Abstract
Purpose
To review the current data on retrograde ejaculation (RE) and ejaculatory dysfunction (EjD) after endoscopic and minimally invasive surgical treatment of benign prostatic obstruction (BPO) and, their perceived impact in the quality of life (QoL) and sexual life of patients and their partners.
Methods
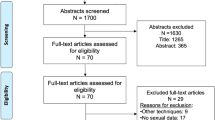
Narrative review of systematic reviews (SR) assessing comparative rates of RE, EjD or erectile dysfunction (EF) was carried out. Relevant articles on the prevalence of RE, EjD or EF and on their impact in the QoL or sexual life of patients and partners were manually selected based on relevance.
Results
Twelve SRs reporting on comparisons of different endoscopic/minimally invasive treatments of BPO were found. Data on outcomes varied widely. Overall, after conventional TURP or laser techniques 42–75% of patients present RE. Prostatic incision and ablative procedures present lowest rates of de novo RE or EjD whereas laser adenomectomy and ejaculation preservation procedures preserve antegrade ejaculation in 46–68% of patients. EjDs is associated to LUTS and present in 10% of sexualy active men before intervention. It modulates the QoL and sexual life of the couple. In spite of the scarce literature assessing patient’s and partner’s perception of postoperative EjD, it strongly suggests that both parties value the maintenance of the ejaculatory function.
Conclusion
Ejaculation-preserving techniques and minimally invasive techniques successfully prevent BPO treatment-induced RE or EjD in 70–100% of the cases. While this is appealing to patients and spouses, technique selection and treatment durability are issues to be discussed with the couple.
Similar content being viewed by others
References
Drake M, Lewis AL, Younbg GJ et al (2020) Diagnostic assessment of lower urinary tract symptoms in men considering prostate surgery: a noninferiority randomized controlled trial or urodynamics in 26 hospitals. Eur Urol 78:701–710
Gravas S, Cornu JN, Gacci M et al (2020) Management of non-neurogenic male LUTS. EAU Guidelines. http://uroweb.org/guideline/treatmetn-of-non-neurogenic-male-luts/ Accessed 2nd Dec 2020. ISBN 978-94-92671-07-3
Madersbacher S, Marberger M (1999) Is transurethral resection of the prostate still justified? BJU Int 83:227–237
Parsons KJ, Barry MJ, Dahm P et al (2020) AUA Guideline on the management of benign prostatic hyperplasia: surgical management of benign prostatic hyperplasia/lower urinary tract symptoms (2018, amended 2019, 2020). http://auanet.org/ Accessed 2nd Dec 2020
Alloussi SH, Lang C, Eichel R, Alloussi S (2014) Ejaculation-preserving transurethral resection of prostate and bladder neck: short- and long-term results of a new innovative resection technique. J Endourol 28(1):84–89
De Lay KJ, Nutt M, McVary KT (2016) Ejaculatory dysfunction in the treatment of lower urinary tract symptoms. Transl Androl Urol 5:450–459
Rosen R, Altwein J, Boyle P et al (2003) Lower urinary tract symptoms and male sexual dysfunction: the multinational survey of the aging male (MSAM-7). Eur Urol 44:637–649
Rowland DC, McMahon G, Abdo C, Chen J, Jannini E, Waldinger MD, Ahn TY (2010) Disorders of orgasm and ejaculation in men. J Sex Med 7:1668–1686
Cacciamani GE, Cuhna F, Tafuri A et al (2019) Anterograde ejaculation preservation after endoscopic treatments in patients with bladder outlet obstruction: systematic review and pooled-analysis of randomized clinical trials. Minerva Urol Nefrol 71:427–434
Marra G, Sturch P, Oderda M, Tabatabaei S, Muir G, Gontero P (2016) Systematic review of lower urinary tract symptoms/benign prostatic hyperplasia surgical treatments on men’s ejaculatory function: time for a bespoke approach? Int J Urol 23:22–35
Lebdai A, Chevrot A, Doizi S et al (2019) Do patients have to choose between ejaculation and miction? A systematic review about ejaculation preservation technics for benign prostatic obstruction surgical treatment. WJU 37:299–308
Lai S, Peng P, Diao T et al (2019) Comparison of photoselective green light laser vaporisation versus traditional transurethral resection for benign prostate hyperplasia: an updated systematic review and meta-analysis of randomised controlled trials and prospective studies. BMJ Open 9:e028855
Zong HT, Peng X-X, Yang CC, Zhang Y (2012) The impact of transurethral procedures for benign prostate hyperplasia on male sexual function: a meta-analysis. J Androl 33:427–434
Frieben RW, Lin HC, Hinh PP, Berardinelli F, Canfield SE, Wang R (2010) The impact of minimally invasive surgeries for the treatment of symptomatic benign prostatic hyperplasia on male sexual function: a systematic review. Asian J Androl 12:500–508
Liu Y, Cheng Y, Zhuo L et al (2020) Impact on sexual function of endoscopic enucleation vs transurethral resection of the prostate for lower urinary tract symptoms due to benign prostatic hyperplasia: a systematic review and meta-analysis. J Endourol 34:1064–1074
Cornu JN, Ahyai S, Bachmann A et al (2015) A systematic review and meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic obstruction: an update. Eur Urol 67:1066–1096
DeCao H, Wang J, Huang Y et al (2015) Comparison between thulium laser resection of prostate and transurethral plasmakinetic resection of prostate or transurethral resection of prostate. Sci Rep 5:14542
Sun F, Sun X, Shi Q, Zhai Y (2018) Transurethral procedures in the treatment of benign prostatic hyperplasia a systematic review and meta-analysis of effectiveness and complications. Medicine (Baltimore) 97(51):e13360
Yang Q, Peters TJ, Donovan JL, Wilt TJ, Abrams P (2001) Transurethral incision compared with transurethral resection of the prostate for bladder outlet obstruction: a systematic review and meta-analysis of randomized controlled trials. J Urol 165:1526–1532
Lokeshwar SD, Valancy D, Lima TFN, Braun RB, Ramasamy R (2020) A systematic review of reported ejaculatory dysfunction in clinical trials evaluating minimally invasive treatment modalities for BPH. Curr Urol Rep 21:1–10
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A (1997) The International index of erectile function IIEF: a multidimensional scale for assessment of erectile dysfunction. Urology 49:822–830
Rosen RC, Catania J, Pollack L, Althof S, O’Leary M, Seftel AD (2004) Male Sexual Health Questionnaire (MSHQ): scale development anf psychometric validation. Urology 64:777–782
Bouhadana D, Nguyen DD, Zorn KC, Elterman DS, Bhojani N (2020) Patient perspectives on benign prostatic hyperplasia surgery: a focus on sexual health. J Sex Med 17(2108):e2112
Paduch DA, Polzer P, Morgentaler A et al (2015) Clinical and demographic correlates of ejaculatory dysfunctions other than premature ejaculation: a prospective observational study. J Sex Med 12:2276–2286
Rosen RC, Fitzpatrick JM, for the ALF-LIFE Study Group (2009) Urinary tract symptoms suggestive of benign prostatic hyperplasia. BJUI 104:974–983
Chitali S, Collins R, Hull S, Smith E, Irving S (2007) Is the current practice providing an integrated approach to the management of LUTS and ED in primary care? An audit and literature review. J Sex Med 4(6):1713–2172. https://doi.org/10.1111/j.1743-6109.2007.00598.x
Donovan JL, Peters TJ, Neal DE et al (2000) A randomized trial comparing transurethral resection of the prostate, laser therapy and conservative treatment of men with symptoms associated with benign prostatic enlargement: the CLasP study. J Urol 164:65–70
Coyne KS, Sexton CC, Thompson CL, Milsom I, Irwin D, Kopp ZS, Aiyer LP (2009) The prevalence of lower urinary tract symptoms (LUTS) in the USA, the UK and Sweden: results from the epidemiology of LUTS (EpiLUTS) study. BJU Int 104(3):352–360
Wein AJ, Coyne KS, Tubaro A, Sexton CC, Kopp ZS, Aiyer LP (2009) The impact of lower urinary tract symptoms on male sexual health: EpiLUTS. BJU Int 103(s3):33–41
Brookes ST, Donovan JL, Peters TJ, Abrams P, Neal DE et al (2002) Sexual dysfunction in men after treatment for lower urinary tract symptom: evidence from randomized controlled trial. BMJ 324:1–6
Nottingham CU, Agarwal DK, Valadon C, Large T, Rivera ME, Krambeck AE (2020) Correlating patient anxiety with urinary symptoms before and after holmium laser enucleation of the prostate. J Endourol 34:782–787
Kim JK, Cho MC, Son H, Ku JH, Oh SJ, Paick JS (2017) Patient perception of ejaculatory volume reduction after holmium laser eznucleation of the prostate (HoLEP). Urology 99:142–147
Mitropoulos D, Anastasiou I, Giannopoulou C et al (2002) Symptomatic benign prostate hyperplasia: impact on partners’ quality of life. Eur Urol 41:240–245
Kim SC, Lee SY (2009) Men’s lower urinary tract symptoms are also mental and physcal sufferings for their spouses. J Korean Med Sci 24:320–325
Roehrborn CG, Marks L, Harkaway R (2006) Enlarged prostate: A landmark national survey of its prevalence and impact on US men and their partners. Prostate Cancer Prostatic Dis 9(1):30–34
Rosen RC, Heiman JR, Long JS, Fisher WA, Sand MS (2016) Men with sexual problems and their partners: findings from the international survey of relationships. Arch Sex Behav 45:159–173
Burri A, Buchmeier J, Porst H (2018) The importance of male ejaculation for female sexual satisfaction and function. J Sex Med 15:1600–1608
Briganti A, Naspro R, Gallina A et al (2006) Impact on sexual function of holmium laser enucleation versus transurethral resection of the prostate: results of a prospective, 2-center randomized trial. J Urol 175:1817–1821
Kasman AM, Bhambhvani HP, Eisenberg ML (2020) Ejaculatory dysfunction in patients presenting to a men’s health clinic: a retrospective cohort study. J Sex Med 8:454–550
Cho MC, Kim JK, Song SH et al (2018) Patient-reported ejaculatory function and satisfaction in men with lower urinary tract symptoms/benign prostatic hyperplasia. Asian J Androl 20:69–74
Hellstrom WJ, Giuliano F, Rosen RC (2009) Ejaculatory dysfunction and its association with lower urinary tract symptoms of benign prostatic hyperplasia and BPH treatment. Urology 74:15–21
Author information
Authors and Affiliations
Contributions
GC: data collection, design and writing of the manuscript. MPL: data collection, design and writing of the manuscript. SG: conception and design of the article and critical review. SA: conception and design of the article and critical review. JdlR: conception and design of the article and critical review.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors declares any conflict of interest for the present work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Calik, G., Laguna, M.P., Gravas, S. et al. Preservation of antegrade ejaculation after surgical relief of benign prostatic obstruction is a valid endpoint. World J Urol 39, 2277–2289 (2021). https://doi.org/10.1007/s00345-021-03682-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-021-03682-w