Abstract
The National Institute for Health and Clinical Excellence (NICE) is required to consider cost effectiveness when issuing guidance about the use of health technologies within the UK NHS. Cost effectiveness is a means of supporting a system objective of maximizing population health gain from the available budget.
There is a range of sources of variation between individuals in disease prognosis, and in the costs and effects of health technologies. It is often possible to explain some of this variation on the basis of the clinical and sociodemographic characteristics of patients. This facilitates subgroup-specific estimates of parameters in decision analytic models and provides a means of assessing heterogeneity in cost effectiveness between different types of patient. Given the objective of the NHS, there is a clear need for NICE, and similar decision makers in other systems, to reflect this heterogeneity by being as specific as possible about the characteristics of the recipients of new treatments.
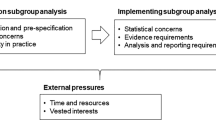
The use of subgroup analysis in cost-effectiveness analysis raises a number of methodological questions that have been given little consideration in the literature. They include a need to define the possible sources of heterogeneity that exist, which extends beyond relative treatment effect (which is the focus of clinical trial analysis) to include, for example, sources relating to baseline event rates. There is also the issue of how heterogeneity in model parameters should be estimated and how uncertainty should be appropriately quantified. A major issue also exists concerning the appropriateness, in terms of equity, of using all or some of the subgroup analyses as a basis of decision making. NICE needed to consider these and other issues when updating its methods guidance.

Similar content being viewed by others
References
Claxton K, Briggs A, Buxton M, et al. Value based pricing for NHS dmgs: an opportunity not to be missed? BMJ 2008; 336: 251–254
Culyer A, McCabe C, Briggs A, et al. Searching for a threshold, not setting one: the role of the National Institute for Health and Clinical Excellence. J Health Serv Res Pol 2007; 12: 56–58
Coyle D, Buxton MJ, O’Brien BJ. Stratified cost-effectiveness anaylsis: a framework for establishing efficient limited use criteria. Health Econ 2003; 12: 421–427
Stinnett AA, Mullahy J. Net health benefits: a new framework for the analysis of uncertainty in cost-effectiveness analysis. Med Decis Making 1998; 18 Suppl.: S68–S80
Mark DB, Hlatky MA, Califf RM, et al. Cost effectiveness of thrombolytic therapy with tissue plasminogen activator as compared with streptokinase for acute myocardial infarction. N Engl J Med 1995; 332: 1418–1424
Gail M, Simon R. Testing for qualitative interactions between treatment effects and patient subsets. Biometrics 1985; 41: 361–372
Briggs A, Mihaylova B, Sculpher MJ, et al. The cost-effectiveness of perindopril in reducing cardiovascular events in patients with stable coronary artery disease using data from the EUROPA study. Heart 2007; 93: 1081–1086
Henriksson M, Epstein DM, Palmer SJ, et al. The cost-effectiveness of an early interventional strategy in non-ST-elevation acute coronary syndrome based on the RITA 3 trial. Heart 2008; 94: 717–723
Sloan F, Feldman RD, Steinwald AB. Effects of teaching on hospital costs. J Health Econ 1983; 2: 1–28
Ramsay CR, Grant AM, Wallace SA, et al. Statistical assessment of the learning curves of health technologies. Health Technol Assess 2001; 5 (12): 1–104
Owens DK, Nease RF. A normative analytic framework for development of practice guidelines for specific clinical populations. Med Decis Mak 1997; 17 (4): 409–426
Sculpher MJ, Gafni A. Recognizing diversity in public preferences: the use of preference sub-groups in cost-effectiveness analysis. Health Econ 2001; 10: 317–324
Oxman AD, Guyatt GH. A consumer’s guide to subgroup analyses. Ann Intern Med 1992 Jan 1; 116 (1): 78–84
Claxton K. The irrelevance of inference: a decision-making approach to the stochastic evaluation of health care technologies. J Health Econ 1999; 18: 342–364
National Institute for Health and Clinical Excellence. Guide to the methods of technology appraisal. London: NICE, 2004
Thompson SG, Smith TC, Sharp SJ. Investigating underlying risk as a source of heterogeneity in meta-analysis. Stat Med 1997; 16: 2741–2758
Cooper NJ, Sutton AJ, Abrams KR. Decision analytical economic modelling within a Bayesian framework: application to prophylactic antibiotics use for caesarean section. Stat Methods Med Res 2002; 11: 491–512
Bagust A, Grayson A, Palmer N, et al. Cost-effectiveness of a drug-eluting coronary artery stenting in a UK setting: cost-utility study. Heart 2006; 92 (1): 6–74
Epstein DM, Chalabi Z, Claxton K, et al. Efficiency, equity and budgetary policies: informing decisions using mathematical programming. Med Dec Making 2007; 27: 128–137
National Institute for Health and Clinical Excellence. Social value judgements: principles for the development of NICE guidance [draft for public consultation]. London: NICE, 2008
Acknowledgements
This paper was initially prepared as a briefing paper for NICE as part of the process of updating the Institute’s 2004 Guide to the Methods of Technology Appraisal. The work was funded by NICE through its Decision Support Unit (DSU), which is based at the universities of Sheffield, Leicester, York, Leeds and at the London School of Hygiene and Tropical Medicine.
The author has no conflicts of interest that are directly relevant to the content of this article.
The author gratefully acknowledges Karl Claxton, John Brazier and Alex Sutton for comments on earlier drafts. Any remaining errors are the responsibility of the author alone.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sculpher, M. Subgroups and Heterogeneity in Cost-Effectiveness Analysis. Pharmacoeconomics 26, 799–806 (2008). https://doi.org/10.2165/00019053-200826090-00009
Published:
Issue Date:
DOI: https://doi.org/10.2165/00019053-200826090-00009