Abstract
Background
Colorectal cancer incidence is on the rise, necessitating precise symptom management. However, causal relationships among symptoms have been challenging to establish due to reliance on cross-sectional data. Cross-lagged panel network (CLPN) analysis offers a solution, leveraging longitudinal data for insight.
Objective
We employed CLPN analysis to construct symptom networks in colorectal cancer patients at three perioperative time points, aiming to identify predictive relationships and intervention opportunities.
Methods
We evaluated the prevalence and severity of symptoms throughout the perioperative period, encompassing T1 the first day of admission, T2 2–3 days postoperatively, and T3 discharge, utilizing the M. D. Anderson Symptom Inventory Gastrointestinal Cancer Module (MDASI-GI). To identify crucial nodes in the network and explore predictive and interactive effects among symptoms, CLPNs were constructed from longitudinal data in R.
Results
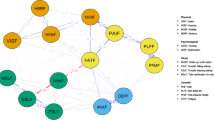
The analysis revealed a stable network, with disturbed sleep exhibiting the highest out-EI (outgoing expected influence) during T1. Distress had a sustained impact throughout the perioperative. Disturbed sleep at T1 predicted T2 bloating, fatigue, distress, and pain. T1 distress predicted T2 sadness severity. T2 distress primarily predicted T3 fatigue, disturbed sleep, changes in taste, and bloating. T2 shortness of breath predicted T3 changes in taste and loss of appetite. Furthermore, biochemical markers like RBC and ALB had notable influence on symptom clusters during T1→T2 and T2→T3, respectively.
Conclusion
Prioritizing disturbed sleep during T1 and addressing distress throughout the perioperative phase is recommended. Effective symptom management not only breaks the chain of symptom progression, enhancing healthcare impact, but also eases patient symptom burdens.





Similar content being viewed by others
Data availability
The dataset for this study will not be made publicly available due to ethical restrictions. The dataset will be personally available if there is reasonable request. Readers and all interested researchers may contact Shang Bin (Sevenage007@163.com).
References
Sung H, Ferlay J, Siegel RL et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries[J]. CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Zhou J, Zheng R, Zhang S, et al. Colorectal cancer burden and trends: comparison between China and major burden countries in the world[J]. Chin J Cancer Res, 2021, 33(1): 1-10. https://doi.org/10.21147/j.issn.1000-9604.2021.01.01.
Shen XF, Zhou CM, Hua Q et al (2022) Impact of operation duration on short-term and long-term prognosis in patients undergoing radical colorectal[J]. J Cancer 13(3):1160–1167. https://doi.org/10.7150/jca.65817
Renna ME, Shrout MR, Madison AA et al (2022) Depression and anxiety in colorectal cancer patients: ties to pain, fatigue, and inflammation[J]. Psychooncology 31(9):1536–1544. https://doi.org/10.1002/pon.5986
Storey S, Luo X, Ofner S et al (2022) Hyperglycemia, symptoms, and symptom clusters in colorectal cancer survivors with type 2 diabetes[J]. Support Care Cancer 30(12):10149–10157. https://doi.org/10.1007/s00520-022-07442-3
Zielinska A, Wlodarczyk M, Makaro A et al (2021) Management of pain in colorectal cancer patients[J]. Crit Rev Oncol Hematol 157:103122. https://doi.org/10.1016/j.critrevonc.2020.103122
Wei JN, Li SX (2018) The relationship between nutritional risks and cancer-related fatigue in patients with colorectal cancer fast-track surgery[J]. Cancer Nurs 41(6):E41–E47. https://doi.org/10.1097/ncc.0000000000000541
Agasi-Idenburg SC, Thong MSY, Punt CJA et al (2017) Comparison of symptom clusters associated with fatigue in older and younger survivors of colorectal cancer[J]. Support Care Cancer 25(2):625–632. https://doi.org/10.1007/s00520-016-3451-4
Gijzen M W M, Rasing S P A, Creemers D H M, et al. Suicide ideation as a symptom of adolescent depression. a network analysis[J]. J Affect Disord, 2021, 278: 68-77. https://doi.org/10.1016/j.jad.2020.09.029.
Zhu Z, Sun YL, Kuang Y et al (2023) Contemporaneous symptom networks of multidimensional symptom experiences in cancer survivors: a network analysis[J]. Cancer Med 12(1):663–673. https://doi.org/10.1002/cam4.4904
Ivziku D, De Maria M, Ferramosca FMP et al (2022) What determines physical, mental and emotional workloads on nurses? A cross-sectional study[J]. J Nurs Manag 30(8):4387–4397. https://doi.org/10.1111/jonm.13862
Smith GL, Banegas MP, Acquati C et al (2022) Navigating financial toxicity in patients with cancer: a multidisciplinary management approach[J]. CA Cancer J Clin 72(5):437–453. https://doi.org/10.3322/caac.21730
Hao JL, Gu LY, Liu P et al (2021) Symptom clusters in patients with colorectal cancer after colostomy: a longitudinal study in Shanghai[J]. J Int Med Res 49(12):3000605211063105. https://doi.org/10.1177/03000605211063105
Rha SY, Lee J (2021) Stable symptom clusters and evolving symptom networks in relation to chemotherapy cycles[J]. J Pain Symptom Manage 61(3):544–554. https://doi.org/10.1016/j.jpainsymman.2020.08.008
Jing F, Zhu Z, Qiu JJ et al (2023) Contemporaneous symptom networks and correlates during endocrine therapy among breast cancer patients: a network analysis[J]. Front Oncol 13:1081786. https://doi.org/10.3389/fonc.2023.1081786
Fried EI, Boschloo L, Van Borkulo CD et al (2015) Commentary: “Consistent superiority of selective serotonin reuptake inhibitors over placebo in reducing depressed mood in patients with major depression”[J]. Front Psychiatry 6:117. https://doi.org/10.3389/fpsyt.2015.00117
Jones PJ, Ma R, Mcnally RJ (2021) Bridge centrality: a network approach to understanding comorbidity[J]. Multivariate Behav Res 56(2):353–367. https://doi.org/10.1080/00273171.2019.1614898
De Rooij BH, Oerlemans S, Van Deun K et al (2021) Symptom clusters in 1330 survivors of 7 cancer types from the PROFILES registry: a network analysis[J]. Cancer 127(24):4665–4674. https://doi.org/10.1002/cncr.33852
Sheikh-Wu SF, Anglade D, Gattamorta K et al (2022) Positive psychology mediates the relationship between symptom frequency and quality of life among colorectal cancer survivors during acute cancer survivorship[J]. Eur J Oncol Nurs 58:102136. https://doi.org/10.1016/j.ejon.2022.102136
Ross EJ, Cassisi JE, Joseph D et al (2022) Cross-lagged analyses between gastrointestinal symptoms, psychological distress, and disability in emerging adults[J]. Appl Psychol Health Well Being 14(3):920–936. https://doi.org/10.1111/aphw.12358
Rhemtulla M, Bork R V, Cramer A O J J M B R. Cross-lagged network models[J]. Multivariate Behav Res, 2017
Chavez-Baldini U, Verweij K, De Beurs D et al (2022) The interplay between psychopathological symptoms: transdiagnostic cross-lagged panel network model[J]. Bjpsych Open 8(4):e116. https://doi.org/10.1192/bjo.2022.516
Liang YM, Yang LX, Xi JZ et al (2022) The unique role of sleep problems among symptoms of posttraumatic stress disorder: a cross-lagged panel network analysis[J]. Acta Psychol 54(10):1206–1215. https://doi.org/10.3724/sp.J.1041.2022.01206
Blanken TF, Van Der Zweerde T, Van Straten A et al (2019) Introducing network intervention analysis to investigate sequential, symptom-specific treatment effects: a demonstration in co-occurring insomnia and depression[J]. Psychother Psychosom 88(1):52–54. https://doi.org/10.1159/000495045
Chen R-W, Yang S-L, Xu Z-Y, et al. Validation and application of the Chinese version of the M. D. Anderson symptom inventory in breast cancer patients[J]. J Pain Symptom Manage, 2019, 57(4): 820-827. https://doi.org/10.1016/j.jpainsymman.2019.01.007.
Epskamp S, Cramer A O J, Waldorp L J, et al. qgraph: network visualizations of relationships in psychometric data[J]. J Stat Softw, 2012, 48(4): 1-18. https://doi.org/10.18637/jss.v048.i04.
Robinaugh DJ, Millner AJ, Mcnally RJ (2016) Identifying highly influential nodes in the complicated grief network[J]. J Abnorm Psychol 125(6):747–57. https://doi.org/10.1037/abn0000181
Epskamp S, Borsboom D, Fried EI (2018) Estimating psychological networks and their accuracy: a tutorial paper[J]. Behav Res Methods 50(1):195–212. https://doi.org/10.3758/s13428-017-0862-1
Epskamp S, Fried EI (2018) A tutorial on regularized partial correlation networks[J]. Psychol Methods 23(4):617–634. https://doi.org/10.1037/met0000167
Funkhouser CJ, Chacko AA, Correa KA et al (2021) Unique longitudinal relationships between symptoms of psychopathology in youth: a cross-lagged panel network analysis in the ABCD study[J]. J Child Psychol Psychiatry 62(2):184–194. https://doi.org/10.1111/jcpp.13256
Robleda G, Roche-Campo F, Sanchez V et al (2015) Postoperative discomfort after abdominal surgery: an observational study[J]. J Perianesth Nurs 30(4):272–279. https://doi.org/10.1016/j.jopan.2014.06.005
Zhang S, Guo W P, Jiao Y L, et al. Systematic review and meta-analysis of the effect of transcutaneous electrical acupoint stimulation on gastrointestinal function after laparoscopic surgery[J]. Ann Palliat Med, 2021, 10(11): 11840-11848. https://doi.org/10.21037/apm-21-3046.
Zhu Q, Yang JD, Zhang Y et al (2021) Early mobilization intervention for patient rehabilitation after renal transplantation[J]. Am J Transl Res 13(6):7300–7305
Abraham J, Meng A, Siraco S et al (2020) A qualitative study of perioperative depression and anxiety in older adults[J]. Am J Geriatr Psychiatry 28(10):1107–1118. https://doi.org/10.1016/j.jagp.2020.02.010
Wilson N, Lee JJ, Bei B (2019) Postpartum fatigue and depression: a systematic review and meta-analysis[J]. J Affect Disord 246:224–233. https://doi.org/10.1016/j.jad.2018.12.032
Tomaso C C, Johnson A B, Nelson T D. The effect of sleep deprivation and restriction on mood, emotion, and emotion regulation: three meta-analyses in one[J]. Sleep, 2021, 44(6): zsaa289. https://doi.org/10.1093/sleep/zsaa289.
Chang JR, Fu SN, Li X et al (2022) The differential effects of sleep deprivation on pain perception in individuals with or without chronic pain: a systematic review and meta-analysis[J]. Sleep Med Rev 66:101695. https://doi.org/10.1016/j.smrv.2022.101695
Zhu GH, Li J, Li J et al (2021) The characteristics and related factors of insomnia among postoperative patients with gastric cancer: a cross-sectional survey[J]. Support Care Cancer 29(12):7315–7322. https://doi.org/10.1007/s00520-021-06295-6
Dinan TG, Cryan JF (2017) Brain-gut-microbiota axis and mental health[J]. Psychosom Med 79(8):920–926. https://doi.org/10.1097/psy.0000000000000519
Maunsell R, Sodergren S, Hopkinson J et al (2021) Nutritional care in colorectal cancer-what is the state of play?[J]. Colorectal Dis 23(12):3227–3233. https://doi.org/10.1111/codi.15933
Hsu JC, Watari I, Funaki Y et al (2018) Unilateral nasal obstruction induces degeneration of fungiform and circumvallate papillae in rats[J]. J Formos Med Assoc 117(3):220–226. https://doi.org/10.1016/j.jfma.2017.04.013
Kang B, Zhao ZQ, Liu XY et al (2022) Effect of hypoalbuminemia on short-term outcomes after colorectal cancer surgery: a propensity score matching analysis[J]. Front Nutr 9:e925086. https://doi.org/10.3389/fnut.2022.925086
Altintas MM, Kaya S, Kocaoglu AE et al (2022) Does preoperative anaemia have an effect on the perioperative period in colorectal cancer surgery?[J]. Niger J Clin Pract 25(7):1102–1106. https://doi.org/10.4103/njcp.njcp_1664_21
Robleda G, Banos JE (2021) Health care professionals’ assessment of patient discomfort after abdominal surgery[J]. J Perianesth Nurs 36(5):553–558. https://doi.org/10.1016/j.jopan.2020.11.007
Xu C, He J, Wang H et al (2022) Single-cell transcriptomic analysis identifies an immune-prone population in erythroid precursors during human ontogenesis[J]. Nature Immunology 23(7):1109–1120. https://doi.org/10.1038/s41590-022-01245-8
Acknowledgements
The authors would like to appreciate all the staff who helped us complete this project.
Funding
This study was supported by the “QingLan Project” of universities in Jiangsu Province. Funders were not involved in this study.
Qinglan Project of Jiangsu Province of China,Su Teacher's Letter (2023) No. 51
Author information
Authors and Affiliations
Contributions
Bin SHANG: Conceptualization; Data curation; Investigation; Methodology; Writing – original draft; Writing – review & editing.
Zekun BIAN: Investigation; Methodology; Writing – review & editing.
Caifeng LUO: Conceptualization; Supervision; Writing – review & editing.
Fei LV: Writing – review & editing; Funding acquisition.
Jing WU: Supervision; Investigation.
Shuhong LV: Investigation.
Qing WEI: Investigation.
Corresponding author
Ethics declarations
Consent for publication
Not applicable
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This study was conducted in compliance with the principles outlined in the Declaration of Helsinki. The research protocol was approved by the Medical Ethics Committee of Jiangsu University (No. 20221019-1). Prior to their participation, written informed consent was obtained from all subjects involved in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shang, B., Bian, Z., Luo, C. et al. Exploring the dynamics of perioperative symptom networks in colorectal cancer patients: a cross-lagged panel network analysis. Support Care Cancer 32, 62 (2024). https://doi.org/10.1007/s00520-023-08288-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-023-08288-z