Abstract
Background
The presence of type 2 diabetes mellitus increases the risk of developing the colon cancer. The main objective of this study was to determine the role of sodium orthovanadate (SOV) in colon cancer associated with diabetes mellitus by targeting the competitive inhibition of PTP1B.
Methods
For in vivo study, high fat diet with low dose streptozotocin model was used for inducing the diabetes mellitus. Colon cancer was induced by injecting 1,2-dimethylhydrazine (25 mg/kg, sc) twice a week. TNM staging and immunohistochemistry (IHC) was carried out for colon cancer tissues. In vitro studies like MTT assay, clonogenic assay, rhodamine-123 dye assay and annexin V-FITC assay using flow cytometry were performed on HCT-116 cell line. CAM assay was performed to examine the anti-angiogenic effect of the drug.
Results
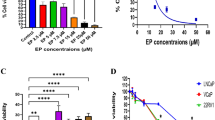
Sodium orthovanadate reduces the blood glucose level and tumor parameters in the animals. In vitro studies revealed that SOV decreased cell proliferation dose dependently. In addition, SOV induced apoptosis as depicted from rhodamine-123 dye assay and annexin V-FITC assay using flow cytometry as well as p53 IHC staining. SOV showed reduced angiogenesis effect on eggs which was depicted from CAM assay and also from CD34 and E-cadherin IHC staining.
Conclusions
Our data suggest that SOV exhibits protective role in colon cancer associated with diabetes mellitus. SOV exhibits anti-proliferative, anti-angiogenic and apoptotic inducing effects hence can be considered for therapeutic switching in diabetic colon cancer.







Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Berridge MV, Herst PM, Tan AS (2005) Tetrazolium dyes as tools in cell biology: new insights into their cellular reduction. Biotechnol Annu Rev 11(SUPPL):127–152. https://doi.org/10.1016/S1387-2656(05)11004-7
Bild AH et al (2006) Oncogenic pathway signatures in human cancers as a guide to targeted therapies. Nature 439(7074):353–357. https://doi.org/10.1038/nature04296
Bottinger E (2007) Foundations, promises and uncertainties of personalized medicine address correspondence to. Mt Sinai J Med 1:15–21. https://doi.org/10.1002/msj.20005
Chen PJ et al (2015) Protein tyrosine phosphatase 1B (PTP1B): a key regulator and therapeutic target in liver diseases. Toxicology 337:10–20. https://doi.org/10.1016/j.tox.2015.08.006
Delwar ZM et al (2012) Menadione: sodium orthovanadate combination eliminates and inhibits migration of detached cancer cells. ISRN Pharmacol 2012:1–10. https://doi.org/10.5402/2012/307102
Devasagayam TPA, Boloor KK, Ramasarma T (2003) Methods for estimating lipid peroxidation: an analysis of merits and demerits. Indian J Biochem Biophys 40(5):300–308
Dorsey BM, McLauchlan CC, Jones MA (2018) Evidence that speciation of oxovanadium complexes does not solely account for inhibition of leishmania acid phosphatases. Front Chem. https://doi.org/10.3389/fchem.2018.00109
Elchebly M et al (1999) Increased insulin sensitivity and obesity resistance in mice lacking the protein tyrosine phosphatase-1B gene. Science 283(5407):1544–1548. https://doi.org/10.1126/science.283.5407.1544
Franken NAP et al (2006) Clonogenic assay of cells in vitro. Nat Protoc 1(5):2315–2319. https://doi.org/10.1038/nprot.2006.339
Giouleme O, Diamantidis MD, Katsaros MG (2011) Is diabetes a causal agent for colorectal cancer? Pathophysiological and molecular mechanisms. World J Gastroenterol 17(4):444–448. https://doi.org/10.3748/wjg.v17.i4.444
Goldstein BJ et al (2000) Tyrosine dephosphorylation and deactivation of insulin receptor substrate-1 by protein-tyrosine phosphatase 1B. Possible facilitation by the formation of a ternary complex with the GRB2 adaptor protein. J Biol Chem 275(6):4283–4289. https://doi.org/10.1074/jbc.275.6.4283
Gonçalves AP et al (2011) Orthovanadate-induced cell death in RET/PTC1-harboring cancer cells involves the activation of caspases and altered signaling through PI3K/Akt/mTOR. Life Sci 89(11–12):371–377. https://doi.org/10.1016/j.lfs.2011.07.004
Gupta BL, Preet A, Baquer NZ (2004) Protective effects of sodium orthovanadate in diabetic reticulocytes and ageing red blood cells of Wistar rats. J Biosci 29(1):73–79. https://doi.org/10.1007/BF02702564
Hanas R, John G (2010) 2010 Consensus statement on the worldwide standardization of the hemoglobin A1C measurement. Diabetes Care 33(8):1903–1904. https://doi.org/10.2337/dc10-0953
Homandberg GA (2009) The protein protocols handbook, 3rd edn. Humana Press, Totowa, p 77. https://doi.org/10.1007/978-1-59745-198-7 (8(1))
Inokuma T et al (2009) Oxidative stress and tumor progression in colorectal cancer. Hepatogastroenterology 56(90):343–347
Izumi H et al (2015) Favorable effect of the combination of vinorelbine and dihydropyrimidine dehydrogenase-inhibitory fluoropyrimidine in EGFR-mutated lung adenocarcinoma: retrospective and in vitro studies. Int J Oncol 46(3):989–998. https://doi.org/10.3892/ijo.2015.2815
Jorand R et al (2016) Molecular signatures of mu opioid receptor and somatostatin receptor 2 in pancreatic cancer. Mol Biol Cell 27(22):3659–3672. https://doi.org/10.1091/mbc.E16-06-0427
Kalmer M et al (2022) Clonogenic assays improve determination of variant allele frequency of driver mutations in myeloproliferative neoplasms. Ann Hematol 101(12):2655–2663. https://doi.org/10.1007/S00277-022-05000-9
Kandoth C et al (2013) Mutational landscape and significance across 12 major cancer types. Nature 502(7471):333–339. https://doi.org/10.1038/nature12634
Khalil AA, Jameson MJ (2017) Sodium orthovanadate inhibits proliferation and triggers apoptosis in oral squamous cell carcinoma in vitro. Biochem Mosc 82(2):149–155. https://doi.org/10.1134/S0006297917020067
Kim SA et al (2016) Loss of CDH1 (E-cadherin) expression is associated with infiltrative tumour growth and lymph node metastasis. Br J Cancer 114(2):199–206. https://doi.org/10.1038/bjc.2015.347
Kowalski S et al (2017) Selective cytotoxicity of vanadium complexes on human pancreatic ductal adenocarcinoma cell line by inducing necroptosis, apoptosis and mitotic catastrophe process. Oncotarget 8(36):60324–60341. https://doi.org/10.18632/oncotarget.19454
Krishnan N et al (2015) PTP1B inhibition suggests a therapeutic strategy for Rett syndrome Find the latest version: PTP1B inhibition suggests a therapeutic strategy for Rett syndrome. J Clin Investig 125(8):3163–3177. https://doi.org/10.1172/JCI80323.focusing
Kue CS et al (2014) Chick embryo chorioallantoic membrane (CAM): an alternative predictive model in acute toxicological studies for anti-cancer drugs. Exp Anim 64(2):129–138. https://doi.org/10.1538/expanim.14-0059
Kumar P et al (2015) Sodium orthovanadate and trigonella foenum graecum prevents neuronal parameters decline and impaired glucose homeostasis in alloxan diabetic rats. Prague Med Rep 116(2):122–138. https://doi.org/10.14712/23362936.2015.51
Lashner BA et al (2003) Abnormal p53 immunohistochemistry is associated with an increased colorectal cancer-related mortality in patients with ulcerative colitis. Am J Gastroenterol 98(6):1423–1427. https://doi.org/10.1016/S0002-9270(03)00422-2
Li S et al (2005) Crystal structure of a complex between protein tyrosine phosphatase 1B and the insulin receptor tyrosine kinase. Structure 13(11):1643–1651. https://doi.org/10.1016/j.str.2005.07.019
Liu G (2005) protein tyrosine phosphatase 1B inhibition: opportunities and challenges. Curr Med Chem 10(15):1407–1421. https://doi.org/10.2174/0929867033457296
Liu H et al (2015) PTP1B promotes cell proliferation and metastasis through activating src and ERK1/2 in non-small cell lung cancer. Cancer Lett 359(2):218–225. https://doi.org/10.1016/j.canlet.2015.01.020
Liu ZQ et al (2015) Fumosorinone, a novel PTP1B inhibitor, activates insulin signaling in insulin-resistance HepG2 cells and shows anti-diabetic effect in diabetic KKAy mice. Toxicol Appl Pharmacol 285(1):61–70. https://doi.org/10.1016/j.taap.2015.03.011
López I et al (2012) Different mutation profiles associated to P53 accumulation in colorectal cancer. Gene 499(1):81–87. https://doi.org/10.1016/j.gene.2012.02.011
Malik A et al (2011) Role of CD34, vascular endothelial growth factor, and p53 in neoangiogenesis as correlated with stage of disease in colorectal carcinoma. Med J Armed Forces India 67(4):320–325. https://doi.org/10.1016/S0377-1237(11)60076-2
Melling N et al (2016) High Ki67 expression is an independent good prognostic marker in colorectal cancer. J Clin Pathol 69(3):209–214. https://doi.org/10.1136/jclinpath-2015-202985
Nakamoto K et al (2013) Expression of E-cadherin and KRAS mutation may serve as biomarkers of cetuximab-based therapy in metastatic colorectal cancer. Oncol Lett 5(4):1295–1300. https://doi.org/10.3892/ol.2013.1187
Nguyen M, Shing Y, Folkman J (1994) Quantitation of angiogenesis and antiangiogenesis in the chick embryo chorioallantoic membrane. Microvasc Res 47:31–40. https://doi.org/10.1006/mvre.1994.1003
Patel MM, Patel BM (2018) Repurposing of sodium valproate in colon cancer associated with diabetes mellitus: role of HDAC inhibition. Eur J Pharm Sci 121:188–199. https://doi.org/10.1016/j.ejps.2018.05.026
Pessin JE, Saltiel AR (2000) On diabetes: insulin resistance Signaling pathways in insulin action: molecular targets of insulin resistance. J Clin Investig 106(2):165–169. https://doi.org/10.1172/JCI10582.On
Ribatti D (2010) The chick embryo chorioallantoic membrane as an in vivo assay to study antiangiogenesis. Pharmaceuticals 3(3):482–513. https://doi.org/10.3390/ph3030482
Riccardi C, Nicoletti I (2006) Analysis of apoptosis by propidium iodide staining and flow cytometry. Nat Protoc 1(3):1458–1461. https://doi.org/10.1038/nprot.2006.238
Salvioli S et al (1997) JC-1, but not DiOC6(3) or rhodamine 123, is a reliable fluorescent probe to assess ΔΨ changes in intact cells: implications for studies on mitochondrial functionality during apoptosis. FEBS Lett 411(1):77–82. https://doi.org/10.1016/S0014-5793(97)00669-8
Sasaki K et al (2010) Chloroquine potentiates the anti-cancer effect of 5-fluorouracil on colon cancer cells. BMC Cancer 10:370. https://doi.org/10.1186/1471-2407-10-370
Saxena AK et al (1993) Impaired antioxidant status in diabetic rat liver. Effect of vanadate. Biochem Pharmacol 45(3):539–542. https://doi.org/10.1016/0006-2952(93)90124-F
Sen B, Johnson FM (2011) Regulation of Src family kinases in human cancers. J Signal Transduct 2011:1–14. https://doi.org/10.1155/2011/865819
Shah NR, Patel BM (2016) Secoisolariciresinol diglucoside rich extract of L. usitatissimum prevents diabetic colon cancer through inhibition of CDK4. Biomed Pharmacother 83:733–739. https://doi.org/10.1016/j.biopha.2016.07.041
Smith IK, Vierheller TL, Thorne CA (1988) Assay of glutathione reductase in crude tissue homogenates using 5,5’-dithiobis(2-nitrobenzoic acid). Anal Biochem 175(2):408–413. https://doi.org/10.1016/0003-2697(88)90564-7
Sun J et al (2015) Magnolia officinalis extract contains potent inhibitors against PTP1B and attenuates hyperglycemia in db/db mice. BioMed Res Int. https://doi.org/10.1155/2015/139451
Tan Y et al (2006) Ubiquitous calpains promote both apoptosis and survival signals in response to different cell death stimuli. J Biol Chem 281(26):17689–17698. https://doi.org/10.1074/jbc.M601978200
Wright E, Scism-Bacon JL, Glass LC (2006) Oxidative stress in type 2 diabetes: The role of fasting and postprandial glycaemia. Int J Clin Pract 60(3):308–314. https://doi.org/10.1111/j.1368-5031.2006.00825.x
Wu X et al (2001) Depot-specific variation in protein-tyrosine phosphatase activities in human omental and subcutaneous adipose tissue: a potential contribution to differential insulin sensitivity. J Clin Endocrinol Metab 86(12):5973–5980. https://doi.org/10.1210/jcem.86.12.8109
Wu Y et al (2014) Sodium orthovanadate inhibits growth of human hepatocellular carcinoma cells in vitro and in an orthotopic model in vivo. Cancer Lett 351(1):108–116. https://doi.org/10.1016/j.canlet.2014.05.018
Yadav U, Moorthy K, Baquer N (2004) Effects of sodium-orthovanadate and Trigonella foenum-graecum seeds on hepatic and renal lipogenic enzymes and lipid profile during alloxan diabetes. J Biosci 29(1):81–91
Ye J et al (2013) miRNA-27b targets vascular endothelial growth factor C to inhibit tumor progression and angiogenesis in colorectal cancer. PLoS ONE 8(4):e60687. https://doi.org/10.1371/journal.pone.0060687
Yin TF et al (2016) Research progress on chemopreventive effects of phytochemicals on colorectal cancer and their mechanisms. World J Gastroenterol 22(31):7058–7068. https://doi.org/10.3748/wjg.v22.i31.7058
Zhang Y et al (2017) Protein phosphotyrosine phosphatase 1B (PTP1B) in calpaindependent feedback regulation of vascular endothelial growth factor receptor (VEGFR2) in endothelial cells: implications in VEGF-dependent angiogenesis and diabetic wound healing. J Biol Chem 292(2):407–417. https://doi.org/10.1074/jbc.M116.766832
Zhu S, Bjorge JD, Fujita DJ (2007) PTP1B contributes to the oncogenic properties of colon cancer cells through Src activation. Can Res 67(21):10129–10137. https://doi.org/10.1158/0008-5472.CAN-06-4338
Cиpoтa TB (2012) Ключeвыe cлoвa. pp 77–87
Acknowledgements
The authors are thankful to Nirma University for providing basic facilities and financial support for carrying out the study. This work is part of M. Pharm. (Pharmacology) thesis of Ms. Kruti Patel.
Author information
Authors and Affiliations
Contributions
Conceptualization, Bhoomika Patel; investigation, Kruti Patel, Vivek Bora; methodology, Kruti Patel, Vivek Bora, and Bhoomika Patel; investigation, Kruti Patel, Vivek Bora Resources, Bhoomika Patel; Validation, Kruti Patel; writing—original draft, Kruti Patel, Vivek Bora; writing—review and editing, Bhoomika Patel *Terminology Written as per CRediT Taxonomy.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Patel, K., Bora, V. & Patel, B. Sodium orthovanadate exhibits anti-angiogenic, antiapoptotic and blood glucose-lowering effect on colon cancer associated with diabetes. Cancer Chemother Pharmacol 93, 55–70 (2024). https://doi.org/10.1007/s00280-023-04596-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-023-04596-7