Abstract
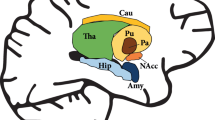
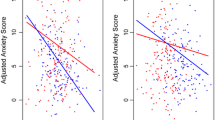
Subcortical brain regions play essential roles in the pathology of social anxiety disorder (SAD). While adolescence is the peak period of SAD, the relationships between altered development of the subcortical regions during this period and SAD are still unclear. This study investigated the age-dependent alterations in structural co-variance among subcortical regions and between subcortical and cortical regions, aiming to reflect aberrant coordination during development in the adolescent with SAD. High-resolution T1-weighted images were obtained from 76 adolescents with SAD and 67 healthy controls (HC), ranging from 11 to 17.9 years. Symptom severity was evaluated with the Social Anxiety Scale for Children (SASC) and the Depression Self Rating Scale for Children (DSRS-C). Structural co-variance and sliding age-window analyses were used to detect age-dependent group differences in inter-regional coordination patterns among subcortical regions and between subcortical and cortical regions. The volume of the striatum significantly correlated with SAD symptom severity. The SAD group exhibited significantly enhanced structural co-variance among key regions of the striatum (putamen and caudate). While the co-variance decreased with age in healthy adolescents, the co-variance in SAD adolescents stayed high, leading to more apparent group differences in middle adolescence. Moreover, the striatum’s mean structural co-variance with cortical regions decreased with age in HC but increased with age in SAD. Adolescents with SAD suffer aberrant developmental coordination among the key regions of the striatum and between the striatum and cortical regions. The degree of incoordination is age-dependent, which may represent a neurodevelopmental trait of SAD.



Similar content being viewed by others
Data Availability
Requests for access to the anonymized data can be sent to the corresponding author and reviewed by the IRB. The code and image-derived statistics are shared at: https://github.com/PHI-group/StableProjects.
References
Mathew SJ, Coplan JD, Gorman JM (2001) Neurobiological mechanisms of social anxiety disorder. Am J Psychiatry 158:1558–1567. https://doi.org/10.1176/appi.ajp.158.10.1558
American Psychiatric Association (2013). Diagnostic and statistical manual of mental disorders (5th ed.). https://doi.org/10.1176/appi.books.9780890425596
Richey JA, Rittenberg A, Hughes L et al (2014) Common and distinct neural features of social and non-social reward processing in autism and social anxiety disorder. Soc Cogn Affect Neurosci 9:367–377. https://doi.org/10.1093/scan/nss146
Todd BK (2007) Social anxiety spectrum and diminished positive experiences: theoretical synthesis and meta-analysis. Clin Psychol Rev. https://doi.org/10.1016/j.cpr.2006.12.003
Beesdo K, Knappe S, Pine DS (2009) Anxiety and anxiety disorders in children and adolescents: developmental issues and implications for DSM-V. Psychiatr Clin North Am 32:483–524. https://doi.org/10.1016/j.psc.2009.06.002
Xie S, Zhang X, Cheng W (2021) Adolescent anxiety disorders and the developing brain: comparing neuroimaging findings in adolescents and adults. Gen Psychiatry. https://doi.org/10.1136/gpsych-2020-100411
Natu VS, Gomez J, Barnett M et al (2019) Apparent thinning of human visual cortex during childhood is associated with myelination. Proc Natl Acad Sci USA 116:20750–20759. https://doi.org/10.1073/pnas.1904931116
Heller AS, Cohen AO, Dreyfuss MFW et al (2016) Changes in cortico-subcortical and subcortico-subcortical connectivity impact cognitive control to emotional cues across development. Soc Cogn Affect Neurosci 11:1910–1918. https://doi.org/10.1093/scan/nsw097
Tottenham N, Galván A (2016) Stress and the adolescent brain: amygdala-prefrontal cortex circuitry and ventral striatum as developmental targets. Neurosci Biobehav Rev 70:217–227. https://doi.org/10.1016/j.neubiorev.2016.07.030
Spear LP (2000) The adolescent brain and age-related behavioral manifestations. Neurosci Biobehav Rev 24:417–463. https://doi.org/10.1016/S0149-7634(00)00014-2
Caouette JD, Guyer AE (2014) Gaining insight into adolescent vulnerability for social anxiety from developmental cognitive neuroscience. Dev Cogn Neurosci 8:65–76. https://doi.org/10.1016/j.dcn.2013.10.003
Etkin A, Wager TD (2007) Functional neuroimaging of anxiety: a meta-analysis of emotional processing in PTSD, social anxiety disorder, and specific phobia. Am J Psychiatry 164:1476–1488. https://doi.org/10.1176/appi.ajp.2007.07030504
Phelps EA, LeDoux JE (2005) Contributions of the amygdala to emotion processing: from animal models to human behavior. Neuron 48:175–187. https://doi.org/10.1016/j.neuron.2005.09.025
Schultz J, Willems T, Gädeke M et al (2019) A human subcortical network underlying social avoidance revealed by risky economic choices. Elife 8:e45249. https://doi.org/10.7554/eLife.45249
Miskovic V, Schmidt LA (2012) Social fearfulness in the human brain. Neurosci Biobehav Rev 36:459–478. https://doi.org/10.1016/j.neubiorev.2011.08.002
Shin LM, Liberzon I (2010) The neurocircuitry of fear, stress, and anxiety disorders. Neuropsychopharmacology 35:169–191. https://doi.org/10.1038/npp.2009.83
Tovote P, Fadok JP, Lüthi A (2015) Neuronal circuits for fear and anxiety. Nat Rev Neurosci 16:317–331. https://doi.org/10.1038/nrn3945
de Carvalho MR, Rozenthal M, Nardi AE (2010) The fear circuitry in panic disorder and its modulation by cognitive-behaviour therapy interventions. World J Biol Psychiatry 11:188–198. https://doi.org/10.1080/15622970903178176
Freitas-Ferrari MC, Hallak JEC, Trzesniak C et al (2010) Neuroimaging in social anxiety disorder: a systematic review of the literature. Prog Neuropsychopharmacol Biol Psychiatry 34:565–580. https://doi.org/10.1016/j.pnpbp.2010.02.028
Brühl AB, Delsignore A, Komossa K et al (2014) Neuroimaging in social anxiety disorder—a meta-analytic review resulting in a new neurofunctional model. Neurosci Biobehav Rev 47:260–280. https://doi.org/10.1016/j.neubiorev.2014.08.003
Marchand WR (2010) Cortico-basal ganglia circuitry: a review of key research and implications for functional connectivity studies of mood and anxiety disorders. Brain Struct Funct 215:73–96. https://doi.org/10.1007/s00429-010-0280-y
Ruff CC, Fehr E (2014) The neurobiology of rewards and values in social decision making. Nat Rev Neurosci 15:549–562. https://doi.org/10.1038/nrn3776
Becker MPI, Simon D, Miltner WHR et al (2017) Altered activation of the ventral striatum under performance-related observation in social anxiety disorder. Psychol Med 47:2502–2512. https://doi.org/10.1017/S0033291717001076
Crane NA, Chang F, Kinney KL et al (2021) Individual differences in striatal and amygdala response to emotional faces are related to symptom severity in social anxiety disorder. NeuroImage Clin 30
Taber-Thomas BC, Morales S, Hillary FG et al (2016) Altered topography of intrinsic functional connectivity in childhood risk for social anxiety. Depress Anxiety 33:995–1004. https://doi.org/10.1002/da.22508
Guyer AE, Choate VR, Detloff A et al (2012) Striatal functional alteration during incentive anticipation in pediatric anxiety disorders. Am J Psychiatry 169:205–212. https://doi.org/10.1176/appi.ajp.2011.11010006
Carlton CN, Sullivan-Toole H, Ghane M et al (2020) Reward circuitry and motivational deficits in social anxiety disorder: what can be learned from mouse models? Front Neurosci 14:154. https://doi.org/10.3389/fnins.2020.00154
Zhu H, Qiu C, Meng Y et al (2017) Altered topological properties of brain networks in social anxiety disorder: a resting-state functional MRI study. Sci Rep 7:43089. https://doi.org/10.1038/srep43089
Schneier FR, Abi-Dargham A, Martinez D et al (2009) Dopamine transporters, D2 receptors, and dopamine release in generalized social anxiety disorder. Depress Anxiety 26:411–418. https://doi.org/10.1002/da.20543
van der Wee NJ, van Veen JF, Stevens H et al (2008) Increased serotonin and dopamine transporter binding in psychotropic medication-naive patients with generalized social anxiety disorder shown by 123I-beta-(4-iodophenyl)-tropane SPECT. J Nucl Med 49:757–763. https://doi.org/10.2967/jnumed.107.045518
Bas-Hoogendam JM, van Steenbergen H, Tissier RLM et al (2018) Subcortical brain volumes, cortical thickness and cortical surface area in families genetically enriched for social anxiety disorder—a multiplex multigenerational neuroimaging study. EBioMedicine 36:410–428. https://doi.org/10.1016/j.ebiom.2018.08.048
Monique E, Daniel SP, Michael H (2006) Triadic model of the neurobiology of motivated behavior in adolescence. Psychol Med 36:299–312. https://doi.org/10.1017/S0033291705005891
Ernst M (2014) The triadic model perspective for the study of adolescent motivated behavior. Brain Cogn 89:104–111. https://doi.org/10.1016/j.bandc.2014.01.006
Ernst M, Fudge JL (2009) A developmental neurobiological model of motivated behavior: anatomy, connectivity and ontogeny of the triadic nodes. Neurosci Biobehav Rev 33:367–382. https://doi.org/10.1016/j.neubiorev.2008.10.009
Burgoyne RD, Graham ME, Cambray-Deakin M (1993) Neurotrophic effects of NMDA receptor activation on developing cerebellar granule cells. J Neurocytol 22:689–695. https://doi.org/10.1007/BF01181314
Bullmore ET, Frangou S, Murray RM (1997) The dysplastic net hypothesis: an integration of developmental and dysconnectivity theories of schizophrenia. Schizophr Res 28:143–156. https://doi.org/10.1016/s0920-9964(97)00114-x
Mechelli A, Friston KJ, Frackowiak RS et al (2005) Structural covariance in the human cortex. J Neurosci 25:8303–8310. https://doi.org/10.1523/JNEUROSCI.0357-05.2005
Alexander-Bloch A, Giedd JN, Bullmore E (2013) Imaging structural co-variance between human brain regions. Nat Rev Neurosci 14:322–336. https://doi.org/10.1038/nrn3465
Liu Z, Hu Y, Zhang Y et al (2021) Altered gray matter volume and structural co-variance in adolescents with social anxiety disorder: evidence for a delayed and unsynchronized development of the fronto-limbic system. Psychol Med 51:1742–1751. https://doi.org/10.1017/S0033291720000495
Alexander-Bloch A, Raznahan A, Bullmore E et al (2013) The convergence of maturational change and structural covariance in human cortical networks. J Neurosci 33:2889–2899. https://doi.org/10.1523/JNEUROSCI.3554-12.2013
Duan X, Wang R, Xiao J et al (2020) Subcortical structural covariance in young children with autism spectrum disorder. Prog Neuropsychopharmacol Biol Psychiatry 99:109874. https://doi.org/10.1016/j.pnpbp.2020.109874
Wannan CMJ, Cropley VL, Chakravarty MM et al (2019) Evidence for network-based cortical thickness reductions in Schizophrenia. Am J Psychiatry 176:552–563. https://doi.org/10.1176/appi.ajp.2019.18040380
Liu Y, Liu J, Wang Y (2011) Reliability and validity of Chinese version of the Mini International Neuropsychiatric Interview for Children and Adolescents (child version). Chin Ment Health J 25:8–13
Yu L (2010) Reliability and validity of Chinese version of the Mini International Neuropsychiatric Interview for Children and Adolescents (Parent Version)
Dale AM, Fischl B, Sereno MI (1999) Cortical surface-based analysis: I. Segmentation and surface reconstruction. Neuroimage 9:179–194. https://doi.org/10.1006/nimg.1998.0395
Fischl B, Sereno MI, Dale AM (1999) Cortical surface-based analysis. II: inflation, flattening, and a surface-based coordinate system. Neuroimage 9:195–207. https://doi.org/10.1006/nimg.1998.0396
Desikan RS, Ségonne F, Fischl B et al (2006) An automated labeling system for subdividing the human cerebral cortex on MRI scans into gyral based regions of interest. Neuroimage 31:968–980. https://doi.org/10.1016/j.neuroimage.2006.01.021
Fischl B, Salat DH, Busa E et al (2002) Whole brain segmentation: automated labeling of neuroanatomical structures in the human brain. Neuron 33:341–355. https://doi.org/10.1016/S0896-6273(02)00569-X
Gaser C, Dahnke R, Thompson PM et al (2022) CAT—a computational anatomy toolbox for the analysis of structural MRI data. bioRxiv 2022.06.11.495736. https://doi.org/10.1101/2022.06.11.495736
La Greca AM, Stone WL (1993) Social anxiety scale for children-revised: factor structure and concurrent validity. J Clin Child Psychol 22:17–27. https://doi.org/10.1207/s15374424jccp2201_2
Birleson P, Hudson I, Buchanan DG et al (1987) Clinical evaluation of a self-rating scale for depressive disorder in childhood (depression Self-Rating Scale). J Child Psychol Psychiatry 28:43–60. https://doi.org/10.1111/j.1469-7610.1987.tb00651.x
Hardin AP, Hackell JM (2017) Age limit of pediatrics. Pediatrics 140:e20172151. https://doi.org/10.1542/peds.2017-2151
Vijayakumar N, Ball G, Seal ML et al (2021) The development of structural covariance networks during the transition from childhood to adolescence. Sci Rep 11:9451. https://doi.org/10.1038/s41598-021-88918-w
Váša F, Seidlitz J, Romero-Garcia R et al (2018) Adolescent tuning of association cortex in human structural brain networks. Cereb Cortex 28:281–294. https://doi.org/10.1093/cercor/bhx249
Oldham S, Murawski C, Fornito A et al (2018) The anticipation and outcome phases of reward and loss processing: a neuroimaging meta-analysis of the monetary incentive delay task. Hum Brain Mapp 39:3398–3418. https://doi.org/10.1002/hbm.24184
Raznahan A, Shaw PW, Lerch JP et al (2014) Longitudinal four-dimensional mapping of subcortical anatomy in human development. Proc Natl Acad Sci 111:1592–1597. https://doi.org/10.1073/pnas.1316911111
Telzer EH (2016) Dopaminergic reward sensitivity can promote adolescent health: a new perspective on the mechanism of ventral striatum activation. Dev Cogn Neurosci 17:57–67. https://doi.org/10.1016/j.dcn.2015.10.010
Larsen B, Luna B (2015) In vivo evidence of neurophysiological maturation of the human adolescent striatum. Dev Cogn Neurosci 12:74–85. https://doi.org/10.1016/j.dcn.2014.12.003
Bhanji JP, Delgado MR (2014) The social brain and reward: social information processing in the human striatum. Wiley Interdiscip Rev Cogn Sci 5:61–73. https://doi.org/10.1002/wcs.1266
Hanson JL, Hariri AR, Williamson DE (2015) Blunted ventral striatum development in adolescence reflects emotional neglect and predicts depressive symptoms. Biol Psychiatry 78:598–605. https://doi.org/10.1016/j.biopsych.2015.05.010
Zhang Y, Zhu C, Chen H et al (2015) Frequency-dependent alterations in the amplitude of low-frequency fluctuations in social anxiety disorder. J Affect Disord 174:329–335. https://doi.org/10.1016/j.jad.2014.12.001
Wager TD, Davidson ML, Hughes BL et al (2008) Prefrontal-subcortical pathways mediating successful emotion regulation. Neuron 59:1037–1050. https://doi.org/10.1016/j.neuron.2008.09.006
van den Bos W, Cohen MX, Kahnt T et al (2012) Striatum-medial prefrontal cortex connectivity predicts developmental changes in reinforcement learning. Cereb Cortex 22:1247–1255. https://doi.org/10.1093/cercor/bhr198
Bas-Hoogendam JM, van Steenbergen H, Nienke Pannekoek J et al (2017) Voxel-based morphometry multi-center mega-analysis of brain structure in social anxiety disorder. NeuroImage Clin 16:678–688. https://doi.org/10.1016/j.nicl.2017.08.001
Wang X, Cheng B, Wang S et al (2021) Distinct grey matter volume alterations in adult patients with panic disorder and social anxiety disorder: a systematic review and voxel-based morphometry meta-analysis. J Affect Disord 281:805–823. https://doi.org/10.1016/j.jad.2020.11.057
Zhao Y, Chen L, Zhang W et al (2017) Gray matter abnormalities in non-comorbid medication-naive patients with major depressive disorder or social anxiety disorder. EBioMedicine 21:228–235. https://doi.org/10.1016/j.ebiom.2017.06.013
Wang X, Cheng B, Luo Q et al (2018) Gray matter structural alterations in social anxiety disorder: a voxel-based meta-analysis. Front Psychiatry. https://doi.org/10.3389/fpsyt.2018.00449
Østby Y, Tamnes CK, Fjell AM et al (2009) Heterogeneity in subcortical brain development: a structural magnetic resonance imaging study of brain maturation from 8 to 30 years. J Neurosci 29:11772–11782. https://doi.org/10.1523/jneuroSCI.1242-09.2009
Low LK, Cheng H-J (2006) Axon pruning: an essential step underlying the developmental plasticity of neuronal connections. Philos Trans R Soc B Biol Sci 361:1531–1544. https://doi.org/10.1098/rstb.2006.1883
Albaugh MD, Nguyen T-V, Ducharme S et al (2017) Age-related volumetric change of limbic structures and subclinical anxious/depressed symptomatology in typically developing children and adolescents. Biol Psychol 124:133–140. https://doi.org/10.1016/j.biopsycho.2017.02.002
Foell J, Palumbo IM, Yancey JR et al (2019) Biobehavioral threat sensitivity and amygdala volume: a twin neuroimaging study. Neuroimage 186:14–21. https://doi.org/10.1016/j.neuroimage.2018.10.065
Lee KH, Yoo JH, Lee J et al (2020) The indirect effect of peer problems on adolescent depression through nucleus accumbens volume alteration. Sci Rep 10:12870. https://doi.org/10.1038/s41598-020-69769-3
Heshmati M, Russo SJ (2015) Anhedonia and the brain reward circuitry in depression. Curr Behav Neurosci Rep 2:146–153. https://doi.org/10.1007/s40473-015-0044-3
Zhang Y, Liu W, Lebowitz ER et al (2020) Abnormal asymmetry of thalamic volume moderates stress from parents and anxiety symptoms in children and adolescents with social anxiety disorder. Neuropharmacology 180:108301. https://doi.org/10.1016/j.neuropharm.2020.108301
Boyes A, McLoughlin LT, Anderson H et al (2022) Basal ganglia correlates of wellbeing in early adolescence. Brain Res 1774:147710. https://doi.org/10.1016/j.brainres.2021.147710
Rubin RD, Watson PD, Duff MC et al (2014) The role of the hippocampus in flexible cognition and social behavior. Front Hum Neurosci 8:742
Felix-Ortiz AC, Tye KM (2014) Amygdala inputs to the ventral hippocampus bidirectionally modulate social behavior. J Neurosci 34:586–595. https://doi.org/10.1523/JNEUROSCI.4257-13.2014
Ashar YK, Clark J, Gunning FM et al (2021) Brain markers predicting response to cognitive-behavioral therapy for social anxiety disorder: an independent replication of Whitfield-Gabrieli et al 2015. Transl Psychiatry. 11: 260. https://doi.org/10.1038/s41398-021-01366-y
Whitfield-Gabrieli S, Ghosh SS, Nieto-Castanon A et al (2016) Brain connectomics predict response to treatment in social anxiety disorder. Mol Psychiatry 21:680–685. https://doi.org/10.1038/mp.2015.109
Craske MG, Meuret AE, Ritz T et al (2016) Treatment for anhedonia: a neuroscience driven approach. Depress Anxiety 33:927–938. https://doi.org/10.1002/da.22490
Bystritsky A, Khalsa SS, Cameron ME et al (2013) Current diagnosis and treatment of anxiety disorders. Pharm Ther 38:30–57
Gorwood P (2008) Neurobiological mechanisms of anhedonia. Dialogues Clin Neurosci 10:291–299
Strege MV, Swain D, Bochicchio L et al (2018) A pilot study of the effects of mindfulness-based cognitive therapy on positive affect and social anxiety symptoms. Front Psychol 9:866
Bas-Hoogendam JM, Groenewold NA, Aghajani M et al (2022) ENIGMA-anxiety working group: rationale for and organization of large-scale neuroimaging studies of anxiety disorders. Hum Brain Mapp 43:83–112. https://doi.org/10.1002/hbm.25100
Acknowledgements
This work was supported by the National Natural Science Foundation of China (81971682, 81571756); Shanghai Science and Technology Commission (20Y11906700); Project of Shanghai Children’s Health Service Capacity Construction (GDEK201702); Clinical Research Project of Shanghai Mental Health Center (CRC2018DSJ01-5; CRC2019ZD04); Natural Science Foundation of Shanghai (20ZR1472800); Shanghai Municipal Commission of Education (Gaofeng Clinical Medicine-20171929); Shanghai Science and Technology Commission (18JC1420305); Shanghai Municipal Health Commission (2019ZB0201; 2018BR17); Shanghai Clinical Research Center for Mental Health (19MC1911100); and Research Funds from Shanghai Mental Health Center (13dz2260500, 2018-YJ-02, 2018-YJ-05).
Funding
2030 Science and Technology Innovation Key R&D Program, China (2022ZD0209101); National Natural Science Foundation of China (81971682); Shanghai Science and Technology Commission (20ZR1472800, 20Y11906700, 18JC1420305); Project of Shanghai Children’s Health Service Capacity Construction (GDEK201702); Clinical Research Project of Shanghai Mental Health Center (CRC2018DSJ01-5); Shanghai Municipal Commission of Education (Gaofeng Clinical Medicine-20171929); Shanghai Municipal Health Commission (2019ZB0201); Shanghai Clinical Research Center for Mental Health (19MC1911100); Research Funds from Shanghai Mental Health Center (13dz2260500).
Author information
Authors and Affiliations
Contributions
Zhi Yang and Wenhong Cheng conceived this work. Wenhong Cheng, Wenjing Liu, Zhen Liu, and Changminghao Ma recruited participants. Jingjing Liu, Shuqi Xie, Shuyu Jin, Yang Hu, Lei Zhang completed data acquisition. Yue Ding, Yufeng Xia, Xiaochen Zhang, Yinzhi Kang, Zhishan Hu, Wenhong Cheng and Zhi Yang provided critical comments related to the interpretation of the study findings. Shuqi Xie helped to check the content of the article. Jingjing Liu completed data analysis and led on drafting the manuscript with subsequent iterations refined by Zhi Yang. All authors have approved the final version for publication.
Corresponding authors
Ethics declarations
Conflict of interests
The authors declare no conflict of interests.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, J., Xie, S., Hu, Y. et al. Age-dependent alterations in the coordinated development of subcortical regions in adolescents with social anxiety disorder. Eur Child Adolesc Psychiatry 33, 51–64 (2024). https://doi.org/10.1007/s00787-022-02118-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-022-02118-z