Abstract
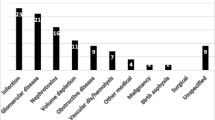
Acute kidney injury (AKI) is a known independent risk factor for morbidity/mortality but there is scarcity of robust data on it among childhood nephrotic syndrome (NS). We assessed the incidence of AKI among hospitalized children with NS as well as looked for any significant risk factors. Prospective observational study conducted across two tertiary pediatric hospitals in Eastern India from September 2020 to August 2021. Children aged 1–18 years admitted with NS and without any nephritic features or pre-existing chronic kidney disease (CKD) were included. In 200 admissions (n = 176; 63% female, median age 4 years [IQR: 3–7]), AKI occurred in 36 (18%; 95% CI 13 to 36%). Two children required kidney replacement therapy and one death was recorded. In 27/36 (75%), AKI resolved within 48 h, 4 had persistent AKI, 3 acute kidney disease, and two progressed to CKD. On multivariate regression analysis: fractional excretion of sodium ≤ 0.2% (OR 12.77; 95% CI 3.5–46.4), male gender (OR 6.38; 95% CI 2.76–14.74), underlying infection (OR 5.44; 95% CI 2.4–11.86), nephrotoxic drugs (OR 4.83; 95% CI 2.21–10.54), and albumin ≤ 1.4 g/dl (OR 4.35; 95% CI 1.55–12.8) were associated with AKI. A predictive equation using these five variables on admission had high AUC (0.86) in correctly identifying 17 children who subsequently developed AKI.
Conclusion: In a low resource setting, AKI is common among hospitalized children with NS. Larger multi-center prospective studies are needed to refine prediction equations and test its utility in preventing AKI development.
What is Known: • Acute Kidney Injury is a known independent risk factor for increased morbidity and mortality. • There are few studies to assess the incidence of Acute kidney injury in hospitalised cases of childhood nephrotic syndrome.. | |
What is New: • This is the largest prospective cohort of children suffering from nephrotic syndrome, in India, proposing a novel algorithm for predicting the risk of AKI among hospitalised cases of childhood nephrotic syndrome. |
Graphical Abstract





Similar content being viewed by others
Data Availability
Data will be stored in ICH nephrology division and available on request.
References
Chanchlani R, Parekh RS (2016) Ethnic differences in childhood nephrotic syndrome. Front Pediatr 4:39
Gipson DS, Massengill SF, Yao L, Nagaraj S, Smoyer WE, Mahan JD et al (2009) Management of childhood onset nephrotic syndrome. Pediatrics 124(2):747–757
Sinha A, Bagga A, Banerjee S, Mishra K, Mehta A, Agarwal I et al (2021) Steroid sensitive nephrotic syndrome: revised guidelines. Indian Pediatr 58(5):461–481
Kaddourah A, Basu RK, Bagshaw SM, Goldstein SL (2017) AWARE Investigators. Epidemiology of acute kidney injury in critically ill children and young adults. N Engl J Med 376(1):11–20
Rheault MN, Wei CC, Hains DS, Wang W, Kerlin BA, Smoyer WE (2014) Increasing frequency of acute kidney injury amongst children hospitalized with nephrotic syndrome. Pediatr Nephrol Berl Ger 29(1):139–147
Rheault MN, Zhang L, Selewski DT, Kallash M, Tran CL, Seamon M et al (2015) AKI in children hospitalized with nephrotic syndrome. Clin J Am Soc Nephrol CJASN 10(12):2110–2118
Sharma M, Mahanta A, Barman AK, Mahanta PJ (2018) Acute kidney injury in children with nephrotic syndrome: a single-center study. Clin Kidney J 11(5):655–658
Yang EM, Yoo KH, Ahn YH, Kim SH, Lee JW, Chung WY et al (2021) Lower albumin level and longer disease duration are risk factors of acute kidney injury in hospitalized children with nephrotic syndrome. Pediatr Nephrol Berl Ger 36(3):701–709
Kim MY, Cho MH, Kim JH, Ahn YH, Choi HJ, Ha IS et al (2018) Acute kidney injury in childhood-onset nephrotic syndrome: incidence and risk factors in hospitalized patients. Kidney Res Clin Pract 37(4):347–355
Fujinaga S, Kusaba K (2019) Impact of acute kidney injury at the onset of idiopathic nephrotic syndrome in Japanese children. Clin Exp Nephrol 23(9):1171–1172
Guan N, Yao Y, Xiao H, Ding J, Zhong X, Wang F et al (2021) Factors predicting the recovery from acute kidney injury in children with primary nephrotic syndrome. Clin Exp Nephrol 25(9):1011–1017
Sato M, Ishikura K, Ando T, Kikunaga K, Terano C, Hamada R et al (2021) Prognosis and acute complications at the first onset of idiopathic nephrotic syndrome in children: a nationwide survey in Japan (JP-SHINE study). Nephrol Dial Transplant Off Publ Eur Dial Transpl Assoc Eur Ren Assoc 36(3):475–481
Prasad BS, Kumar M, Dabas A, Mishra K (2019) Profile of acute kidney injury in hospitalized children with idiopathic nephrotic syndrome. Indian Pediatr 56(2):119–122
Kumar R, Agrwal S, Mantan M, Yadav S (2021) Acute kidney injury in children hospitalized with a relapse of nephrotic syndrome: a short-term outcome study. Saudi J Kidney Dis Transpl 32(2):437–44
Indian Pediatric Nephrology Group, Indian Academy of Pediatrics, Bagga A, Ali U, Banerjee S, Kanitkar M, Phadke KD et al (2008) Management of steroid sensitive nephrotic syndrome: revised guidelines. Indian Pediatr 45(3):203–14
Khwaja A (2012) KDIGO clinical practice guidelines for acute kidney injury. Nephron Clin Pract 120(4):c179-184
Holmes J, Roberts G, May K, Tyerman K, Geen J, Williams JD et al (2017) The incidence of pediatric acute kidney injury is increased when identified by a change in a creatinine-based electronic alert. Kidney Int 92(2):432–439
Chawla LS, Bellomo R, Bihorac A, Goldstein SL, Siew ED, Bagshaw SM et al (2017) Acute kidney disease and renal recovery: consensus report of the Acute Disease Quality Initiative (ADQI) 16 Workgroup. Nat Rev Nephrol 13(4):241–257
Schwartz GJ, Muñoz A, Schneider MF, Mak RH, Kaskel F, Warady BA et al (2009) New equations to estimate GFR in children with CKD. J Am Soc Nephrol JASN 20(3):629–637
Kapur G, Valentini RP, Imam AA, Mattoo TK (2009) Treatment of severe edema in children with nephrotic syndrome with diuretics alone–a prospective study. Clin J Am Soc Nephrol CJASN 4(5):907–913
Fujita H, Shinjoh M, Ishii T, Awazu M (2016) Utility of fractional excretion of urea in the differential diagnosis of acute kidney injury in children. Pediatr Nephrol Berl Ger 31(8):1349–1353
Moffett BS, Goldstein SL (2011) Acute kidney injury and increasing nephrotoxic-medication exposure in noncritically-ill children. Clin J Am Soc Nephrol CJASN 6(4):856–863
Thomas ME, Blaine C, Dawnay A, Devonald MAJ, Ftouh S, Laing C et al (2015) The definition of acute kidney injury and its use in practice. Kidney Int 87(1):62–73
Menon S (2018) Acute kidney injury in nephrotic syndrome. Front Pediatr 6:428
Bohlin AB (1984) Clinical course and renal function in minimal change nephrotic syndrome. Acta Paediatr Scand 73(5):631–636
Berg U, Bohlin AB (1982) Renal hemodynamics in minimal change nephrotic syndrome in childhood. Int J Pediatr Nephrol 3(3):187–192
Bohman SO, Jaremko G, Bohlin AB, Berg U (1984) Foot process fusion and glomerular filtration rate in minimal change nephrotic syndrome. Kidney Int 25(4):696–700
Koomans HA (2001) Pathophysiology of acute renal failure in idiopatic nephrotic syndrome. Nephrol Dial Transplant Off Publ Eur Dial Transpl Assoc Eur Ren Assoc 16(2):221–224
Venkataseshan VS, Faraggiana T, Grishman E, Marquet E, Churg J (1993) Renal failure due to tubular obstruction by large protein casts in patients with massive proteinuria. Clin Nephrol 39(6):321–326
Lowenstein J, Schacht RG, Baldwin DS (1981) Renal failure in minimal change nephrotic syndrome. Am J Med 70(2):227–233
Sakarcan A, Timmons C, Seikaly MG (1994) Reversible idiopathic acute renal failure in children with primary nephrotic syndrome. J Pediatr 125(5 Pt 1):723–727
Chen T, Lv Y, Lin F, Zhu J (2011) Acute kidney injury in adult idiopathic nephrotic syndrome. Ren Fail 33(2):144–149
Wang F, Ding J (2021) Pediatric acute kidney injury to the subsequent CKD transition. Kidney Dis Basel Switz 7(1):10–13
Meena J, Bagga A (2020) Current perspectives in management of edema in nephrotic syndrome. Indian J Pediatr 87(8):633–640
Acknowledgements
We would like to acknowledge the contribution of Dr. Sayantani Roy Choudhury (statistician) for her help with the statistics.
Author information
Authors and Affiliations
Contributions
RS conceptualized the project. RS, SG, SP, and RP were involved in obtaining ethics approval. RS, SG, DD, SP, SS, and RP were involved in patient recruitment. All the authors were involved in result analysis and manuscript preparation. The manuscript was reviewed by all of them (applicable for submissions with multiple authors).
Corresponding author
Ethics declarations
Ethical approval
Institutional ethics committee approval was granted (IEC/208/2020).
Conflict of interest
The authors declare no competing interests.
Additional information
Communicated by Gregorio Milani.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
431_2023_4903_MOESM1_ESM.png
Supplement Fig. 1: Variance Inflation Factor (VIF) table to check multicollinearity showed all values of VIF to be less than two suggesting no confounding factors. (PNG 34 KB)
431_2023_4903_MOESM2_ESM.doc
Supplement Table 1: Overview of studies published in English literature exploring incidence of AKI in childhood nephritic syndrome (DOC 48 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ghosh, S., Akhtar, S., Pradhan, S.K. et al. Incidence and risk factors of acute kidney injury among childhood nephrotic syndrome: a prospective cohort study. Eur J Pediatr 182, 2443–2451 (2023). https://doi.org/10.1007/s00431-023-04903-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-023-04903-7