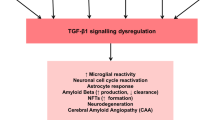
Abstract
Tubulin-associated unit (tau) is an important microtubule-associated protein. The abnormal intracellular aggregation of tau has been strongly associated with Alzheimer's disease (AD). Accumulating evidence has conclusively demonstrated that tau is present in the cytoplasm of neurons and is also actively released into the extracellular space. However, the types of tau species that are released are unclear, as is the mechanism of their release by donor neurons and subsequent uptake by recipient neurons in AD. Understanding the underlying mechanisms of abnormal tau cell-to-cell transmission can provide novel insights into the etiology and pathogenesis of AD and can help identify new targets for the development of AD therapies focused on counteracting neurodegeneration or even preventing it. From this perspective, the present review focuses on recent advances in understanding the mechanisms regulating the levels of extracellular tau and discusses the role of such mechanisms in the propagation of tau-associated pathology.

Similar content being viewed by others
Availability of data and material
All articles referenced in this review are available.
Abbreviations
- AD:
-
Alzheimer's disease
- CSF:
-
Cerebrospinal fluid
- EV:
-
Extracellular vesicle
- MT:
-
Microtubule
- NFT:
-
Neurofibrillary tangle
- PHF:
-
Paired helical filaments
- PM:
-
Plasma membrane
- PTM:
-
Post-translational modification
- Tau:
-
Tubulin-associated unit
- TNTs:
-
Tunneling nanotubes
References
Dotti CG, Banker GA, Binder LI (1987) The expression and distribution of the microtubule-associated proteins tau and microtubule-associated protein 2 in hippocampal neurons in the rat in situ and in cell culture. Neuroscience 23:121–130
Brunello CA, Merezhko M, Uronen R-L, Huttunen HJ (2020) Mechanisms of secretion and spreading of pathological tau protein. Cell Mol Life Sci 77:1721–1744
LoPresti P, Szuchet S, Papasozomenos SC et al (1995) Functional implications for the microtubule-associated protein tau: localization in oligodendrocytes. Proc Natl Acad Sci 92:10369–10373
Pooler AM, Noble W, Hanger DP (2014) A role for tau at the synapse in Alzheimer’s disease pathogenesis. Neuropharmacology 76:1–8
Slachevsky A, Guzmán-Martínez L, Delgado C et al (2017) Tau platelets correlate with regional brain atrophy in patients with Alzheimer’s disease. J Alz Dis 55:1595–1603
Goedert M, Spillantini MG, Jakes R, Rutherford D, Crowther RA (1989) Multiple isoforms of human microtubule-associated protein tau: sequences and localization in neurofibrillary tangles in Alzheimer’s disease. Neuron 3:519–526
Qian W, Liu F (2014) Regulation of alternative splicing of tau exon 10. Neurosci Bull 30:367–377
Pampuscenko K, Morkuniene R, Krasauskas L, Smirnovas V, Tomita T, Borutaite V (2021) Distinct neurotoxic effects of extracellular tau species in primary neuronal-glial cultures. Mol Neurobiol 58:658–667
Schöll M, Maass A, Mattsson N, Ashton NJ, Blennow K, Zetterberg H, Jagust W (2019) Biomarkers for tau pathology. Mol Cell Neurosci 97:18–33
Violet M, Delattre L, Tardivel M et al (2014) A major role for Tau in neuronal DNA and RNA protection in vivo under physiological and hyperthermic conditions. Front Cell Neurosci 8:84
Sultan A, Nesslany F, Violet M et al (2011) Nuclear tau plays a key role in neuronal DNA protection. J Biol Chem 286:4566–4675
Fuster-Matanzo A, Hernández F, Ávila J (2018) Tau spreading mechanisms; implications for dysfunctional tauopathies. Int J Mol Sci 19:645
Avila J, Lucas JJ, Perez M, Hernandez F (2004) Role of tau protein in both physiological and pathological conditions. Physiol Rev 84:361–384
Dujardin S, Bégard S, Caillierez R et al (2018) Different tau species lead to heterogeneous tau pathology propagation and misfolding. Acta Neuropathol Microbiol 6:132
Hu W, Wu F, Zhang Y, Gong C-X, Iqbal K, Liu F (2017) Expression of tau pathology-related proteins in different brain regions: a molecular basis of tau pathogenesis. Front Aging Neurosci 9:311
Schweers O, Mandelkow EM, Biernat J, Mandelkow E (1995) Oxidation of cysteine-322 in the repeat domain of microtubule-associated protein tau controls the in vitro assembly of paired helical filaments. Proc Natl Acad Sci USA 92:8463–8467
Schoch KM, DeVos SL, Miller RL et al (2016) Increased 4R-Tau induces pathological changes in a human-tau mouse model. Neuron 90:941–947
Tuerde D, Kimura T, Miyasaka T et al (2018) Isoform-independent and -dependent phosphorylation of microtubule-associated protein tau in mouse brain during postnatal development. J Biol Chem 293:1781–1793
Bunker JM, Wilson L, Jordan MA, Feinstein SC (2004) Modulation of microtubule dynamics by tau in living cells: implications for development and neurodegeneration. Mol Biol Cell 15:2720–2728
Barghorn S, Mandelkow E (2002) Toward a unified scheme for the aggregation of tau into Alzheimer paired helical filaments. Biochemistry 41:14885–14896
Karch CM, Jeng AT, Goate AM (2012) Extracellular tau levels are influenced by variability in tau that is associated with tauopathies. J Biol Chem 287:42751–42762
Stoothoff W, Jones PB, Spires-Jones TL et al (2009) Differential effect of three-repeat and four-repeat tau on mitochondrial axonal transport. J Neurochem 111:417–427
Goedert M, Spillantini MG, Potier MC, Ulrich J, Crowther RA (1989) Cloning and sequencing of the cDNA encoding an isoform of microtubule-associated protein tau containing four tandem repeats: differential expression of tau protein mRNAs in the human brain. EMBO J 8:393–399
Morris M, Knudsen GM, Maeda S, Trinidad JC, Ioanoviciu A, Burlingame AL (2015) Tau post-translational modifications in wild-type and human amyloid precursor protein transgenic mice. Nat Neurosci 18:1183–1189
Mandelkow EM, Mandelkow E (2012) Biochemistry and cell biology of tau protein in neurofibrillary degeneration. Cold Spring Harb Perspect Med 2:a006247
Yuzwa SA, Cheung AH, Okon M, McIntosh LP, Vocadlo DJ (2014) O-GlcNAc modification of tau directly inhibits its aggregation without perturbing the conformational properties of tau monomers. J Mol Biol 426:1736–1752
Sohn PD, Tracy TE, Son HI, Zhou Y, Leite RE, Miller BL, Seeley WW, Grinberg LT, Gan L (2016) Acetylated tau destabilizes the cytoskeleton in the axon initial segment and is mislocalized to the somatodendritic compartment. Mol Neurodegener 11:47
Kolarova M, García-Sierra F, Bartos A, Ricny J, Ripova D (2012) Structure and pathology of tau protein in Alzheimer disease. Int J Alzheimers Dis 2012:731526
Min SW, Cho SH, Zhou Y et al (2010) The acetylation of tau inhibits its degradation and contributes to tauopathy. Neuron 67:953–966
Trzeciakiewicz H, Tseng JH, Wander CM, Madden V, Tripathy A, Yuan CX, Cohen TJ (2017) A dual pathogenic mechanism links tau acetylation to sporadic tauopathy. Sci Rep 7:44102
Cohen TJ, Guo JL, Hurtado DE, Kwong LK, Mills IP, Trojanowski JQ, Lee VM (2011) The acetylation of tau inhibits its function and promotes pathological tau aggregation. Nat Commun 2:252
Thomas SN, Funk KE, Wan Y et al (2012) Dual modification of Alzheimer’s disease PHF-tau protein by lysine methylation and ubiquitylation: A mass spectrometry approach. Acta Neuropathol 123:105–117
Watanabe T, Ihara N, Itoh T, Fujita T, Sugimoto Y (2000) Deletion mutation in Drosophila ma-l homologous, putative molybdopterin cofactor sulfurase gene is associated with bovine xanthinuria type II. J Biol Chem 275:21789–21792
Ledesma MD, Bonay P, Avila J (1995) Tau protein from Alzheimer’s disease patients is glycated at its tubulin-binding domain. J Neurochem 65:1658–1664
Necula M, Kuret J (2004) Pseudophosphorylation and glycation of tau protein enhance but do not trigger fibrillization in vitro. J Biol Chem 279:49694–49703
Funk KE, Thomas SN, Schafer KN, Cooper GL, Liao Z, Clark DJ, Yang AJ, Kuret J (2014) Lysine methylation is an endogenous post-translational modification of tau protein in human brain and a modulator of aggregation propensity. Biochem J 462:77–88
Reynolds MR, Lukas TJ, Berry RW, Binder LI (2006) Peroxynitrite-mediated tau modifications stabilize preformed filaments and destabilize microtubules through distinct mechanisms. Biochemistry 45:4314–4326
Cappelletti G, Tedeschi G, Maggioni MG, Negri A, Nonnis S et al (2004) Nitration of tau protein in neuron-like PC12 cells. FEBS Lett 562:35–39
Reynolds MR, Berry RW, Binder LI (2005) Site-specific nitration differentially influences tau assembly in vitro. Biochemistry 44:13997–14009
Reyes JF, Fu Y, Vana L, Kanaan NM, Binder LI (2011) Tyrosine nitration within the proline-rich region of tau in Alzheimer’s disease. Am J Pathol 178:2275–2285
Liu F, Iqbal K, Grundke-Iqbal I, Hart GW, Gong CX (2004) O-GlcNAcylation regulates phosphorylation of tau, a mechanism involved in Alzheimer’s disease. Proc Natl Acad Sci USA 101:10804–10809
Marcus JN, Schachter J (2011) Targeting post-translational modifications on tau as a therapeutic strategy for Alzheimer’s disease. J Neurogenet 25:127–133
Simić G, Diana A, Hof PR (2003) Phosphorylation pattern of tau associated with distinct changes in the growth cone cytoskeleton. Prog Mol Subcell Biol 32:33–48
Lee S, Shea TB (2012) Caspase-mediated truncation of Tau potentiates aggregation. Int J Alzheimers Dis 2012:731063
Jarero-Basulto JJ, Luna-Muñoz J, Mena R, Kristofikova Z, Ripova D, Perry G, Binder LI, Garcia-Sierra F (2013) Proteolytic cleavage of polymeric tau protein by caspase-3: implications for Alzheimer disease. J Neuropathol Exp Neurol 72:1145–11461
Nakamura K, Zhen Zhou X, Ping LuK (2013) Cis phosphorylated tau as the earliest detectable pathogenic conformation in Alzheimer’s disease, offering novel diagnostic and therapeutic strategies. Prion 7:117–120
Martin L, Latypova X, Terro F (2011) Post-translational modifications of tau protein: implications for Alzheimer’s disease. Neurochem Int 58:458–471
Nakamura K, Greenwood A, Binder L, Bigio EH, Denial S, Nicholson L, Zhou XZ, Lu KP (2012) Proline isomer-specific antibodies reveal the early pathogenic tau conformation in Alzheimer’s disease. Cell 149:232–244
Biernat J, Wu YZ, Timm T, Zheng-Fischhöfer Q, Mandelkow E, Meijer L, Mandelkow EM (2002) Protein kinase MARK/PAR-1 is required for neurite outgrowth and establishment of neuronal polarity. Mol Biol Cell 13:4013–4028
Biernat J, Mandelkow EM (1999) The development of cell processes induced by tau protein requires phosphorylation of serine 262 and 356 in the repeat domain and is inhibited by phosphorylation in the proline-rich domains. Mol Biol Cell 10:727–740
Hanger DP, Anderton BH, Noble W (2009) Tau phosphorylation: the therapeutic challenge for neurodegenerative disease. Trends Mol Med 15:112–119
Dorval V, Fraser PE (2006) Small ubiquitin-like modifier (SUMO) modification of natively unfolded proteins tau and alpha-synuclein. J Biol Chem 281:9919–9924
Luo HB, Xia YY, Shu XJ et al (2014) SUMOylation at K340 inhibits tau degradation through deregulating its phosphorylation and ubiquitination. Proc Natl Acad Sci USA 111:16586–16591
Derisbourg M, Leghay C, Chiappetta G et al (2015) Role of the Tau N-terminal region in microtubule stabilization revealed by new endogenous truncated forms. Sci Rep 5:9659
Zhao X, Kotilinek LA, Smith B, Hlynialuk C, Zahs K, Ramsden M, Cleary J, Ashe KH (2016) Caspase-2 cleavage of tau reversibly impairs memory. Nat Med 22:1268–1276
Zabik NL, Imhof MM, Martic-Milne M (2017) Structural evaluations of tau protein conformation: methodologies and approaches. Biochem Cell Biol 95:338–349
Dickey CA, Yue M, Lin WL et al (2006) Deletion of the ubiquitin ligase CHIP leads to the accumulation, but not the aggregation, of both endogenous phospho- and caspase-3-cleaved tau species. J Neurosci 26:6985–6996
Petrucelli L, Dickson D, Kehoe K et al (2004) CHIP and Hsp70 regulate tau ubiquitination, degradation and aggregation. Hum Mol Genet 13:703–714
Morishima-Kawashima M, Hasegawa M, Takio K, Suzuki M, Titani K, Ihara Y (1993) Ubiquitin is conjugated with amino-terminally processed tau in paired helical filaments. Neuron 10:1151–1160
Huseby CJ, Hoffman CN, Cooper GL et al (2019) Quantification of tau protein lysine methylation in aging and Alzheimer’s disease. J Alzheimers Dis 71:979–991
Braak H, Braak E (1996) Development of Alzheimer-related neurofibrillary changes in the neocortex inversely recapitulates cortical myelogenesis. Acta Neuropathol 92:197–201
Oudart J-B, Zucchini L, Maquart F-X et al (2017) Tau protein as a possible marker of cerebrospinal fluid leakage in cerebrospinal fluid rhinorrhea: a pilot study. Biochem Med (Zagreb) 27:030703
Zetterberg H (2017) Review: Tau in biofluids - relation to pathology, imaging, and clinical features. Neuropathol Appl Neurobiol 43:194–199
Chai X, Dage JL, Citron M (2012) Constitutive secretion of tau protein by an unconventional mechanism. Neurobiol Dis 48:356–366
Kanmert D, Cantlon A, Muratore CR et al (2015) C-terminally truncated forms of tau, but not full-length tau or its C-terminal fragments, are released from neurons independently of cell death. J Neurosci 35:10851–10865
Yamada K, Patel TK, Hochgräfe K, Mahan TE, Jiang H, Stewart FR, Mandelkow EM, Holtzman DM (2015) Analysis of in vivo turnover of tau in a mouse model of tauopathy. Mol Neurodegener 10:55
Janelidze S, Stomrud E, Smith R et al (2020) Cerebrospinal fluid p-tau217 performs better than p-tau181 as a biomarker of Alzheimer’s disease. Nat Commun 11:683
Majerova P, Zilkova M, Kazmerova Z, Kovac A, Paholikova K, Kovacech B, Zilka N, Novak M (2014) Microglia display modest phagocytic capacity for extracellular tau oligomers. J Neuroinflammation 11:161
Goedert M (2016) The ordered assembly of tau is a gain-of-toxic function that causes human tauopathies. Alzheimers Dement 12:1040–1050
Weismiller WA, Murphy R, Wei G, Ma B, Nussinov R, Margittai M (2018) Structural disorder in four-repeat tau fibrils reveals a new mechanism for barriers to cross-seeding of Tau isoforms. J Biol Chem 293:17336–17348
Falcon B, Cavallini A, Angers R et al (2015) Conformation determines the seeding potencies of native and recombinant Tau aggregates. J Biol Chem 290:1049–1065
Pooler AM, Phillips EC, Lau DH, Noble W, Hanger DP (2013) Physiological release of endogenous tau is stimulated by neuronal activity. EMBO Rep 14:389–394
Wang Y, Mandelkow E (2016) Tau in physiology and pathology. Nat Rev Neurosci 17:5–21
Yamada K, Holth JK, Liao F et al (2014) Neuronal activity regulates extracellular tau in vivo. J Exp Med 211:387–393
Plouffe V, Mohamed NV, Rivest-McGraw J, Bertrand J, Lauzon M, Leclerc N (2012) Hyperphosphorylation and cleavage at D421 enhance tau secretion. PLoS ONE 7:e36873
Bright J, Hussain S, Dang V et al (2015) Human secreted tau increases amyloid-beta production. Neurobiol Aging 36:693–709
Dujardin S, Bégard S, Caillierez R et al (2014) Ectosomes: a new mechanism for non-exosomal secretion of tau protein. PLoS ONE 9:e100760
Mohamed N-V, Desjardins A, Leclerc N (2017) Tau secretion is correlated with an increase in Golgi dynamics. PLoS ONE 12:e0178288
Shanya Jiang S, Bhaskar K (2020) Degradation and transmission of tau by autophagic-endolysosomal networks and potential therapeutic targets for tauopathy. Front Mol Neurosci 16:586731
Saman S, Kim W, Raya M et al (2012) Exosome-associated tau is secreted in tauopathy models and is selectively phosphorylated in cerebrospinal fluid in early Alzheimer disease. J Biol Chem 287:3842–3849
Merezhko M, Uronen R-L, Huttunen HJ (2020) The cell biology of tau secretion. Front Mol Neurosci 13:569818
Rustom A, Saffrich R, Markovic I, Walther P, Gerdes HH (2004) Nanotubular highways for intercellular organelle transport. Science 303:1007–1010
Dujardin S, Lécolle K, Caillierez R et al (2014) Neuron-to-neuron wild-type Tau protein transfer through a trans-synaptic mechanism: relevance to sporadic tauopathies. Acta Neuropathol Microbiol 2:14
Sokolow S, Henkins KM, Bilousova T et al (2015) Presynaptic C-terminal truncated tau is released from cortical synapses in Alzheimer’s disease. J Neurochem 133:368–379
Farfel JM, Yu L, De Jager PL, Schneider JA, Bennett DA (2016) Association of APOE with tau-tangle pathology with and without β-amyloid. Neurobiol Aging 37:19–25
Meraz-Ríos MA, Lira-De León KI, Campos-Peña V, De Anda-Hernández MA, Mena-López R (2010) Tau oligomers and aggregation in Alzheimer’s disease. J Neurochem 112:1353–1267
Uchihara T (2020) Neurofibrillary changes undergoing morphological and biochemical changes: How does tau with the profile shift of from four repeats to three repeats spread in the Alzheimer’s brain? Neuropathology 40:450–459
Mroczko B, A, (2019) The role of protein misfolding and tau oligomers (tauOs) in Alzheimer’s disease (AD). Int J Mol Sci 20:4661
Cárdenas-Aguayo Mdel C, Gómez-Virgilio L, DeRosa S, Meraz-Ríos MA (2014) Role of tau oligomers in the onset of Alzheimer’s disease neuropathology. ACS Chem Neurosci 5:1178–1191
Shafiei SS, Guerrero-Muñoz MJ, Castillo-Carranza DL (2017) Tau oligomers: cytotoxicity, propagation, and mitochondrial damage. Front Aging Neurosci 9:83
Grundke-Iqbal I, Iqbal K, Quinlan M, Tung YC, Zaidi MS, Wisniewski HM (1986) Microtubule-associated protein tau A component of Alzheimer’s paired helical filaments. J Biol Chem 261:6084–6089
Wischik CM, Schelter BO, Wischik DJ, Storey JMD, Harrington CR (2018) Modeling prion-like processing of tau protein in Alzheimer’s disease for pharmaceutical development. J Alzheimers Dis 62:1287–1303
Goedert M, Jakes R (1990) Expression of separate isoforms of human tau protein: correlation with the tau pattern in brain and effects on tubulin polymerization. EMBO J 9:4225–4230
Mukaetova-Ladinska EB, Garcia-Siera F, Hurt J et al (2000) Staging of cytoskeletal and beta-amyloid changes in human isocortex reveals biphasic synaptic protein response during progression of Alzheimer’s disease. Am J Pathol 157:623–636
Wharton SB, Minett T, Drew D et al (2016) Epidemiological pathology of Tau in the aging brain: application of staging for neuropil threads (BrainNet Europe protocol) to the MRC cognitive function and aging brain study. Acta Neuropathol Microbiol 4:11
Ahmed Z, Cooper J, Murray TK et al (2014) A novel in vivo model of tau propagation with rapid and progressive neurofibrillary tangle pathology: the pattern of spread is determined by connectivity, not proximity. Acta Neuropathol 127:667–683
Kidd M (1963) Paired helical filaments in electron microscopy of Alzheimer’s disease. Nature 197:192–193
Ballatore C, Lee VM-Y, Trojanowski JQ (2007) Tau-mediated neurodegeneration in Alzheimer’s disease and related disorders. Nat Rev Neurosci 8:663–672
Nilson AN, English KC, Gerson JE et al (2017) Tau oligomers associate with inflammation in the brain and retina of tauopathy mice and in neurodegenerative diseases. J Alzheimers Dis 55:1083–1099
Seppala TT, Koivisto AM, Hartikainen P, Helisalmi S, Soininen H, Herukka SK (2011) Longitudinal changes of CSF biomarkers in Alzheimer’s disease. J Alzheimers Dis 25:583–594
Morozova V, Cohen LS, El-Hadi Makki A, Shur A, Pilar G, El Idrissi A, Alonso AD (2019) Normal and pathological tau uptake mediated by M1/M3 muscarinic receptors promotes opposite neuronal changes. Front Cell Neurosci 13:403
Wu JW, Herman M, Liu L et al (2013) Small misfolded Tau species are internalized via bulk endocytosis and anterogradely and retrogradely transported in neurons. J Biol Chem 288:1856–1870
Ruan Z, Pathak D, Kalavai SV et al (2021) Alzheimer’s disease brain-derived extracellular vesicles spread tau pathology in interneurons. Brain 144:288–309
DeVos SL, Corjuc BT, Oakley DH, Nobuhara CK, Bannon RN, Chase A, Commins C, Gonzalez JA, Dooley PM, Frosch MP, Hyman BT (2018) Synaptic tau seeding precedes tau pathology in human alzheimer’s disease brain. Front Neurosci 12:267
Tardivel M, Bégard S, Bousset L, Dujardin S, Coens A, Melki R, Buée L, Colin M (2016) Tunneling nanotube (TNT)-mediated neuron-to neuron transfer of pathological Tau protein assemblies. Acta Neuropathol Commun 4:117
Merezhko M, Brunello CA, Yan X, Vihinen H, Jokitalo E, Uronen R-L, Huttunen HJ (2018) Secretion of tau via an unconventional non-vesicular mechanism. Cell Rep 25:2027–2035
Pérez M, Avila J, Hernández F (2019) Propagation of tau via extracellular vesicles. Front Neurosci 13:698
Falcon B, Noad J, McMahon H, Randow F, Goedert M (2018) Galectin-8–mediated selective autophagy protects against seeded tau aggregation. J Biol Chem 293:2438–2451
Evans LD, Wassmer T, Fraser G, Smith J, Perkinton M, Billinton A, Livesey FJ (2018) Extracellular monomeric and aggregated tau efficiently enter human neurons through overlapping but distinct pathways. Cell Rep 22:3612–3624
Holmes BB, DeVos SL, Kfoury N et al (2013) Heparan sulfate proteoglycans mediate internalization and propagation of specific proteopathic seeds. Proc Natl Acad Sci USA 110:E3138–E3147
Narasimhan S, Changolkar L, Riddle DM et al (2020) Human tau pathology transmits glial tau aggregates in the absence of neuronal tau. J Exp Med 217:e20190783
Narasimhan S, Guo JL, Changolkar L, Stieber A, McBride JD, Silva LV, He Z, Zhang B, Gathagan RJ, Trojanowski JQ, Lee VMY (2017) Pathological tau strains from human brains recapitulate the diversity of tauopathies in nontransgenic mouse brain. J Neurosci 37:11406–11423
Reid MJ, Beltran-Lobo P, Johnson L, Perez-Nievas BG, Noble W (2020) Astrocytes in Tauopathies. Front Neurol 11:572850
Asai H, Ikezu S, Tsunoda S, Medalla M, Luebke J, Haydar T, Wolozin B, Butovsky O, Kügler S, Ikezu T (2015) Depletion of microglia and inhibition of exosome synthesis halt tau propagation. Nat Neurosci 18:1584–1593
Funding
The authors gratefully acknowledge the financial support provided by the Beijing Science and Technology Planning Project (grant number No. Z171100001017106) and the National Natural Science Foundation of China (No. 81904194).
Author information
Authors and Affiliations
Contributions
As the co-first author, Yun Wei and Meixia Liu wrote the manuscript. Dongxin Wang helped with initial writing. Yun Wei edited and revised the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no competing interests.
Ethics approval and consent to participate
This article is a review and does not involve human or animal specimens.
Consent to publish
All authors gave their consent for the publishing of the manuscript.
Rights and permissions
About this article
Cite this article
Wei, Y., Liu, M. & Wang, D. The propagation mechanisms of extracellular tau in Alzheimer’s disease. J Neurol 269, 1164–1181 (2022). https://doi.org/10.1007/s00415-021-10573-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-021-10573-y