq data. R-H Y, J-N C, J-Y Z and Y D did the pathologic analysis. X L designed the study, analyzed the data, and wrote the manuscript. C-K S supervised the study and revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No conflicts needed to be declared.
Ethics approval and consent to participate
This study of patient samples was approved by the Clinical Ethics Review Board of the Third Affiliated Hospital of Sun Yat-sen University ([2019]02-387-01). A written informed consent was obtained from all the patients at the time of admission. The animal experiments were carried out under the approval of the Institutional Animal Care and Use Committee of the Third Affiliated Hospital of Sun Yat‐sen University ([2020]02-311).
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wen, JY., Li, X., Chen, JN. et al. CD45− erythroid progenitor cells promote lymph node metastasis in gastric cancer by inducing a hybrid epithelial/mesenchymal state in lymphatic endothelial cells. Gastric Cancer 26, 918–933 (2023). https://doi.org/10.1007/s10120-023-01425-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10120-023-01425-x