Abstract
Purpose
To examine the anatomy of the inferior oblique (IO) muscle and its surrounding structures to clarify why IO muscle entrapment develops less in orbital floor trapdoor fractures.
Methods
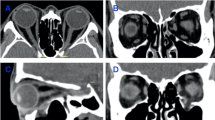
Computed tomographic (CT) images on the unaffected sides were obtained from 64 patients with unilateral orbital fractures. On coronal planes, presence or absence of an infraorbital groove below the IO muscle was confirmed. At the level of the medial margin of the infraorbital groove/canal, the distance from the orbital floor to the IO muscle (IO-floor distance), the thickness of the orbital floor, and the shortest distance from the inferior rectus (IR) muscle to the orbital floor (shortest IR-floor distance) were measured. On quasi-sagittal planes, the distances from the inferior orbital rim to the inferior margin of the IO muscle (IO-rim distance) and the most anterior point of the infraorbital groove (groove-rim distance) were measured.
Results
The infraorbital groove was found below the IO muscle in eight patients (12.5%), and the IO-rim and IO-floor distances were significantly longer than the groove-rim and shortest IR-floor distances, respectively (p < 0.001). The orbital floor below the IO muscle was significantly thicker than that below the IR muscle (p < 0.001).
Conclusion
Although the medial margin of the infraorbital groove is the most common fracture site, the IO muscle was not located above the groove in most cases. A longer IO-floor distance and thicker orbital floor below the IO muscle may also contribute to less occurrence of IO muscle entrapment in orbital floor trapdoor fractures.


Similar content being viewed by others
References
Ana-Magadia MG, Valencia MRP, Naito M, Nakano T, Miyazaki H, Kakizaki H, Takahashi Y (2020) Location of the myoneural junction of the inferior oblique muscle: an anatomic study. Ann Anat. https://doi.org/10.1016/j.aanat.2019.151429
Challa NK, Alghamdi WM (2021) Normal ocular protrusion values in South Indian population and effect of age, gender and refractive status on ocular protrusion. Clin Ophthalmol 15:1445–1451. https://doi.org/10.2147/OPTH.S302154
Kim S, Kim TK, Kim SH (2009) Clinicoradiologic findings of entrapped inferior oblique muscle in fracture of the orbital floor. Korean J Ophthalmol 23:224–227. https://doi.org/10.3341/kjo.2009.23.3.224
Koornneef L (1977) New insights in the human orbital connective tissue: result of a new anatomical approach. Arch Ophthalmol 95:1269–1273. https://doi.org/10.1001/archopht.1977.04450070167018
Lee JH, Shim HS, Woo KI, Kim YD (2013) Inferior oblique underaction: a transient complication related to inferior orbital wall fracture in childhood. Acta Ophthalmol 91:685–690. https://doi.org/10.1111/j.1755-3768.2012.02466.x
Lee PAL, Kono S, Kakizaki H, Takahashi Y (2021) Entrapment of the inferior oblique and inferior rectus muscles in orbital trapdoor fracture. Orbit. https://doi.org/10.1080/01676830.2021.1914669
Miller JM, Demer JL, Poukens V, Pavlovski DS, Nguyen HN, Rossi EA (2003) Extraocular connective tissue architecture. J Vis 3:240–251. https://doi.org/10.1167/3.3.5
Nardi M (1996) Hypertropia and posterior blowout fracture. Ophthalmology 103:995–996. https://doi.org/10.1016/s0161-6420(96)30550-2
Schmidt P, Kempin R, Langner S, Beule A, Kindler S, Koppe T, Völzke H, Ittermann T, Jürgens C, Tost F (2019) Association of anthropometric markers with globe position: a population-based MRI study. PLoS ONE. https://doi.org/10.1371/journal.pone.0211817
Silverman N, Spindle J, Tang SX, Wu A, Hong BK, Shore JW, Wester S, Levin F, Connor M, Burt B, Nakra T, Shepler T, Hink E, El-Sawy T, Shinder R (2017) Orbital floor fracture with entrapment: Imaging and clinical correlations in 45 cases. Orbit 36:331–336. https://doi.org/10.1080/01676830.2017.1337180
Takahashi Y, Nakano T, Miyazaki H, Kakizaki H (2016) An anatomical study of the orbital floor in relation to the infraorbital groove: implications of predisposition to orbital floor fracture site. Graefes Arch Clin Exp Ophthalmol 254:2049–2055. https://doi.org/10.1007/s00417-016-3455-2
Takahashi Y, Sabundayo MS, Miyazaki H, Mito H, Kakizaki H (2017) Incarceration of the inferior oblique muscle branch of the oculomotor nerve in patients with orbital floor trapdoor fracture. Graefes Arch Clin Exp Ophthalmol 255:2059–2065. https://doi.org/10.1007/s00417-017-3790-y
Takahashi Y, Sabundayo MS, Miyazaki MH, Kakizaki H (2018) Orbital trapdoor fractures: different clinical profiles between adult and paediatric patients. Br J Ophthalmol 102:885–891. https://doi.org/10.1136/bjophthalmol-2017-310890
Tsutsumi S, Nakamura M, Tabuchi T, Yasumoto Y, Ito M (2013) An anatomic study of the inferior oblique nerve with high-resolution magnetic resonance imaging. Surg Radiol Anat 35:377–383. https://doi.org/10.1007/s00276-012-1040-x
Vaidya A, Lee PAL, Kitaguchi Y, Kakizaki H, Takahashi Y (2020) Spontaneous orbital decompression in thyroid eye disease: new measurement methods and its influential factors. Graefes Arch Clin Exp Ophthalmol 258:2321–2329. https://doi.org/10.1007/s00417-020-04762-0
Valencia MR, Miyazaki H, Ito M, Nishimura K, Kakizaki H, Takahashi Y (2021) Radiological findings of orbital blowout fractures: a review. Orbit 40:98–109. https://doi.org/10.1080/01676830.2020.1744670
Acknowledgements
Other contributors: no one contributed to the work who did not meet our authorship criteria.
Funding
None.
Author information
Authors and Affiliations
Contributions
SK manuscript writing. AV manuscript editing. HM manuscript editing. HK manuscript editing, supervision, and funding. YT protocol/project development, data collection, data analysis, and manuscript writing/editing.
Corresponding author
Ethics declarations
Conflicts of interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This study was approved by the Institutional Review Board (IRB) of our institution (No. 2021–40) and followed the tenets of the 1964 Declaration of Helsinki.
Consent to participate
The IRB granted a waiver of informed consent for this study on the basis of the ethical guidelines for medical and health research involving human subjects established by the Japanese Ministry of Education, Culture, Sports, Science, and Technology and the Ministry of Health, Labour, and Welfare. The waiver was granted because the study was a retrospective review and not an interventional study and because it was difficult to obtain consent from patients who had been treated several years prior to this study. Nevertheless, at the request of the IRB, an outline of the study was published on the website of our institution and this was made available for public viewing. This public posting also gave patients an opportunity to decline participation, although no refusal was made known to us. Personal identifiers were removed from the records prior to data analysis.
Consent for publication
All authors agreed with publication of this paper.
Data availability and material
All data are included in this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kono, S., Vaidya, A., Miyazaki, H. et al. Anatomical implication of less occurrence of inferior oblique muscle entrapment in orbital floor trapdoor fracture. Surg Radiol Anat 43, 1823–1828 (2021). https://doi.org/10.1007/s00276-021-02808-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-021-02808-4