Abstract
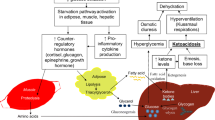
Diabetic ketoacidosis (DKA) is a life-threatening complication of diabetes mellitus. While it can occur in all types of diabetes mellitus, it is seen most often in patients with type 1 diabetes, either at presentation or as a result of non-compliance with medical therapy. DKA is characterized by hyperglycemia, acidosis, dehydration, and electrolyte abnormalities, which result from a deficiency of insulin and an excess of counter-regulatory hormones.
Therapy is aimed at repleting fluids, and correcting acidosis and electrolyte disturbances by administration of intravenous fluid and intravenous insulin. Rapid correction should be avoided as it may result in untoward effects, including cerebral edema. Frequent monitoring of neurologic status and metabolic parameters aids in avoidance or early detection of complications. While much is still not understood about the most serious complication, cerebral edema, recent studies suggest that its development may be tied to a loss of cerebral autoregulation and a vasogenic mechanism of edema formation. Treatment of cerebral edema includes fluid restriction and administration of mannitol. Once DKA has resolved, subcutaneous insulin is initiated with careful consideration of its pharmacokinetics to avoid a period of insulin deficiency and metabolic decompensation.

Similar content being viewed by others
Notes
Corrected serum sodium = measured sodium + (1.6 × glucose [mg/dL] − 100)/100.
References
Barnes AJ, Bloom SR, Goerge K, et al. Ketoacidosis in pancreatectomized man. N Engl J Med 1977; 296(22): 1250–3
Lanng S, Hansen A, Thorsteinsson B, et al. Glucose tolerance in patients with cystic fibrosis: five year prospective study. BMJ 1995; 311: 655–9
Nabarro JDN, Spencer AG, Stowers JM. Metabolic studies in severe diabetic ketosis. Q J Med 1952; 82: 225–48
American Diabetes Association. Type 2 diabetes in children and adolescents. Diabetes Care 2000; 23(3): 381–9
Laffel LM, Wentzell K, Loughlin C, et al. Sick day management using blood 3-hydroxybutyrate (3-OHB) compared with urine ketone monitoring reduces hospital visits in young people with T1DM: a randomized clinical trial. Diabet Med 2006; 23(3): 278–84
Rosenbloom AL. Intracerebral crises during treatment of diabetic ketoacidosis. Diabetes Care 1990; 13(1): 22–33
Muir AB, Quisling RG, Yang MC, et al. Cerebral edema in childhood diabetic ketoacidosis: natural history, radiographic findings, and early identification. Diabetes Care 2004; 27(7): 1541–6
Glaser N, Barnett P, McCaslin I, et al., on behalf of the Pediatric Emergency Medicine Collaborative Research Committee of the American Academy of Pediatrics. Risk factors for cerebral edema in children with diabetic ketoacidosis: The Pediatric Emergency Medicine Collaborative Research Committee of the American Academy of Pediatrics. N Engl J Med 2001; 344(4): 264–9
Glaser NS, Wootton-Gorges SL, Marcin JP, et al. Mechanism of cerebral edema in children with diabetic ketoacidosis. J Pediatr 2004; 145(2): 164–71
Roberts JS, Vavilala MS, Schenkman KA, et al. Cerebral hyperemia and impaired cerebral autoregulation associated with diabetic ketoacidosis in critically ill children. Crit Care Med 2006; 34(8): 2217–23
Figueroa RE, Hoffman WH, Momin Z, et al. Study of subclinical cerebral edema in diabetic ketoacidosis by magnetic resonance imaging T2 relaxometry and apparent diffusion coefficient maps. Endocr Res 2005; 31(4): 345–55
Clark JA, Burny I, Sarnaik AP, et al. Acute thiamine deficiency in diabetic ketoacidosis: diagnosis and management. Pediatr Crit Care Med 2006; 7(6): 595–9
Haddad NG, Croffie JM, Eugster EA. Pancreatic enzyme elevations in children with diabetic ketoacidosis. J Pediatr 2004; 145(1): 122–4
Carl GF, Hoffman WH, Passmore GG, et al. Diabetic ketoacidosis promotes a prothrombotic state. Endocr Res 2003; 29(1): 73–82
Worly JM, Fortenberry JD, Hansen I, et al. Deep venous thrombosis in children with diabetic ketoacidosis and femoral central venous catheters. Pediatrics 2004; 113(1): e57–60
Gutierrez JA, Bagatell R, Samson MP, et al. Femoral central venous catheter-associated deep venous thrombosis in children with diabetic ketoacidosis. Crit Care Med 2003; 31(1): 80–3
Casteels K, Beckers D, Wouters C. Rhabdomyolysis in diabetic ketoacidosis. Pediatr Diabetes 2003; 4(1): 29–31
Koves IH, Neutze J, Donath S, et al. The accuracy of clinical assessment of dehydration during diabetic ketoacidosis in childhood. Diabetes Care 2004; 27(10): 2485–7
Hanas R, Donaghue K, Klingensmith G, et al., editors of the ISPAD. Clinical practice consensus guidelines 2006–2007. Pediatr Diabetes 2006; 7(6): 341–2
Wolfsdorf J, Glaser N, Sperling MA, et al. Diabetic ketoacidosis in infants, children and adolescents: a consensus statement from the American Diabetes Association. Diabetes Care 2006; 29(5): 1150–9
Kitabchi AE, Umpierrez GE, Murphy MB, et al., on behalf of the American Diabetes Association. Hyperglycemic crises in diabetes. Diabetes Care 2004; 27(Suppl. 1) S94–102
Edge JA, Jakes RW, Roy Y, et al. The UK case-control study of cerebral oedema complicating diabetic ketoacidosis in children. Diabetologia 2006; 49(9): 2002–9
Hoorn EJ, Carlotti AP, Costa LA, et al. Preventing a drop in effective plasma osmolality to minimize the likelihood of cerebral edema during treatment of children with diabetic ketoacidosis. J Pediatr 2007; 150(5): 467–73
Wilson HK, Keuer SP, Lea AS, et al. Phosphate therapy in diabetic ketoacidosis. Arch Intern Med 1982; 142(3): 517–20
Rachmiel M, Perlman K, Daneman D. Insulin analogues in children and teens with type 1 diabetes: advantages and caveats. Pediatr Clin North Am 2005; 52(6): 1651–75
Hirsch IB. Insulin analogues. N Engl J Med. 2005; 352(2): 174–83
Danne T, Becker RH, Heise T, et al. Pharmacokinetics, prandial glucose control, and safety of insulin glulisine in children and adolescents with type 1 diabetes. Diabetes Care 2005; 28(9): 2100–5
Homko C, Deluzio A, Jimenez C, et al. Comparison of insulin aspart and lispro: pharmacokinetic and metabolic effects. Diabetes Care 2003; 26(7): 2027–31
Stephens JM, Sulway MJ, Watkins PJ. Relationship of blood acetoacetate and 3-hydroxybutyrate in diabetes. Diabetes 1971; 20(7): 485–9
Noyes KJ, Crofton P, Bath LE, et al. Hydroxybutyrate near-patient testing to evaluate a new end-point for intravenous insulin therapy in the treatment of diabetic ketoacidosis in children. Pediatr Diabetes 2007 Jun; 8(3): 150–6
Prisco F, Picardi A, Iafusco D, et al. Blood ketone bodies in patients with recent-onset type 1 diabetes (a multicenter study). Pediatr Diabetes 2006; 7(4): 223–8
Green SM, Rothrock SG, Ho JD, et al. Failure of adjunctive bicarbonate to improve outcome in severe pediatric diabetic ketoacidosis. Ann Emerg Med 1998; 31(1): 41–8
Taylor CJ, Nicola PA, Wang S, et al. Transporters involved in regulation of intracellular pH in primary cultured rat brain endothelial cells. J Physiol 2006; 576 (Pt 3): 769–85
Dunger DB, Edge JA. Predicting cerebral edema during diabetic ketoacidosis. N Engl J Med 2001 Jan; 344(4): 302–3
Dunger DB, Sperling MA, Acerini CL, et al. ESPE/LWPES consensus statement on diabetic ketoacidosis in children and adolescents. Arch Dis Child 2004; 89(2): 188–94
Dunger DB, Sperling MA, Acerini CL, et al. European Society for Paediatric Endocrinology/Lawson Wilkins Pediatric Endocrine Society consensus statement on diabetic ketoacidosis in children and adolescents. Pediatrics 2004; 113(2): el33–40
Bastin ME, Carpenter TK, Armitage PA, et al. Effects of dexamethasone on cerebral perfusion and water diffusion in patients with high-grade glioma. Am J Neuroradiol 2006; 27: 402–8
Shabbir N, Oberfield SE, Corrales R, et al. Recovery from symptomatic brain swelling in diabetic ketoacidosis. Clin Pediatr (Phila) 1992; 31(9): 570–3
Tasker RC, Lutman D, Peters MJ. Hyperventilation in severe diabetic ketoacidosis. Pediatr Crit Care Med 2005; 6(4): 405–11
Marcin JP, Glaser N, Barnett P, et al., on behalf of The Pediatric Emergency Medicine Collaborative Research Committee. Factors associated with adverse outcomes in children with diabetic ketoacidosis-related cerebral edema. J Pediatr 2002; 141(6): 793–7
Franklin B, Liu J, Ginsberg-Fellner F. Cerebral edema and ophthalmoplegia reversed by mannitol in new case of insulin-dependent diabetes mellitus. Pediatrics 1982; 69(1): 87–90
Roberts MD, Slover RH, Chase HP. Diabetic ketoacidosis with intracerebral complications. Pediatr Diabetes 2001; 2(3): 109–14
Yildizdas D, Altunbasak S, Celik U, et al. Hypertonic saline treatment in children with cerebral edema. Indian Pediatr 2006; 43(9): 771–9
Kamat P, Vats A, Gross M, et al. Use of hypertonic saline for the treatment of altered mental status associated with diabetic ketoacidosis. Pediatr Crit Care Med 2003; 4(2): 239–42
Delia Manna T, Steinmetz L, Campos PR, et al. Subcutaneous use of a fast-acting insulin analog: an alternative treatment for pediatric patients with diabetic ketoacidosis. Diabetes Care 2005; 28(8): 1856–61
Umpierrez GE, Cuervo R, Karabell A, et al. Treatment of diabetic ketoacidosis with subcutaneous insulin aspart. Diabetes Care 2004; 27(8): 1873–8
Umpierrez GE, Latif K, Stoever J, et al. Efficacy of subcutaneous insulin lispro versus continuous intravenous regular insulin for the treatment of patients with diabetic ketoacidosis. Am J Med 2004; 117(5): 291–6
Ersoz HO, Ukinc K, Kose M, et al. Subcutaneous lispro and intravenous regular insulin treatments are equally effective and safe for the treatment of mild and moderate diabetic ketoacidosis in adult patients. Int J Clin Pract 2006; 60(4): 429–33
Lam TI, Anderson SE, Glaser N, et al. Bumetanide reduces cerebral edema formation in rats with diabetic ketoacidosis. Diabetes 2005; 54(2): 510–6
Acknowledgments
No sources of funding were used to assist in the preparation of this review. Lynne L. Levitsky has received consulting fees and honoraria from sanofi-aventis. Nicole A. Sherry has no conflicts of interest that are directly relevant to the content of this review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sherry, N.A., Levitsky, L.L. Management of Diabetic Ketoacidosis in Children and Adolescents. Pediatr-Drugs 10, 209–215 (2008). https://doi.org/10.2165/00148581-200810040-00002
Published:
Issue Date:
DOI: https://doi.org/10.2165/00148581-200810040-00002