Abstract
Introduction
Maternal obesity is associated with a range of pregnancy complications, including fetal growth restriction (FGR), whereby a fetus fails to reach its genetically determined growth. Placental insufficiency and reduced nutrient transport play a role in the onset of FGR.
Objectives
Metabolomic profiling was used to reveal altered maternal and fetal metabolic pathways in a model of diet induced obesity during pregnancy, leading to reduced fetal growth.
Methods
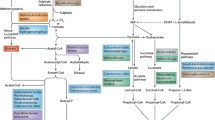
We examined the metabolome of maternal and fetal livers, and placenta following a high fat and salt intake. Sprague–Dawley rats were assigned to (a) control diet (CD; 1 % salt, 10 % kcal from fat), (b) high salt diet (SD; 4 % salt, 10 % kcal from fat), (c) high fat diet (HF; 1 % salt, 45 % kcal from fat) or (d) high-fat high-salt diet (HFSD; 4 % salt, 45 % kcal from fat) 21 days prior to pregnancy and during gestation. Metabolites from maternal and fetal livers, and placenta were identified using gas and liquid chromatography combined with mass spectrometry.
Results
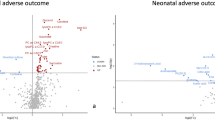
Maternal HF intake resulted in reduced fetal weight. Altered metabolite profiles were observed in the HF maternal and fetal liver, and placenta. Polyunsaturated fatty acid metabolism was significantly altered in maternal and fetal liver by maternal fat intake.
Conclusion
Excess of linoleic and α-linoleic acid (essential fatty acids) may be detrimental during placentation and associated with a reduction in fetal weight. Additionally, maternal, placental and fetal response to increased fat consumption seems likely to involve palmitoleic acid utilization as an adaptive response during maternal obesity.




Similar content being viewed by others
References
Aggio, R., Villas-Boas, S. G., & Ruggiero, K. (2011). Metab: An R package for high-throughput analysis of metabolomics data generated by GC-MS. Bioinformatics, 27, 2316–2318. doi:10.1093/bioinformatics/btr379.
Akyol, A., Langley-Evans, S. C., & McMullen, S. (2009). Obesity induced by cafeteria feeding and pregnancy outcome in the rat. British Journal of Nutrition, 102, 1601–1610. doi:10.1017/S0007114509990961.
Anderson, N. H., Sadler, L. C., Stewart, A. W., Fyfe, E. M., & McCowan, L. M. E. (2013). Independent risk factors for infants who are small for gestational age by customised birthweight centiles in a multi-ethnic New Zealand population. Australian and New Zealand Journal of Obstetrics and Gynaecology, 53, 136–142. doi:10.1111/ajo.12016.
Austdal, M., et al. (2015a). First trimester urine and serum metabolomics for prediction of preeclampsia and gestational hypertension: A prospective screening study. International Journal of Molecular Sciences, 16, 21520–21538. doi:10.3390/ijms160921520.
Austdal, M., et al. (2015b). Metabolic profiles of placenta in preeclampsia using HR-MAS MRS metabolomics. Placenta, 36, 1455–1462. doi:10.1016/j.placenta.2015.10.019.
Ay, L., et al. (2009). Maternal anthropometrics are associated with fetal size in different periods of pregnancy and at birth. The Generation R Study. The Generation R Study. BJOG, 116, 953–963. doi:10.1111/j.1471-0528.2009.02143.x.
Benjamini, Y., & Hochberg, Y. (1995). Controlling the false discovery rate—a practical and powerful approach to multiple testing. Journal of the Royal Statistical Society Series B-Methodological, 57, 289–300.
Brown, M., et al. (2011). Automated workflows for accurate mass-based putative metabolite identification in LC/MS-derived metabolomic datasets. Bioinformatics, 27, 1108–1112. doi:10.1093/bioinformatics/btr079.
Cao, H., Gerhold, K., Mayers, J. R., Wiest, M. M., Watkins, S. M., & Hotamisligil, G. S. (2008). Identification of a lipokine, a lipid hormone linking adipose tissue to systemic metabolism. Cell, 134, 933–944. doi:10.1016/j.cell.2008.07.048.
Cetin, I., et al. (2002). Intrauterine growth restriction is associated with changes in polyunsaturated fatty acid fetal-maternal relationships. Pediatric Research, 52, 750–755. doi:10.1203/01.Pdr.0000031923.07968.D5.
Development Core Team, R. (2008). R: A language and environment for statistical computing. Vienna: R Foundation for Statistical Computing.
Diaz, S. O., et al. (2013). Second trimester maternal urine for the diagnosis of trisomy 21 and prediction of poor pregnancy outcomes. Journal of Proteome Research, 12, 2946–2957. doi:10.1021/pr4002355.
Economides, D. L., Nicolaides, K. H., & Campbell, S. (1991). Metabolic and endocrine findings in appropriate and small for gestational age fetuses. Journal of Perinatal Medicine, 19, 97–105.
Fanos, V., Atzori, L., Makarenko, K., Melis, G. B., & Ferrazzi, E. (2013). Metabolomics application in maternal-fetal medicine. BioMed Research International, 2013, 720514. doi:10.1155/2013/720514.
Gardosi, J., Kady, S. M., McGeown, P., Francis, A., & Tonks, A. (2005). Classification of stillbirth by relevant condition at death (ReCoDe): Population based cohort study. British Medical Journal, 331, 1113–1117. doi:10.1136/bmj.38629.587639.7C.
Garg, M. L., Blake, R. J., Wills, R. B., & Clayton, E. H. (2007). Macadamia nut consumption modulates favourably risk factors for coronary artery disease in hypercholesterolemic subjects. Lipids, 42, 583–587. doi:10.1007/s11745-007-3042-8.
Gueorguieva, R., & Krystal, J. H. (2004). Move over ANOVA—Progress in analyzing repeated-measures data and its reflection in papers published in the archives of general psychiatry. Archives of General Psychiatry, 61, 310–317. doi:10.1001/archpsyc.61.3.310.
Hajer, G. R., van Haeften, T. W., & Visseren, F. L. (2008). Adipose tissue dysfunction in obesity, diabetes, and vascular diseases. European Heart Journal, 29, 2959–2971. doi:10.1093/eurheartj/ehn387.
Hayes, E. K., et al. (2012). Adverse Fetal and neonatal outcomes associated with a life-long high fat diet: Role of altered development of the placental vasculature. PLoS One. doi:10.1371/journal.pone.0033370.
Hill, M., Parizek, A., Kancheva, R., & Jirasek, J. E. (2011). Reduced progesterone metabolites in human late pregnancy. Physiological Research, 60, 225–241.
Horgan, R. P., et al. (2011). Metabolic profiling uncovers a phenotypic signature of small for gestational age in early pregnancy. Journal of Proteome Research, 10, 3660–3673. doi:10.1021/pr2002897.
Howie, G. J., Sloboda, D. M., Kamal, T., & Vickers, M. H. (2009). Maternal nutritional history predicts obesity in adult offspring independent of postnatal diet. Journal of Physiology, 587, 905–915. doi:10.1113/jphysiol.2008.163477.
Huang, L., Yu, X., Keim, S., Li, L., Zhang, L., & Zhang, J. (2014). Maternal prepregnancy obesity and child neurodevelopment in the Collaborative Perinatal Project. International Journal of Epidemiology, 43, 783–792. doi:10.1093/ije/dyu030.
Innis, S. M. (2008). Dietary omega 3 fatty acids and the developing brain. Brain Research, 1237, 35–43. doi:10.1016/j.brainres.2008.08.078.
Kenny, L. C., et al. (2010). Robust early pregnancy prediction of later preeclampsia using metabolomic biomarkers. Hypertension, 56, 741–749. doi:10.1161/HYPERTENSIONAHA.110.157297.
Kovo, M., et al. (2013). The placental factor in early- and late-onset normotensive fetal growth restriction. Placenta, 34, 320–324. doi:10.1016/j.placenta.2012.11.010.
Kusinski, L. C., et al. (2012). eNOS knockout mouse as a model of fetal growth restriction with an impaired uterine artery function and placental transport phenotype. American Journal of Physiology-Regulatory Integrative and Comparative Physiology, 303, R86–R93. doi:10.1152/ajpregu.00600.2011.
Kyriakakou, M., et al. (2009). The role of IGF-1 and ghrelin in the compensation of intrauterine growth restriction. Reproductive Sciences, 16, 1193–1200. doi:10.1177/1933719109344629.
Mark, P. J., et al. (2011). A maternal high-fat diet in rat pregnancy reduces growth of the fetus and the placental junctional zone, but not placental labyrinth zone growth. Journal of Developmental Origins of Health and Disease, 2, 63–70. doi:10.1017/S2040174410000681.
Matthan, N. R., Dillard, A., Lecker, J. L., Ip, B., & Lichtenstein, A. H. (2009). Effects of dietary palmitoleic acid on plasma lipoprotein profile and aortic cholesterol accumulation are similar to those of other unsaturated fatty acids in the F1B golden Syrian hamster. Journal of Nutrition, 139, 215–221. doi:10.3945/jn.108.099804.
Mayhew, T. M., Ohadike, C., Baker, P. N., Crocker, I. P., Mitchell, C., & Ong, S. S. (2003). Stereological investigation of placental morphology in pregnancies complicated by pre-eclampsia with and without intrauterine growth restriction. Placenta, 24, 219–226. doi:10.1053/plac.2002.0900.
McCowan, L. M. E., George-Haddad, M., Stacey, T., & Thompson, J. M. D. (2007). Fetal growth restriction and other risk factors for stillbirth in a New Zealand setting. Australian and New Zealand Journal of Obstetrics and Gynaecology, 47, 450–456. doi:10.1111/j.1479-828X.2007.00778.x.
McCowan, L. M. E., et al. (2013). Clinical prediction in early pregnancy of infants small for gestational age by customised birthweight centiles: Findings from a healthy nulliparous cohort. PLoS One. doi:10.1371/journal.pone.0070917.
McDonald, S. D., Han, Z., Mulla, S., Beyene, J., & Grp, K. S. (2010). Overweight and obesity in mothers and risk of preterm birth and low birth weight infants: Systematic review and meta-analyses. British Medical Journal. doi:10.1136/bmj.c3428.
Mele, J., Muralimanoharan, S., Maloyan, A., & Myatt, L. (2014). Impaired mitochondrial function in human placenta with increased maternal adiposity. The American Journal of Physiology—Endocrinology and Metabolism, 307, E419–E425. doi:10.1152/ajpendo.00025.2014.
Regnault, T. R. H., de Vrijer, B., Galan, H. L., Wilkening, R. B., Battaglia, F. C., & Meschia, G. (2013). Umbilical uptakes and transplacental concentration ratios of amino acids in severe fetal growth restriction. Pediatric Research, 73, 602–611. doi:10.1038/pr.2013.30.
Reynolds, C. M., Vickers, M. H., Harrison, C. J., Segovia, S. A., & Gray, C. (2014). High fat and/or high salt intake during pregnancy alters maternal meta-inflammation and offspring growth and metabolic profiles. Physiological Reports. doi:10.14814/phy2.12110.
Roex, A., Nikpoor, P., van Eerd, E., Hodyl, N., & Dekker, G. (2012). Serial plotting on customised fundal height charts results in doubling of the antenatal detection of small for gestational age fetuses in nulliparous women. Australian and New Zealand Journal of Obstetrics and Gynaecology, 52, 78–82. doi:10.1111/j.1479-828X.2011.01408.x.
Salihu, H. M., Mbah, A. K., Alio, A. P., Kornosky, J. L., Bruder, K., & Belogolovkin, V. (2009). Success of programming fetal growth phenotypes among obese women. Obstetrics and Gynecology, 114, 333–339. doi:10.1097/AOG.0b013e3181ae9a47.
Simopoulos, A. P. (2011). Importance of the omega-6/omega-3 balance in health and disease: Evolutionary aspects of diet. World Review of Nutrition and Dietetics, 102, 10–21. doi:10.1159/000327785.
Smart, K. F., Aggio, R. B., Van Houtte, J. R., & Villas-Boas, S. G. (2010). Analytical platform for metabolome analysis of microbial cells using methyl chloroformate derivatization followed by gas chromatography-mass spectrometry. Nature Protocols, 5, 1709–1729. doi:10.1038/nprot.2010.108.
Stein, S. E. (1999). An integrated method for spectrum extraction and compound identification from gas chromatography/mass spectrometry data. Journal of the American Society for Mass Spectrometry, 10, 770–781. doi:10.1016/S1044-0305(99)00047-1.
Sumner, L. W., et al. (2007). Proposed minimum reporting standards for chemical analysis. Metabolomics, 3, 211–221. doi:10.1007/s11306-007-0082-2.
Uauy, R., Hoffman, D. R., Peirano, P., Birch, D. G., & Birch, E. E. (2001). Essential fatty acids in visual and brain development. Lipids, 36, 885–895.
Xia, J. G., & Wishart, D. S. (2011). Web-based inference of biological patterns, functions and pathways from metabolomic data using MetaboAnalyst. Nature Protocols, 6, 743–760. doi:10.1038/nprot.2011.319.
Yang, Z. H., Miyahara, H., & Hatanaka, A. (2011). Chronic administration of palmitoleic acid reduces insulin resistance and hepatic lipid accumulation in KK-Ay Mice with genetic type 2 diabetes. Lipids in Health and Disease, 10, 120. doi:10.1186/1476-511X-10-120.
Zhang, L. X., et al. (2014). Untargeted fatty acid profiles based on the selected ion monitoring mode. Analytica Chimica Acta, 839, 44–50. doi:10.1016/j.aca.2014.06.040.
Acknowledgments
The authors would like to express their gratitude for support provided by the Vernon Jansen Unit and the Centre for Genomics, Proteomics and Metabolomics. Technical assistance was provided by Rachna Patel, Angelica Bernal, Minglan Li, Elizabeth McKenzie and Margaret Coe. Financial assistance was provided by Gravida: National Centre for Growth and Development (Project no. STF-13-24), Lotteries Health Research Fellowship, Faculty Development Research Funding (FDRF) and the Nutricia Research Foundation.
Author contributions
KS, PNB, CG and MHV designed research; KM and CJH conducted the research with support from KR in the biostatistical analysis; KS, CG and KM wrote manuscript; MHV, PNB, JLS, CMR, KR and SGV-B critically evaluated the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
KM, CG, CMR, MHV, CJH, JLS, KR, SGV-B, PNB, KS declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving animals were in accordance with the ethical standards of the institution or practice at which the studies were conducted. Animal procedures were approved by the Animal Ethics Committee of the University of Auckland (approval R1069). This article does not contain any studies with human participants performed by any of the authors.
Additional information
Karen Mumme and Clint Gray have contributed equally.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mumme, K., Gray, C., Reynolds, C.M. et al. Maternal-fetal hepatic and placental metabolome profiles are associated with reduced fetal growth in a rat model of maternal obesity. Metabolomics 12, 83 (2016). https://doi.org/10.1007/s11306-016-1014-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11306-016-1014-9