Abstract
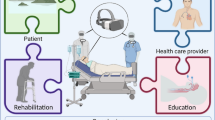
The ongoing Covid-19 pandemic has generated a strong impetus to digitalize the economy and aspects of our daily life. Clinical medicine traditionally being conservative has seen a limited uptake of these new technologies which has seen widespread adoption in other industries. But due to disruptive nature of the pandemic, clinical medicine has also been forced to adapt and capitalize on these new technologies. Chief amongst them is the utilization of extended reality (XR) technologies, which is an umbrella term that encompasses a spectrum of virtual reality (VR) and Augmented reality (AR) devices that blend the physical world with the digital world. VR technologies immerses users in 3D worlds while AR technologies project 3D objects into the user’s physical environment while permitting full visibility of the user’s surroundings. XR technologies can assist in infection control measures by revolutionizing clinical ward rounds. Patient’s key blood results and vitals can be projected above each patient enhancing the speed of clinical ward rounds for large number of patient’s in community isolation facilities. Examination findings can then be dictated and automatically recorded. XR technologies can also assist clinicians during the planning and execution of highly infective/risky procedures. XR can help proceduralists simulate the procedure, limiting timing spent during the actual procedure. While XR guided robots can actually perform the high risk and delicate procedures, limiting infection risk for the proceduralist. XR technologies can overcome the disruption caused clinical education due to Covid-19 pandemic infection control measures. They can help simulate patient interaction/ clinical scenarios for medical students while keeping both patient and medical students safe from infection. Covid-19 has also generated much psychosocial distress due to the isolation stemming from infection control. XR technologies can be used to help bridge the psychosocial isolation by connecting patients with their family members, hobbies or home towns. This can be especially therapeutic when counselling patients that suffer pandemic related depression/anxiety. Particularly in palliative patients XR technologies can help simulate experiences that would be physically impossible for them.
Samuel Wang Sherng Young was principally involved in formulating the topic, performing the literature review and writing the chapter.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Azuma, R., Baillot, Y., Behringer, R., Feiner, S., Julier, S., MacIntyre, B.: Recent advances in augmented reality. IEEE Comput. Graphics Appl. 21(6), 34–47 (2001)
Cipresso, P., Giglioli, I.A.C., Raya, M.A., Riva, G.: The past, present, and future of virtual and augmented reality research: a network and cluster analysis of the literature. Front Psychol. 9, 2086
Peterson, D.C., Mlynarczyk, G.S.: Analysis of traditional versus three-dimensional augmented curriculum on anatomical learning outcome measures. Anat. Sci. Educ. 9(6), 529–536 (2016)
Chan, F., Aguirre, S., Bauser-Heaton, H., Hanley, F., Perry, S. (eds.): Head tracked stereoscopic pre-surgical evaluation of major aortopulmonary collateral arteries in the newborns. In: Radiological Society of North America 2013 Scientific Assembly and Annual Meeting (2013)
Qian, M., Jiang, J.: COVID-19 and social distancing. J. Publ. Health 1–3 (2020)
Lewnard, J.A., Lo, N.C.: Scientific and ethical basis for social-distancing interventions against COVID-19. Lancet. Infect. Dis 20(6), 631–633 (2020)
Shaker, M.S., Oppenheimer, J., Grayson, M., Stukus, D., Hartog, N., Hsieh, E.W.Y., et al.: COVID-19: pandemic contingency planning for the allergy and immunology clinic. J Allergy Clin Immunol: Pract. 8(5), 1477–88.e5 (2020)
Schwartz, A.M., Wilson, J.M., Boden, S.D., Moore, T.J, Jr., Bradbury, T.L., Jr., Fletcher, N.D.: Managing resident workforce and education during the COVID-19 pandemic: evolving strategies and lessons learned. JBJS Open Access 5(2) (2020)
Dornan, T.: Osler, Flexner, apprenticeship and ‘the new medical education.’ J. R. Soc. Med. 98(3), 91–95 (2005)
Lee, A.K.F., Cho, R.H.W., Lau, E.H.L., Cheng, H.K., Wong, E.W.Y., Ku, P.K.M., et al.: Mitigation of head and neck cancer service disruption during COVID-19 in Hong Kong through telehealth and multi-institutional collaboration. Head Neck 42(7), 1454–1459 (2020)
Jain, U.: Risk of COVID-19 due to shortage of personal protective equipment. Cureus 12(6), e8837–e (2020)
Howard, B.E.: High-Risk Aerosol-generating procedures in COVID-19: respiratory protective equipment considerations. Otolaryngol. Head Neck Surg. 163(1), 98–103 (2020)
Qian, M., Nicholson, J., Tanaka, D., Dias, P., Wang, E., Qiu, L. (eds.): Augmented reality (AR) assisted laryngoscopy for endotracheal intubation training. In: Virtual, Augmented and Mixed Reality Applications and Case Studies. Springer International Publishing, Cham (2019)
Kaur, R., Weiss, T.T., Perez, A., Fink, J.B., Chen, R., Luo, F., et al.: Practical strategies to reduce nosocomial transmission to healthcare professionals providing respiratory care to patients with COVID-19. Crit. Care 24(1), 571 (2020)
Hemmerling, T.M., Taddei, R., Wehbe, M., Zaouter, C., Cyr, S., Morse, J.: First robotic tracheal intubations in humans using the Kepler intubation system. BJA: Br. J. Anaesth. 108(6), 1011–1016 (2012)
Wang, X., Tao, Y., Tao, X., Chen, J., Jin, Y., Shan, Z., et al.: An original design of remote robot-assisted intubation system. Sci. Rep. 8(1), 13403 (2018)
Zemmar, A., Lozano, A.M., Nelson, B.J.: The rise of robots in surgical environments during COVID-19. Nat. Mach. Intell. 2(10), 566–572 (2020)
Bai, H.X., Wang, R., Xiong, Z., Hsieh, B., Chang, K., Halsey, K., et al.: Artificial intelligence augmentation of radiologist performance in distinguishing COVID-19 from Pneumonia of other origin at chest CT. Radiology 296(3), E156–E165 (2020)
Harmon, S.A., Sanford, T.H., Xu, S., Turkbey, E.B., Roth, H., Xu, Z., et al.: Artificial intelligence for the detection of COVID-19 pneumonia on chest CT using multinational datasets. Nat Commun. 11(1), 4080 (2020)
Mei, X., Lee, H.C., Diao, K.Y., Huang, M., Lin, B., Liu, C., et al.: Artificial intelligence-enabled rapid diagnosis of patients with COVID-19. Nat Med. 26(8), 1224–1228 (2020)
Li, M., Lei, P., Zeng, B., Li, Z., Yu, P., Fan, B., et al.: Coronavirus disease (COVID-19): spectrum of CT findings and temporal progression of the disease. Acad. Radiol. 27(5), 603–608 (2020)
Suri, J.S., Puvvula, A., Biswas, M., Majhail, M., Saba, L., Faa, G., et al.: COVID-19 pathways for brain and heart injury in comorbidity patients: a role of medical imaging and artificial intelligence-based COVID severity classification: a review. Comput. Biol. Med. 124, 103960 (2020)
Mohammadzadeh, N., Gholamzadeh, M., Saeedi, S., Rezayi, S.: The application of wearable smart sensors for monitoring the vital signs of patients in epidemics: a systematic literature review. J. Ambient. Intell. Hum. Comput. 1–15 (2020)
Dias, D., Paulo Silva Cunha, J.: Wearable health devices-vital sign monitoring, systems and technologies. Sensors (Basel) 18(8), 2414 (2018)
Tong, Ng W.: COVID-19: protection of workers at the workplace in Singapore. Saf. Health Work (2020). https://doi.org/10.1016/j.shaw.2020.09.013
Pulia, M.S., O’Brien, T.P., Hou, P.C., Schuman, A., Sambursky, R.: Multi-tiered screening and diagnosis strategy for COVID-19: a model for sustainable testing capacity in response to pandemic. Ann. Med. 52(5), 207–214 (2020)
Kamphuis, C., Barsom, E., Schijven, M., Christoph, N.: Augmented reality in medical education? Perspect. Med. Educ. 3(4), 300–311 (2014)
Iwanaga, J., Loukas, M., Dumont, A.S., Tubbs, R.S.: A review of anatomy education during and after the COVID-19 pandemic: revisiting traditional and modern methods to achieve future innovation. Clin. Anat. 34(1), 108–114 (2021)
Wahadat, A.R., Sadeghi, A.H., Tanis, W.: Heart team meetings during COVID-19: different formats of multidisciplinary heart team meetings under the gathering restriction rules due to the coronavirus disease-2019 pandemic are discussed. Eur. Heart J. 41(20), 1872–1874 (2020)
Rogawski McQuade, E.T., Guertin, K.A., Becker, L., Operario, D., Gratz, J., Guan, D., et al.: Assessment of seroprevalence of SARS-CoV-2 and risk factors associated with COVID-19 infection among outpatients in Virginia. JAMA Netw. Open. 4(2), e2035234–e (2021)
Ford, D., Harvey, J.B., McElligott, J., King, K., Simpson, K.N., Valenta, S., et al.: Leveraging health system telehealth and informatics infrastructure to create a continuum of services for COVID-19 screening, testing, and treatment. J. Am. Med. Inform. Assoc. 27(12), 1871–1877 (2020)
Kaushik, A., Patel, S., Dubey, K.: Digital cardiovascular care in COVID-19 pandemic: a potential alternative? J. Card. Surg. 35(12), 3545–3550 (2020)
Wosik, J., Fudim, M., Cameron, B., Gellad, Z.F., Cho, A., Phinney, D., et al.: Telehealth transformation: COVID-19 and the rise of virtual care. J. Am. Med. Inform. Assoc. 27(6), 957–962 (2020)
Zaidi, S.T.R., Hasan, S.S.: Personal protective practices and pharmacy services delivery by community pharmacists during COVID-19 pandemic: results from a national survey. Res. Social Adm. Pharm. 17(1), 1832–1837 (2021)
Koonin, L.M., Hoots, B., Tsang, C.A., Leroy, Z., Farris, K., Jolly, T., et al.: Trends in the use of telehealth during the emergence of the COVID-19 pandemic—United States. MMWR Morb Mortal Wkly Rep. 69(43), 1595–1599 (2020)
Aaron Baum, P.J.K., Mark, D.: Schwartz. Reduced in-person and increased telehealth outpatient visits during the COVID-19 pandemic. Annal. Internal Med. 174(1), 129–319 (2021)
Worster, B., Swartz, K.: Telemedicine and palliative care: an increasing role in supportive oncology. Curr. Oncol. Rep. 19(6), 37 (2017)
Carbone, M., Freschi, C., Mascioli, S., Ferrari, V., Ferrari, M. (eds.): A wearable augmented reality platform for telemedicine. In: Augmented Reality, Virtual Reality, and Computer Graphics. Springer International Publishing, Cham (2016)
Wang, S.S., Teo, W.Z., Chai, Y.W.: Virtual reality as a bridge in palliative care during COVID-19. J. Palliat. Med. (2020)
Ritchey, K.C., Foy, A., McArdel, E., Gruenewald, D.A.: Reinventing palliative care delivery in the Era of COVID-19: how telemedicine can support end of life care. Am. J. Hosp. Palliat. Med. 37(11), 992–7 (2020)
Edwards, M.A., Patel, A.C.: Telemedicine in the state of Maine: a model for growth driven by rural needs. Telemed. J. E Health 9(1), 25–39 (2003)
Newman, L., Bidargaddi, N., Schrader, G.: Service providers’ experiences of using a telehealth network 12 months after digitisation of a large Australian rural mental health service. Int. J. Med. Informatics 94, 8–20 (2016)
Pfefferbaum, B., North, C.S.: Mental health and the Covid-19 pandemic. N Engl J Med. (2020)
Gros, D.F., Morland, L.A., Greene, C.J., Acierno, R., Strachan, M., Egede, L.E., et al.: Delivery of evidence-based psychotherapy via video telehealth. J. Psychopathol. Behav. Assess. 35(4), 506–521 (2013)
Chen, L., Day, T.W., Tang, W., John, N.W. (eds.): Recent developments and future challenges in medical mixed reality. In: 2017 IEEE International Symposium on Mixed and Augmented Reality (ISMAR) (2017)
Kabalci, Y.: 5G mobile communication systems: fundamentals, challenges, and key technologies. In: Kabalci, E., Kabalci, Y. (eds.) Smart Grids and Their Communication Systems, pp. 329–359. Springer Singapore, Singapore (2019)
Hilty, D.M., Randhawa, K., Maheu, M.M., McKean, A.J.S., Pantera, R., Mishkind, M.C., et al.: A review of telepresence, virtual reality, and augmented reality applied to clinical care. J. Technol. Behav. Scie. 5(2), 178–205 (2020)
Terry, J., Davies, A., Williams, C., Tait, S., Condon, L.: Improving the digital literacy competence of nursing and midwifery students: a qualitative study of the experiences of NICE student champions. Nurse Educ. Pract. 34, 192–198 (2019)
Machleid, F., Kaczmarczyk, R., Johann, D., Balčiūnas, J., Atienza-Carbonell, B., von Maltzahn, F. et al.: Perceptions of digital health education among european medical students: mixed methods survey. J. Med. Internet Res. 22(8), e19827–e (2020)
Mesko, B., Győrffy, Z., Kollár, J.: Digital literacy in the medical curriculum: a course with social media tools and gamification. JMIR Med Educ. 1(2), e6 (2015)
Al-Qirim, N.: Championing telemedicine adoption and utilization in healthcare organizations in New Zealand. Int. J. Med. Inform. 76(1), 42–54 (2007)
Day, K., Gu, Y. (eds.): Influencing factors for adopting personal health record (PHR). HIC (2012)
McAlearney, A.S., Schweikhart, S.B., Medow, M.A.: Doctors’ experience with handheld computers in clinical practice: qualitative study. BMJ 328(7449), 1162 (2004)
Jamil, F., Farooqi, S., Waseem, T.: Why the art of clinician is dying? Opinions & judgements: a systematic
Sorenson, C., Drummond, M., Bhuiyan, K.B.: Medical technology as a key driver of rising health expenditure: disentangling the relationship. Clinicoecon Outcomes Res. 5, 223–234 (2013)
Hermer, L.D., Brody, H.: Defensive medicine, cost containment, and reform. J. Gen. Intern. Med. 25(5), 470–473 (2010)
Vollbrecht, H., Arora, V., Otero, S., Carey, K., Meltzer, D., Press, V.G.: Evaluating the need to address digital literacy among hospitalized patients: cross-sectional observational study. J. Med. Internet Res. 22(6), e17519 (2020)
van der Vaart, R., Drossaert, C.H.C., de Heus, M., Taal, E., van de Laar, M.A.F.J.: Measuring actual ehealth literacy among patients with rheumatic diseases: a qualitative analysis of problems encountered using health 1.0 and health 2.0 applications. J. Med. Internet Res. 15(2), e27 (2013)
Neter, E., Brainin, E.: eHealth literacy: extending the digital divide to the realm of health information. J. Med. Internet Res. 14(1), e19 (2012)
Strusani, D., Houngbonon, G.V.: What COVID-19 means for digital infrastructure in emerging markets (2020)
McGinnis, J.M., Powers, B., Grossmann, C.: Digital infrastructure for the learning health system: the foundation for continuous improvement in health and health care: workshop series summary (2011)
National Academies of Sciences E, Medicine. The promises and perils of digital strategies in achieving health equity: workshop summary (2016)
Wood, B.R., Young, J.D., Abdel-Massih, R.C., McCurdy, L., Vento, T.J., Dhanireddy, S., et al.: Advancing digital health equity: a policy paper of the infectious diseases society of america and the HIV medicine association. Clin. Infect. Dis. 72(6), 913–919 (2020)
McKee, M., van Schalkwyk, M.C., Stuckler, D.: The second information revolution: digitalization brings opportunities and concerns for public health. Eur. J. Publ. Health 29(Supplement_3), 3–6 (2019)
Thuemmler, C., Paulin, A., Jell, T., Lim, A.K.: Information technology—next generation: the impact of 5G on the evolution of health and care services. In: Information Technology-New Generations, pp. 811–817. Springer (2018)
West, D.M.: How 5G technology enables the health internet of things. Brookings Center for Technology Innovation 3, 1–20 (2016)
Wu, T., Wu, F., Qiu, C., Redouté, J.M., Yuce, M.R.: A rigid-flex wearable health monitoring sensor patch for IoT-connected healthcare applications. IEEE Internet Things J. 7(8), 6932–6945 (2020)
Manas, M., Sinha, A., Sharma, S., Mahboob, M.R.: A novel approach for IoT based wearable health monitoring and messaging system. J. Ambient. Intell. Humaniz. Comput. 10(7), 2817–2828 (2019)
Fan, Y., Xu, P., Jin, H., Ma, J., Qin, L.: Vital sign measurement in telemedicine rehabilitation based on intelligent wearable medical devices. IEEE Access 7, 54819–54823 (2019)
Albahri, A.S., Alwan, J.K., Taha, Z.K., Ismail, S.F., Hamid, R.A., Zaidan, A.A., et al.: IoT-based telemedicine for disease prevention and health promotion: state-of-the-art. J. Netw. Comput. Appl. 173, 102873 (2021)
Thomson, E.A., Nuss, K., Comstock, A., Reinwald, S., Blake, S., Pimentel, R.E., et al.: Heart rate measures from the apple watch, fitbit charge HR 2, and electrocardiogram across different exercise intensities. J. Sports Sci. 37(12), 1411–1419 (2019)
Benedetto, S., Caldato, C., Bazzan, E., Greenwood, D.C., Pensabene, V., Actis, P.: Assessment of the fitbit charge 2 for monitoring heart rate. PloS one 13(2), e0192691 (2018)
Chen, M., Hao, Y., Hwang, K., Wang, L., Wang, L.: Disease prediction by machine learning over big data from healthcare communities. IEEE Access 5, 8869–8879 (2017)
Beam, A.L., Kohane, I.S.: Big data and machine learning in health care. JAMA 319(13), 1317–1318 (2018)
Bates, D.W., Heitmueller, A., Kakad, M., Saria, S.: Why policymakers should care about “big data” in healthcare. Health Policy Technol. 7(2), 211–216 (2018)
Rodriguez-Villa, E., Torous, J.: Regulating digital health technologies with transparency: the case for dynamic and multi-stakeholder evaluation. BMC Med. 17(1), 1–5 (2019)
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Wang, S.S.Y. (2022). Use of Extended Reality in Medicine During the Covid-19 Pandemic. In: Pillai, A.S., Guazzaroni, G. (eds) Extended Reality Usage During COVID 19 Pandemic. Intelligent Systems Reference Library, vol 216. Springer, Cham. https://doi.org/10.1007/978-3-030-91394-6_1
Download citation
DOI: https://doi.org/10.1007/978-3-030-91394-6_1
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-91393-9
Online ISBN: 978-3-030-91394-6
eBook Packages: Intelligent Technologies and RoboticsIntelligent Technologies and Robotics (R0)