Summary
Synopsis
Alendronate is an aminobisphosphonate which appears to attenuate, rather than completely inhibiting bone turnover, by suppressing the activity of osteoclasts.
Clinical trials have established that 10 mg/day orally administered alendronate is the optimum dosage. Despite its poor bioavailability after oral administration, alendronate is highly effective at preventing bone loss associated with the absence of endogenous estrogen. A sustained increase in bone mass was observed during alendronate therapy without accelerated loss after withdrawal of the drug. Increased bone mass was associated with a reduction in the risk and rate of occurrence of vertebral fractures. A recent study demonstrated a 47% reduction in the risk of developing new radiographic vertebral fractures over 3 years in women with low bone mass and pre-existing vertebral fractures.
There have been few direct comparisons in clinical trials. However, when compared with calcium or low dosages of salmon calcitonin (salcatonin) therapy in women with postmenopausal osteoporosis, alendronate induced a sustained increase in bone mass during therapy that was not seen with the comparator.
In clinical trials alendronate was generally well tolerated when taken as recommended. Adverse events tended to be transient and usually associated with the upper gastrointestinal tract; the most common events included abdominal pain, nausea, dyspepsia, constipation and diarrhoea, which are also common with other bisphosphonates. Of potential concern are the small number of reports of patients developing oesophageal ulcération; however, this adverse event was attributed to noncompliance with the manufacturer’s recommendations for administration of the drug. In addition, alendronate has not been associated with osteomalacia.
Studies are still required to establish the long term efficacy of alendronate, particularly with regard to other available therapies. Although estrogen replacement therapy is generally considered the treatment of choice for the management of postmenopausal osteoporosis, many women are unable or unwilling to receive estrogens on a long term basis. Thus, alendronate, with its demonstrated beneficial effects and its good tolerability profile (when taken as recommended), is a promising alternative treatment option for the management of postmenopausal osteoporosis.
Pharmacodynamic Properties
Animal studies have indicated that at concentrations which elicit a physiological response, alendronate adsorbs to exposed bone surfaces and prevents the resorptive activity of osteoclasts without injuring them.
Alendronate increases bone strength in ovariectomised rats but the effect on bone stiffness is inconclusive. Nevertheless, the potential effects of alendronate on bone metabolism in the absence of estrogen have been demonstrated.
In postmenopausal women, biochemical markers of bone resorption were dose-dependently decreased 3 weeks after the initiation of alendronate (5 to 40 mg/day) and were reduced by at least 47% after 3 months. Similar decreases in markers of bone formation were observed 6 to 9 months after initiation of therapy. The depressed levels of all markers were maintained for the duration of therapy. Alendronate attenuated the increased level of bone turnover observed in postmenopausal women to within 1 standard deviation of that observed in premenopausal women.
In preclinical trials, alendronate showed a marked, dose-dependent efficacy in preventing osteoporosis related to non—weight bearing and immobilisation.
Pharmacokinetic Properties
The bioavailability of alendronate after oral administration is less than 1% and is reduced by the presence of food and divalent ions, such as calcium, in the stomach; an increase in gastric pH effects an increase in bioavailability. Alendronate is rapidly distributed from plasma; over 95% is cleared 6 hours after intravenous infusion, with the remainder being undetectable after a further 6 hours.
Elimination of alendronate appears to be exclusively via the urine in a multiphasic manner. Clinical studies have estimated a 10-year elimination half-life, suggesting a prolonged sequestration of the drug within bone tissue.
Alendronate has a high specific affinity for actively metabolising bone tissue, and to date, no metabolites have been identified. The latter may be a reflection of the stability of the drug.
Therapeutic Use in Postmenopausal Osteoporosis
In several large clinical studies in postmenopausal women with osteoporosis, alendronate (usually 5 to 20 mg/day) increased bone mineral density (BMD); effects were sustained over a period of 2 to 3 years during continued administration of the drug and for up to 12 months after discontinuation of treatment. For example, alendronate 10 mg/day for 3 years increased BMD in the lumbar spine 6.8 to 9.6% compared with decreases of approximately 0.7% noted in placebo recipients. There is evidence that both cortical and trabecular bone tissue are affected, suggesting that observed total bone mass increases of up to 1.6% with alendronate 10 mg/day were not merely the result of bone mineral redistribution.
In studies that monitored fracture rate, daily administration of alendronate 5 to 20mg compared with placebo prevented the rate of development of new vertebral fractures. A consistent but nonsignificant dose-related decrease in the risk of fractures was observed which was independent of age and the presence of existing fractures. Alendronate also reduced the severity of fractures which occurred. Pooled data from 5 studies of 2 to 3 years’ duration indicate that the relative risk rate and cumulative proportion of non-vertebral fractures were linear over time with placebo, but reduced in alendronate recipients. In addition, results from the Fracture Intervention Trial demonstrated a significant 47% decrease in the risk of developing new radiographic vertebral fractures in postmenopausel women with low bone mass and pre-existing vertebral fractures who received alendronate for 3 years compared with placebo recipients.
There have been few direct comparisons in clinical trials. However, when compared with calcium or low dosages of salmon calcitonin therapy in women with postmenopausal osteoporosis, alendronate induced a sustained increase in bone mass during therapy that was not seen with the comparator.
Tolerability
Alendronate 5 to 20 mg/day was generally well tolerated in clinical trials. The most commonly reported adverse events included abdominal pain, nausea, dyspepsia, constipation and diarrhoea which were reported in 3 to 7% of patients. However, there were no statistically significant differences between the frequency of adverse events reported by alendronate or placebo recipients. In addition, the incidence of adverse events does not appear to be dose related over this range.
Patient withdrawals due to therapy-related adverse events were generally low for both alendronate 5 to 20 mg/day (1.9 to 7.4%) and placebo (2 to 6.8%) recipients; events associated with the upper gastrointestinal tract were the most common reason for withdrawal.
Subsequent to marketing, a small number of patients (less than 1%) have developed oesophageal ulcération after taking alendronate. This adverse event has generally been attributed to noncompliance with the manufacturer’s administration recommendations.
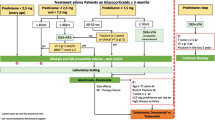
Dosage and Administration
The recommended daily oral dosage of alendronate is 10mg. To help improve bioavailability, the tablet should be taken on waking after an overnight fast, with a full glass of water (not mineral water), no less than 30 (preferably 60) minutes prior to eating or drinking. Patients should also avoid lying down for at least 30 minutes immediately after taking the tablet to avoid potential irritation of the upper gastrointestinal mucosa. Dosage adjustments are not necessary for elderly patients or patients with mild to moderate renal insufficiency.
Similar content being viewed by others
References
Fleisch H. New bisphosphonates in osteoporosis. Osteoporos Int 1993; 3 Suppl. 2: 15–22
O’Doherty DP, Bickerstaff DR, McCloskey EV, et al. Treatment of Paget’s disease of bone with aminohydroxybutylidene bisphosphonate. J Bone Miner Res 1990 May; 5: 483–91
Nussbaum SR, Warrell JRP, Rude R, et al. Dose-response study of alendronate sodium for the treatment of cancer-associated hypercalcemia. J Clin Oncol 1993 Aug; 11: 1618–23
Adami S, Bolzicco GP, Rizzo A, et al. The use of dichloromethylene bisphosphonate and aminobutane bisphosphonate in hypercalcemia of malignancy. Bone Miner 1987; 2: 395–404
Fleisch H. Bone and mineral metabolism. In: Bisphosphonates in bone disease from the laboratory to the patient. 1st ed. Berne: Stampfli & Co Ltd, 1993: 8–24
Kanis JA, Gertz BJ, Singer F, et al. Rationale for the use of alendronate in osteoporosis. Osteoporos Int 1995 Jan; 5: 1–13
Rodan GA, Seedor JG, Balena R. Preclinical pharmacology of alendronate. Osteoporos Int 1993; 3 Suppl. 3: 7–12
Fleisch H. Bisphosphonates: pharmacology and use in the treatment of tumour-induced hypercalcaemic and metastatic bone disease. Drugs 1991; 42(6): 919–44
Sato M, Grasser W, Endo N, et al. Bisphosphonate action. Alendronate localization in rat bone and effects on osteoclast ultrastructure. J Clin Invest 1991 Dec; 88: 2095–105
Zimolo Z, Wesolowski G, Rodan GA. Acid extrusion is induced by osteoclast attachment to bone: inhibition by alendronate and calcitonin. J Clin Invest 1995 Nov; 96: 2277–83
Sato M, Grasser W. Effects of bisphosphonates on isolated rat osteoclasts as examined by reflected light microscopy. J Bone Miner Res 1990 Jan; 5: 31–40
Flanagan AM, Chambers TJ. Dichloromethylenebisphosphonate (Cl2MBP) inhibits bone resorption through injury to osteoclasts that resorb Cl2MBP-coated bone. Bone Miner 1989; 6: 33–43
Thompson DD, Seedor JG, Quartuccio H, et al. The bisphosphonate, alendronate, prevents bone loss in ovariectomized baboons. J Bone Miner Res 1992 Aug; 7: 951–60
Hughes DE, Wright KR, Uy HL, et al. Bisphosphonates promote apoptosis in murine osteoclasts in vitro and in vivo. J Bone Miner Res 1995; 10(10): 1478–87
Guy JA, Shea M, Peter CP, et al. Continuous alendronate treatment throughout growth, maturation, and aging in the rat results in increases in bone mass and mechanical properties. Calcif Tissue Int 1993 Oct; 53: 283–8
Toolan BC, Shea M, Myers ER, et al. Effects of 4-amino-1-hydroxybutylidene bisphosphonate on bone biomechanics in rats. J Bone Miner Res 1992 Dec; 7: 1399–406
Thompson D, Seedor JG, Weinreb M, et al. Aminohydroxybutane bisphosphonate inhibits bone loss due to immobilization in rats. J Bone Miner Res 1990 Mar; 5: 279–86
Bikle DD, Morey-Holton ER, Doty SB, et al. Alendronate increases skeletal mass of growing rats during unloading by inhibiting resorption of calcified cartilage. J Bone Miner Res 1994 Nov; 9: 1777–87
Apseloff G, Girten B, Walker M, et al. Aminohydroxybutane bisphosphonate and clenbuterol prevent bone changes and retard muscle atrophy respectively in tail-suspended rats. J Pharmacol Exp Ther 1993 Mar; 264: 1071–8
Apseloff G, Girten B, Weisbrode SE, et al. Effects of aminohydroxybutane bisphosphonate on bone growth when administered after hind-limb bone loss in tail-suspended rats. J Pharmacol Exp Ther 1993 Oct; 267: 515–21
Garnero P, Shih WJ, Gineyts E, et al. Comparison of new biochemical markers of bone turnover in late postmenopausal osteoporotic women in response to alendronate treatment. J Clin Endocrinol Metab 1994 Dec; 79: 1693–700
Vasikaran SD, Gertz BJ, Sciberras DG, et al. Intravenous alendronate therapy in postmenopausal osteoporosis. Bone Miner 1992; 17
Harris ST, Gertz BJ, Genant HK, et al. The effect of short term treatment with alendronate on vertebral density and biochemical markers of bone remodeling in early postmenopausal women. J Clin Endocrinol Metab 1993 Jun; 76: 1399–406
Rossini M, Gatti D, Zamberlan N, et al. Long-term effects of a treatment course with oral alendronate of postmenopausal osteoporosis. J Bone Miner Res 1994 Nov; 9: 1833–7
Tucci JR, Tonino RP, Emkey RD, et al. Effect of three-years of oral alendronate treatment in postmenopausal women with osteoporosis. Am J Med 1996; 101: 488–501
Adami S, Passeri M, Ortolani S, et al. Effects of oral alendronate and intranasal salmon calcitonin on bone mass and biochemical markers of bone turnover in postmenopausal women with osteoporosis. Bone 1995; 17: 383–90
Devogelaer JP, Broil H, Correa-Rotter R, et al. Oral alendronate induces progressive increases in bone mass of the spine, hip and total body over three years in postmenopausal women with osteoporosis. Bone 1996 Feb; 18(2): 141–50
Chesnut III CH, McClung MR, Ensrud KE, et al. Alendronate treatment of the postmenopausal osteoporotic woman: effect of multiple dosages on bone mass and bone remodeling. Am J Med 1995 Aug; 99: 144–52
Gertz BJ, Holland SD, Kline WF, et al. Clinical pharmacology of alendronate sodium. Osteoporos Int 1993; 3 Suppl. 3: 13–6
Kline WF, Matuszewski BK, Bayne WF. Determination of 4-amino-1-hydroxybutane-1,1-bisphosphonic acid in urine by automated pre-column derivatization with 2,3-naphthalene dicarboxyaldehyde and high-performance liquid chromatography with fluorescence detection. J Chromatogr 1990 Dec 14; 534: 139–49
Tsai EW, Chamberlin SD, Forsyth RJ, et al. Determination of bisphosphonate drugs in pharmaceutical dosage formulations by ion chromatography with indirect UV detection. J Pharm Biomed Anal 1994 Aug; 12: 983–91
Gertz BJ, Kline WF, Matuszewski BK, et al. Oral bioavailability and dose proportionality of alendronate (aminohydroxy-butylidene bisphosphonate) in postmenopausal women. J Bone Miner Res 1991 Aug 27; 6 Suppl. 1: S281
Gertz BJ, Holland SD, Kline WF, et al. Studies of the oral bioavailability of alendronate. Clin Pharmacol Ther 1995 Sept; 58(3): 288–98 (400610)
Lin JH, Duggan DE, Chen I-W, et al. Physiological disposition of alendronate, a potent anti-osteolytic bisphosphonate, in laboratory animals. Drug Metab Dispos 1991 Sep–Oct; 19: 926–32
Lin JH, Chen I-W, deLuna FA, et al. The role calcium in plasma protein binding and renal handling of alendronate in hypo-and hypercalcemic rats [abstract]. Pharm Res 1992 Oct; 9 Suppl.: 276
Lin JH, Chen I-W, Deluna FA, et al. Renal handling of alendronate in rats. An uncharacterized renal transport system. Drug Metab Dispos 1992 Jul–Aug; 20: 608–13
Lin JH, Chen I-W, Deluna FA. Nonlinear kinetics of alendronate: plasma protein binding and bone uptake. Drug Metab Dispos 1994 May–Jun; 22: 400–5
FDA. Guidelines for preclinical and clinical evaluation of agents used in the prevention or treatment of postmenopausal osteoporosis. Draft Apr 1994.
Liberman UA, Weiss SR, Broil J, et al. Effect of oral alendronate on bone mineral density and the incidence of fractures in postmenopausal osteoporosis. N Engl J Med 1995 Nov 30; 333(33): 1437–43
Karpf DB, Shapiro D, Seeman E, et al. Prevention of nonvertebral fractures by alendronate: a meta-analysis. Merk research laboratories, Rahway, New Jersey. 1996. (Data on file).
Melton III LJ, Atkinson EJ, O’Fallon WM, et al. Long-term fracture prediction by bone mineral assessed at different skeletal sites. J Bone Miner Res 1993; 8(10): 1227–33
Ross PD, Davis JW, Epstein RS, et al. Pre-existing fractures and bone mass predict vertebral fracture incidence in women. Ann Intern Med 1991 Jun 1; 114(11): 919–23
Kanis JA. What constitutes evidence for drug efficacy in osteoporosis? Drugs Aging 1993; 3(5): 391–9
Odvina C, Wegerdal JE, Libanati CR, et al. Relationship between trabecular vertebral body density and fratures: a quantitative definition of spinal osteoporosis. Metabolism 1988 Mar; 37(3): 221–8
Ott SM, Kilcoyne RF, Chesnut III CH. Ability of four different techniques of measuring bone mass to diagnose vertebral fractures in postmenopausal women. J Bone Miner Res 1987; 2(3): 201–10
Bone HG, Downs Jr RW, Tucci JR, et al. Dose-response relationships for alendronate treatment in osteoporotic elderly women. J Clin Endocrinol Metab 1997 Jan; 82: 265–74
Seeman E, Nagant de Deuxchaisnes C, Meunier P, et al. Treatment of postmenopausal osteoporosis with oral alendronate [abstract]. Bone 1995 Jan; 16 Suppl: 120S
Stock JL, Bell NH, Chesnut III CH, et al. Resolution af alendronate effects on bone mineral density and bone turnover after multi-year treatment of osteoporotic women (abstract pTu717). Osteoporos Int 1996 May; 21 Suppl. 6: 262
Bankhurst A, McIlwain H, Emkey R, et al. Three-year treatment with alendronate prevents fractures on women with post-menopausal osteoporosis. Arthritis Rheum 1995 Sept; 38(9): S359
Eisman JA, Chistiansen C, McClung M, et al. Alendronate prevents bone loss at the spine and hip in recently postmenopausal women [abstract]. Rahway, New Jersey, USA: Merck Research Labs., Merck Sharp and Dohme, year unknown.
Passed M, Baroni MC, Pedrazzoni M, et al. Intermittent treatment with intravenous 4-amino-l-hydroxybutylidene-1,1-bisphosphonate (AHBuBP) in the therapy of postmenopausal osteoporosis. Bone Miner 1991 Dec; 15: 237–47
Sandoz Pharmaceuticals Corporation. Miacalcin (calcitoninsalmon) Nasal spray prescribing information. East Hanover, New Jersey 07936; 1995.
Minne HW, Leidig G, Wuster C, et al. A newly developed spine deformity index (SDI) to quantitate vertebral crush fractures in patients with osteoporosis. Bone Miner 1988; 3: 335–49
Black DM, Cummings SR, Karpf DB, et al. Randomised trial of the effect of alendronate on risk of fracture in women with existing vertebral fractures. Lancet 1996 Dec 7; 348: 1535–41
Merck & Co. Alendronate prescribing information. West Point, Pennsylvania, USA, Sept 1995.
De Groen PC, Lubbe DF, Hirsch LJ, et al. esophagatis associated with the use of alendronate. N Engl J Med 1996 Oct 3; 335(14): 1016–21
Dunn CJ, Fitton A, Sorkin EM. Etidronic acid: a review of its pharmacological properties and therapeutic efficacy in resorptive bone disease. Drugs Aging 1994 Dec; 5(6): 446–74
Fleisch H. Pathophysiology of Osteoporosis. Bone Miner 1993; 22: S3–s6
Randell A, Sambrook PN, Nguyen TV, et al. Direct clinical and welfare costs of all symptomatic osteoporotic fractures in elderly men and women. Bone 1995; 16(1): 120s
Eriksen EF, Colvard DS, Berg NJ, et al. Evidence of estrogen receptors in normal human osteoblast-like cells. Science 1988; 241: 84–6
WHO Study Group, editor. WHO study group on assessment of fracture risk and its application to screening for postmenopausal osteoporosis: report of a WHO study group. Geneva: World Health Organisation, 1994
Mack TM, Pike MC, Henderson BE, et al. Estrogens and endometrial cancer in a retirement community. N Engl J Med 1976 Jun 3: 1262–7
Ettinger B, Friedman GD, Bush T, et al. Reduced mortality associated with long-term postmenopausal estrogen therapy. Obstet Gynecol 1996; 87: 6–12
Clissold SP, Fitton A, Chrisp P. Intranasal salmon calcitonin: a review of its properties and potential utility in metabolic bone disorders associated with aging. Drugs Aging 1991 Sept/Oct; 1(5): 405–23
Patel S, Lyons AR, Hosking DJ. Drugs used in the treatment of metabolic bone disease. Clinical pharmacology and therapeutic use. Drugs 1993 Oct; 46: 594–617
Plosker GL, McTavish D. Intranasal salcatonin (salmon calcitonin): a review of its pharmacological properties and role in the management of postmenopausal osteoporosis. Drugs Aging 1996 May; 8(5): 378–400
Tilyard MW. 1,25-Dihydroxyvitamin D3 (Calcitrol) in the treatment of postmenopausal osteoporosis. Aktuel Rheumatol 1994; 19: 23–6
Fleisch H. Bisphosphonates — preclinical. In: Bisphosphonates in bone disease from the laboratory to the patient. 1st ed. Berne: Stampfli and Co Ltd, 1993: 26–57
O’Doherty DP, Gertz BJ, Tindale W, et al. Effects of five daily 1 h infusions of alendronate in Paget’s disease of bone. J Bone Miner Res 1992 Jan; 7: 81–7
Ostovic D, Brenner GS. Development of subcutaneous and intramuscular formulations of calcium alendronate salts. Drug Dev Ind Pharm 1995; 21(10): 1157–69
Author information
Authors and Affiliations
Corresponding author
Additional information
Various sections of the manuscript reviewed by: D.R. Abernethy, Division of Clinical Pharmacology, Georgetown University Medical Center, Washington DC, USA; S. Adami, Centro Ospedaliero Clinicizzato di Medicina Riabilitativa di Valeggio, Verona, Italy; J.P. Devogelaer, Département de Médecine Interne, Cliniques Universitaires Saint-Luc, Brussels, Belgium; S.T. Harris, Departments of Medicine and Radiology, University of California, San Francisco, California, USA; J.A. Kanis, Sheffield Metabolic Bone Unit, The University of Sheffield, Sheffield, England; M. Passeri, Istituto di Clinica Medica Generale e Terapia Medica, Università di Parma, Parma, Italy; S. Patel, Department of Rheumatology, St George’s Hospital, London, England; L.G. Raisz, Division of Endocrinology and Metabolism, The University of Connecticut Health Center, Farmington, Connecticut, USA; I.R. Reid, Faculty of Medicine and Health Science, University of Auckland, Auckland, New Zealand; M. Rossini, Centro Ospedaliero Clinicizzato di Medicina Riabilitativa di Valeggio, Verona, Italy; J.R. Tucci, Department of Medicine, Roger Williams Medical Center, Providence, Rhode Island, USA.
Rights and permissions
About this article
Cite this article
Jeal, W., Barradell, L.B. & McTavish, D. Alendronate. Drugs 53, 415–434 (1997). https://doi.org/10.2165/00003495-199753030-00006
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-199753030-00006