Abstract
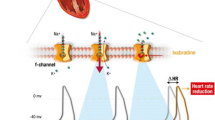
High heart rates predict cardiovascular morbidity and mortality in the healthy population, in hypertensive patients, and in those with coronary heart disease (CHD) or heart failure. If channel inhibition with ivabradine is an effective approach to reduce heart rate pharmacologically, with the prospect of preventing complications. The antianginal effects of heart rate-lowering with ivabradine have been shown to be similar to those with β-adrenoceptor antagonists (β-blockers) in patients with CHD. The BEAUTIfUL and SHIfT trials will provide evidence on whether If channel inhibition with ivabradine is able to reduce mortality and morbidity in patients with CHD with impaired left ventricular function and heart failure.
Future perspectives for additional study are potential roles of ivabradine in the treatment of hypertension and atherosclerosis, and their complications. Further clinical and mechanistic studies to clarify the pathophysiological background are needed to fully define the role of heart rate reduction in the broad spectrum of cardiovascular interventions.





Similar content being viewed by others
References
Levine JH. Rest rate and life expectancy. J Am Coll Cardiol 1997; 30: 1104–6
Coburn FA, Ross MG, Rivera MS. Observations on the relation of heart rate, life span, weight and mineralization in the digoxin-treated A/J mouse. Hopkins Med 1971; 128: 169–93
Singh BN. Morbidity and mortality in cardiovascular disorders: impact of reduced heart rate. J Cardiovasc Pharmacol Ther 2001; 6: 313–31
Kannel W, Wilson P, Blaire S. Epidemiologic assessment of the role of physical activity and fitness in development of cardiovascular disease. Am Heart J 1985; 109: 876–85
Gillum R, Makuc D, Feldman J. Pulse rate, coronary heart disease, and death: the NHANES I epidemiologic follow-up study. Am Heart J 1991; 121: 172–7
Wilhelmsen I, Berglund G, Elmfeldt D, et al. The multifactor primary prevention trial in Goteborg, Sweden. Eur Heart J 1986; 7: 279–88
Dyer A, Perski V, Stamler J, et al. Heart rate as a prognostic factor for coronary heart disease and mortality: findings in three Chicago epidemiologic studies. Am J Epidemiol 1980; 112: 736–49
Goldberg R, Larson M, Levy D. Factors associated with survival to 75 years of age in middle-aged men and women: the Framingham study. Arch Intern Med 1996; 156: 505–9
Palatini P, Casiglia E, Julius S, et al. Heart rate: a risk factor for cardiovascular mortality in elderly men. Arch Intern Med 1999; 159: 585–92
Cole RC, Foody MJ, Blackstone HE, et al. Heart rate recovery after submaximal exercise testing as a predictor of mortality in a cardiovascularly healthy cohort. Ann Intern Med 2000; 132: 552–5
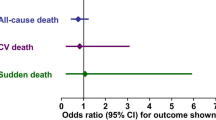
Jouven X, Empana J-P, Schwartz PJ, et al. Heart-rate profile during exercise as a predictor of sudden death. N Engl J Med 2005; 352: 1951–8
Mensink GB, Hofmeister H. The relationship between resting heart rate and all-cause cardiovascular and cancer mortality. Eur Heart J 1997; 18: 1404–10
Benetos A, Rucnichi A, Thomas F, et al. Influence of heart rate on mortality in a French population: role of age, gender and blood pressure. Hypertension 1999; 33: 44–52
Graham I, Atar D, Borch-Johnsen K, et al. European guidelines on cardiovascular disease prevention in clinical practice [executive summary]: Fourth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice Task Force Members (chairman-Prof. Graham). Euro Heart J 2007; 28: 2375–414
Levy RL, White PD, Stroud WD. Transient tachycardia: prognostic significance alone and in association with transient hypertension. JAMA 1945; 129: 585–8
Palatini P, Casiglia E, Pauletto P. Relation between physical training and ambulatory blood pressure in stage I hypertensive subjects: results of the HARVEST trial. Hypertension and Ambulatory Recording Venetia Study. Circulation 1994; 90: 2870–2
Gillman M, Kannel W, Belanger A. Influence of heart rate on mortality among persons with hypertension: the Framingham study. Am Heart J 1993; 125: 1148–54
Benetos A, Adamopoulos C, Bureau J-M. Determinants of accelerated progression of arterial stiffness in normotensive subjects and in treated hypertensive subjects over a 6-year period. Circulation 2002; 105: 1202–7
Mangioni AA, Mircoli L, Giannattasio C. Heart rate-dependence of arterial distensibility in vivo. J Hypertens 1996; 14: 897–901
Bassiouny HS, Zarins CK, Kadowaki MH, et al. Hemodynamic stress and experimental aortoiliac atherosclerosis. J Vasc Surg 1994; 19: 426–34
Beere PA, Glagov S, Zarins CK. Retarding effect of lowered heart rate on coronary atherosclerosis. Science 1984; 226: 180–2
Perski A, Hamsten A, Lindvall K, et al. Heart rate correlates with severity of coronary atherosclerosis in young postinfarction patients. Am Heart J 1988; 116: 1369–73
Diaz A, Bourassa GM, Guertin MC, et al. Long-term prognostic value of resting heart rate in patients with suspected or proven coronary artery disease. Eur Heart J 2005; 26: 967–74
Hjalmarson A, Gilpin E, Kjekshus J, et al. Influence of heart rate on mortality after acute myocardial infarction. Am J Cardiol 1990; 65: 547–53
Zuanetti G, Hernándes-Bernal F, Rossi A, et al. Relevance of heart rate as a prognostic factor in myocardial infarction: the GISSI experience. Eur Heart J 1999; 1 Suppl. H: H52–7
Kjekshus J, Gullestad L. Heart rate as a therapeutic target in heart failure. Eur Heart J 1999; 1 Suppl. H: H64–9
Borer JS, Fox K, Juilon P, et al. Antianginal and antiischemic effects of ivabradine, and I(f) inhibitor, in stable angina: a randomized, double-blind, multicentered, placebo-controlled trial. Circulation 2003; 207: 817–23
Mulder P, Barbier S, Chagraoui A, et al. Long-term heart rate reduction induced by the selective If current inhibitor ivabradaine improves left ventricular function and intrinsic myocardial structure in congestive heart failure. Circulation 2004; 109: 1674–9
Serruys PW, Unger F, Sousa JE, et al. Comparison of coronaryartery bypass surgery and stenting for the treatment of multivessel disease. N Engl J Med 2001; 344: 1117–24
Daly CA, Clemens F, Sendon JL, et al. The initial management of stable angina in Europe, from the Euro Heart Survey: a description of pharmacological management and revascularization strategies initiated within the first month of presentation to a cardiologist in the Euro Heart Survey of Stable Angina. Eur Heart J 2005; 26: 1011–22
Borer JS. Drug insight: If inhibitors as specific heart-rate-reducing agents [published erratum appears in Nat Clin Pract Cardiovasc Med 2006; 3 (4): 231]. Nat Clin Pract Cardiovasc Med 2004; 1(2): 103–9
Umana E, Solares A, Alpert MA. Tachycardia-induced cardiomyopathy. Am J Med 2003; 114: 51–5
Bowditch HP. Über die Eigentümlichkeit der Reizbarkeit, welche die Muskelfasern des Herzens zeigen. Ber Sachs Ges (Akad) Wiss 1871; 23: 652–85
Hasenfuss G, Reinecke H, Studer R, et al. Relation between myocardial function and expression of sarcoplasmatic reticulum Ca2+-ATPase in failing and nonfailing human myocardium. Circ Res 1994; 75: 434–42
Böhm M, La Rosee K, Schmidt U, et al. Force-frequency relationship and inotropic stimulation in the nonfailing and failing human myocardium: implications for the medical treatment of heart failure. Clin Invest 1992; 70: 421–5
Hoppe UC, La Rosée K, Larbig R, et al. Selective inhibition of the pacemaker channel If improves symptoms in severe dilated cardiomyopathy. Clin Res Cardiol 2007; 96: 243–6
Fox K, Ferrari R, Tendera M, et al. Rationale and design of a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease and left ventricular systolic dysfunction: the morBidity-mortality EvAlUaTion of the I(f) inhibitor ivabradine in patients with coronary disease and left ventricULar dysfunction (BEAUTIfUL) study. Am Heart J 2006; 152: 860–6
Current Controlled Trials. Effects of ivabradine on cardiovascular events in patients with moderate to severe chronic heart failure and left ventricular systolic dysfunction. A three-year randomised double-blind placebo-controlled international multicentre study (SHIft) [online]. Available from URL: http://www.controlled-trials.com/ISRCTN70429960 [Accessed 2007 Nov 7]
Reil JC, Böhm M. The role of heart rate in the development of cardiovascular disease. Clin Res Cardiol 2007; 96: 585–92
Fox K, Borer J, Camm A, et al. Resting heart rate in cardiovascular disease. J Am Coll Cardiol 2007; 50: 823–30
Acknowledgements
Dr M.B. Böhm is an established investigator at the Deutsche Forschungsgemeinschaft (German Research Foundation) [Klinishe Forshungsgruppe (clinical research group) KFO 186]. He serves as consultant for Servier and receives fees as a speaker. He is a member of the Executive Board of the SHIfT trial. Editorial support for the preparation of the manuscript was provided by Wolters Kluwer Health Medical Communications. The authors have no conflicts of interest directly relevant to the contents of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Böhm, M., Reil, JC. Perspectives of If Inhibition by Ivabradine in Cardiology. Drugs 67 (Suppl 2), 43–49 (2007). https://doi.org/10.2165/00003495-200767002-00006
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-200767002-00006