Abstract
Background and objective
Lowering BP to normal levels without quality of life deterioration is the most important means of reducing cardiovascular risk. Recent studies have challenged the position of β-adrenoceptor antagonists (β-blockers) as first-line antihypertensive drugs. Nebivolol is a third-generation, highly selective β1-blocker that causes vasodilation through nitric oxide (NO) release. This meta-analysis investigates the efficacy and tolerability of nebivolol compared with other antihypertensive drugs and placebo in patients with hypertension.
Methods
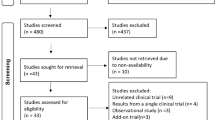
Twelve randomized controlled studies were included in which nebivolol 5 mg once daily was compared with the recommended clinical doses of other antihypertensive drugs (n = 9), placebo (n = 2), and both (n = 1). The clinical studies were selected after a MEDLINE search up to 2007 using the key words ‘nebivolol’ and ‘hypertension.’
Results
Antihypertensive response rates (the percentage of patients achieving target BP levels or a defined DBP reduction) were higher with nebivolol than with ACE inhibitors (odds ratio [OR] 1.92; p = 0.001) and all antihypertensive drugs combined (OR 1.41; p = 0.001) and similar to β-blockers, calcium channel antagonists (CCAs) and the angiotensin receptor antagonist (ARA) losartan. Moreover, a higher percentage of patients receiving nebivolol achieved target BP levels compared with patients treated with losartan (OR 1.98; p = 0.004), CCAs (OR 1.44; p = 0.024), and all antihypertensive drugs combined (OR 1.35; p = 0.012). The percentage of patients experiencing adverse events did not differ between nebivolol and placebo; adverse event rates were significantly lower with nebivolol than losartan (OR 0.52; p = 0.016), other β-blockers (OR 0.56; p = 0.007), nifedipine (OR 0.49; p < 0.001), and all antihypertensive drugs combined (OR 0.59; p < 0.001).
Conclusion
Results of previous pharmacokinetic studies suggest that nebivolol 5 mg may not conform completely to the definition of a classic β-blocker demonstrating additional antihypertensive effect due to endothelial NO release-mediated vasodilation. This meta-analysis showed that nebivolol 5 mg achieved similar or better rates of treatment response and BP normalization than other drug classes and other antihypertensive drugs combined, with similar tolerability to placebo and significantly better tolerability than losartan, CCAs, other β-blockers, and all antihypertensive drugs combined. Although not definitive, this meta-analysis suggests that nebivolol 5 mg is likely to have advantages over existing antihypertensives and may have a role in the first-line treatment of hypertension.






Similar content being viewed by others
References
Carlberg B, Samuelsson O, Lindholm LH. Atenolol in hypertension: is it a wise choice? Lancet 2004; 364: 1684–9.
Lindholm LH, Carlberg B, Samuelsson O. Should beta blockers remain first choice in the treatment of primary hypertension? A meta-analysis. Lancet 2005; 366: 1545–53.
Dahlof B, Devereux RB, Kjeldsen SE, et al. Cardiovascular morbidity and mortality in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet 2002; 359: 995–1003.
Dahlof B, Sever PS, Poulter NR, et al. Prevention of cardiovascular events with an antihypertensive regimen of amlodipine adding perindopril as required versus atenolol adding bendroflumethiazide as required, in the Anglo-Scandinavian Cardiac Outcomes Trial-Blood Pressure Lowering Arm (ASCOT-BPLA): a multicentre randomised controlled trial. Lancet 2005; 366: 895–906.
Van Bortel LM, de Hoon JN, Kool MJ, et al. Pharmacological properties of nebivolol in man. Eur J Clin Pharmacol 1997; 51: 379–84.
Dawes M, Brett SE, Chowienczyk PJ, et al. The vasodilator action of nebivolol in forearm vasculature of subjects with essential hypertension. Br J Clin Pharmacol 1999; 48: 460–3.
Tzemos N, Lim PO, MacDonald TM. Nebivolol reverses endothelial dysfunction in essential hypertension: a randomized, double-blind, crossover study. Circulation 2001; 104: 511–4.
Zanchetti A. Clinical pharmacodynamics of nebivolol: new evidence of nitric oxide-mediated vasodilating activity and peculiar haemodynamic properties in hypertensive patients. Blood Press Suppl 2004; 1: 17–32.
Brixius K, Bundkirchen A, Bolck B, et al. Nebivolol, bucindolol, metoprolol and carvedilol are devoid of intrinsic sympathomimetic activity in human myocardium. Br J Pharmacol 2001; 133: 1330–8.
Agabiti Rosei E, Rizzoni D. Metabolic profile of nebivolol, a β-adrenoceptor antagonist with unique characteristics. Drugs 2007; 67: 1097–107.
Celik T, Iyisoy A, Kursaklioglu H, et al. Comparative effects of nebivolol and metoprolol on oxidative stress, insulin resistance, plasma adiponectin and soluble P-selectin levels in hypertensive patients. J Hypertens 2006; 24: 591–6.
Troost R, Schwedhelm E, Rojczyk S, et al. Nebivolol decreases systemic oxidative stress in healthy volunteers. Br J Clin Pharmacol 2000; 50: 377–9.
Ambrosioni E, Borghi C. Tolerability of nebivolol in head-to-head clinical trials versus other cardioselective β-blockers in the treatment of hypertension: a meta-analysis. High Blood Press Cardiovasc Prev 2005; 12: 27–35.
Pesant Y, Marc-Aurèle J, Bielmann P, et al. Metabolic and antihypertensive effects of nebivolol and atenolol in normometabolic patients with mild-to-moderate hypertension. Am J Ther 1999; 6: 137–47.
Hauf-Zachariou U, Widmann L, Zülsdorf B, et al. A double-blind comparison of the effects of carvedilol and captopril on serum lipid concentrations in patients with mild to moderate essential hypertension and dyslipidaemia. Eur J Clin Pharmacol 1993; 45: 95–100.
Giugliano D, Acampora R, Marfella R, et al. Metabolic and cardiovascular effects of carvedilol and atenolol in non-insulin-dependent diabetes mellitus and hypertension: a randomized, controlled trial. Ann Intern Med 1997; 126: 955–9.
Ruffolo Jr RR, Feuerstein GZ. Pharmacology of carvedilol: rationale for use in hypertension, coronary artery disease, and congestive heart failure. Cardiovasc Drugs Ther 1997; 11 Suppl. 1: 247–56.
Mancia G, De Backer G, Dominiczak A, et al. 2007 Guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens 2007; 25: 1105–87.
Rosendorff C, Black HR, Cannon CP, et al. Treatment of hypertension in the prevention and management of ischemic heart disease: a scientific statement from the American Heart Association Council for High Blood Pressure Research and the Councils on Clinical Cardiology and Epidemiology and Prevention. Circulation 2007; 115: 2761–88.
Chobanian AV, Bakris GL, Black HR, et al. Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003; 42: 1206–52.
Lindholm LH. The problem of uncontrolled hypertension. J Hum Hypertens 2002; 14: 231–6.
Staessen JA, Wang JG, Thijs L. Cardiovascular protection and blood pressure reduction: a meta-analysis [published erratum appears in Lancet 2002; 359: 360]. Lancet 2001; 358: 1305–15.
Perkovic V, Ninomiya T, Arima H, et al. chronic kidney disease, cardiovascular events, and the effects of perindopril-based blood pressure lowering: data from the PROGRESS Study. J Am Soc Nephrol 2007; 18: 2766–72.
Waeber B, Burnier M, Brunner HR. Compliance with antihypertensive therapy. Clin Exp Hypertens 1999; 21: 973–85.
Frishman WH. Importance of medication adherence in cardiovascular disease and the value of once-daily treatment regimens. Cardiol Rev 2007; 15: 257–63.
Van Bortel LM, Breed JG, Joosten J, et al. Nebivolol in hypertension: a double-blind placebo-controlled multicenter study assessing its antihypertensive efficacy and impact on quality of life. J Cardiovasc Pharmacol 1993; 21: 856–62.
Van Nueten L, Dupont AG, Vertommen C, et al. A dose-response trial of nebivolol in essential hypertension. J Hum Hypertens 1997; 11: 139–44.
Van Nueten L, Taylor FR, Robertson JIS. Nebivolol vs atenolol and placebo in essential hypertension: a double-blind randomised trial. J Hum Hypertens 1998; 12: 135–40.
Van Nueten L, Schelling A, Vertommen C, et al. Nebivolol vs enalapril in the treatment of essential hypertension: a double-blind randomised trial. J Hum Hypertens 1997; 11: 813–9.
Agabiti Rosei E, Rizzoni D, Comini S, et al., on behalf of the Nebivolol-Lisinopril Study Group. Evaluation of the efficacy and tolerability of nebivolol versus lisinopril in the treatment of essential arterial hypertension: a randomized, multicenter, double-blind study. Blood Press 2003; 12 Suppl. 1: 30–5.
Van Bortel LM, Bulpitt CJ, Fici F. Quality of life and antihypertensive effect with nebivolol and losartan. Am J Hypertens 2005; 18: 1060–6.
Uhlir O, Fejfusa M, Havranek K, et al. Nebivolol versus metoprolol in the treatment of hypertension. Drug Invest 1991; 3 Suppl. 1: 107–10.
Grassi G, Trevano FQ, Facchini A, et al. Efficacy and tolerability profile of nebivolol vs. atenolol in mild-to-moderate essential hypertension: results of a double-blind randomized multicentre trial. Blood Press Suppl 2003; 2: 35–40.
Czuriga I, Riecansky I, Bodnar J, et al., for the NEBIS Investigators Group. Comparison of the new cardioselective beta-blocker nebivolol with bisoprolol in hypertension: the Nebivolol, Bisoprolol Multicenter Study (NEBIS). Cardiovasc Drugs Ther 2003; 17: 257–63.
Van Nueten L, Lacourciere Y, Vyssoulis G, et al. Nebivolol versus nifedipine in the treatment of essential hypertension: a double blind, randomized, comparative trial. Am J Ther 1998; 5: 237–43.
Lacourciere Y, Poirier L, Lefebvre J, et al. Comparative effects of a new cardioselective beta-blocker nebivolol and nifedipine sustained release on 24 hour ambulatory blood pressure and plasma lipoproteins. J Clin Pharmacol 1992; 32: 660–6.
Mazza A, Gil-Extremera B, Maldonato A, et al. Nebivolol vs amlodipine as first-line treatment of essential arterial hypertension in the elderly. Blood Press 2002; 11: 182–8.
Lacourciere Y, Lefebvre J, Poirier L, et al. Treatment of ambulatory hypertensives with nebivolol orhydrochlorothiazide alone and in combination. A randomized, double-blind, placebo-controlled, factorial-design trial. Am J Hypertens 1994; 7: 137–45.
Bremner AD. Antihypertensive medication and quality of life-silent treatment of a silent killer? Cardiovasc Drugs Ther 2002; 16: 353–64.
Kostis JB, Shelton B, Gosselin G, et al. Adverse effects of enalapril in the Studies of Left Ventricular Dysfunction (SOLVD). Am Heart J 1996; 131: 350–5.
Ostergren J, Storstein L, Karlberg BE, et al. Quality of life in hypertensive patients treated with either carvedilol or enalapril. Blood Press 1996; 5: 41–9.
Doumas M, Tsakiris A, Douma S, et al. Beneficial effects of switching from beta-blockers to nebivolol on the erectile function of hypertensive patients. Asian J Androl 2006: 8: 177–82.
Brixius K, Middeke M, Lichtenthal A, et al. Nitric oxide, erectile dysfunction and beta-blocker treatment (MR NOED study): benefit of nebivolol versus metoprolol in hypertensive men. Clin Exp Pharmacol Physiol 2007; 34: 327–31.
Boydak B, Nalbantgil S, Fici F, et al. A randomised comparison of the effects of nebivolol and atenolol with and without chlorthalidone on the sexual function of hypertensive men. Clin Drug Invest 2005; 25: 409–16.
Van Bortel LM, van Baak MA. Exercise tolerance with nebivolol and atenolol. Cardiovasc Drugs Ther 1992; 6: 239–47.
Predel HG, Mainka W, Schillings W, et al. Integrated effects of vasodilating β-blocker nebivolol on exercise performance, energy metabolism, cardiovascular and neurohormonal parameters in physically active patients with arterial hypertension. J Hum Hypertens 2001; 15: 715–21.
Neutel JM, Schnaper H, Cheung DG, et al. Antihypertensive effects of beta-blockers administered once daily: 24-hour measurements. Am Heart J 1990; 120: 166–71.
Triposkiadis F, Giamouzis G, Kelepeshis G, et al. Acute hemodynamic effects of moderate doses of nebivolol versus metoprolol in patients with systolic heart failure. Int J Clin Pharmacol Ther 2007; 45: 71–7.
Krukemyer JJ, Boudoulas H, Binkley PF, et al. Comparison of hypersensitivity to adrenergic stimulation after abrupt withdrawal of propranolol and nadolol: influence of half-life differences. Am Heart J 1990; 120: 572–9.
Mayor S. NICE removes beta blockers as first line treatment for hypertension. BMJ 2006; 333: 8.
Pedersen ME, Cockcroft JR. The vasodilatory beta-blockers. Curr Hypertens Rep 2007; 9: 269–77.
Andre DE, Arnet U, Yang Z, et al. Nebivolol inhibits human aortic smooth muscle cell growth: effects on cell cycle regulatory proteins. J Cardiovasc Pharmacol 2000; 35: 845–8.
Van Bortel LM, Hoeks AP, Kool MJ, et al. Introduction to large artery properties as a target for risk reduction by antihypertensive therapy. J Hypertens 1992; 10 Suppl. 6: S123–6.
van Merode T, Van Bortel LM, Smeets FA, et al. Verapamil and nebivolol improve carotid artery distensibility in hypertensive patients. J Hypertens 1989; 7 Suppl. 6: S262–3.
Falciani M, Rinaldi B, D’Agostino B, et al. Effects of nebivolol on human platelet aggregation. J Cardiovasc Pharmacol 2001; 38: 922–9.
Celik T, Yuksel UC, Iyisoy A, et al. Effects of nebivolol on platelet activation in hypertensive patients: a comparative study with metoprolol. Int J Cardiol 2007; 116: 206–11.
Acknowledgments
Editorial assistance was provided by Wolters Kluwer Health. No sources of funding were used to assist in the preparation of this study. Professor Van Bortel has received honoraria from Menarini for presentations on nebivolol and nitric oxide at scientific meetings. Dr Mascagni has provided statistical expertise to Menarini for nebivolol.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Van Bortel, L.M., Fici, F. & Mascagni, F. Efficacy and Tolerability of Nebivolol Compared with Other Antihypertensive Drugs. Am J Cardiovasc Drugs 8, 35–44 (2008). https://doi.org/10.2165/00129784-200808010-00005
Published:
Issue Date:
DOI: https://doi.org/10.2165/00129784-200808010-00005