Abstract
One of the major issues related to medical devices and especially urinary stents are infections caused by different strains of bacteria and fungi, mainly in light of the recent rise in microbial resistance to existing antibiotics. Lately, it has been shown that nanomaterials could be superior alternatives to conventional antibiotics. Generally, nanoparticles are used for many applications in the biomedical field primarily due to the ability to adjust and control their physicochemical properties as well as their great reactivity due to the large surface-to-volume ratio. This has led to the formation of a new research field called nanomedicine which can be defined as the use of nanotechnology and nanomaterials in diagnostics, imaging, observing, prevention, control, and treatment of diseases. For example, coverings or coatings based on nanomaterials are now seen as a promising strategy for preventing or treating biofilms formation on healthcare kits, implants, and medical devices. Toxicity, inappropriate delivery, or degradation of conventionally used drugs for the treatment of infections may be avoided by using nanoparticles without or with encapsulated/immobilized active substances. Most of the materials which are used and examined for the preparation of the nanoparticles with encapsulated/immobilized active substances or smart reactive nanomaterials with antimicrobial effects are polymers, naturally derived antimicrobials, metal-based and non-metallic materials. This chapter provides an overview of the current state and future perspectives of the nanoparticle-based systems based on these materials for prevention, control, or elimination of biofilm-related infections on urinary stents. It also addresses manufacturing conditions indicating the huge potential for the improvement of existing and development of new promising stent solutions.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
- Nanoparticles
- Nanotechnology
- Antimicrobials
- Polymers
- Metal-based nanoparticles
- Non-metallic nanoparticles
1 Introduction
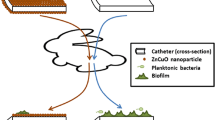
According to the literature, one of the most common complications related to indwelling urinary stents is microbial adhesion to their surface which leads to biofilm formation, and often thereafter to infection and, in some patients, urosepsis [1,2,3]. Bacteria in a biofilm can be up to 1000-fold more resistant to antimicrobial drugs [4]. The traditional methodology of using therapeutic intervention for developing an antimicrobial urinary stent very often lacks clinically meaningful benefit [5]. For that reason, urinary stent modifications using alternative methods and materials with antimicrobial functionality such as nanoparticle-based systems are being intensively investigated. Coverings or coatings, functionalization, blending and drug impregnation based on nanoparticles are mainly applied for these purposes [6]. In such a system i.e. product, nanoparticles may be used as the primary ingredient, constituent, or sub-constituent. Nanoparticles have demonstrated a broad-spectrum of antimicrobial properties against both Gram-positive and Gram-negative bacteria [7,8,9,10,11,12]. The growing interest toward antimicrobial potential of nanoparticles within the scientific community can be easily evaluated by searching the appropriate keywords through some of the recognized literature databases. According to one of them, SCOPUS, in the last 30 years more than 14,000 peer-reviewed documents have been published containing keywords such as “antimicrobial” and “nanoparticles” (Fig. 1). Interestingly, in the more specified search which refers only to the utilization of nanoparticles in urinary infections, it could be observed a similar profile i.e. growing tendency, except with a significantly lower number of published documents, (less than 2%). Even more interesting is the fact that when this search is expanded on the keywords such as antimicrobial + nanoparticles + urinary (ureteral) + stents, only two documents are listed. Although this type of searching has some limitations, it is obvious that, so far, the potential of the nanoparticles is not sufficiently investigated in this field.
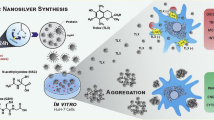
Until now, the antimicrobial mechanism of action of the nanoparticles is not fully explained but it is considered to be based either on induction of the oxidative stress [13], metal ion release [14], or non-oxidative mechanisms [15]. These mechanisms can occur also simultaneously (Fig. 2). In literature it has been anticipated that some nanoparticles neutralize the electric charge of the bacterial cell surface and consequently modify its penetrability, leading to bacterial death [16]. Also, nanoparticles may increase the production of reactive oxygen species resulting in constraints on the antioxidative defense system and thereafter mechanical damage to the bacterial cell membrane. So, nanoparticles can disrupt and penetrate the bacterial cell membrane, induce the creation of reactive oxygen species, stimulate intracellular antibacterial activity, and interact with DNA and proteins [16] (Fig. 2).
Nanoparticles exhibit antimicrobial activity through multiple mechanisms: cell wall disruption and alteration in membrane permeability, generation of ROS, nucleus/DNA damage, protein denaturation, inhibition of electron transport chain; and consequently the humpering of bacterial metabolic processes
All these led to their pronounced antibacterial properties. The effect of nanoparticles on biofilm formation depends on several parameters such as the type of the nanoparticles (metallic, nonmetallic, polymeric, etc.), their morphology (size and shape), electric charge, hydrophobicity, composition, polar interaction, etc. [17]. For example, Slomberg and coauthors examined the efficacy of silica nanoparticles containing nitric oxide against Gram-negative Pseudomonas aeruginosa and Gram-positive Staphylococcus aureus biofilms as a function of particle size and shape [18]. Smaller particles exhibited better nitric oxide delivery and enhanced bacteria killing compared to the larger ones. Also, the rod-like particles proved to be more effective than spherical particles in delivering nitric oxide and inducing greater antibacterial action throughout the biofilm. This chapter gives an extensive overview of the different types of nanoparticles and nanostructured materials for the prevention, control, or elimination of biofilm-related infections on urinary stents. It addresses polymeric nanoparticles, naturally derived antimicrobials, non-metallic and metal-based nanoparticles, production methods, characterizations as well as their applications.
2 Polymeric Nanoparticles
The most commonly used methods for achieving an antimicrobial effect of polymeric micro and nanoparticles are by controlled release of encapsulated/immobilized antimicrobial within the polymeric matrix [19,20,21,22,23] or by prevention of initial bacterial attachment by coating/covering of the surfaces by polymers [24,25,26,27]. It is considered a better option to inhibit the initial formation of biofilm, rather than trying to eliminate already colonized microorganisms. Surface coating and functionalization aim to have a bacteriostatic effect, while drug impregnation and blending can achieve a bactericidal effect [6]. Surface modification of catheters by polymers can be bioactive or biopassive. Biopassive coating is accomplished through the use of hydrophilic polymer materials, which prevent bacterial adhesion. The bioactive coating can refer to the coating of catheter surface with antimicrobial molecules or controlled release of antimicrobial from the particles on the surface [28, 29]. Water-soluble antimicrobials can be rapidly removed from catheters [5]. Drug-eluting stents showed uncontrolled drug release, potentiating the possibility of development of resistance, so recently researches focused on controlled release antibiotic, and antibiotic combination stent coatings.
Srisang et al. reported the synthesis of chlorhexidine loaded nanoparticles, in form of poly(-ethylene glycol)-block-poly(e-caprolactone) micelles, and poly(e-caprolactone) nanospheres, and coating of Foley catheter surface in multiple layers. In both cases, bacteria started to colonize the coated catheter only after 21 days, which indicates the prolonged release of chlorhexidine [30].
Non-adhesive hydrophilic implants are developed to prevent host irritation and bacterial adhesion [31]. Palmieri et al. designed a nanocomposite coating made of hydrophilic polymer polyethylene glycol and hydrophobic polyphenol curcumin deposited on the surface of graphene oxide nanoparticles. This coating decreased adherence and biofilm formation of Candida albicans on polyurethane catheters [32].
More research dealing with polymers such as poly(glycolic acid), poly(lactic-co-glycolic acid), polyamine, etc. are reported below since they are also involving non-metallic or metallic nanoparticles.
2.1 Naturally Derived Antimicrobials
Naturally derived antimicrobials such as essential oils, curcumin, enzymes, hyaluronic acid, and antimicrobial peptides in combination with synthetic antibiotics/nanoantibiotics [33, 34] are likely to exert sufficient inhibitory effect on uropathogens. These compounds are the basis of many modern pharmaceuticals, mainly antibiotics [35]. Due to low bioavailability, stability, and biocompatibility, they are often loaded into nanoparticles to improve their characteristics [36]. These nanosystems, comprised of phytochemicals or microbial metabolites, and especially in combination with nanoantibiotics [33], have the potential to be used as antimicrobial coating of urinary catheters [6].
Venkat Kumar et al. synthesized kanamycin–chitosan nanoparticles by ionic gelation, which were then covalently immobilized on polyurethane ureteral stents. These stents exhibited increased, synergistic antibacterial activity, which is suggested to be a result of the disruption of negatively charged bacterial membranes, due to the polycationic nature of these nanoparticles and therefore increased positive surface charge of stents [37].
Phenazine-1-carboxamide is an aromatic compound isolated from P. aeruginosa. It was used for functionalization of silica nanoparticles, which were then applied for coating of urethral stents, by Kanugala et al. They report promising antibacterial and antifungal activity on S. aureus and C. albicans, and also activity against mixed-species biofilms [38].
Kumar et al. reported functionalization of silver nanoparticles with Kocuran, an exopolysaccharide from Kocuria rosea [39]. These Kocuran-capped silver glyconanoparticles were used as a coating for silicone urethral catheters and showed significant antibacterial and antiadhesive properties against E. coli and S. aureus.
There have been attempts to inhibit biofilm growth by interfering with bacterial communication, quorum sensing. “Quorum quenching” molecules are compounds that interfere with quorum sensing by various mechanisms and can be utilized to create antibiofilm coatings. Nanocoatings made of α-amylase and acylase, capable of degrading bacterial exopolysaccharides and quorum sensing molecules, respectively, were deposited layer by layer on silicone urinary catheter surface. This coating exhibited inhibition of P. aeruginosa and S. aureus biofilms, consisting either of α-amylase or acylase, but especially in form of hybrid nanocoatings of both enzymes, which inhibited even mixed-species P. aeruginosa and E. coli biofilms [40]. NanoQuench was a European project for developing quorum quenching enzymes and nanoantibiotics for novel coatings, aiming to prevent biofilm formation on urinary catheters, with a focus on Gram-negative P. aeruginosa biofilms. One of the project’s results is antibiofilm multilayer nanovancomycin and acylase coating, which was shown to be efficient in-vitro [41].
Nanobiosystem composed of magnetite nanoparticles coated with Rosmarinus officinalis essential oil was efficient in reducing adherence to catheter surface, and biofilm formation by C. albicans and C. tropicalis [42].
Phytochemicals-capped gold nanoparticles were synthesized using Aegle marmelos leaf extract, for the further purpose of prevention of urinary catheter infections. Obtained nanotriangles exhibited major antimicrobial activity against S. aureus, P. aeruginosa, K. pneumoniae and E. faecalis [43].
3 Non-metallic Nanoparticles
A wide class of oxides, nitrides, silicide and carbide, hydroxyapatite, diamond-like carbon, and others are used as antimicrobials [16, 44, 45]. Surface coatings with these nanomaterials have gained significant attention due to their antimicrobial activity. Graphene-based nanomaterials have different surface chemistry (graphite, graphene oxide GO, and reduced graphene oxide RGO) and different microbial activity mechanisms. GO has a more potent antimicrobial effect against Escherichia coli when compared to graphite and RGO [46]. Amorphous carbon was also used as a matrix material for the incorporation of metallic clusters [47].
Laube and co-workers used diamond-like carbon (DLC) material for coating ureteral stents. They published an in vitro and in vivo study in which they observed that there was a reduction in encrustation, biofilm formation, and patients’ symptoms [48].
Nanostructured coatings of diamond-like carbon, molybdenum disulfide and tungsten disulfide nanoparticles were deposited on a polydimethylsiloxane substrate. These coatings were compared in terms of resistance to the formation of urinary deposits. It was found that tungsten disulfide was the most resistant to encrustations after 4 weeks of immersion in artificial urine [49].
To obtain functionalized catheter surface with improved resistance to microbial colonization and biofilm formation Fe2O3/C12 nanoparticles were coated on 2-((4-ethylphenoxy) methyl)-N-(substituted-phenylcarbamothioyl)-benzamide used as adsorption shell. This material showed improved resistance to Staphylococcus aureus and Pseudomonas aeruginosa, and did not show cytotoxicity [50].
Boron nitride (BN) has physicochemical properties similar to graphene-based nanomaterial, but it holds an advantage in terms of biocompatibility with human cells. Boron nitride composite with polyethylene was studied for biomedical applications. It was demonstrated that bacterial activity of BN/PE composite correlates with BN concentration [51].
Nitric oxide (NO) has been a well-known antimicrobial agent. Commonly used NO donor in the medical research S-Nitroso-N-acetyl-dl-penicillamine (SNAP) was impregnated in commercial urinary catheters [52].
It was shown that catheters have very high antimicrobial efficacy and effectively reduce biofilm formation over a longer period. However, the issue of NO storage remains, as the polymers are limited reservoirs for NO.
3.1 Metal-Based Nanoparticles
Metal-based nanoparticles are very popular antimicrobials [53]. They do not bind to a specific receptor in the bacterial cell which makes them have non-specific bacterial toxicity mechanisms and consequently makes the development of resistance by bacteria to be difficult. As a result, a large majority of metal-based nanoparticle efficacy studies performed so far have shown promising results in both Gram-positive and Gram-negative bacteria [54, 55]. Several review papers can be found regarding this subject, among few of them have been published most recently [17, 56,57,58].
In the field of urinary catheters, silver-based coatings are in use for over 20 years but their true efficacy is still a matter of debate [59, 60]. The narrow boundary between beneficial and toxic effects, especially in the prolonged applications remains a major concern in Ag utilization. One of the promising approaches to overcome the toxicity issue of Ag, is to functionalize it with more biocompatible compounds. As already mentioned above, Kumar et al., proposed the usage of exopolysaccharide Kocuran, as a capping and reducing agent of silver nanoparticles [39]. Related to the subject of Ag NPs functionalization, Ashmore and colleagues manage to coat Ag NPs with polyvinylpyrrolidone (PVP) and compared the antibacterial efficacy with the non-coated AgNPs [61]. As a result, a significant improvement in antibacterial efficacy was achieved. It is worth noting that two types of Ag-PVP NPs were prepared, either containing 10% of Ag or 99% and both of them have shown better antimicrobial properties against E. coli than non-coated AgNPs. In addition, the authors reported that Ag-PVP NPs also promote downregulation of the expression of genes that are involved in the cellular growth of E. coli.
Based on in vitro investigations of Giri and colleagues [62] reducing the surface charge of AuNPs broadens the therapeutic window, so a higher concentration of these particles can be used without toxicity concerns.
I. Carvalho et al. reported in their study, that deposition of Ag and Ag–Au bimetallic clusters on thermoplastic polyurethane tape (as one of the materials used in the ureteral stent manufacture) have positive outcomes [47]. The coating was performed by physical methods (sputtering and plasma gas condensation) and the authors characterized it as a promising for long periods, since the release of silver in artificial urine did not reach the maximum amount of coating even after 30 days. Nevertheless, these released Ag were sufficient for the prevention of biofilm formation and achievement of antibacterial effect against E. coli while preserving good biocompatibility. Comparing the antibacterial effects, amount of released Ag, and morphology of deposited Ag and Ag–Au clusters, the authors concluded that the size of the deposited cluster determines the mechanism and release kinetic of Ag. In the case of smaller homogeneously distributed clusters, the release of Ag ions is favored, while in the case of larger deposits the release of Ag NPs is the dominant process. In both scenarios, the bactericidal effect against E. coli was very similar. The other coatings investigated in this study achieved a slow Ag release and no antibacterial effect, suggesting that the release kinetics of Ag is directly responsible for the antibacterial properties of coatings.
Rocca et al. performed an interesting strategy in the coating of silicone catheters. The authors described a simple method for producing Au nanoplates by reduction of Au salt with gentamycin at elevated temperature [63]. The coating was performed in situ, during the synthesis procedure, and lasted only 15 min. Regardless of the duration of coating, deposited Au nanoplates were efficient in preventing the growth of three bacterial strains (S. aureus, P. aeruginosa and E. coli) after 18 h of incubation. The observed anti-biofouling effect of Au nanoplates was explained through the topographic change at the nano-scale level, which disrupts attachments of the bacterial cells. Additionally, the authors also confirmed the effectiveness of coating by testing it in stimulated flow conditions, using the physiological solution and syringe pump [63].
In the work performed by Ron et al., encrustation of silicone catheters was remarkably prevented in in vitro conditions, by coating with rhenium-doped molybdenum disulfide (Re:IF-MoS2) nanoparticles [64]. As the authors stated, these NPs displayed a unique tendency to self-assemble into mosaic-like arrangements, modifying the surface at the nanoscale to be encrustation-repellent. Encrustation investigation was conducted using a custom-built device and artificial urine. The effectiveness of Re:IF-MoS2 nanoparticles coating lies in their specific physicochemical properties such as negative charge, low surface free energy, and nanotexture, providing them a superior solid-lubrication behavior.
The second approach, besides stents coating, is the impregnation of nanoparticles in the drug-eluting stents. Recently, Gao et al. performed a thorough investigation of biodegradable stents with a renewable surface capable of contact killing of bacteria [65]. The renewable property was accomplished through surface degradation of poly(glycolic acid)/poly(lactic-co-glycolic acid) (PGA/PGLA) layer, while antibacterial properties were achieved by impregnation of hyperbranched poly(amide-amine)-capped Ag shell and Au core nanoparticles in PGA–PGLA. In vitro and in vivo testing have confirmed that this particular stent design provides good mechanical properties, high antibacterial activity, the low release of Ag ions, and good biocompatibility. According to the authors, the capping agent (poly(amide-amine) was most responsible for high bactericidal effects and low cytotoxicity of nanoparticles by providing a high-stabile structure. The stent degradation in artificial urine was gradual, constantly detaching adhered bacteria and proteins, and releasing enough amounts of nanoparticles. As a result, the authors reported good antibiofilm properties after 2 weeks-examination and lower levels of inflammatory and necrotic cells, 3 weeks after implantation.
A similar comprehensive approach in designing antibacterial and repellent coating was reported by Dayyoub et al. [66]. This group of scientists successfully developed a film of poly(lactic-co-glycolide) (PLGA) to release norfloxacin and Ag NPs, coated with tetraether lipid The strength of this multifunctional system lies in the fact that it consists of dual antimicrobial agents (norfloxacin is a broad-spectrum synthetic antibiotic almost exclusively indicated in the treatment of urinary tract infections) impregnated in the biodegradable matrix. The authors used this film to coat polyurethane and silicone sheets, which results in effective inhibition of bacteria adhesion, compared to uncoated sheets. Thanks to the fact that degradation of PLGA creates an acidic environment, it neutralizes alkali products of urea hydrolysis and thus reduces the encrustation, based on in vitro experiments in artificial urine that lasted two weeks.
Agarwala et al. investigated antibacterial/antibiofilm activity of iron oxide and copper oxide nanoparticles against multidrug-resistant biofilm forming uropathogens. They found that CuO nanoparticles are more effective as an antibacterial material than Fe2O3 nanoparticles [67].
Besides mentioned studies, a significant number of additional papers could be found regarding the antimicrobial activity of metal-based NPs and some of them are summarized in Table 1.
4 Conclusion
The effectiveness of nanoparticles against numerous bacterial strains including those that cause biofilm formations in urinary stents is well documented in many papers. However, the important issues that should be addressed in the nanoparticles utilization are the release from the inner surface of the stents and the stability of the coating. The harsh environment, to which the urinary stents are exposed, represents the obstacle that must be considered with great percussion when choosing the coating/impregnation technique and concentrations of nanoparticles. Literature data are constantly expanding with new findings regarding antibacterial activity, encrustation repellence, and biocompatibility, but lacking those regarding release profiles and how these profiles are influenced by the chemistry and flow conditions. Nevertheless, the reported studies have confirmed the nanoparticle-based strategy exhibit great potential and that it’s a matter of time when it will find its way to commercially available product.
References
Kehinde EO, Rotimi VO, Al-Hunayan A, Abdul-Halim H, Boland F, Al-Awadi KA. Bacteriology of urinary tract infection associated with indwelling J ureteral stents. J Endourol. 2004;18(9):891–6. https://doi.org/10.1089/end.2004.18.891.
Azevedo AS, Almeida C, Melo LF, Azevedo NF. Impact of polymicrobial biofilms in catheter-associated urinary tract infections. Crit Rev Microbiol. 2017;43(4):423–39. https://doi.org/10.1080/1040841X.2016.1240656.
Kumon H, Hashimoto H, Nishimura M, Monden K, Ono N. Catheter-associated urinary tract infections: impact of catheter materials on their management. Int J Antimicrob Agents. 2001;17(4):311–6.
Soto SM. Importance of biofilms in urinary tract infections: new therapeutic approaches. Adv Biol. 2014;2:1–13.
Samuel U, Guggenbichler JP. Prevention of catheter-related infections: the potential of a new nano-silver impregnated catheter. Int J Antimicrob Agents. 2004;23(SUPPL. 1):75–8.
Anjum S, Singh S, Benedicte L, Roger P, Panigrahi M, Gupta B. Biomodification strategies for the development of antimicrobial urinary catheters: overview and advances. Glob Chall. 2018;2(1):1700068.
Filipović N, Ušjak D, Milenković MT, Zheng K, Liverani L, Boccaccini AR, et al. Comparative study of the antimicrobial activity of selenium nanoparticles with different surface chemistry and structure. Front Bioeng Biotechnol. 2021;8:1591.
Stevanović M, Filipović N, Djurdjević J, Lukić M, Milenković M, Boccaccini A. 45S5Bioglass®-based scaffolds coated with selenium nanoparticles or with poly(lactide-co-glycolide)/selenium particles: processing, evaluation and antibacterial activity. Colloids Surf B Biointerfaces. 2015;132:208–15.
Stanković A, Sezen M, Milenković M, Kaišarević S, Andrić N, Stevanović M. PLGA/nano-ZnO composite particles for use in biomedical applications: preparation, characterization, and antimicrobial activity. J Nanomater. 2016;2016:1–10.
Stevanović M, Bračko I, Milenković M, Filipović N, Nunić J, Filipič M, et al. Multifunctional PLGA particles containing poly(l-glutamic acid)-capped silver nanoparticles and ascorbic acid with simultaneous antioxidative and prolonged antimicrobial activity. Acta Biomater. 2014;10(1):151–62.
Stevanović M, Jordović B, Uskoković D. Morphological changes of poly(dI-lactide-co-glycolide) nano-particles containing ascorbic acid during in vitro degradation process. J Microsc. 2008;232(3):511–6.
Stevanović M, Lukić MJ, Stanković A, Filipović N, Kuzmanović M, Janićijević Ž. Biomedical inorganic nanoparticles: preparation, properties, and perspectives. In: Materials for biomedical engineering. Amsterdam: Elsevier; 2019. p. 1–46. https://linkinghub.elsevier.com/retrieve/pii/B9780081028148000019
Gurunathan S, Woong Han J, Abdal Daye A, Eppakayala V, Kim J. Oxidative stress-mediated antibacterial activity of graphene oxide and reduced graphene oxide in Pseudomonas aeruginosa. Int J Nanomed. 2012;7:5901. http://www.dovepress.com/oxidative-stress-mediated-antibacterial-activity-of-graphene-oxide-and-peer-reviewed-article-IJN
Nagy A, Harrison A, Sabbani S, Munson RS Jr, Dutta PK, WJW. Silver nanoparticles embedded in zeolite membranes: release of silver ions and mechanism of antibacterial action. Int J Nanomed. 2011;6:1833. http://www.dovepress.com/silver-nanoparticles-embedded-in-zeolite-membranes-release-of-silver-i-peer-reviewed-article-IJN
Leung YH, Ng AMC, Xu X, Shen Z, Gethings LA, Wong MT, et al. Mechanisms of antibacterial activity of MgO: non-ROS mediated toxicity of MgO nanoparticles towards Escherichia coli. Small. 2014;10(6):1171–83. https://doi.org/10.1002/smll.201302434.
Wang L, Hu C, Shao L. The antimicrobial activity of nanoparticles: present situation and prospects for the future. Int J Nanomed. 2017;12:1227–49. https://www.dovepress.com/the-antimicrobial-activity-of-nanoparticles-present-situation-and-pros-peer-reviewed-article-IJN
Han C, Romero N, Fischer S, Dookran J, Berger A, Doiron AL. Recent developments in the use of nanoparticles for treatment of biofilms. Nanotechnol Rev. 2017;6(5):383–404. https://doi.org/10.1515/ntrev-2016-0054/html.
Slomberg DL, Lu Y, Broadnax AD, Hunter RA, Carpenter AW, Schoenfisch MH. Role of size and shape on biofilm eradication for nitric oxide-releasing silica nanoparticles. ACS Appl Mater Interfaces. 2013;5(19):9322–9. https://doi.org/10.1021/am402618w.
Filipović N, Stevanović M, Nunić J, Cundrič S, Filipič M, Uskoković D. Synthesis of poly(ε-caprolactone) nanospheres in the presence of the protective agent poly(glutamic acid) and their cytotoxicity, genotoxicity and ability to induce oxidative stress in HepG2 cells. Colloids Surf B Biointerfaces. 2014;117:414–24.
Filipović N, Veselinović L, RaŽić S, Jeremić S, Filipič M, Žegura B, et al. Poly (ε-caprolactone) microspheres for prolonged release of selenium nanoparticles. Mater Sci Eng C. 2019;96:776–89.
Filipović N, Stevanović M, Radulović A, Pavlović V, Uskoković D. Facile synthesis of poly(ε-caprolactone) micro and nanospheres using different types of polyelectrolytes as stabilizers under ambient and elevated temperature. Compos Part B Eng. 2013;45(1):1471–9.
Stevanović M. Biomedical applications of nanostructured polymeric materials. In Nanostructured polymer composites for biomedical applications. Amsterdam: Elsevier; 2019. p. 1–19. https://linkinghub.elsevier.com/retrieve/pii/B9780128167717000016
Stevanović MMM, Uskoković DP. Poly(lactide-co-glycolide)-based micro and nanoparticles for the controlled drug delivery of vitamins. Curr Nanosci. 2009;5(1):1–14. http://www.eurekaselect.com/openurl/content.php?genre=article&issn=1573-4137&volume=5&issue=1&spage=1
Cano A, Ettcheto M, Espina M, López-Machado A, Cajal Y, Rabanal F, et al. State-of-the-art polymeric nanoparticles as promising therapeutic tools against human bacterial infections. J Nanobiotechnol. 2020;18(1):156. https://doi.org/10.1186/s12951-020-00714-2.
Venkatesan N, Shroff S, Jayachandran K, Doble M. Polymers as ureteral stents. J Endourol. 2010;24(2):191–8. https://doi.org/10.1089/end.2009.0516.
Škrlová K, Malachová K, Muñoz-Bonilla A, Měřinská D, Rybková Z, Fernández-García M, et al. Biocompatible polymer materials with antimicrobial properties for preparation of stents. Nanomaterials. 2019;9(11):1548. https://www.mdpi.com/2079-4991/9/11/1548
Stevanović M. Polymeric micro- and nanoparticles for controlled and targeted drug delivery. In Nanostructures for drug delivery. Amsterdam: Elsevier; 2017. p. 355–78. https://linkinghub.elsevier.com/retrieve/pii/B9780323461436000117
Yassin MA, Elkhooly TA, Elsherbiny SM, Reicha FM, Shokeir AA. Facile coating of urinary catheter with bio-inspired antibacterial coating. Heliyon. 2019;5(12):e02986. https://linkinghub.elsevier.com/retrieve/pii/S2405844019366459
Badran MM, Alomrani AH, Harisa GI, Ashour AE, Kumar A, Yassin AE. Novel docetaxel chitosan-coated PLGA/PCL nanoparticles with magnified cytotoxicity and bioavailability. Biomed Pharmacother. 2018;106:1461–8.
Srisang S, Wongsuwan N, Boongird A, Ungsurungsie M, Wanasawas P, Nasongkla N. Multilayer nanocoating of Foley urinary catheter by chlorhexidine-loaded nanoparticles for prolonged release and anti-infection of urinary tract. Int J Polym Mater Polym Biomater. 2020;69(17):1081–9.
Scotland KB, Lo J, Grgic T, Lange D. Ureteral stent-associated infection and sepsis: pathogenesis and prevention: a review. Biofouling. 2019;35(1):117–27.
Palmieri V, Bugli F, Cacaci M, Perini G, De Maio F, Delogu G, et al. Graphene oxide coatings prevent Candida albicans biofilm formation with a controlled release of curcumin-loaded nanocomposites. Nanomedicine. 2018;13(22):2867–79.
Manjula R, Chavadi M. Nanoantibiotics: the next-generation antimicrobials. Cham: Springer; 2020. p. 375–88. https://doi.org/10.1007/978-3-030-41464-1_16.
Bračič M, Fras-Zemljič L, Pérez L, Kogej K, Stana-Kleinschek K, Kargl R, et al. Protein-repellent and antimicrobial nanoparticle coatings from hyaluronic acid and a lysine-derived biocompatible surfactant. J Mater Chem B. 2017;5(21):3888–97. http://xlink.rsc.org/?DOI=C7TB00311K
Dinic M, Pecikoza U, Djokic J, Stepanovic-Petrovic R, Milenkovic M, Stevanovic M, et al. Exopolysaccharide produced by probiotic strain Lactobacillus paraplantarum BGCG11 reduces inflammatory hyperalgesia in rats. Front Pharmacol. 2018;9:1.
Watkins R, Wu L, Zhang C, Davis RM, Xu B. Natural product-based nanomedicine: recent advances and issues. Int J Nanomed. 2015;10:6055–74.
Venkat Kumar G, Su CH, Velusamy P. Surface immobilization of kanamycin–chitosan nanoparticles on polyurethane ureteral stents to prevent bacterial adhesion. Biofouling. 2016;32(8):861–70.
Kanugala S, Jinka S, Puvvada N, Banerjee R, Kumar CG. Phenazine-1-carboxamide functionalized mesoporous silica nanoparticles as antimicrobial coatings on silicone urethral catheters. Sci Rep. 2019;9(1):1–16.
Kumar CG, Sujitha P. Green synthesis of Kocuran-functionalized silver glyconanoparticles for use as antibiofilm coatings on silicone urethral catheters. Nanotechnology. 2014;25(32):325101. https://doi.org/10.1088/0957-4484/25/32/325101.
Ivanova K, Fernandes MM, Francesko A, Mendoza E, Guezguez J, Burnet M, et al. Quorum-quenching and matrix-degrading enzymes in multilayer coatings synergistically prevent bacterial biofilm formation on urinary catheters. ACS Appl Mater Interfaces. 2015;7(49):27066–77.
NanoQuench Project. 2015. https://cordis.europa.eu/project/id/331416/reporting/it.
Chifiriuc C, Grumezescu V, Grumezescu A, Saviuc C, Lazăr V, Andronescu E. Hybrid magnetite nanoparticles/Rosmarinus officinalis essential oil nanobiosystem with antibiofilm activity. Nanoscale Res Lett. 2012;7(1):209. https://doi.org/10.1186/1556-276X-7-209.
Arunachalam K, Annamalai SK, Arunachalam AM, Raghavendra R, Kennedy S. One step green synthesis of phytochemicals mediated gold nanoparticles from Aegle marmales for the prevention of urinary catheter infection. Int J Pharm Pharm Sci. 2014;6(1):700–6.
Karwowska E. Antibacterial potential of nanocomposite-based materials—a short review. Nanotechnol Rev. 2017;6(2):243–54. https://doi.org/10.1515/ntrev-2016-0046/html.
Ušjak D, Dinić M, Novović K, Ivković B, Filipović N, Stevanović M, et al. Methoxy-substituted hydroxychalcone reduces biofilm production, adhesion and surface motility of Acinetobacter baumannii by inhibiting ompA gene expression. Chem Biodivers. 2021;18(1):e2000786. https://doi.org/10.1002/cbdv.202000786.
Zou X, Zhang L, Wang Z, Luo Y. Mechanisms of the antimicrobial activities of graphene materials. J Am Chem Soc. 2016;138(7):2064–77. https://doi.org/10.1021/jacs.5b11411.
Carvalho I, Dias N, Henriques M, Calderon VS, Ferreira P, Cavaleiro A, et al. Antibacterial effects of bimetallic clusters incorporated in amorphous carbon for stent application. ACS Appl Mater Interfaces. 2020;12(22):24555–63. https://doi.org/10.1021/acsami.0c02821.
Laube N, Kleinen L, Bradenahl J, Meissner A. Diamond-like carbon coatings on ureteral stents-a new strategy for decreasing the formation of crystalline bacterial biofilms? J Urol. 2007;177(5):1923–7.
Cardona A, Iacovacci V, Mazzocchi T, Menciassi A, Ricotti L. Novel nanostructured coating on PDMS substrates featuring high resistance to urine. ACS Appl Biol Mater. 2019;2(1):255–65. https://doi.org/10.1021/acsabm.8b00586.
Anghel I, Limban C, Grumezescu AM, Anghel AG, Bleotu C, Chifiriuc MC. In vitro evaluation of anti-pathogenic surface coating nanofluid, obtained by combining Fe3O4/C12 nanostructures and 2-((4-ethylphenoxy) methyl)-N-(substituted-phenylcarbamothioyl)-benzamides. Nanoscale Res Lett. 2012;7(1):1–10.
Pandit S, Gaska K, Mokkapati VR, Forsberg S, Svensson M, Kádár R, et al. Antibacterial effect of boron nitride flakes with controlled orientation in polymer composites. RSC Adv. 2019;9(57):33454–9.
Colletta A, Wu J, Wo Y, Kappler M, Chen H, Xi C, et al. S-Nitroso-N-acetylpenicillamine (SNAP) impregnated silicone foley catheters: a potential biomaterial/device to prevent catheter-associated urinary tract infections. ACS Biomater Sci Eng. 2015;1(6):416–24. https://doi.org/10.1021/acsbiomaterials.5b00032.
Stevanovic M. Assembly of polymers/metal nanoparticles and their applications as medical devices. Adv Biomater Biodevices. 2014;18:343–66.
Sánchez-López E, Gomes D, Esteruelas G, Bonilla L, Lopez-Machado AL, Galindo R, et al. Metal-based nanoparticles as antimicrobial agents: an overview. Nanomaterials. 2020;10(2):292. https://www.mdpi.com/2079-4991/10/2/292
Stevanović M, Uskoković V, Filipović M, Škapin SD, Uskoković D. Composite PLGA/AgNpPGA/AscH nanospheres with combined osteoinductive, antioxidative, and antimicrobial activities. ACS Appl Mater Interfaces. 2013;5(18):9034–42.
Qindeel M, Barani M, Rahdar A, Arshad R, Cucchiarini M. Nanomaterials for the diagnosis and treatment of urinary tract infections. Nanomaterials. 2021;11(2):546.
Aderibigbe B. Metal-based nanoparticles for the treatment of infectious diseases. Molecules. 2017;22(8):1370.
Singh A, Gautam PK, Verma A, Singh V, Shivapriya PM, Shivalkar S, et al. Green synthesis of metallic nanoparticles as effective alternatives to treat antibiotics resistant bacterial infections: a review. Biotechnol Rep. 2020;25:e00427.
Beattie M, Taylor J. Silver alloy vs. uncoated urinary catheters: a systematic review of the literature. J Clin Nurs. 2011;20(15–16):2098–108. https://doi.org/10.1111/j.1365-2702.2010.03561.x.
Liu XS, Zola JC, McGinnis DE, Squadrito JF, Zeltser IS. Do silver alloy-coated catheters increase risk of urethral strictures after robotic-assisted laparoscopic radical prostatectomy? Urology. 2011;78(2):365–7.
Ashmore D, Chaudhari A, Barlow B, Barlow B, Harper T, Vig K, et al. Evaluation of E. coli inhibition by plain and polymer-coated silver nanoparticles. Rev Inst Med Trop Sao Paulo. 2018;60:e18. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0036-46652018005000209&lng=en&tlng=en
Giri K, Rivas Yepes L, Duncan B, Kolumam Parameswaran P, Yan B, Jiang Y, et al. Targeting bacterial biofilms via surface engineering of gold nanoparticles. RSC Adv. 2015;5(128):105551–9. http://xlink.rsc.org/?DOI=C5RA16305F
Rocca DM, Aiassa V, Zoppi A, Silvero Compagnucci J, Becerra MC. Nanostructured gold coating for prevention of biofilm development in medical devices. J Endourol. 2020;34(3):345–51. https://doi.org/10.1089/end.2019.0686.
Ron R, Zbaida D, Kafka IZ, Rosentsveig R, Leibovitch I, Tenne R. Attenuation of encrustation by self-assembled inorganic fullerene-like nanoparticles. Nanoscale. 2014;6(10):5251. http://xlink.rsc.org/?DOI=c3nr06231g
Gao L, Wang Y, Li Y, Xu M, Sun G, Zou T, et al. Biomimetic biodegradable Ag@Au nanoparticle-embedded ureteral stent with a constantly renewable contact-killing antimicrobial surface and antibiofilm and extraction-free properties. Acta Biomater. 2020;114:117–32. https://linkinghub.elsevier.com/retrieve/pii/S1742706120304116
Dayyoub E, Frant M, Pinnapireddy SR, Liefeith K, Bakowsky U. Antibacterial and anti-encrustation biodegradable polymer coating for urinary catheter. Int J Pharm. 2017;531(1):205–14. https://linkinghub.elsevier.com/retrieve/pii/S0378517317307792
Agarwala M, Choudhury B, Yadav RNS. Comparative study of antibiofilm activity of copper oxide and iron oxide nanoparticles against multidrug resistant biofilm forming uropathogens. Indian J Microbiol. 2014;54(3):365–8.
Chutrakulwong F, Thamaphat K, Tantipaibulvut S, Limsuwan P. In situ deposition of green silver nanoparticles on urinary catheters under photo-irradiation for antibacterial properties. Processes. 2020;8(12):1630.
Prateeksha P, Bajpai R, Rao CV, Upreti DK, Barik SK, Singh BN. Chrysophanol-Functionalized silver nanoparticles for anti-adhesive and anti-biofouling coatings to prevent urinary catheter-associated infections. ACS Appl Nano Mater. 2021;4(2):1512–28.
LewisOscar F, Nithya C, Vismaya S, Arunkumar M, Pugazhendhi A, Nguyen-Tri P, et al. In vitro analysis of green fabricated silver nanoparticles (AgNPs) against Pseudomonas aeruginosa PA14 biofilm formation, their application on urinary catheter. Prog Org Coatings. 2021;151:106058.
Koc H, Kilicay E, Karahaliloglu Z, Hazer B, Denkbas EB. Prevention of urinary infection through the incorporation of silver–ricinoleic acid–polystyrene nanoparticles on the catheter surface. J Biomater Appl. 2021;36(3):385–405.
Mandakhalikar KD, Wang R, Rahmat JN, Chiong E, Neoh KG, Tambyah PA. Restriction of in vivo infection by antifouling coating on urinary catheter with controllable and sustained silver release: a proof of concept study. BMC Infect Dis. 2018;18(1):370.
Wang R, Neoh KG, Kang E, Tambyah PA, Chiong E. Antifouling coating with controllable and sustained silver release for long‐term inhibition of infection and encrustation in urinary catheters. J Biomed Mater Res Part B Appl Biomater. 2015;103(3):519–28.
Zhang S, Liang X, Gadd GM, Zhao Q. Superhydrophobic coatings for urinary catheters to delay bacterial biofilm formation and catheter-associated urinary tract infection. ACS Appl Bio Mater. 2020;3(1):282–91.
Evliyaoğlu Y, Kobaner M, Çelebi H, Yelsel K, Doğan A. The efficacy of a novel antibacterial hydroxyapatite nanoparticle-coated indwelling urinary catheter in preventing biofilm formation and catheter-associated urinary tract infection in rabbits. Urol Res. 2011;39(6):443–9.
Huang W-C, Tsai P-J, Chen Y-C. Multifunctional Fe3O4@Au Nanoeggs as photothermal agents for selective killing of nosocomial and antibiotic-resistant bacteria. Small. 2009;5(1):51–6.
Hosseini SS, Ghaemi E, Noroozi A, Niknejad F. Zinc oxide nanoparticles inhibition of initial adhesion and als1 and als3 gene expression in candida albicans strains from urinary tract infections. Mycopathologia. 2019;184(2):261–71.
Hosseini SS, Ghaemi E, Koohsar F. Influence of ZnO nanoparticles on Candida albicans isolates biofilm formed on the urinary catheter. Iran J Microbiol. 2018;10(6):424–32.
Shalom Y, Perelshtein I, Perkas N, Gedanken A, Banin E. Catheters coated with Zn-doped CuO nanoparticles delay the onset of catheter-associated urinary tract infections. Nano Res. 2017;10(2):520–33.
Dybowska-Sarapuk Ł, Kotela A, Krzemiński J, Wróblewska M, Marchel H, Romaniec M, et al. Graphene nanolayers as a new method for bacterial biofilm prevention: preliminary results. J AOAC Int. 2017;100(4):900–4.
Vladkova T, Angelov O, Stoyanova D, Gospodinova D, Gomes L, Soares A, et al. Magnetron co-sputtered TiO2/SiO2/Ag nanocomposite thin coatings inhibiting bacterial adhesion and biofilm formation. Surf Coatings Technol. 2020;384:125322.
Lellouche J, Kahana E, Elias S, Gedanken A, Banin E. Antibiofilm activity of nanosized magnesium fluoride. Biomaterials. 2009;30(30):5969–78.
Acknowledgments
Funds for the realization of this work were provided by the Ministry of Education, Science and Technological Development of the Republic of Serbia, Agreement on realization and financing of scientific research work of the Institute of Technical Sciences of SASA in 2021 (Record number: 451-03-9/2021-14/200175). We are also thankful to COST Action CA16217.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2022 The Author(s)
About this chapter
Cite this chapter
Filipović, N., Tomić, N., Kuzmanović, M., Stevanović, M.M. (2022). Nanoparticles. Potential for Use to Prevent Infections. In: Soria, F., Rako, D., de Graaf, P. (eds) Urinary Stents. Springer, Cham. https://doi.org/10.1007/978-3-031-04484-7_26
Download citation
DOI: https://doi.org/10.1007/978-3-031-04484-7_26
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-04483-0
Online ISBN: 978-3-031-04484-7
eBook Packages: MedicineMedicine (R0)