Abstract
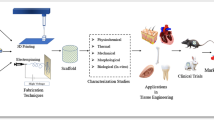
Soft tissues connect, support, or surround other structures and organs of the body, including skeletal muscles, tendon vessels, and nerves supplying these components. Also, organs such as the heart, brain, liver, and kidney are considered as soft tissues. Acute and chronic injury may cause transient or permanent damage to organs and soft tissues. If the damage is severe, the natural physiological repair and restoration mechanisms are not possible. The repair or regeneration using tissue engineered (TE) scaffolds has been considered as a clinical solution. TE approach involves the replacement of damaged parts using grafts made from natural or synthetic or composite polymers. Choosing the polymer with appropriate biological, physicochemical, and mechanical properties is the key to make a successful TE scaffold, and it is still a challenging task. Moreover, the fabrication technique and choice of cells or growth factors for encapsulation to develop the graft also play a crucial role. Therefore, in this chapter, we have highlighted the grafts developed for engineering soft tissues such as blood vessels, skin, cartilage, intervertebral disc, tendon, and skeletal muscle. We have restricted our focus on electrospun scaffolds, and injectable hydrogels prepared using polymers include collagen (Col), chitosan (CS), hyaluronic acid (HA) alginate (Alg), poly(caprolactone) (PCL), poly(lactic acid) (PLA), poly(glycolic-lactic acid) (PLGA), and their composites. This chapter will help the readers to understand the choice of materials and fabrication techniques for developing successful TE scaffolds for soft tissue engineering applications.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Albanna MZ, Bou-Akl TH, Walters HL III, Matthew HW (2012) Improving the mechanical properties of chitosan-based heart valve scaffolds using chitosan fibers. J Mech Behav Biomed Mater 5(1):171–180
Antunes BP, Moreira AF, Gaspar V, Correia I (2015) Chitosan/arginine–chitosan polymer blends for assembly of nanofibrous membranes for wound regeneration. Carbohydr Polym 130:104–112
Ardila D, Tamimi E, Doetschman T, Wagner W, Geest JV (2019) Modulating smooth muscle cell response by the release of TGFβ2 from tubular scaffolds for vascular tissue engineering. J Control Release 299:44–52
Asghari F, Samiei M, Adibkia K, Akbarzadeh A, Davaran S (2017) Biodegradable and biocompatible polymers for tissue engineering application: a review. Artif Cells, Nanomed Biotechnol 45(2):185–192
Baudis S, Heller C, Liska R, Stampfl J, Bergmeister H, Weigel G (2009) (meth) acrylate-based photoelastomers as tailored biomaterials for artificial vascular grafts. J Polym Sci A Polym Chem 47(10):2664–2676
Bhardwaj N, Chouhan D, Mandal B (2017) Tissue engineered skin and wound healing: current strategies and future directions. Curr Pharm Des 23(24):3455–3482
Bhardwaj N, Chouhan D, Mandal BB (2018) 3D functional scaffolds for skin tissue engineering. In: Functional 3D tissue engineering scaffolds. Elsevier, Amsterdam, pp 345–365
Bhattacharjee M, Coburn J, Centola M, Murab S, Barbero A, Kaplan DL, Martin I, Ghosh S (2015) Tissue engineering strategies to study cartilage development, degeneration and regeneration. Adv Drug Deliv Rev 84:107–122
Bishi DK, Mathapati S, Venugopal JR, Guhathakurta S, Cherian KM, Ramakrishna S, Verma RS (2013) Trans-differentiation of human mesenchymal stem cells generates functional hepatospheres on poly (L-lactic acid)-co-poly (ε-caprolactone)/collagen nanofibrous scaffolds. J Mater Chem B 1(32):3972–3984
Blanton PL, Biggs NL (1970) Ultimate tensile strength of fetal and adult human tendons. J Biomech 3(2):181–189
Boland ED, Telemeco TA, Simpson DG, Wnek GE, Bowlin GL (2004) Utilizing acid pretreatment and electrospinning to improve biocompatibility of poly (glycolic acid) for tissue engineering. J Biomed Mater Res Part B 71(1):144–152
Borselli C, Storrie H, Benesch-Lee F, Shvartsman D, Cezar C, Lichtman JW, Vandenburgh HH, Mooney DJ (2010) Functional muscle regeneration with combined delivery of angiogenesis and myogenesis factors. Proc Natl Acad Sci 107(8):3287–3292
Bowles RD, Setton LA (2017) Biomaterials for intervertebral disc regeneration and repair. Biomaterials 129:54–67
Butler DL, Kay MD, Stouffer DC (1986) Comparison of material properties in fascicle-bone units from human patellar tendon and knee ligaments. J Biomech 19(6):425–432
Buxboim A, Ivanovska IL, Discher DE (2010) Matrix elasticity, cytoskeletal forces and physics of the nucleus: how deeply do cells ‘feel’outside and in? J Cell Sci 123(3):297–308
Casper M, Fitzsimmons J, Stone J, Meza A, Huang Y, Ruesink T, O’Driscoll S, Reinholz G (2010) Tissue engineering of cartilage using poly-ɛ-caprolactone nanofiber scaffolds seeded in vivo with periosteal cells. Osteoarthr Cartil 18(7):981–991
Chan TR, Stahl PJ, Li Y, Yu SM (2015) Collagen–gelatin mixtures as wound model, and substrates for VEGF-mimetic peptide binding and endothelial cell activation. Acta Biomater 15:164–172
Chang WG, Niklason LE (2017) A short discourse on vascular tissue engineering. NPJ Regener Med 2(1):1–8
Cheema U, Yang SY, Mudera V, Goldspink G, Brown R (2003) 3-D in vitro model of early skeletal muscle development. Cell Motil Cytoskeleton 54(3):226–236
Chen J-P, Su C-H (2011) Surface modification of electrospun PLLA nanofibers by plasma treatment and cationized gelatin immobilization for cartilage tissue engineering. Acta Biomater 7(1):234–243
Chen H, Huang J, Yu J, Liu S, Gu P (2011a) Electrospun chitosan-graft-poly (ɛ-caprolactone)/poly (ɛ-caprolactone) cationic nanofibrous mats as potential scaffolds for skin tissue engineering. Int J Biol Macromol 48(1):13–19
Chen J, Yu Q, Wu B, Lin Z, Pavlos NJ, Xu J, Ouyang H, Wang A, Zheng MH (2011b) Autologous tenocyte therapy for experimental Achilles tendinopathy in a rabbit model. Tissue Eng A 17(15–16):2037–2048
Chen H, Xing X, Tan H, Jia Y, Zhou T, Chen Y, Ling Z, Hu X (2017) Covalently antibacterial alginate-chitosan hydrogel dressing integrated gelatin microspheres containing tetracycline hydrochloride for wound healing. Mater Sci Eng C 70:287–295
Chenite A, Chaput C, Wang D, Combes C, Buschmann M, Hoemann C, Leroux J, Atkinson B, Binette F, Selmani A (2000) Novel injectable neutral solutions of chitosan form biodegradable gels in situ. Biomaterials 21(21):2155–2161
Cheung H-Y, Lau K-T, Lu T-P, Hui D (2007) A critical review on polymer-based bio-engineered materials for scaffold development. Compos Part B 38(3):291–300
Chevrier A, Hoemann C, Sun J, Buschmann M (2011) Temporal and spatial modulation of chondrogenic foci in subchondral microdrill holes by chitosan-glycerol phosphate/blood implants. Osteoarthr Cartil 19(1):136–144
Cima L, Vacanti J, Vacanti C, Ingber D, Mooney D, Langer R (1991) Tissue engineering by cell transplantation using degradable polymer substrates. J Biomech Eng 113(2):143–151
Creaney L, Hamilton B (2008) Growth factor delivery methods in the management of sports injuries: the state of play. Br J Sports Med 42(5):314–320
de Valence S, Tille J-C, Mugnai D, Mrowczynski W, Gurny R, Möller M, Walpoth BH (2012) Long term performance of polycaprolactone vascular grafts in a rat abdominal aorta replacement model. Biomaterials 33(1):38–47
Deng D, Wang W, Wang B, Zhang P, Zhou G, Zhang WJ, Cao Y, Liu W (2014) Repair of Achilles tendon defect with autologous ASCs engineered tendon in a rabbit model. Biomaterials 35(31):8801–8809
Dhandayuthapani B, Krishnan UM, Sethuraman S (2010) Fabrication and characterization of chitosan-gelatin blend nanofibers for skin tissue engineering. J Biomed Mater Res B Appl Biomater 94(1):264–272
Dimatteo R, Darling NJ, Segura T (2018) In situ forming injectable hydrogels for drug delivery and wound repair. Adv Drug Deliv Rev 127:167–184
Ding F, Deng H, Du Y, Shi X, Wang Q (2014) Emerging chitin and chitosan nanofibrous materials for biomedical applications. Nanoscale 6(16):9477–9493
Du L, Yang Q, Zhang J, Zhu M, Ma X, Zhang Y, Wang L, Xu B (2019) Engineering a biomimetic integrated scaffold for intervertebral disc replacement. Mater Sci Eng C 96:522–529
Ehterami A, Salehi M, Farzamfar S, Samadian H, Vaez A, Ghorbani S, Ai J, Sahrapeyma H (2019) Chitosan/alginate hydrogels containing alpha-tocopherol for wound healing in rat model. J Drug Deliv Sci Technol 51:204–213
Eke G, Mangir N, Hasirci N, MacNeil S, Hasirci V (2017) Development of a UV crosslinked biodegradable hydrogel containing adipose derived stem cells to promote vascularization for skin wounds and tissue engineering. Biomaterials 129:188–198
Enea D, Cecconi S, Calcagno S, Busilacchi A, Manzotti S, Gigante A (2015) One-step cartilage repair in the knee: collagen-covered microfracture and autologous bone marrow concentrate. A pilot study. Knee 22(1):30–35
Engler AJ, Sen S, Sweeney HL, Discher DE (2006) Matrix elasticity directs stem cell lineage specification. Cell 126(4):677–689
Eslahi N, Abdorahim M, Simchi A (2016) Smart polymeric hydrogels for cartilage tissue engineering: a review on the chemistry and biological functions. Biomacromolecules 17(11):3441–3463
Fadaie M, Mirzaei E, Geramizadeh B, Asvar Z (2018) Incorporation of nanofibrillated chitosan into electrospun PCL nanofibers makes scaffolds with enhanced mechanical and biological properties. Carbohydr Polym 199:628–640
Farnebo S, Woon CY, Schmitt T, Joubert L-M, Kim M, Pham H, Chang J (2014) Design and characterization of an injectable tendon hydrogel: a novel scaffold for guided tissue regeneration in the musculoskeletal system. Tissue Eng A 20(9–10):1550–1561
Fasolino I, Guarino V, Cirillo V, Ambrosio L (2017) 5-Azacytidine-mediated hMSC behavior on electrospun scaffolds for skeletal muscle regeneration. J Biomed Mater Res A 105(9):2551–2561
Feng Y, Li Q, Wu D, Niu Y, Yang C, Dong L, Wang C (2017) A macrophage-activating, injectable hydrogel to sequester endogenous growth factors for in situ angiogenesis. Biomaterials 134:128–142
Ghasemi-Mobarakeh L, Prabhakaran MP, Balasubramanian P, Jin G, Valipouri A, Ramakrishna S (2013) Advances in electrospun nanofibers for bone and cartilage regeneration. J Nanosci Nanotechnol 13(7):4656–4671
Gilbert-Honick J, Grayson W (2020) Vascularized and innervated skeletal muscle tissue engineering. Adv Healthc Mater 9(1):1900626
Gilbert-Honick J, Iyer SR, Somers SM, Lovering RM, Wagner K, Mao H-Q, Grayson WL (2018) Engineering functional and histological regeneration of vascularized skeletal muscle. Biomaterials 164:70–79
Gloria A, Russo T, D’Amora U, Santin M, De Santis R, Ambrosio L (2020) Customised multiphasic nucleus/annulus scaffold for intervertebral disc repair/regeneration. Connect Tissue Res 61(2):152–162
Goldman SM, Henderson BE, Walters TJ, Corona BT (2018) Co-delivery of a laminin-111 supplemented hyaluronic acid based hydrogel with minced muscle graft in the treatment of volumetric muscle loss injury. PLoS One 13(1)
Goodarzi P, Falahzadeh K, Nematizadeh M, Farazandeh P, Payab M, Larijani B, Beik AT, Arjmand B (2018) Tissue engineered skin substitutes. In: Cell biology and translational medicine, vol 3. Springer, Cham, pp 143–188
Guenther D, Oks A, Ettinger M, Liodakis E, Petri M, Krettek C, Jagodzinski M, Haasper C (2013) Enhanced migration of human bone marrow stromal cells in modified collagen hydrogels. Int Orthop 37(8):1605–1611
Guo B, Qu J, Zhao X, Zhang M (2019) Degradable conductive self-healing hydrogels based on dextran-graft-tetraaniline and N-carboxyethyl chitosan as injectable carriers for myoblast cell therapy and muscle regeneration. Acta Biomater 84:180–193
Hagiwara K, Chen G, Kawazoe N, Tabata Y, Komuro H (2016) Promotion of muscle regeneration by myoblast transplantation combined with the controlled and sustained release of bFGFcpr. J Tissue Eng Regen Med 10(4):325–333
Hasan A, Memic A, Annabi N, Hossain M, Paul A, Dokmeci MR, Dehghani F, Khademhosseini A (2014) Electrospun scaffolds for tissue engineering of vascular grafts. Acta Biomater 10(1):11–25
He W, Ma Z, Teo WE, Dong YX, Robless PA, Lim TC, Ramakrishna S (2009) Tubular nanofiber scaffolds for tissue engineered small-diameter vascular grafts. J Biomed Mater Res Part A 90(1):205–216
Helary C, Zarka M, Giraud-Guille MM (2012) Fibroblasts within concentrated collagen hydrogels favour chronic skin wound healing. J Tissue Eng Regen Med 6(3):225–237
Herman I (2007) Physics of the human body. Springer, Cham
Huang H, Zhang X, Hu X, Dai L, Zhu J, Man Z, Chen H, Zhou C, Ao Y (2014) Directing chondrogenic differentiation of mesenchymal stem cells with a solid-supported chitosan thermogel for cartilage tissue engineering. Biomed Mater 9(3):035008
Hunt JA, Chen R, van Veen T, Bryan N (2014) Hydrogels for tissue engineering and regenerative medicine. J Mater Chem B 2(33):5319–5338
Ignatova M, Manolova N, Markova N, Rashkov I (2009) Electrospun non-woven nanofibrous hybrid mats based on chitosan and PLA for wound-dressing applications. Macromol Biosci 9(1):102–111
Janik H, Marzec M (2015) A review: fabrication of porous polyurethane scaffolds. Mater Sci Eng C 48:586–591
Ji QX, Deng J, Xing XM, Yuan CQ, Yu XB, Xu QC, Yue J (2010) Biocompatibility of a chitosan-based injectable thermosensitive hydrogel and its effects on dog periodontal tissue regeneration. Carbohydr Polym 82(4):1153–1160
Jiang T, Xu G, Wang Q, Yang L, Zheng L, Zhao J, Zhang X (2017) In vitro expansion impaired the stemness of early passage mesenchymal stem cells for treatment of cartilage defects. Cell Death Dis 8(6):e2851–e2851
Jiang T, Kai D, Liu S, Huang X, Heng S, Zhao J, Chan BQY, Loh XJ, Zhu Y, Mao C (2018) Mechanically cartilage-mimicking poly (PCL-PTHF urethane)/collagen nanofibers induce chondrogenesis by blocking NF–kappa B signaling pathway. Biomaterials 178:281–292
Jin G, Prabhakaran MP, Nadappuram BP, Singh G, Kai D, Ramakrishna S (2012) Electrospun poly (L-lactic acid)-co-poly (ϵ-caprolactone) nanofibres containing silver nanoparticles for skin-tissue engineering. J Biomater Sci Polym Ed 23(18):2337–2352
Jin G, Prabhakaran MP, Kai D, Annamalai SK, Arunachalam KD, Ramakrishna S (2013) Tissue engineered plant extracts as nanofibrous wound dressing. Biomaterials 34(3):724–734
Ju YM, San Choi J, Atala A, Yoo JJ, Lee SJ (2010) Bilayered scaffold for engineering cellularized blood vessels. Biomaterials 31(15):4313–4321
Kashi M, Baghbani F, Moztarzadeh F, Mobasheri H, Kowsari E (2018) Green synthesis of degradable conductive thermosensitive oligopyrrole/chitosan hydrogel intended for cartilage tissue engineering. Int J Biol Macromol 107:1567–1575
Kay MA, Glorioso JC, Naldini L (2001) Viral vectors for gene therapy: the art of turning infectious agents into vehicles of therapeutics. Nat Med 7(1):33–40
Kempson G (1982) Relationship between the tensile properties of articular cartilage from the human knee and age. Ann Rheum Dis 41(5):508–511
Kerin A, Wisnom M, Adams M (1998) The compressive strength of articular cartilage. Proc Inst Mech Eng H J Eng Med 212(4):273–280
Kheradmandi M, Vasheghani-Farahani E, Ghiaseddin A, Ganji F (2016) Skeletal muscle regeneration via engineered tissue culture over electrospun nanofibrous chitosan/PVA scaffold. J Biomed Mater Res A 104(7):1720–1727
Khorshidi S, Solouk A, Mirzadeh H, Mazinani S, Lagaron JM, Sharifi S, Ramakrishna S (2016) A review of key challenges of electrospun scaffolds for tissue-engineering applications. J Tissue Eng Regen Med 10(9):715–738
Kim J, Lin B, Kim S, Choi B, Evseenko D, Lee M (2015) TGF-β1 conjugated chitosan collagen hydrogels induce chondrogenic differentiation of human synovium-derived stem cells. J Biol Eng 9(1):1
Kim H-J, Min DJ, Lee SH, Lim JW, Jung N, Ryu HW, Jeong JH (2019) Tunable 3D Agarose-well to enhance structural integrity of a reconstructed human skin equivalent. Mater Lett 253:298–301
Kishore V, Bullock W, Sun X, Van Dyke WS, Akkus O (2012) Tenogenic differentiation of human MSCs induced by the topography of electrochemically aligned collagen threads. Biomaterials 33(7):2137–2144
Kuo SM, Chang SJ, Wang H-Y, Tang SC, Yang S-W (2014) Evaluation of the ability of xanthan gum/gellan gum/hyaluronan hydrogel membranes to prevent the adhesion of postrepaired tendons. Carbohydr Polym 114:230–237
Kuraitis D, Zhang P, Zhang Y, Padavan D, McEwan K, Sofrenovic T, McKee D, Zhang J, Griffith M, Cao X (2011) A stromal cell-derived factor-1 releasing matrix enhances the progenitor cell response and blood vessel growth in ischaemic skeletal muscle. Eur Cell Mater 22(109):e23
Law JX, Liau LL, Saim A, Yang Y, Idrus R (2017) Electrospun collagen nanofibers and their applications in skin tissue engineering. Tissue Eng Regener Med 14(6):699–718
Lee JM, Yeong WY (2016) Design and printing strategies in 3D bioprinting of cell-hydrogels: a review. Adv Healthc Mater 5(22):2856–2865
Lee C, Grodzinsky A, Spector M (2003) Biosynthetic response of passaged chondrocytes in a type II collagen scaffold to mechanical compression. J Biomed Mater Res Part A 64(3):560–569
Lee H, Kim W, Lee J, Yoo JJ, Kim GH, Lee SJ (2019) Effect of hierarchical scaffold consisting of aligned dECM Nanofibers and poly (lactide-co-glycolide) struts on the orientation and maturation of human muscle progenitor cells. ACS Appl Mater Interfaces 11(43):39449–39458
Levett PA, Melchels FP, Schrobback K, Hutmacher DW, Malda J, Klein TJ (2014) A biomimetic extracellular matrix for cartilage tissue engineering centered on photocurable gelatin, hyaluronic acid and chondroitin sulfate. Acta Biomater 10(1):214–223
Li WJ, Danielson KG, Alexander PG, Tuan RS (2003) Biological response of chondrocytes cultured in three-dimensional nanofibrous poly (ϵ-caprolactone) scaffolds. J Biomed Mater Res Part A 67(4):1105–1114
Li W-J, Tuli R, Okafor C, Derfoul A, Danielson KG, Hall DJ, Tuan RS (2005) A three-dimensional nanofibrous scaffold for cartilage tissue engineering using human mesenchymal stem cells. Biomaterials 26(6):599–609
Li H, Williams GR, Wu J, Lv Y, Sun X, Wu H, Zhu L-M (2017) Thermosensitive nanofibers loaded with ciprofloxacin as antibacterial wound dressing materials. Int J Pharm 517(1–2):135–147
Liao I-C, Leong KW (2011) Efficacy of engineered FVIII-producing skeletal muscle enhanced by growth factor-releasing co-axial electrospun fibers. Biomaterials 32(6):1669–1677
Liao CJ, Chen CF, Chen JH, Chiang SF, Lin YJ, Chang KY (2002) Fabrication of porous biodegradable polymer scaffolds using a solvent merging/particulate leaching method. J Biomed Mater Res 59(4):676–681
Liao N, Unnithan AR, Joshi MK, Tiwari AP, Hong ST, Park C-H, Kim CS (2015) Electrospun bioactive poly (ɛ-caprolactone)–cellulose acetate–dextran antibacterial composite mats for wound dressing applications. Colloids Surf A Physicochem Eng Asp 469:194–201
Liu Y, Skardal A, Shu XZ, Prestwich GD (2008) Prevention of peritendinous adhesions using a hyaluronan-derived hydrogel film following partial-thickness flexor tendon injury. J Orthop Res 26(4):562–569
Liu S, Zhao J, Ruan H, Tang T, Liu G, Yu D, Cui W, Fan C (2012) Biomimetic sheath membrane via electrospinning for antiadhesion of repaired tendon. Biomacromolecules 13(11):3611–3619
Liu Y, Zhou G, Liu Z, Guo M, Jiang X, Taskin MB, Zhang Z, Liu J, Tang J, Bai R (2017) Mussel inspired polynorepinephrine functionalized electrospun polycaprolactone microfibers for muscle regeneration. Sci Rep 7(1):1–10
Lü S, Gao C, Xu X, Bai X, Duan H, Gao N, Feng C, Xiong Y, Liu M (2015) Injectable and self-healing carbohydrate-based hydrogel for cell encapsulation. ACS Appl Mater Interfaces 7(23):13029–13037
MacNeil S (2008) Biomaterials for tissue engineering of skin. Mater Today 11(5):26–35
Man Z, Hu X, Liu Z, Huang H, Meng Q, Zhang X, Dai L, Zhang J, Fu X, Duan X (2016) Transplantation of allogenic chondrocytes with chitosan hydrogel-demineralized bone matrix hybrid scaffold to repair rabbit cartilage injury. Biomaterials 108:157–167
Martinello T, Bronzini I, Volpin A, Vindigni V, Maccatrozzo L, Caporale G, Bassetto F, Patruno M (2014) Successful recellularization of human tendon scaffolds using adipose-derived mesenchymal stem cells and collagen gel. J Tissue Eng Regen Med 8(8):612–619
Matsumura G, Miyagawa-Tomita S, Shin’oka T, Ikada Y, Kurosawa H (2003) First evidence that bone marrow cells contribute to the construction of tissue-engineered vascular autografts in vivo. Circulation 108(14):1729–1734
Menzoian JO, Koshar AL, Rodrigues N (2011) Alexis carrel, Rene Leriche, Jean Kunlin, and the history of bypass surgery. J Vasc Surg 54(2):571–574
Metcalfe AD, Ferguson MW (2007) Tissue engineering of replacement skin: the crossroads of biomaterials, wound healing, embryonic development, stem cells and regeneration. J R Soc Interface 4(14):413–437
Miguel SP, Ribeiro MP, Coutinho P, Correia IJ (2017) Electrospun polycaprolactone/aloe vera_chitosan nanofibrous asymmetric membranes aimed for wound healing applications. Polymers 9(5):183
Miguel SP, Figueira DR, Simões D, Ribeiro MP, Coutinho P, Ferreira P, Correia IJ (2018) Electrospun polymeric nanofibres as wound dressings: a review. Colloids Surf B: Biointerfaces 169:60–71
Mohabatpour F, Karkhaneh A, Sharifi AM (2016) A hydrogel/fiber composite scaffold for chondrocyte encapsulation in cartilage tissue regeneration. RSC Adv 6(86):83135–83145
Mondschein RJ, Kanitkar A, Williams CB, Verbridge SS, Long TE (2017) Polymer structure-property requirements for stereolithographic 3D printing of soft tissue engineering scaffolds. Biomaterials 140:170–188
Moshiri A, Oryan A, Meimandi-Parizi A (2015) Synthesis, development, characterization and effectiveness of bovine pure platelet gel-collagen-polydioxanone bioactive graft on tendon healing. J Cell Mol Med 19(6):1308–1332
Mouthuy P-A, Zargar N, Hakimi O, Lostis E, Carr A (2015) Fabrication of continuous electrospun filaments with potential for use as medical fibres. Biofabrication 7(2):025006
Naderi-Meshkin H, Andreas K, Matin MM, Sittinger M, Bidkhori HR, Ahmadiankia N, Bahrami AR, Ringe J (2014) Chitosan-based injectable hydrogel as a promising in situ forming scaffold for cartilage tissue engineering. Cell Biol Int 38(1):72–84
Naghashzargar E, Farè S, Catto V, Bertoldi S, Semnani D, Karbasi S, Tanzi MC (2015) Nano/micro hybrid scaffold of PCL or P3HB nanofibers combined with silk fibroin for tendon and ligament tissue engineering. J Appl Biomater Funct Mater 13(2):156–168
Nakayama KH, Alcazar C, Yang G, Quarta M, Paine P, Doan L, Davies A, Rando TA, Huang NF (2018) Rehabilitative exercise and spatially patterned nanofibrillar scaffolds enhance vascularization and innervation following volumetric muscle loss. NPJ Regen Med 3(1):1–8
Namba J, Shimada K, Saito M, Murase T, Yamada H, Yoshikawa H (2007) Modulation of peritendinous adhesion formation by alginate solution in a rabbit flexor tendon model. J Biomed Mater Res Part B 80(1):273–279
Narayanan N, Jiang C, Wang C, Uzunalli G, Whittern N, Chen D, Jones OG, Kuang S, Deng M (2020) Harnessing Fiber diameter-dependent effects of myoblasts toward biomimetic scaffold-based skeletal muscle regeneration. Front Bioeng Biotechnol 8:203
Nerurkar NL, Mauck RL, Elliott DM (2008) Integrating theoretical and experimental methods for functional tissue engineering of the annulus fibrosus. Spine 33(25):2691
Nerurkar NL, Elliott DM, Mauck RL (2010) Mechanical design criteria for intervertebral disc tissue engineering. J Biomech 43(6):1017–1030
Nöth U, Rackwitz L, Heymer A, Weber M, Baumann B, Steinert A, Schütze N, Jakob F, Eulert J (2007) Chondrogenic differentiation of human mesenchymal stem cells in collagen type I hydrogels. J Biomed Mater Res Part A 83(3):626–635
O'Halloran DM, Pandit AS (2007) Tissue-engineering approach to regenerating the intervertebral disc. Tissue Eng 13(8):1927–1954
Organization WHO (2010) Injuries and violence: the facts. WHO, Geneva
Oryan A, Kamali A, Moshiri A, Baharvand H, Daemi H (2018) Chemical crosslinking of biopolymeric scaffolds: current knowledge and future directions of crosslinked engineered bone scaffolds. Int J Biol Macromol 107:678–688
Pantelic MN, Larkin LM (2018) Stem cells for skeletal muscle tissue engineering. Tissue Eng Part B Rev 24(5):373–391
Pereira R, Carvalho A, Vaz DC, Gil M, Mendes A, Bártolo P (2013) Development of novel alginate based hydrogel films for wound healing applications. Int J Biol Macromol 52:221–230
Peterson GI, Schwartz JJ, Zhang D, Weiss BM, Ganter MA, Storti DW, Boydston AJ (2016) Production of materials with spatially-controlled cross-link density via vat photopolymerization. ACS Appl Mater Interfaces 8(42):29037–29043
Powell HM, Supp DM, Boyce ST (2008) Influence of electrospun collagen on wound contraction of engineered skin substitutes. Biomaterials 29(7):834–843
Pulkkinen H, Tiitu V, Valonen P, Jurvelin J, Rieppo L, Töyräs J, Silvast T, Lammi M, Kiviranta I (2013) Repair of osteochondral defects with recombinant human type II collagen gel and autologous chondrocytes in rabbit. Osteoarthr Cartil 21(3):481–490
Qazi TH, Mooney DJ, Pumberger M, Geissler S, Duda GN (2015) Biomaterials based strategies for skeletal muscle tissue engineering: existing technologies and future trends. Biomaterials 53:502–521
Qiu Y, Lim JJ, Scott L Jr, Adams RC, Bui HT, Temenoff JS (2011) PEG-based hydrogels with tunable degradation characteristics to control delivery of marrow stromal cells for tendon overuse injuries. Acta Biomater 7(3):959–966
Qu J, Zhao X, Liang Y, Zhang T, Ma PX, Guo B (2018) Antibacterial adhesive injectable hydrogels with rapid self-healing, extensibility and compressibility as wound dressing for joints skin wound healing. Biomaterials 183:185–199
Quapp K, Weiss J (1998) Material characterization of human medial collateral ligament. J Biomech Eng 120(6):757–763
Radhakrishnan J, Subramanian A, Krishnan UM, Sethuraman S (2017) Injectable and 3D bioprinted polysaccharide hydrogels: from cartilage to osteochondral tissue engineering. Biomacromolecules 18(1):1–26
Rhim C, Lowell DA, Reedy MC, Slentz DH, Zhang SJ, Kraus WE, Truskey GA (2007) Morphology and ultrastructure of differentiating three-dimensional mammalian skeletal muscle in a collagen gel. Muscle Nerve 36(1):71–80
Rho KS, Jeong L, Lee G, Seo B-M, Park YJ, Hong S-D, Roh S, Cho JJ, Park WH, Min B-M (2006) Electrospinning of collagen nanofibers: effects on the behavior of normal human keratinocytes and early-stage wound healing. Biomaterials 27(8):1452–1461
Rossi CA, Flaibani M, Blaauw B, Pozzobon M, Figallo E, Reggiani C, Vitiello L, Elvassore N, De Coppi P (2011) In vivo tissue engineering of functional skeletal muscle by freshly isolated satellite cells embedded in a photopolymerizable hydrogel. FASEB J 25(7):2296–2304
Rujitanaroj PO, Pimpha N, Supaphol P (2008) Wound-dressing materials with antibacterial activity from electrospun gelatin fiber mats containing silver nanoparticles. Polymer 49(21):4723–4732
Schmitt A, Rödel P, Anamur C, Seeliger C, Imhoff AB, Herbst E, Vogt S, van Griensven M, Winter G, Engert J (2015) Calcium alginate gels as stem cell matrix–making paracrine stem cell activity available for enhanced healing after surgery. PLoS One 10(3):e0118937
Schnabel LV, Lynch ME, van der Meulen MC, Yeager AE, Kornatowski MA, Nixon AJ (2009) Mesenchymal stem cells and insulin-like growth factor-I gene-enhanced mesenchymal stem cells improve structural aspects of healing in equine flexor digitorum superficialis tendons. J Orthop Res 27(10):1392–1398
Schneider DC (1983) Viscoelasticity and tearing strength of the human skin. University of California, Berkley, CA
Schneider U, Rackwitz L, Andereya S, Siebenlist S, Fensky F, Reichert J, Löer I, Barthel T, Rudert M, Nöth U (2011) A prospective multicenter study on the outcome of type I collagen hydrogel–based autologous chondrocyte implantation (CaReS) for the repair of articular cartilage defects in the knee. Am J Sports Med 39(12):2558–2565
Schuurman W, Levett PA, Pot MW, van Weeren PR, Dhert WJ, Hutmacher DW, Melchels FP, Klein TJ, Malda J (2013) Gelatin-methacrylamide hydrogels as potential biomaterials for fabrication of tissue-engineered cartilage constructs. Macromol Biosci 13(5):551–561
Seifu DG, Purnama A, Mequanint K, Mantovani D (2013) Small-diameter vascular tissue engineering. Nat Rev Cardiol 10(7):410
Shamsah AH, Cartmell SH, Richardson SM, Bosworth LA (2019a) Mimicking the annulus Fibrosus using electrospun polyester blended scaffolds. Nano 9(4):537
Shamsah AH, Cartmell SH, Richardson SM, Bosworth LA (2019b) Tissue engineering the annulus Fibrosus using 3D rings of electrospun PCL: PLLA angle-ply Nanofiber sheets. Front Bioeng Biotechnol 7:437
Shinoka T, Breuer CK, Tanel RE, Zund G, Miura T, Ma PX, Langer R, Vacanti JP, Mayer JE (1995) Tissue engineering heart valves: valve leaflet replacement study in a lamb model. Ann Thorac Surg 60:S513–S516
Silva JC, Udangawa RN, Chen J, Mancinelli CD, Garrudo FF, Mikael PE, Cabral JM, Ferreira FC, Linhardt RJ (2020) Kartogenin-loaded coaxial PGS/PCL aligned nanofibers for cartilage tissue engineering. Mater Sci Eng C 107:110291
Simon S (1998) Muscles: our muscular system. HarperCollins Publishers, New York
Smith A, Passey S, Greensmith L, Mudera V, Lewis M (2012) Characterization and optimization of a simple, repeatable system for the long term in vitro culture of aligned myotubes in 3D. J Cell Biochem 113(3):1044–1053
Smoak MM, Han A, Watson E, Kishan A, Grande-Allen KJ, Cosgriff-Hernandez E, Mikos AG (2019) Fabrication and characterization of electrospun decellularized muscle-derived scaffolds. Tissue Eng Part C Methods 25(5):276–287
Stegemann JP, Kaszuba SN, Rowe SL (2007) Advances in vascular tissue engineering using protein-based biomaterials. Tissue Eng 13(11):2601–2613
Sun X, Yin H, Wang Y, Lu J, Shen X, Lu C, Tang H, Meng H, Yang S, Yu W (2018) In situ articular cartilage regeneration through endogenous reparative cell homing using a functional bone marrow-specific scaffolding system. ACS Appl Mater Interfaces 10(45):38715–38728
Sundaramurthi D, Krishnan UM, Sethuraman S (2014) Electrospun nanofibers as scaffolds for skin tissue engineering. Polym Rev 54(2):348–376
Tang X, Saveh-Shemshaki N, Kan H-M, Khan Y, Laurencin CT (2019) Biomimetic Electroconductive Nanofibrous matrices for skeletal muscle regenerative engineering. Regen Eng Transl Med 6:228–237
Thu H-E, Zulfakar MH, Ng S-F (2012) Alginate based bilayer hydrocolloid films as potential slow-release modern wound dressing. Int J Pharm 434(1–2):375–383
Tiburcy M, Meyer T, Soong PL, Zimmermann W-H (2014) Collagen-based engineered heart muscle. In: Cardiac tissue engineering. Springer, Cham, pp 167–176
Tillman BW, Yazdani SK, Lee SJ, Geary RL, Atala A, Yoo JJ (2009) The in vivo stability of electrospun polycaprolactone-collagen scaffolds in vascular reconstruction. Biomaterials 30(4):583–588
Uppal R, Ramaswamy GN, Arnold C, Goodband R, Wang Y (2011) Hyaluronic acid nanofiber wound dressing—production, characterization, and in vivo behavior. J Biomed Mater Res B Appl Biomater 97(1):20–29
Uysal O, Arslan E, Gulseren G, Kilinc MC, Dogan I, Ozalp H, Caglar YS, Guler MO, Tekinay AB (2019) Collagen peptide presenting Nanofibrous scaffold for intervertebral disc regeneration. ACS Applied Bio Materials 2(4):1686–1695
Vacanti JP, Langer R (1999) Tissue engineering: the design and fabrication of living replacement devices for surgical reconstruction and transplantation. Lancet 354:S32–S34
Vandenburgh HH, Karlisch P, Farr L (1988) Maintenance of highly contractile tissue-cultured avian skeletal myotubes in collagen gel. In Vitro Cell Dev Biol 24(3):166–174
Venugopal JR, Zhang Y, Ramakrishna S (2006) In vitro culture of human dermal fibroblasts on electrospun polycaprolactone collagen nanofibrous membrane. Artif Organs 30(6):440–446
Vijayavenkataraman S, Lu W, Fuh J (2016) 3D bioprinting of skin: a state-of-the-art review on modelling, materials, and processes. Biofabrication 8(3):032001
von Burkersroda F, Schedl L, Göpferich A (2002) Why degradable polymers undergo surface erosion or bulk erosion. Biomaterials 23(21):4221–4231
Wakitani S, Goto T, Young RG, Mansour JM, Goldberg VM, Caplan AI (1998) Repair of large full-thickness articular cartilage defects with allograft articular chondrocytes embedded in a collagen gel. Tissue Eng 4(4):429–444
Walden G, Liao X, Donell S, Raxworthy MJ, Riley GP, Saeed A (2017) A clinical, biological, and biomaterials perspective into tendon injuries and regeneration. Tissue Eng Part B Rev 23(1):44–58
Wang Y, Zhang C-L, Zhang Q, Li P (2011) Composite electrospun nanomembranes of fish scale collagen peptides/chito-oligosaccharides: antibacterial properties and potential for wound dressing. Int J Nanomed 6:667
Wang L-S, Du C, Toh WS, Wan AC, Gao SJ, Kurisawa M (2014a) Modulation of chondrocyte functions and stiffness-dependent cartilage repair using an injectable enzymatically crosslinked hydrogel with tunable mechanical properties. Biomaterials 35(7):2207–2217
Wang L, Cao L, Shansky J, Wang Z, Mooney D, Vandenburgh H (2014b) Minimally invasive approach to the repair of injured skeletal muscle with a shape-memory scaffold. Mol Ther 22(8):1441–1449
Wang Z, Zhang W, Xie C, Wen F, Ma C, Lin N, San Thian E, Wang X (2019) Geometric anisotropy on biomaterials surface for vascular scaffold design: engineering and biological advances. J Phys: Mater 2(3):032003
Wegst U, Ashby M (2004) The mechanical efficiency of natural materials. Philos Mag 84(21):2167–2186
Wehrhan F, Nkenke E, Melnychenko I, Amann K, Schlegel KA, Goerlach C, Zimmermann WH, Schultze-Mosgau S (2010) Skin repair using a porcine collagen I/III membrane—vascularization and epithelization properties. Dermatol Surg 36(6):919–930
Wise SG, Byrom MJ, Waterhouse A, Bannon PG, Ng MK, Weiss AS (2011) A multilayered synthetic human elastin/polycaprolactone hybrid vascular graft with tailored mechanical properties. Acta Biomater 7(1):295–303
Wright L, McKeon-Fischer K, Cui Z, Nair L, Freeman J (2014) PDLA/PLLA and PDLA/PCL nanofibers with a chitosan-based hydrogel in composite scaffolds for tissue engineered cartilage. J Tissue Eng Regen Med 8(12):946–954
Xie J, MacEwan MR, Ray WZ, Liu W, Siewe DY, Xia Y (2010) Radially aligned, electrospun nanofibers as dural substitutes for wound closure and tissue regeneration applications. ACS Nano 4(9):5027–5036
Yang Q, Xu H, Hurday S, Xu B (2016) Construction strategy and progress of whole intervertebral disc tissue engineering. Orthop Surg 8(1):11–18
Yang F, Tadepalli V, Wiley BJ (2017) 3D printing of a double network hydrogel with a compression strength and elastic modulus greater than those of cartilage. ACS Biomater Sci Eng 3(5):863–869
Yang Z, Cao H, Gao S, Yang M, Lyu J, Tang K (2018) Effect of tendon stem cells in chitosan/β-Glycerophosphate/collagen hydrogel on Achilles tendon healing in a rat model. Med Sci Monit Int Med J Exp Clin Res 24:4633
Ye H, Zhang K, Kai D, Li Z, Loh XJ (2018) Polyester elastomers for soft tissue engineering. Chem Soc Rev 47(12):4545–4580
Yokoyama A, Sekiya I, Miyazaki K, Ichinose S, Hata Y, Muneta T (2005) In vitro cartilage formation of composites of synovium-derived mesenchymal stem cells with collagen gel. Cell Tissue Res 322(2):289–298
Yuan L, Li B, Yang J, Ni Y, Teng Y, Guo L, Fan H, Fan Y, Zhang X (2016) Effects of composition and mechanical property of injectable collagen I/II composite hydrogels on chondrocyte behaviors. Tissue Eng A 22(11–12):899–906
Yuan D, Chen Z, Xiang X, Deng S, Liu K, Xiao D, Deng L, Feng G (2019) The establishment and biological assessment of a whole tissue-engineered intervertebral disc with PBST fibers and a chitosan hydrogel in vitro and in vivo. J Biomed Mater Res B Appl Biomater 107(7):2305–2316
Zhang Y, Venugopal J, Huang Z-M, Lim CT, Ramakrishna S (2006) Crosslinking of the electrospun gelatin nanofibers. Polymer 47(8):2911–2917
Zhang Y, Yu J, Ren K, Zuo J, Ding J, Chen X (2019) Thermosensitive hydrogels as scaffolds for cartilage tissue engineering. Biomacromolecules 20(4):1478–1492
Zhao X, Lang Q, Yildirimer L, Lin ZY, Cui W, Annabi N, Ng KW, Dokmeci MR, Ghaemmaghami AM, Khademhosseini A (2016) Photocrosslinkable gelatin hydrogel for epidermal tissue engineering. Adv Healthc Mater 5(1):108–118
Zhao X, Sun X, Yildirimer L, Lang Q, Lin ZYW, Zheng R, Zhang Y, Cui W, Annabi N, Khademhosseini A (2017) Cell infiltrative hydrogel fibrous scaffolds for accelerated wound healing. Acta Biomater 49:66–77
Zhou Y, Yang D, Chen X, Xu Q, Lu F, Nie J (2008) Electrospun water-soluble carboxyethyl chitosan/poly (vinyl alcohol) nanofibrous membrane as potential wound dressing for skin regeneration. Biomacromolecules 9(1):349–354
Zhu Y, Cao Y, Pan J, Liu Y (2010) Macro-alignment of electrospun fibers for vascular tissue engineering. J Biomed Mater Res Part B 92(2):508–516
Acknowledgement
Author C.K.B.V thank the Indian Institute of Technology Madras, India, for the financial support in terms of fellowship and infrastructure support. We also thank the Science & Engineering Research Board (SERB), Department of Science and Technology (Project no. ECR/2017/003064), Government of India for financial support.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Balavigneswaran, C.K., Muthuvijayan, V. (2021). Biomaterials for Soft Tissue Engineering: Concepts, Methods, and Applications. In: Bhaskar, B., Sreenivasa Rao, P., Kasoju, N., Nagarjuna, V., Baadhe, R.R. (eds) Biomaterials in Tissue Engineering and Regenerative Medicine. Springer, Singapore. https://doi.org/10.1007/978-981-16-0002-9_11
Download citation
DOI: https://doi.org/10.1007/978-981-16-0002-9_11
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-16-0001-2
Online ISBN: 978-981-16-0002-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)