Abstract
Background: Treatment with analgesics before surgery may be effective in reducing post-operative pain. This approach is defined as “pre-emptive analgesia” and recent reviews show conflicting results.
Objectives: The aim of this study was to investigate the efficacy of pre-emptive analgesia with sublingual morphine sulphate, compared with sublingual midazolam in patients undergoing elective abdominal surgery.
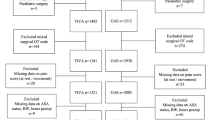
Methods: Prior to surgery, 29 patients were randomized and premedicated with sublingual morphine sulphate 0.5 mg/kg (Group A; n = 15) or with sublingual midazolam 0.03 mg/kg (Group B; n = 14). General anaesthesia was maintained with sevoflurane and fentanyl. Post-operatively, intravenous (IV) acetaminophen 0.02 mg/kg was given to all patients and a bolus of IV morphine 0.1 mg/kg was given to Group B patients. Post-operative pain was controlled by IV morphine via a patient-controlled analgesia (PCA) device. IV acetaminophen 0.02 mg/kg was also administered four times daily. Efficacy was assessed using static Visual Analogue Scale (sVAS) scores, dynamic VAS (dVAS) scores, number of PCA doses administered and number of failed doses registered from the PCA device at 4, 6, 24 and 48 hours after surgery. Results were statistically analysed using the Student t-test; a value of p < 0.05 was considered significant.
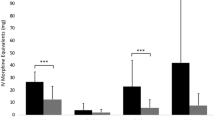
Results: Significantly lower sVAS and dVAS scores were observed in Group A patients than in Group B at all assessment periods (p < 0.05 for all time points). There were less PCA administered and failed doses in Group A, compared with Group B (all time points p < 0.05). There was no difference in the occurrence of common side effects between the two treatments.
Conclusions: In patients undergoing elective abdominal surgery, premedication with sublingual morphine sulphate results in a better control of post-operative pain, compared to premedication with sublingual midazolam. The beneficial effect of pre-operative sublingual morphine sulphate was apparent in the immediate post-operative period and was sustained over the 48-hour assessment period.



Similar content being viewed by others
References
Wall PD. The prevention of postoperative pain. Pain 1988 Jun; 33(3): 289–90
Dahl JB, Moiniche S. Pre-emptive analgesia. Br Med Bull 2004; 71: 13–27
Woolf CJ, Chong MS. Preemptive analgesia—treating postoperative pain by preventing the establishment of central sensitization. Anesth Analg 1993 Aug; 77(2): 362–79
Ong CK, Lirk P, Seymour RA, et al. The efficacy of preemptive analgesia for acute postoperative pain management: a meta-analysis. Anesth Analg 2005 Mar; 100(3): 757–73, table of contents
Zhang H, Zhang J, Streisand JB. Oral mucosal drug delivery: clinical pharmacokinetics and therapeutic applications. Clin Pharmacokinet 2002; 41(9): 661–80
Crile GW. The kinetic theory of shock and its prevention through anoci-association. Lancet 1913; 185: 7–16
Moiniche S, Kehlet H, Dahl JB. A qualitative and quantitative systematic review of preemptive analgesia for postoperative pain relief: the role of timing of analgesia. Anesthesiology 2002 Mar; 96(3): 725–41
Grape S, Tramer MR. Do we need preemptive analgesia for the treatment of postoperative pain? Best Pract Res Clin Anaes-thesiol 2007 Mar; 21(1): 51–63
Acknowledgements
The funds were provided from the Department of Critical Care Medicine and Surgery, University of Florence and Azienda Ospedaliero-Universitaria Careggi Florence, Italy and no external funds were provided in design and conduct of study, the collection, the management, analysis or interpretation of data and preparation, review and approval of the manuscript. There were no relevant conflicts of interest for all authors, or for all persons who made substantial contribution to the work, but do not meet criteria for authorship
English language and editorial assistance for the preparation of this manuscript was provided by Stephanie Blick, Wolters Kluwer Health Medical Communications. This assistance was funded by Molteni Farmaceutici, Inc.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Campiglia, L., Cappellini, I., Consales, G. et al. Premedication with Sublingual Morphine Sulphate in Abdominal Surgery. Clin. Drug Investig. 29 (Suppl 1), 25–30 (2009). https://doi.org/10.2165/0044011-200929001-00004
Published:
Issue Date:
DOI: https://doi.org/10.2165/0044011-200929001-00004