Abstract
Background
Laparoscopic treatment has been increasingly adopted for giant hepatic hemangioma (HH), but the role of liver resection or enucleation remains uncertain. The aim of this study is to compare the laparoscopic resection (LR) with laparoscopic enucleation (LE) for HH, and to provide evidence on how to choose the most suitable approach for HH.
Methods
A retrospective analysis of HH patients underwent laparoscopic treatment between March 2015 and August 2022 was performed. Perioperative outcomes were compared based on the surgical approaches, and risk factors for increased blood loss was calculated by logistic regression analysis.
Results
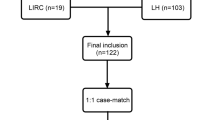
A total of 127 patients in LR group and 287 patients in LE group were enrolled in this study. The median blood loss (300 vs. 200 mL, P < 0.001) was higher in LE group than that in LR group. Independent risk factors for blood loss higher than 400 mL were tumor size ≥ 10 cm, tumor adjacent to major vessels, tumor occupying right liver or caudate lobe, and the portal phase enhancement ratio (PER) ≥ 38.9%, respectively. Subgroup analysis showed that LR was associated with less blood loss (155 vs. 400 mL, P < 0.001) than LE procedure in patients with high PER value. Both LR and LE approaches exhibited similar perioperative outcomes in patients with low PER value.
Conclusions
Laparoscopic treatment for HH could be feasibly and safely performed by both LE and LR. For patients with PER higher than 38.9%, the LR approach is recommended.
Graphical abstract





Similar content being viewed by others
References
Hasan HY, Louis Hinshaw J, Borman EJ, Gegios A, Leverson G, Winslow ER (2014) Assessing normal growth of hepatic hemangiomas during long-term follow-up. JAMA Surg 149:1266–1271
Bo Yoon C, Mindie HN (2005) The diagnosis and management of benign hepatic tumors. J Clin Gastroenterol 39:401–412
Trotter JF, Everson GT (2001) Benign focal lesions of the liver. Clin Liver Dis 5:17
Qiu J, Chen S, Wu H (2015) Quality of life can be improved by surgical management of giant hepatic haemangioma with enucleation as the preferred option. HPB (Oxford) 17:490
Erhan H, Hasan A, Arif O, Ahmet O (2005) Giant liver hemangioma: therapy by enucleation or liver resection. World J Surg 29:890–893
Tan H, Zhou R, Liu L, Si S, Sun Y, Xu L, Liu X, Yang Z (2022) Comparison of efficacy and safety of laparoscopic and open enucleation for liver hemangioma in the right hemi liver: a retrospective cohort study. Ann Transl Med 10:764
Ghosh NK, Rahul R, Singh A, Malage S, Sharma S, Kumar A, Singh RK, Behari A, Saxena R (2023) Surgery for symptomatic hepatic hemangioma: resection vs. enucleation, an experience over two decades. Ann Hepatobiliary Pancreat Surg 27:258–263
Abu Hilal M, Aldrighetti L, Dagher I, Edwin B, Troisi RI, Alikhanov R, Aroori S, Belli G, Besselink M, Briceno J, Gayet B, D’Hondt M, Lesurtel M, Menon K, Lodge P, Rotellar F, Santoyo J, Scatton O, Soubrane O, Sutcliffe R, Van Dam R, White S, Halls MC, Cipriani F, Van der Poel M, Ciria R, Barkhatov L, Gomez-Luque Y, Ocana-Garcia S, Cook A, Buell J, Clavien PA, Dervenis C, Fusai G, Geller D, Lang H, Primrose J, Taylor M, Van Gulik T, Wakabayashi G, Asbun H, Cherqui D (2018) The southampton consensus guidelines for laparoscopic liver surgery: from indication to implementation. Ann Surg 268:11–18
Li L, Xu L, Wang P, Liu F, Wei Y, Xu M, Zhang M, Li B (2022) Advantages of laparoscopic hepatic hemangioma surgery in quality of life: a prospective study. Surg Endosc 36:8967–8974
Liu Q, Liu F, Ding J, Wei Y, Li B (2019) Surgical outcomes and quality of life between laparoscopic and open approach for hepatic hemangioma: a propensity score matching analysis. Medicine (Baltimore) 98:e14485
Pulvirenti E, Toro A, Di Carlo I (2010) An update on indications for treatment of solid hepatic neoplasms in noncirrhotic liver. Future Oncol 6:1243–1250
Aziz H, Brown ZJ, Baghdadi A, Kamel IR, Pawlik TM (2022) A comprehensive review of hepatic hemangioma management. J Gastrointest Surg 26:1998–2007
Liu F, Wei Y, Chen K, Li H, Wang W, Wu H, Wen T, Li B (2019) The extrahepatic glissonian versus hilar dissection approach for laparoscopic formal right and left hepatectomies in patients with hepatocellular carcinoma. J Gastrointest Surg 23:2401–2410
Zhang H, Liu F, Wen N, Li B, Wei Y (2022) Patterns, timing, and predictors of recurrence after laparoscopic liver resection for hepatocellular carcinoma: results from a high-volume HPB center. Surg Endosc 36:1215–1223
Dindo DDN, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Koch M, Garden OJ, Padbury R, Rahbari NN, Adam R, Capussotti L, Fan ST, Yokoyama Y, Crawford M, Makuuchi M, Christophi C, Banting S, Brooke-Smith M, Usatoff V, Nagino M, Maddern G, Hugh TJ, Vauthey JN, Greig P, Rees M, Nimura Y, Figueras J, DeMatteo RP, Buchler MW, Weitz J (2011) Bile leakage after hepatobiliary and pancreatic surgery: a definition and grading of severity by the International Study Group of Liver Surgery. Surgery 149:680–688
Rahbari NN, Garden OJ, Padbury R, Maddern G, Koch M, Hugh TJ, Fan ST, Nimura Y, Figueras J, Vauthey JN, Rees M, Adam R, DeMatteo RP, Greig P, Usatoff V, Banting S, Nagino M, Capussotti L, Yokoyama Y, Brooke-Smith M, Crawford M, Christophi C, Makuuchi M, Büchler MW, Weitz J (2011) Post-hepatectomy haemorrhage: a definition and grading by the International Study Group of Liver Surgery (ISGLS). HPB 13:528–535
Ciria R, Cherqui D, Geller DA, Briceno J, Wakabayashi G (2016) Comparative short-term benefits of laparoscopic liver resection: 9000 cases and climbing. Ann Surg 263:761–777
Jiang B, Shen ZC, Fang XS, Wang XM (2022) Enucleation versus hepatectomy for hepatic hemangiomas: a meta-analysis. Front Surg 9:960768
Nguyen KT, Gamblin TC, Geller DA (2009) World review of laparoscopic liver resection-2804 patients. Ann Surg 250:831–841
Abdel Wahab M, El Nakeeb A, Ali MA, Mahdy Y, Shehta A, Abdulrazek M, El Desoky M, Abdel Wahab R (2018) Surgical management of giant hepatic hemangioma: single center’s experience with 144 patients. J Gastrointest Surg 22:849–858
Aghayan DL, d’Albenzio G, Fretland ÅA, Pelanis E, Røsok BI, Yaqub S, Palomar R, Edwin B (2023) Laparoscopic parenchyma-sparing liver resection for large (≥ 50 mm) colorectal metastases. Surg Endosc 37:225–233
Cheung TT, Wang X, Efanov M, Liu R, Fuks D, Choi GH, Syn NL, Chong CC, Sucandy I, Chiow AK, Marino MV (2021) International robotic and laparoscopic liver resection study group collaborators. Minimally invasive liver resection for huge (≥10 cm) tumors: an international multicenter matched cohort study with regression discontinuity analyses. Hepatobiliary Surg Nutr 10:587–597
Willems E, D’Hondt M, Kingham TP, Fuks D, Choi GH, Syn NL, Sucandy I, Marino MV, Prieto M, Chong CC, Lee JH (2022) International robotic and laparoscopic liver resection study group investigators. Comparison between minimally invasive right anterior and right posterior sectionectomy vs right hepatectomy: an international multicenter propensity score-matched and coarsened-exact-matched analysis of 1100 patients. J Am Coll Surg 235:859–868
Wen ZQ, Yan YQ, Yang JM, Wu MC (2008) Precautions in caudate lobe resection: report of 11 cases. World J Gastroenterol 14:2767
D’Hondt M, Willems E, Parmentier I, Pottel H, De Meyere C, Vansteenkiste F, Besselink MG, Verslype C (2020) Laparoscopic liver resection for liver tumours in proximity to major vasculature: a single-center comparative study. Eur J Surg Oncol 46:539–547
Acknowledgements
None.
Funding
This work was supported by the Sichuan Science and Technology Program (No. 2022YFS0090 and 2023YFS0230).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Haili Zhang, Hongwei Xu, Ningyuan Wen, Bo Li, Kefei Chen, Yonggang Wei have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, H., Xu, H., Wen, N. et al. Laparoscopic liver resection or enucleation for giant hepatic hemangioma: how to choose?. Surg Endosc (2024). https://doi.org/10.1007/s00464-024-10820-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00464-024-10820-z