Abstract
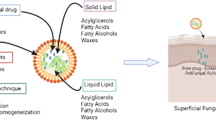
Lipid nanocarriers can be an effective drug delivery system for the treatment of skin infections by overcoming the pitfalls associated with conventional topical formulations and offer various advantages such as improved skin permeability, targeted delivery, minimal side effects, increased solubility and bioavailability. The major hurdle in current scenario is antimicrobial resistance which has led to treatment failure and high mortality. Lipid nanocarriers, in this context can be instrumental in the successful eradication of drug-resistant strains in the skin by fusing with cell membrane of infectious microbes and providing an intimate contact and delivering the anti-infective agent directly to the target site. Various lipid-based carriers include liposomes, transferosomes, ethosomes, solid lipid nanoparticles, nanostructured lipid carriers, microemulsion and nanoemulsion. This book chapter summarizes in brief the skin structure and various type of skin infections and then comprehensively describes various lipid nanocarriers and their application in the treatment of cutaneous infections.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Lam P, Lee K, Wong R, Cheng G, Bian Z, Chui C et al (2018) Recent advances on topical antimicrobials for skin and soft tissue infections and their safety concerns. Crit Rev Microbiol 44(1):40–78
Thakur K, Sharma G, Singh B, Chhibber S, Katare OP (2018a) Current state of nanomedicines in the treatment of topical infectious disorders. Recent Pat Antiinfect Drug Discov 13(2):127–150
Roberts M, Mohammed Y, Pastore M, Namjoshi S, Yousef S, Alinaghi A et al (2017) Topical and cutaneous delivery using nanosystems. J Control Release 247:86–105
Desai P, Patlolla RR, Singh M (2010) Interaction of nanoparticles and cell-penetrating peptides with skin for transdermal drug delivery. Mol Membr Biol 27(7):247–259
Zhang L, Jiang Y, Ding Y, Povey M, York D (2007) Investigation into the antibacterial behaviour of suspensions of ZnO nanoparticles (ZnO nanofluids). J Nanopart Res 9(3):479–489
Lane ME (2013) Skin penetration enhancers. Int J Pharm 447(1–2):12–21
Williams A, Barry B (2012) Penetration enhancers. Adv Drug Deliv Rev 64:128–137
Azagury A, Khoury L, Enden G, Kost J (2014) Ultrasound mediated transdermal drug delivery. Adv Drug Deliv Rev 72:127–143
Han T, Das DB (2015) Potential of combined ultrasound and microneedles for enhanced transdermal drug permeation: a review. Eur J Pharm Biopharm 89:312–328
Nawaz A, Wong TW (2017) Microwave as skin permeation enhancer for transdermal drug delivery of chitosan-5-fluorouracil nanoparticles. Carbohydr Polym 157:906–919
Shahzad Y, Louw R, Gerber M, Du Plessis J (2015) Breaching the skin barrier through temperature modulations. J Control Release 202:1–13
Wang Y, Thakur R, Fan Q, Michniak B (2005) Transdermal iontophoresis: combination strategies to improve transdermal iontophoretic drug delivery. Eur J Pharm Biopharm 60(2):179–191
Garcês A, Amaral M, Lobo JS, Silva A (2018) Formulations based on solid lipid nanoparticles (SLN) and nanostructured lipid carriers (NLC) for cutaneous use: A review. Eur J Pharm Sci 112:159–167
Jain S, Patel N, Shah MK, Khatri P, Vora N (2017) Recent advances in lipid-based vesicles and particulate carriers for topical and transdermal application. J Pharm Sci 106(2):423–445
Sala M, Diab R, Elaissari A, Fessi H (2018) Lipid nanocarriers as skin drug delivery systems: Properties, mechanisms of skin interactions and medical applications. Int J Pharm 535(1–2):1–17
Al-mahallawi AM, Abdelbary AA, Aburahma MH (2015) Investigating the potential of employing bilosomes as a novel vesicular carrier for transdermal delivery of tenoxicam. Int J Pharm 485(1–2):329–340
Barua S, Mitragotri S (2014) Challenges associated with penetration of nanoparticles across cell and tissue barriers: a review of current status and future prospects. Nano Today 9(2):223–243
Baker C, Pradhan A, Pakstis L, Pochan DJ, Shah SI (2005) Synthesis and antibacterial properties of silver nanoparticles. J Nanosci Nanotechnol 5(2):244–249
McGrath J, Eady R, Pope F (2004) Anatomy and organization of human skin. In: Rook’s textbook of dermatology, vol 10. Wiley, Hoboken, p 9781444317633
Agache P (2004) Metrology of the stratum corneum. In: Humbert et al (eds) Measuring the skin. Springer International Publishing, Switzerland, pp 101–111
Gray G, White R, Williams R, Yardleymrc H (1982) Lipid composition of the superficial stratum corneum cells of pig epidermis. Br J Dermatol 106(1):59–63
Wertz PW, Swartzendruber DC, Kitko DJ, Madison KC, Downing DT (1989) The role of the corneocyte lipid envelopes in cohesion of the stratum corneum. J Investig Dermatol 93(1):169–172
Gentilhomme E, Neveux Y (2004) Epidermal physiology. In: Humbert et al (eds) Measuring the skin. Springer International Publishing, Switzerland, p 165
Burgeson RE, Christiano AM (1997) The dermal—epidermal junction. Curr Opin Cell Biol 9(5):651–658
Bisno AL, Stevens DL (1996) Streptococcal infections of skin and soft tissues. N Engl J Med 334(4):240–246
Callahan EF, Adal KA, Tomecki KJ (2000) Cutaneous (non-HIV) infections. Dermatol Clin 18(3):497–508
Hay R (1990) Overview of studies of fluconazole in oropharyngeal candidiasis. Rev Infect Dis 12(Supplement_3):S334–S3S7
Drake LA, Dinehart SM, Farmer ER, Goltz RW, Graham GF, Hordinsky MK et al (1996) Guidelines of care for superficial mycotic infectionsof the skin: Pityriasis (tinea) versicolor. J Am Acad Dermatol 34(2):287–289
Memar O, Tyring SK (1995) Cutaneous viral infections. J Am Acad Dermatol 33(2):279–287
Sterling J, Handfield-Jones S, Hudson P (2001) Guidelines for the management of cutaneous warts. Br J Dermatol 144(1):4–11
Reithinger R, Dujardin J-C, Louzir H, Pirmez C, Alexander B, Brooker S (2007) Cutaneous leishmaniasis. Lancet Infect Dis 7(9):581–596
Pople PV, Singh KK (2010) Targeting tacrolimus to deeper layers of skin with improved safety for treatment of atopic dermatitis. Int J Pharm 398(1–2):165–178
Teichmann A, Heuschkel S, Jacobi U, Presse G, Neubert RH, Sterry W et al (2007) Comparison of stratum corneum penetration and localization of a lipophilic model drug applied in an o/w microemulsion and an amphiphilic cream. Eur J Pharm Biopharm 67(3):699–706
Jadhav M, Kalhapure RS, Rambharose S, Mocktar C, Singh S, Kodama T et al (2018) Novel lipids with three C18-fatty acid chains and an amino acid head group for pH-responsive and sustained antibiotic delivery. Chem Phys Lipids 212:12–25
Hasanpouri A, Lotfipour F, Ghanbarzadeh S, Hamishehkar H (2018) Improvement of dermal delivery of tetracycline using vesicular nanostructures. Res Pharm Sci 13(5):385
Zhang L, Pornpattananangkul D, Hu C-M, Huang C-M (2010) Development of nanoparticles for antimicrobial drug delivery. Curr Med Chem 17(6):585–594
Luan L, Chi Z, Liu C (2019) Chinese white wax solid lipid nanoparticles as a novel nanocarrier of curcumin for inhibiting the formation of Staphylococcus aureus biofilms. Nano 9(5):763
Bangham AD, Horne R (1964) Negative staining of phospholipids and their structural modification by surface-active agents as observed in the electron microscope. J Mol Biol 8(5):660–IN10
Rahman M, Alam K, Beg S, Anwar F, Kumar V (2019) Liposomes as topical drug delivery systems: state of the arts. In: Biomedical applications of nanoparticles. Elsevier, Amsterdam, pp 149–161
Mezei M, Gulasekharam V (1980) Liposomes-a selective drug delivery system for the topical route of administration I. Lotion dosage form. Life Sci 26(18):1473–1477
Egbaria K, Weiner N (1990) Liposomes as a topical drug delivery system. Adv Drug Deliv Rev 5(3):287–300
Rukavina Z, Vanić Ž (2016) Current trends in development of liposomes for targeting bacterial biofilms. Pharmaceutics 8(2):18
Boakye CH, Patel K, Singh M (2015) Doxorubicin liposomes as an investigative model to study the skin permeation of nanocarriers. Int J Pharm 489(1–2):106–116
Verma DD, Verma S, Blume G, Fahr A (2003) Particle size of liposomes influences dermal delivery of substances into skin. Int J Pharm 258(1–2):141–151
Madan S, Nehate C, Barman TK, Rathore AS, Koul V (2019) Design, preparation, and evaluation of liposomal gel formulations for treatment of acne: in vitro and in vivo studies. Drug Dev Ind Pharm 45(3):395–404
Moosavian SA, Fallah M, Jaafari MR (2019) The activity of encapsulated meglumine antimoniate in stearylamine-bearing liposomes against cutaneous leishmaniasis in BALB/c mice. Exp Parasitol 200:30–35
Kavian Z, Alavizade SH, Golmohamadzadeh S, Badiee A, Khamesipour A, Jaafari MR (2019) Development of topical liposomes containing miltefosine for the treatment of Leishmania major infection in susceptible BALB/c mice. Acta Trop. https://doi.org/10.1016/j.actatropica.2019.05.018
Rukavina Z, Klarić MŠ, Filipović-Grčić J, Lovrić J, Vanić Ž (2018) Azithromycin-loaded liposomes for enhanced topical treatment of methicillin-resistant Staphyloccocus aureus (MRSA) infections. Int J Pharm 553(1–2):109–119
Chhibber S, Kaur J, Kaur S (2018) Liposome Entrapment of Bacteriophages Improves Wound Healing in a Diabetic Mouse MRSA Infection. Front Microbiol 9:561
Hsu CY, Yang SC, Sung CT, Weng YH, Fang JY (2017) Anti-MRSA malleable liposomes carrying chloramphenicol for ameliorating hair follicle targeting. Int J Nanomedicine 12:8227–8238
Tanriverdi ST, Hilmioglu Polat S, Yesim Metin D, Kandiloglu G, Ozer O (2016) Terbinafine hydrochloride loaded liposome film formulation for treatment of onychomycosis: in vitro and in vivo evaluation. J Liposome Res 26(2):163–173
Nunes PS, Rabelo AS, Souza JC, Santana BV, da Silva TM, Serafini MR et al (2016) Gelatin-based membrane containing usnic acid-loaded liposome improves dermal burn healing in a porcine model. Int J Pharm 513(1–2):473–482
Tanriverdi ST, Ozer O (2013) Novel topical formulations of Terbinafine-HCl for treatment of onychomycosis. Eur J Pharm Sci 48(4–5):628–636
Gupta M, Goyal AK, Paliwal SR, Paliwal R, Mishra N, Vaidya B et al (2010) Development and characterization of effective topical liposomal system for localized treatment of cutaneous candidiasis. J Liposome Res 20(4):341–350
Touitou E, Dayan N, Bergelson L, Godin B, Eliaz M (2000) Ethosomes - novel vesicular carriers for enhanced delivery: characterization and skin penetration properties. J Control Release 65(3):403–418
Shetty S, Jose J, Kumar L, Charyulu RN (2019) Novel ethosomal gel of clove oil for the treatment of cutaneous candidiasis. J Cosmet Dermatol 18(3):862–869
Faisal W, Soliman GM, Hamdan AM (2018) Enhanced skin deposition and delivery of voriconazole using ethosomal preparations. J Liposome Res 28(1):14–21
Marto J, Vitor C, Guerreiro A, Severino C, Eleuterio C, Ascenso A et al (2016) Ethosomes for enhanced skin delivery of griseofulvin. Colloids Surf B Biointerfaces 146:616–623
Iizhar SA, Syed IA, Satar R, Ansari SA (2016) In vitro assessment of pharmaceutical potential of ethosomes entrapped with terbinafine hydrochloride. J Adv Res 7(3):453–461
Godin B, Touitou E, Rubinstein E, Athamna A, Athamna M (2005) A new approach for treatment of deep skin infections by an ethosomal antibiotic preparation: an in vivo study. J Antimicrob Chemother 55(6):989–994
Cevc G, Blume G (1992) Lipid vesicles penetrate into intact skin owing to the transdermal osmotic gradients and hydration force. Biochim Biophys Acta 1104(1):226–232
Cevc G, Blume G, Schätzlein A, Gebauer D, Paul A (1996) The skin: a pathway for systemic treatment with patches and lipid-based agent carriers. Adv Drug Deliv Rev 18(3):349–378
Trotta M, Peira E, Carlotti ME, Gallarate M (2004) Deformable liposomes for dermal administration of methotrexate. Int J Pharm 270(1–2):119–125
Elsayed MM, Abdallah OY, Naggar VF, Khalafallah NM (2007) Lipid vesicles for skin delivery of drugs: reviewing three decades of research. Int J Pharm 332(1–2):1–16
Jain S, Jain P, Umamaheshwari R, Jain N (2003) Transfersomes—a novel vesicular carrier for enhanced transdermal delivery: development, characterization, and performance evaluation. Drug Dev Ind Pharm 29(9):1013–1026
Qushawy M, Nasr A, Abd-Alhaseeb M, Swidan S (2018) Design, optimization and characterization of a transfersomal gel using miconazole nitrate for the treatment of candida skin infections. Pharmaceutics 10(1). https://doi.org/10.3390/pharmaceutics10010026
Pandit J, Garg M, Jain NK (2014) Miconazole nitrate bearing ultraflexible liposomes for the treatment of fungal infection. J Liposome Res 24(2):163–169
Chhibber S, Shukla A, Kaur S (2017) Transfersomal phage cocktail is an effective treatment against methicillin-resistant Staphylococcus aureus-mediated skin and soft tissue infections. Antimicrob Agents Chemother 61(10):e02146–e02116
Abdellatif MM, Khalil IA, Khalil MAF (2017) Sertaconazole nitrate loaded nanovesicular systems for targeting skin fungal infection: In-vitro, ex-vivo and in-vivo evaluation. Int J Pharm 527(1–2):1–11
Li C, Zhang X, Huang X, Wang X, Liao G, Chen Z (2013) Preparation and characterization of flexible nanoliposomes loaded with daptomycin, a novel antibiotic, for topical skin therapy. Int J Nanomedicine 8:1285–1292
Ashtikar M, Nagarsekar K, Fahr A (2016) Transdermal delivery from liposomal formulations–Evolution of the technology over the last three decades. J Control Release 242:126–140
Gangwar M, Singh R, Goel R, Nath G (2012) Recent advances in various emerging vescicular systems: An overview. Asian Pac J Trop Biomed 2(2):S1176–S1S88
Kumar GP, Rajeshwarrao P (2011) Nonionic surfactant vesicular systems for effective drug delivery—an overview. Acta Pharm Sin B 1(4):208–219
Sohrabi S, Haeri A, Mahboubi A, Mortazavi A, Dadashzadeh S (2016) Chitosan gel-embedded moxifloxacin niosomes: an efficient antimicrobial hybrid system for burn infection. Int J Biol Macromol 85:625–633
Alomrani AH, Al-Agamy MH, Badran MM (2015) In vitro skin penetration and antimycotic activity of itraconazole loaded niosomes: various non-ionic surfactants. J Drug Deliv Sci Technol 28:37–45
Müller RH, Mäder K, Gohla S (2000) Solid lipid nanoparticles (SLN) for controlled drug delivery–a review of the state of the art. Eur J Pharm Biopharm 50(1):161–177
Doktorovová S, Kovačević AB, Garcia ML, Souto EB (2016) Preclinical safety of solid lipid nanoparticles and nanostructured lipid carriers: current evidence from in vitro and in vivo evaluation. Eur J Pharm Biopharm 108:235–252
Guimarães KL, Ré MI (2011) Lipid nanoparticles as carriers for cosmetic ingredients: the first (SLN) and the second generation (NLC). In: Nanocosmetics and nanomedicines. Springer, New York, pp 101–122
López-García R, Ganem-Rondero A (2015) Solid lipid nanoparticles (SLN) and nanostructured lipid carriers (NLC): occlusive effect and penetration enhancement ability. J Cosmet Dermatol Sci Appl 5(02):62
Muller RH, Radtke M, Wissing SA (2002) Nanostructured lipid matrices for improved microencapsulation of drugs. Int J Pharm 242(1–2):121–128
Montenegro L, Lai F, Offerta A, Sarpietro MG, Micicche L, Maccioni AM et al (2016) From nanoemulsions to nanostructured lipid carriers: A relevant development in dermal delivery of drugs and cosmetics. J Drug Deliv Sci Technol 32:100–112
Müller RH, Alexiev U, Sinambela P, Keck CM (2016) Nanostructured lipid carriers (NLC): the second generation of solid lipid nanoparticles. In: Percutaneous penetration enhancers chemical methods in penetration enhancement. Springer, New York, pp 161–185
Beloqui A, Solinís MÁ, Rodríguez-Gascón A, Almeida AJ, Préat V (2016) Nanostructured lipid carriers: Promising drug delivery systems for future clinics. Nanomedicine 12(1):143–161
El-Housiny S, Shams Eldeen MA, El-Attar YA, Salem HA, Attia D, Bendas ER et al (2018) Fluconazole-loaded solid lipid nanoparticles topical gel for treatment of pityriasis versicolor: formulation and clinical study. Drug Deliv 25(1):78–90
Kakadia PG, Conway BR (2018) Solid lipid nanoparticles for targeted delivery of triclosan into skin for infection prevention. J Microencapsul 35(7–8):695–704
Vaghasiya H, Kumar A, Sawant K (2013) Development of solid lipid nanoparticles based controlled release system for topical delivery of terbinafine hydrochloride. Eur J Pharm Sci 49(2):311–322
Bhalekar MR, Pokharkar V, Madgulkar A, Patil N, Patil N (2009) Preparation and evaluation of miconazole nitrate-loaded solid lipid nanoparticles for topical delivery. AAPS PharmSciTech 10(1):289–296
Jain S, Jain S, Khare P, Gulbake A, Bansal D, Jain SK (2010) Design and development of solid lipid nanoparticles for topical delivery of an anti-fungal agent. Drug Deliv 17(6):443–451
Lv Q, Yu A, Xi Y, Li H, Song Z, Cui J et al (2009) Development and evaluation of penciclovir-loaded solid lipid nanoparticles for topical delivery. Int J Pharm 372(1–2):191–198
Lai F, Sinico C, De Logu A, Zaru M, Müller RH, Fadda AM (2007) SLN as a topical delivery system for Artemisia arborescens essential oil: in vitro antiviral activity and skin permeation study. Int J Nanomedicine 2(3):419
Carbone C, Teixeira M, Sousa M, Martins-Gomes C, Silva AM, Souto EMB et al (2019) Clotrimazole-loaded mediterranean essential oils NLC: a synergic treatment of candida skin infections. Pharmaceutics 11(5):231
Khezri K, Farahpour MR, Mounesi RS (2019) Accelerated infected wound healing by topical application of encapsulated Rosemary essential oil into nanostructured lipid carriers. Artif Cells Nanomed Biotechnol 47(1):980–988
Ghodrati M, Farahpour MR, Hamishehkar H (2019) Encapsulation of Peppermint essential oil in nanostructured lipid carriers: In-vitro antibacterial activity and accelerative effect on infected wound healing. Colloids Surf A Physicochem Eng Asp 564:161–169
Alalaiwe A, Wang P-W, Lu P-L, Chen Y-P, Fang J-Y, Yang S-C (2018) Synergistic anti-MRSA activity of cationic nanostructured lipid carriers in combination with oxacillin for cutaneous application. Front Microbiol 9:1493
Gaba B, Fazil M, Khan S, Ali A, Baboota S, Ali J (2015) Nanostructured lipid carrier system for topical delivery of terbinafine hydrochloride. Bull Fac Pharm Cairo Univ 53(2):147–159
Song SH, Lee KM, Kang JB, Lee SG, Kang MJ, Choi YW (2014) Improved skin delivery of voriconazole with a nanostructured lipid carrier-based hydrogel formulation. Chem Pharm Bull 62(8):793–798
Hoar T, Schulman J (1943) Transparent water-in-oil dispersions: the oleopathic hydro-micelle. Nature 152(3847):102
Kreilgaard M, Kemme MJ, Burggraaf J, Schoemaker RC, Cohen AF (2001) Influence of a microemulsion vehicle on cutaneous bioequivalence of a lipophilic model drug assessed by microdialysis and pharmacodynamics. Pharm Res 18(5):593–599
Shukla A, Janich M, Jahn K, Neubert RH (2003) Microemulsions for dermal drug delivery studied by dynamic light scattering: effect of interparticle interactions in oil-in-water microemulsions. J Pharm Sci 92(4):730–738
Al-Adham I, Khalil E, Al-Hmoud N, Kierans M, Collier P (2000) Microemulsions are membrane-active, antimicrobial, self-preserving systems. J Appl Microbiol 89(1):32–39
Solans C, Izquierdo P, Nolla J, Azemar N, Garcia-Celma M (2005) Nano-emulsions. Curr Opin Colloid Interface Sci 10(3–4):102–110
Calderilla-Fajardo S, Cazares-Delgadillo J, Villalobos-Garcia R, Quintanar-Guerrero D, Ganem-Quintanar A, Robles R (2006) Influence of sucrose esters on the in vivo percutaneous penetration of octyl methoxycinnamate formulated in nanocapsules, nanoemulsion, and emulsion. Drug Dev Ind Pharm 32(1):107–113
Mou D, Chen H, Du D, Mao C, Wan J, Xu H et al (2008) Hydrogel-thickened nanoemulsion system for topical delivery of lipophilic drugs. Int J Pharm 353(1–2):270–276
Talaat SM, Elnaggar YS, Abdalla OY (2019) Lecithin microemulsion lipogels versus conventional gels for skin targeting of terconazole: in vitro, ex vivo, and in vivo investigation. AAPS PharmSciTech 20(4):161
Kaur A, Sharma G, Gupta V, Ratho RK, Katare OP (2018) Enhanced acyclovir delivery using w/o type microemulsion: preclinical assessment of antiviral activity using murine model of zosteriform cutaneous HSV-1 infection. Artif Cells Nanomed Biotechnol 46(2):346–354
Alam MA, Al-Janoobi FI, Alzahrani KA, Al-Agamy MH, Abdelgalil AA, Al-Mohizea AM (2017) In-vitro efficacies of topical microemulsions of clotrimazole and ketoconazole; and in-vivo performance of clotrimazole microemulsion. J Drug Deliv Sci Technol 39:408–416
Wan T, Xu T, Pan J, Qin M, Pan W, Zhang G et al (2015) Microemulsion based gel for topical dermal delivery of pseudolaric acid B: in vitro and in vivo evaluation. Int J Pharm 493(1–2):111–120
Chhibber T, Wadhwa S, Chadha P, Sharma G, Katare OP (2015) Phospholipid structured microemulsion as effective carrier system with potential in methicillin sensitive Staphylococcus aureus (MSSA) involved burn wound infection. J Drug Target 23(10):943–952
Ramteke P, Pandey AC, Pandey H (2019) Evaluation of antifungal activity of blended cinnamon oil and usnic acid nanoemulsion using candidiasis and dermatophytosis models. Biocatal Agric Biotechnol 18:101062
Thakur K, Sharma G, Singh B, Jain A, Tyagi R, Chhibber S et al (2018b) Cationic-bilayered nanoemulsion of fusidic acid: an investigation on eradication of methicillin-resistant Staphylococcus aureus 33591 infection in burn wound. Nanomedicine 13(8):825–847
Sosa L, Clares B, Alvarado HL, Bozal N, Domenech O, Calpena AC (2017) Amphotericin B releasing topical nanoemulsion for the treatment of candidiasis and aspergillosis. Nanomedicine 13(7):2303–2312
Thomas L, Zakir F, Mirza MA, Anwer MK, Ahmad FJ, Iqbal Z (2017) Development of curcumin loaded chitosan polymer based nanoemulsion gel: In vitro, ex vivo evaluation and in vivo wound healing studies. Int J Biol Macromol 101:569–579
Cao Z, Spilker T, Fan Y, Kalikin LM, Ciotti S, LiPuma JJ et al (2017) Nanoemulsion is an effective antimicrobial for methicillin-resistant Staphylococcus aureus in infected wounds. Nanomedicine 12(10):1177–1185
Kelmann RG, Colombo M, Lopes SCDA, Nunes RJ, Pistore M, Agnol DD et al (2016) Pentyl gallate nanoemulsions as potential topical treatment of herpes labialis. J Pharm Sci 105(7):2194–2203
Karri VNR, Raman SK, Kuppusamy G, Mulukutla S, Ramaswamy S, Malayandi R (2015) Terbinafine hydrochloride loaded nanoemulsion based gel for topical application. J Pharm Investig 45(1):79–89
Acknowledgement
The author, Karan Razdan, acknowledges the Department of Science and Technology, New Delhi, India, for their financial assistance as DST INSPIRE JRF (IF170172) and is grateful to Commonwealth Scholarship Commission, UK for their support for carrying out the research work at University of Central Lancashire, UK.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Razdan, K., Sinha, V.R., Singh, K.K. (2020). New Paradigms in the Treatment of Skin Infections: Lipid Nanocarriers to the Rescue. In: Rahman, M., Beg, S., Kumar, V., Ahmad, F. (eds) Nanomedicine for Bioactives . Springer, Singapore. https://doi.org/10.1007/978-981-15-1664-1_11
Download citation
DOI: https://doi.org/10.1007/978-981-15-1664-1_11
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-15-1663-4
Online ISBN: 978-981-15-1664-1
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)