Abstract
Objective: To compare the relative cost effectiveness of salmeterol (50μg)/ fluticasone propionate (100μg) with that of oral montelukast (10mg) as initial maintenance therapy in patients with persistent asthma uncontrolled on short-acting β2-agonist therapy alone.
Study design: A cost-effectiveness analysis was performed based on effectiveness and resource utilisation data that was prospectively collected from a randomised, double-blind, double-dummy, 12-week trial.
Patients and methods: Patients (>15 years of age) who had asthma for at least 6 months. Effectiveness measurements in this analysis included improvement in forced expiratory volume in 1 second (FEV1) and symptom-free days (SFDs). Cost of asthma drug treatment as well as costs related to an asthma exacerbation were used in the cost analysis. The study assumed a payer’s perspective. All costs are in 2001 US dollars.
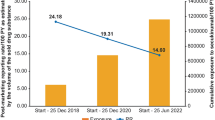
Results: Of the 423 patients eligible for the study, 211 were randomised to salmeterol/fluticasone propionate and 212 to montelukast. Treatment with salmeterol/fluticasone propionate resulted in a significantly higher proportion of patients who achieved a 12% increase in FEV1 (successful treatment) [salmeterol/fluticasone propionate: 71% vs montelukast: 39%; p < 0.001] and percentage of SFDs (salmeterol/fluticasone propionate: 46.8% vs montelukast: 21.5%; p < 0.001) compared with montelukast. The mean daily costs per successfully treated patient were lower in the salmeterol/fluticasone propionate group ($US5.03, 95% CI $US4.61 to $US5.50) compared with the montelukast group ($US8.25, 95% CI $US6.98 to $US9.93). Furthermore, per patient mean daily cost per SFD was lower with salmeterol/fluticasone propionate ($US7.63, 95% CI $US6.90 to $US8.50) compared with montelukast ($US14.89, 95% CI $US12.36 to $US17.98). Incremental cost-effectiveness ratios (ICERs) showed that the additional costs to achieve these benefits with salmeterol/fluticasone propionate were minimal. With regards to improvement in lung function, the ICER was $US1.33 (95% CI $US0.80 to $US2.02) and with regards to SFD, the ICER was $US1.69 (95% CI $US1.01 to $US2.48). Sensitivity analysis demonstrated the stability of the results over a range of assumptions.
Conclusions: From a third-party payer perspective, this analysis shows that based on increased efficacy and only a slight increase in cost, twice-daily treatment with salmeterol/fluticasone propionate is more cost effective than once-daily treatment with montelukast as initial maintenance therapy for persistent asthma. This finding complements the results of the clinical analyses indicating that treatment of both inflammation and bronchoconstriction with products such as salmeterol/fluticasone propionate may be more cost effective as initial maintenance asthma therapy than the use of leukotriene modifiers such as montelukast.








Similar content being viewed by others
References
National Institutes of Health. Practical guide for the diagnosis and management of asthma. Washington (DC): US Department of Health and Human Services, National Institutes of Health; 1997. Publication No.: 97-4053
Centers for Disease Control and Prevention. Forecasted state-specific estimates of self-reported prevalence in the United States, 1998. Morb Mortal Wkly Rep 1998; 47: 1022–5
Centers for Disease Control and Prevention. National Center for Health Statistics Fact Sheet [online]. Available from URL: http://www.cdc.gov/nchs/products/pubs/pubd/hestats/asthma/asthma.htm [Accessed 2002 Jul 24]
Weiss K, Sullivan S. The health economics of asthma and rhinitis: assessing the economic impact. J Allergy Clin Immunol 2001; 107: 3–8
Lundback B, Jenkins C, Price M, et al. Cost-effectiveness of salmeterol/fluticasone propionate combination product 50/250 μg twice daily and budesonide 800 μg twice daily in the treatment of adults and adolescents with asthma. Respir Med 2000; 94: 724–32
Hoskins G, McCowan C, Neville R, et al. Risk factors and costs associated with an asthma attack. Thorax 2000; 55: 19–24
Brinke A, Ouwerkerk M, Zwinderman A, et al. Psychopathology in patients with severe asthma is associated with increased health care utilization. Am J Respir Crit Care Med 2001; 163: 1093–6
Reiss T, Chervinsky P, Dockhorn R, et al. Montelukast, a once daily leukotriene receptor antagonist in the treatment of chronic asthma. Arch Intern Med 1998; 158: 1213–20
Calhoun W, Nelson H, Nathan R, et al. Comparison of fluticasone propionate-salmeterol combination therapy and montelukast in patients who are symptomatic on short acting β2 agonists alone. Am J Respir Crit Care Med 2001; 164: 759–63
National Heart, Lung, and Blood Institute. National Asthma Education and Prevention Task Force on the cost effectiveness, quality of care and financing of asthma care. Bethesda (MD): National Institutes of Health, 1996. Publication no. 55-807
Current competitive price positions, copyright © 2001. Facts and Comparisons 2002. Available from URL: http://www.factsandcomparisons.com [Accessed 2002 Sep 25]
Cardinale V, editor. 2001 Drug topics red book. Montvale (NJ): Medical Economics Co, 2001
Stanford R, McLaughlin T, Okamoto L. The cost of asthma in the emergency department and hospital. Am J Respir Crit Care Med 1999; 160: 211–5
Crane M. Charge what you will...Reimbursements are shrinking. Med Econ 2000; 75: 128–38
Campbell F, Hollis S. What is mean by intention to treat analysis: survey of published randomized controlled trials. BMJ 1999; 319: 670–4
Rutten-van Molken M, Van Doorslaer E, Jansen M, et al. Costs and effects of inhaled corticosteroids and bronchodilators in asthma and chronic obstructive pulmonary disease. Am J Respir Crit Care Med 1995; 151: 975–82
Menendez R, Stanford RH, Edwards L, et al. Cost-efficacy analysis of fluticasone propionate versus zafirlukast in patients with persistent asthma. Pharmacoeconomics 2001; 19 (8): 865–74
Volmer T, Kielhorn A, Weber HH, et al. Cost effectiveness of fluticasone propionate and flunisolide in the treatment of corticosteroid-naive patients with moderate asthma. Pharmacoeconomics 1999 Nov; 16 (5 Pt 2): 525–31
Lord J, Asante M. Estimating uncertainty ranges for costs by the bootstrap procedure combined with probabilistic sensitivity analysis. Health Econ 1999; 8: 323–33
Kielhorn A, Schulenburg J. The health economic handbook. 2nd ed. Chester: Adis International Ltd, 2000
Drummond M, Brien B, Stoddart G, et al. Methods for economic evaluation of health care programs. 2nd ed. Oxford: Oxford University Press, 1997
Pearlman D, White M, Lieberman A. Fluticasone propionate/salmeterol combination compared with montelukast for the treatment of persistant asthma. Ann Allergy Asthma Immunol 2002; 88: 227–35
Stempel D, O’Donnell J, Myer J. Inhaled corticosteroids plus salmeterol or montelukast: effects on resource utilisation and costs. J Allergy Clin Immunol 2002; 109: 433–9
O’Conner R, O’Donnell J, Pinto L, et al. Two year retrospective economic evaluation of three dual controller therapies used in the treatment of asthma. Chest 2002; 121: 1028–35
Acknowledgements
This study was sponsored by a grant from GlaxoSmithKline Inc., Research Triangle Park, NC. Dr Ketan Sheth has received speakers honoria and research grants, and is a consultant to GlaxoSmithKline and Merck.
The authors wish to thank Dr Christopher Leibman and Dr Dev S. Pathak for their contributions with respect to methodology as well as providing valuable insights and thoughtful reviews of earlier drafts of this manuscript. Dr Leibman was a former fellow with Global Health Outcomes at GlaxoSmithKline and Dr Pathak is the Director of the Center for Health Outcomes, Policy, and Evaluation Studies (HOPES) at the Ohio State University.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sheth, K., Borker, R., Emmett, A. et al. Cost-Effectiveness Comparison of Salmeterol/Fluticasone Propionate versus Montelukast in the Treatment of Adults with Persistent Asthma. Pharmacoeconomics 20, 909–918 (2002). https://doi.org/10.2165/00019053-200220130-00004
Published:
Issue Date:
DOI: https://doi.org/10.2165/00019053-200220130-00004