Abstract
Background
Colorectal surgery has benefited from advances in precision medicine such as total mesorectal resection, and recently, mesocolon resection, fluorescent perfusion imaging, and fluorescent node mapping. However, these advances fail to address the variable quality of mesocolon dissection and the directed extent of vascular dissection (including high ligation) or pre-resection anastomotic perfusion mapping, thereby impacting anastomotic leaks. We propose a new paradigm of precision image-directed colorectal surgery involving 3D preoperative resection modeling and intraoperative fluoroscopic and fluorescence vascular imaging which better defines optimal dissection planes and vascular vs. anatomy-based resection lines according to our hypothesis.
Methods
Six pigs had preoperative CT with vascular 3D reconstruction allowing for the preoperative planning of vascular-based dissection. Laparoscopic surgery was performed in a hybrid operating room (OR). Superselective arterial catheterization was performed in branches of the superior mesenteric artery (SMA) or the inferior mesenteric artery (IMA). Intraoperative boluses of 0.1 mg/kg or a continuous infusion of indocyanine green (ICG) (0.01 mg/mL) were administered to guide fluorescent-based sigmoid and ileocecal resections. Fluorescence was assessed using proprietary software at several regions of interest (ROI) in the right and left colon.
Results
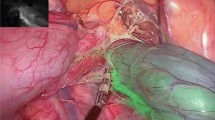
The approach was feasible and safe. Selective catheterization took an average of 43 min. Both bolus and continuous perfusion clearly marked pre-identified vessels (arteries/veins) and the target colon segment, facilitating precise resections based on the visible vascular anatomy. Quantitative software analysis indicated the optimal resection margin for each ROI.
Conclusion
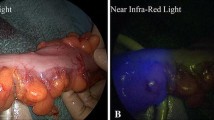
Intra-arterial fluorescent mapping allows visualization of major vascular structures and segmental colonic perfusion. This may help to prevent any inadvertent injury to major vascular structures and to precisely determine perfusion-based resection planes and margins. This could enable tailoring of the amount of colon resected, ensure good anastomotic perfusion, and improve oncological outcomes.





Similar content being viewed by others
References
Dekker E, Tanis PJ, Vleugels JLA, Kasi PM, Wallace MB (2019) Colorectal cancer. Lancet 394:1467–1480
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68:394–424
Arnold M, Sierra MS, Laversanne M, Soerjomataram I, Jemal A, Bray F (2017) Global patterns and trends in colorectal cancer incidence and mortality. Gut 66:683–691
Races A, Males MWMB SEER Cancer Statistics Review 1975–2014
Bertelsen CA, Neuenschwander AU, Jansen JE, Wilhelmsen M, Kirkegaard-Klitbo A, Tenma JR, Bols B, Ingeholm P, Rasmussen LA, Jepsen LV, Iversen ER, Kristensen B, Gogenur I, Danish Colorectal Cancer G (2015) Disease-free survival after complete mesocolic excision compared with conventional colon cancer surgery: a retrospective, population-based study. Lancet Oncol 16:161–168
Dahlberg M, Påhlman L, Bergström R, Glimelius B (1998) Improved survival in patients with rectal cancer: a population-based register study. Br J Surg 85:515–520
Hohenberger W, Weber K, Matzel K, Papadopoulos T, Merkel S (2009) Standardized surgery for colonic cancer: complete mesocolic excision and central ligation–technical notes and outcome. Colorectal Dis 11:354–364
West NP, Kobayashi H, Takahashi K, Perrakis A, Weber K, Hohenberger W, Sugihara K, Quirke P (2012) Understanding optimal colonic cancer surgery: comparison of Japanese D3 resection and European complete mesocolic excision with central vascular ligation. J Clin Oncol 30:1763–1769
Benz S, Tannapfel A, Tam Y, Grünenwald A, Vollmer S, Stricker I (2019) Proposal of a new classification system for complete mesocolic excison in right-sided colon cancer. Tech Coloproctol 23:251–257
Kuzu MA, Ismail E, Çelik S, Şahin MF, Güner MA, Hohenberger W, Açar HI (2017) Variations in the vascular anatomy of the right colon and implications for right-sided colon surgery. Dis Colon Rectum 60:290–298
Alsabilah JF, Razvi SA, Albandar MH, Kim NK (2017) Intraoperative archive of right colonic vascular variability aids central vascular ligation and redefines gastrocolic trunk of henle variants. Dis Colon Rectum 60:22–29
Wu C, Ye K, Wu Y, Chen Q, Xu J, Lin J, Kang W (2019) Variations in right colic vascular anatomy observed during laparoscopic right colectomy. World J Surg Oncol 17:16
Kim DH, Lubner MG, Cahoon AR, Pooler BD, Pickhardt PJ (2018) Flat serrated polyps at CT colonography: relevance, appearance, and optimizing interpretation. Radiographics 38:60–74
Maupoey Ibáñez J, Pàmies Guilabert J, Frasson M, Boscà Robledo A, Giner Segura F, García-Granero Ximénez E (2019) Accuracy of CT-Colonography in the preoperative staging of colon cancer. A prospective study of 217 patients. Colorectal Dis 21:1151–1163
Nesgaard J, Stimec B, Bakka A, Edwin B, Ignjatovic D, Group RS, Oresland T, Færden AE, Thorsen Y, Andersen S (2015) Navigating the mesentery: a comparative pre-and per-operative visualization of the vascular anatomy. Colorectal Dis 17:810–818
Horton KM, Fishman EK (2010) CT angiography of the mesenteric circulation. Radiol Clin 48:331–345
Mari FS, Nigri G, Pancaldi A, De Cecco CN, Gasparrini M, Dall’Oglio A, Pindozzi F, Laghi A, Brescia A (2013) Role of CT angiography with three-dimensional reconstruction of mesenteric vessels in laparoscopic colorectal resections: a randomized controlled trial. Surg Endosc 27:2058–2067
D'Agostino J, Diana M, Vix M, Soler L, Marescaux J (2012) Three-dimensional virtual neck exploration before parathyroidectomy. N Engl J Med 367:1072–1073
Pessaux P, Diana M, Soler L, Piardi T, Mutter D, Marescaux J (2014) Robotic duodenopancreatectomy assisted with augmented reality and real-time fluorescence guidance. Surg Endosc 28:2493–2498
Pessaux P, Diana M, Soler L, Piardi T, Mutter D, Marescaux J (2015) Towards cybernetic surgery: robotic and augmented reality-assisted liver segmentectomy. Langenb Arch Surg 400:381–385
Kong S-H, Haouchine N, Soares R, Klymchenko A, Andreiuk B, Marques B, Shabat G, Piéchaud T, Diana M, Cotin S (2017) Robust augmented reality registration method for localization of solid organs’ tumors using CT-derived virtual biomechanical model and fluorescent fiducials. Surg Endosc 31:2863–2871
van Manen L, Handgraaf HJM, Diana M, Dijkstra J, Ishizawa T, Vahrmeijer AL, Mieog JSD (2018) A practical guide for the use of indocyanine green and methylene blue in fluorescence-guided abdominal surgery. J Surg Oncol 118:283–300
Diana M (2018) Fluorescence-guided surgery applied to the digestive system: the cybernetic eye to see the invisible. Cir Esp 96:65–68
Baiocchi GL, Diana M, Boni L (2018) Indocyanine green-based fluorescence imaging in visceral and hepatobiliary and pancreatic surgery: State of the art and future directions. World J Gastroenterol 24:2921–2930
Diana M (2017) Enabling precision digestive surgery with fluorescence imaging. Transl Gastroenterol Hepatol 2:97
Liu Y-Y, Pop R, Diana M, Kong S-H, Lègner A, Beaujeux R, Marescaux J (2016) Real-time fluorescence angiography by intra-arterial indocyanine green injection to identify obscure gastrointestinal bleeding territory: proof of concept in the porcine model. Surg Endosc 30:2143–2150
Heiliger C, Piecuch J, Frank A, Andrade D, Von Ehrlich-Treuenstätt V, Schiergens T, Rentsch M, Werner J, Karcz K (2018) Intraarterial indocyanine green (ICG) fluorescence augmentation by marking embryonal resection areas in colorectal surgery: a feasibility study in a porcine model. Minim Invasive Ther Allied Technol 28:321–325
Kilkenny C, Browne W, Cuthill IC, Emerson M, Altman DG, Group NCRRGW (2010) Animal research: reporting in vivo experiments: the ARRIVE guidelines. J Gene Med 12:561–563
Pedregosa F, Varoquaux G, Gramfort A, Michel V, Thirion B, Grisel O, Blondel M, Prettenhofer P, Weiss R, Dubourg V (2011) Scikit-learn: machine learning in python. J Mach Learn Res 12:2825–2830
van Dijk LJ, van Noord D, van Mierlo M, Bijdevaate DC, Bruno MJ, Moelker A (2020) Single-center retrospective comparative analysis of transradial, transbrachial, and transfemoral approach for mesenteric arterial procedures. J Vasc Interv Radiol 31:130–138
Khalilzadeh O, Baerlocher MO, Shyn PB, Connolly BL, Devane AM, Morris CS, Cohen AM, Midia M, Thornton RH, Gross K (2017) Proposal of a new adverse event classification by the Society of Interventional Radiology Standards of Practice Committee. J Vasc Interv Radiol 28:1432–1437
Oderich GS, Tallarita T, Gloviczki P, Duncan AA, Kalra M, Misra S, Cha S, Bower TC (2012) Mesenteric artery complications during angioplasty and stent placement for atherosclerotic chronic mesenteric ischemia. J Vasc Surg 55:1063–1071
Alander JT, Kaartinen I, Laakso A, Pätilä T, Spillmann T, Tuchin VV, Venermo M, Välisuo P (2012) A review of indocyanine green fluorescent imaging in surgery. Int J Biomed Imaging. https://doi.org/10.1155/2012/940585
Negoi I, Beuran M, Hostiuc S, Negoi RI, Inoue Y (2018) Surgical anatomy of the superior mesenteric vessels related to colon and pancreatic surgery: a systematic review and meta-analysis. Sci Rep 8:4184
Acknowledgments
The authors are grateful to Guy Temporal, professional in Medical English proofreading for his assistance with manuscript edition.
Funding
This study was partly funded by the IHU Strasbourg through the ANR Grant 10-IAHU-0002 and partly by the ARC Foundation for Cancer Research (9, rue Guy Môquet, BP 90003, 94803 Villejuif Cedex, France), via the ELIOS Grant (PI Michele Diana).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Michele Diana is member of the Scientific Board of Diagnostic Green. Michele Diana is the recipient of a grant from the ARC Foundation (https://www.fondation-arc.org/) for the ELIOS (Endoscopic Luminescent Imaging for precision Oncologic Surgery) project. Jacques Marescaux is the President of the IRCAD Institute, which is partly funded by KARL STORZ and Medtronic. Lee Swanström consults for Medtronic, Boston Scientific, and Olympus. Antonello Forgione, Manuel Barberio, Vincent Agnus, and Benoit Gallix have nothing to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 261585 kb)
Rights and permissions
About this article
Cite this article
Forgione, A., Barberio, M., Agnus, V. et al. Precision image-guided colonic surgery: proof of concept for enhanced preoperative and intraoperative vascular imaging. Surg Endosc 35, 962–970 (2021). https://doi.org/10.1007/s00464-020-08000-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-08000-w