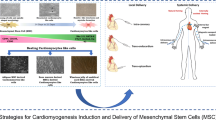
Abstract
Therapeutic angiogenesis and myogenesis restore perfusion of ischemic myocardium and improve left ventricular contractility. These therapeutic modalities must be considered as complementary rather than competing to exploit their advantages for optimal beneficial effects. The resistant nature of cardiomyocytes to gene transfection can be overcome by ex vivo delivery of therapeutic genes to the heart using genetically modified stem cells. This review article gives an overview of different vectors and delivery systems in general used for therapeutic gene delivery to the heart and provides a critical appreciation of the ex vivo gene delivery approach using genetically modified stem cells to achieve angiomyogenesis for the treatment of infarcted heart.
Similar content being viewed by others
Introduction
Myocardial infarction is the most common cause of congestive heart failure. In the U.S. alone, it affects approximately 5 million patients over the age of 65 (1). The economic cost of medical therapy (i.e., early reperfusion, ACE inhibitors, β-adrenergic blockers, and nitroglycerin) and surgical revascularization using conventional methods (i.e., angioplasty, bypass grafting, or transmyocardial laser) is enormous (2). Diastolic dysfunction after infarction episode is responsible for heart failure in more than 30% to 50% of elderly patients and results in poor prognosis (3). Heart transplantation is the gold standard therapeutic intervention but suffers from the lack of donors.
The main therapeutic targets for treatment of infarcted myocardium are to compensate for the loss of cardiomyocytes and to limit the process of left ventricle remodeling. During the last decade, various molecular- and cellular-level approaches have been adopted to address the root cause of the problem. These include heart cell therapy to achieve de novo regeneration of the infarcted myocardium and angiogenic gene therapy for restitution of regional blood flow to the ischemic myocardium. For heart cell therapy, cells from various sources with both nonmyogenic and inherent myogenic potential have been used (Table 1). Nevertheless, only skeletal myoblasts and bone marrow-derived stem cells have been used in the clinical settings owing to their ease of availability from autologous sources without ethical or religious issues and their myogenic differentiation potential (4–7). Additionally, both cell types are excellent carriers of therapeutic transgenes, a property that has been exploited to achieve concurrent angiogenesis and myogenesis for superior prognosis (8). Cell-based ex vivo gene delivery for angiogenic growth factors and cytokines is being used with encouraging results (9,10). This cell-based molecular delivery approach is being used for therapeutic angiogenesis, restenosis, bypass graft failure, myocardial repair and regeneration, and risk-factor management.
Methods to achieve gene modification of cells include gene replacement, gene correction, gene inhibition, and gene overexpression. Transplantation of genetically modified cells in the heart provide an excellent means for localized, continuous, and steady levels of therapeutic proteins at the site of the cell graft without systemic untoward effects (11). In addition, cell-based delivery to the heart provides an alternative method for gene delivery to the cardiomyocytes, which are themselves quite resistant to gene transfection. The genetically modified cells serve as a reservoir of the therapeutic proteins of interest as long as the transgene continues to overexpress itself, and the length of time of expression will be determined by the mode of gene delivery to the cells. More recently, with encouraging results from stem cell transplantation, research has been focused on using stem cells to combine their differentiation potential to adopt cardiac phenotype with their ability to serve as carriers of transgenes.
Cell-Based Gene Delivery to the Heart
Two main strategies for myocardial gene transfer are in situ or direct gene transfer and ex vivo or indirect gene transfer. The direct gene transfer method is advantageous as it is theoretically more efficient and cost-effective (despite its inefficiency and nontargeted delivery in practice so far). Indirect gene delivery involves ex vivo manipulation of stem cells for transgene insertion before engraftment (12). Although the indirect gene transfer method is more labor intensive and time consuming and has some immunological concerns due to ex vivo handling of the cells, it gives targeted transfer of the transgene into the cells of choice (13).
Many different delivery vectors have been used to transfer foreign DNA, either transiently or stably, into a target cell (Table 2). Transient transfection occurs when the transgene expression is episomal and is not incorporated into the genomic DNA of the cell. Stable transfection, in which foreign DNA is incorporated into the genomic DNA of the cell, is considered preferable only in some instances; in vivo gene transfer techniques need only have high transient transfection rates. Furthermore, with stem cells, an important consideration is that gene delivery should not interfere with the differentiation potential of the cells after gene modification.
Replication-deficient recombinant viral vectors have commonly been used for gene transfer into cells because of their high expression efficiency and ability to transfect a wide range of cell types (14–16). Although adenoviruses and retroviruses have high transfection efficiency, their clinical application is limited by possible unwanted effects such as mutagenesis, carcinogenesis, and induction of immune responses (Table 3). Thus it is necessary to develop an efficient and safe nonviral carrier for gene transfection. Although cationic lipids and their formulations help to overcome some of these problems, they have low transfection efficiency compared with viral vectors, are toxic at higher concentrations, and are unable to reach tissues beyond the vasculature (17). Moreover, the positive charge harbored by cationic lipid-based systems may also promote their nonspecific binding to cells such as erythrocytes, lymphocytes, and endothelial cells, as well as to extracellular matrix proteins (18). On the other hand, if the cells interact with serum proteins, such as lipoproteins or immunoglobulins, they may become coated, leading to an increase in their clearance rate from the blood circulation (19). Taken together, all these processes limit the ability of the complexes to reach target tissue. Alternatively, regional in vivo application such as direct injection of vectors into an organ or into the surrounding tissue may help to overcome these barriers. However, maximum effectiveness of such applications is still interrupted by factors such as extracellular matrix and immune reactions (20).
Optimization of Gene Transfer Methods
The most efficient way to improve gene delivery into cells ex vivo before engraftment involves permeabilization with or without physical techniques to cross cellular barriers. This includes electrotransfer, ultrasound-mediated delivery, osmotic shock, laser irradiation, magnetofection, and the use of divalent cationic ions (21,22). Of these strategies, electrotransfer is increasingly used to augment gene transfer into muscle over long periods of time and is as efficient as adenoviral vectors (23). Under the influence of high-voltage pulses, the negatively charged plasmid DNA accumulates around the pores transiently created in the cell membrane, followed by electrophoretic processes that help their passage across the membrane. However, electrotransfer results in local abnormalities and edema of whole muscle, together with severe muscle necrosis and significant polynuclear eosinophilic and mast cell infiltration.
A safer alternative strategy is the use of ultrasound-mediated enhancement of gene delivery into the cells through increased permeabilization of the cell membrane. This allows endosomal escape of the DNA/lipo- or polyplex complexes in the absence of toxicity (24). More recently, it was found that ultrasoundmediated microbubble destruction may enable myocardial HGF or VEGF gene transfer with systemic administration of naked plasmid (25–27). The delivery of these therapeutic genes gave enhanced angiogenesis and reduced infarction size and left ventricular remodeling after myocardial infarction. Divalent cations including Ca2+, Mn2+, Cd2+, and Zn2+ induce membrane fusion with resultant increase in the presence of polyamines (28,29). Zn2+ and Ca2+ have been found to enhance polycation-mediated gene transfer (21,30). Zn2+ induces efficient fusion of liposomes in the presence of peptides containing several histidines. By selectively binding with nitrogen atom of the imidazole group of histidyl residues, Zn2+ doubled the zeta potential of histidylated polyplexes. ZnCl2 increases the fusogenic features of histidine-rich molecules and the intracellular trafficking of polyplexes or lipoplexes (31). However, the underlying mechanism of zinc-mediated optimization of transfection efficiency remains unclear. As of now, two families of Zn2+ transporters are known: the ZIP family (Zrt, Irt-like proteins) that imports zinc (Zn2+ influx) and the ZnT family (Zn2+ transporter) that functions in sequestration of zinc internally (transporting Zn2+ in the direction opposite to that of the ZIP proteins), which controls free zinc buildup in the cells (32).
Nonviral Vectors for Gene Therapy
Naked plasmid DNA shows a low gene-transfer efficiency, which warrants the need for a carrier molecule to assist and increase transgene transfer into the cell. Transfer of transgene into the target cells or tissue is influenced by various factors, some of which are associated with the physical characteristics of the vectors itself together with multiple factors related to the biological system (Table 4). An ideal vector for gene delivery would have characteristics to ensure high efficiency transfection without cytotoxic effects (Table 5).
From among the nonviral gene transfer systems, poly- or lipoplexes are the most widely used vectors for gene transfer (Table 6). Liposomes or polymer complexes improve delivery of plasmid DNA to cytoplasm. Only a small fraction of plasmid DNA enters the nucleus, where it remains extrachromosomal and directs a transient transgene expression. On the other hand, polylysine complexes combined with plasmid DNA (pDNA/ cationic polymer complexes) offer a chemical method of gene transfer that is potentially useful for gene therapy. DNA condensation with cationic polymers reduces the size of a plasmid from several thousand base pairs into particles of 50 to 100 nm (termed polyplexes). This protects the nucleic acids from nuclease degradation and increases the uptake of pDNA by cells (33). Inside the cell, the delivered plasmid reaches to the cytosol and then to the nucleus for gene expression. However, the low amount of plasmid DNA copies delivered to the cytosol is a major limiting factor responsible for the low efficiency of polyplexes to transfect cells. Glycosylated (lactosylated) polylysines and histidylated polylysine complexes have been designed to combine with plasmid DNA and develop polymer-based gene delivery systems (34). Transfection using glycosylated polylysines requires chloroquine or fusogenic peptides, whereas transfection using histidylated polylysine requires membrane destabilization features in endocytic vesicles even in the absence of chloroquine or fusogenic peptides. Glycosyl residues bound to polylysine were used as cell recognition signals for cellular targeting via sugar receptors (membrane lectins as mannosylated and lactosylated glycoconjugates) present at the surface of cells (35). Despite the membrane destabilization features, the plasmid transfer into the cytosol upon polyplex endocytosis is still only weakly efficient.
Polycation (polyplexes) transfection of DNA complexes have been evaluated for their effectiveness, toxicity, and cell-type dependence in a variety of in vivo models. The panel of polycations includes linear and branched polyethylenimines (PEIs) of various molecular weights (70 Da to 800 kDa), poly(N-ethy-4-vinyl pyridinium bromide), polyamidoamine dendrimer (Superfect), poly(propylenimine) dendrimer (Astramol), and a conjugate of Pluronic P123 and polyethylenimine (P123-g-PEI, 2k) (Table 6). The weak base polycations promote transfection by preventing degradation of DNA by lysosomal enzymes and by enhancing the release of DNA from the endocytic vesicles. This is related to the buffering capacity of weak base polycations and has become known as the “proton sponge hypothesis” (36). The electrostatic interactions of polycations with the negatively charged phosphate groups of DNA results in DNA condensation, which is a function of the cation-to-anion ratio, i.e., the ratio of PEI nitrogen to DNA phosphate (N/P). Condensation protects the DNA from degradation by nucleases, and the compact particles can be taken up by cells via natural processes such as adsorptive endocytosis, pinocytosis, and phagocytosis. After the polyplexes have been taken up by the cell, they are released from the endosomes into the cytosol. Their transport from the cytosol into the nucleus remains a major limitation for efficient gene transfer by nonviral vectors.
The method of lipofection involving mixing cationic lipids with plasmid DNA and RNA has gained popularity for transfection of cells. During lipofection, lipids already complexed with the plasmid of interest either fuse with the plasma membrane of the cell or enter the cell via endocytosis, thereby facilitating the passage of plasmid into the target cells. Cationic liposomes are perhaps better termed “cationic amphiphiles” owing to their tendency to coat DNA with a cationic layer of lipid micelles (37,38). This is contrary to the previously held concept in which liposomes were implied to encapsulate DNA and provide protection of DNA from serum DNAse degradation. The use of liposome formulations for gene delivery generally produces high transfection efficiency with low toxicity to the target cells (39,40). In some cases, however, complexation between DNA and liposomes may enhance cytotoxicity of the cationic lipids (41). The cationic lipids encircle the anionic foreign DNA of interest to form a stable complex with a residual net positive charge, which facilitates its interaction with the negatively charged surface of the cell. During lipid-DNA complex interaction with the cell membrane, the foreign DNA gets delivered into the cells. Traversing across the cytoplasm, the DNA enters the nucleus, where it remains extrachromosomal and is transiently expressed for 7 to 10 days. The nucleocytoplasmic trafficking of exogenous DNA is influenced by the size of DNA, nuclear importation, stability of DNA, and cell-cycle status of the target cells (42). The predominant choice of lipid in liposome formulation is a cholesterol moiety, which offers rigidity to the lipid bilayer. There are two main examples of cationic lipids containing cholesterol as their lipid: DC-Chol and the more recent bis-guanidinium-tren-cholesterol (BGTC) (43).
Alternatively, cationic lipids with shorter hydrocarbon chains as their lipid component can be included. In the case of phosphonolipids, shorter hydrocarbon chains allow better transfection in vitro, whereas the longer hydrocarbon chains allow superior transfection in vivo. Similarly, circulation half-life after intravenous injection of cationic lipids shows rapid elimination from the bloodstream (44). Transfection efficiency of cells using a nonviral vector is affected by multiple factors (summarized in Table 4) related to the physiochemical characteristic of the vector formulation and biological factors related to the host. Various commercially available cationic lipid-based formulations, liposomal as well as nonliposomal (Fu-Gene6), are available for routine transfection procedures (Table 6). These formulations have been compared in terms of their size and zeta potential, in vitro transfection activity, resistance to the presence of serum, effect of lipid/ DNA charge (+/−) or volume/weight (vol/wt) ratio, protective effect against nuclease degradation, and stability under different storage conditions, incubation times, and degrees of cell confluence before transfection (21,45).
The use of Bioplex is a new approach achieved by using a peptide nucleic acid (PNA). PNAs serve as anchors for a peptide nuclear localization signal (NLS) to plasmids or oligonucleotides (46). Nucleofection technology also provides a much better rate of gene transfer without visible toxic effects (47,48). During the past decade, it has become evident that intracellular barriers compromise the transfection efficiency of nonviral vectors, whereas nuclear membrane is the major intracellular barrier for DNA entry into the nucleus (Table 4).
Delivery Strategies for Myocardial Gene Transfer in Preclinical Studies
Nonviral myocardial gene delivery remains a challenge because of the resistant nature of cardiomyocytes to transfection. Preliminary methods for myocardial gene delivery in experimental models have assessed various routes of administration. Besides local injection into the target tissue/organ, systemic administration (intravenous, intramuscular, subcutaneous, intraperitoneal, intrapleural, and intrapericardial) has been tried for optimum results. Recently, catheter-based strategies for cardiac gene delivery, including antegrade injection (AI) via coronary arteries, retrograde injection (RI) via coronary veins, and direct myocardial injection (DI) via the coronary sinus (49), have been assessed in animal models. A comparison of these approaches showed that both RI and DI were superior to the AI approach.
Ex vivo delivery of transgenes to the heart using stem cells genetically manipulated to overexpress a gene of interest has shown significant promise (50). In most preclinical studies, skeletal myoblasts and bone marrow-derived cells have been assessed for their ability to serve as carriers of exogenous genes. In addition to serving as carriers of therapeutic genes, they also undergo myogenic differentiation and participate in repair of the infracted myocardium. Cellmediated delivery of therapeutic genes has been used extensively with encouraging results (Table 7). We have shown that cell-mediated delivery is superior to direct introduction of gene delivery vector encoding for the gene of interest (13). Transplantation of human skeletal myoblasts transduced to overexpress VEGF or angiopoietin-1 resulted in enhance blood vessel density in both small and large animal heart models of myocardial infarction (51). Yau et al. used a combination of skeletal myoblasts and heart cells transfected with plasmid VEGF165 using lipid base (52). There was four- to fivefold greater expression of VEGF in the scar area at 1 week after cell transplantation. Askari et al. combined SDF-1α delivery by transplantation of cardiac fibroblasts transfected using commercially available cationic lipid formulation Fu-Gene (Roche Indianapolis USA) (53). The transfected cardiac fibroblasts stably expressed SDF-1α in the myocardium after engraftment. The more interesting aspect of the study was that they simultaneously mobilized bone marrow cells by intraperitoneal administration of filgrastim. The combined cell-mediated SDF-1α gene delivery with cytokine-induced bone marrow cell mobilization caused increased homing of the bone marrow cells into infracted myocardium. In a later study, the same group has also shown that the delivered SDF-lα provides excellent trophic support to the cardiac myocytes during infarction (54).
In a previous study, we aimed to explore the use of synthetic vectors (3 cationic lipid vectors, Lipofectamine 2000, FuGene6, and Polyethylenimine-JetPEI, with the addition of ZnCl2 for optimal transfection of hSDF-lα into skeletal myoblasts (55). We observed significantly enhanced efficiency of hSDF-lα transfection into otherwise transfection-resistant skeletal myoblasts. We observed that hSDF-1α transfection and expression was consistently increased with FuGene6 in the presence of ZnCl2. Our results depict successful and efficient nonviral vector transfection of SkM with hSDF-lα using FuGene6 in the presence of ZnCl2. The transfected cells were later engrafted into an infarcted rat heart, where they survived and underwent myogenic differentiation (Figure 1). Increased angiogenic response was also observed in the infarct and peri-infarct regions, showing that transplantation of transfected SkM in vivo is a useful procedure in indirect gene therapy after myocardial infarction.
(A) Immunostaining of rat heart tissue sections for skeletal myosin heavy chain (fas isoform) showing extensive neomyogenesis at 4 weeks after transplantaion of skeletal myoblasts overexpressing SDF-1α. (B) Control group animal heart tissue injected with basal medium without cells. The cells were transfected with human SDF-1α plasmid using FuGene6 (Roche) in the presence of 125 µM ZnCl2.
We have also investigated the feasibility of transplantation of three different types of cells (smooth muscle cells, fibroblasts, and mesothelial cells) as carriers of transgene into a rodent heart model (21,56). The cells were transfected with a reporter gene encoding for human secreted alkaline phosphatase (pDNA-SEAP) using a commercially available cationic lipid-based vector (FuGene6). The transfection conditions were optimized for maximum transfection efficiency by including ZnCl2 in the transfection complex. Intramyocardial delivery in healthy rats led to a 35-fold increase of SEAP activity, and direct injection into the scar area of the infarcted heart led to a 15-fold overexpression for up to 10 days compared with the untransfected cells.
Various strategies have been adopted to overcome the problem of low transfection efficiency of liposomal vectors. Inclusion of hemagglutinin virus of Japan (HVJ) during DNA complexation with cationic liposome gives high-efficiency transfection of cells (57). Furthermore, HVJ-liposome-DNA complex has low cell toxicity and immunogenicity, allowing repetitive transfections without compromising the survival and in vivo behavior of the transfected cells. This strategy has been extensively used in ex vivo cell-based delivery of therapeutic gene delivery to the heart (58). Using a liposome preparation of phosphatidylserine, dimethylaminoethane-carbamoyl cholesterol, and cholesterol for complexation of VEGF encoding DNA in the presence of HVJ, more than 95% transfection efficiency of skeletal myoblasts was achieved. The cells were later transplanted in an experimental rat heart model, which resulted in increased angiomyogenic response. An important feature of the HVJ-liposome-DNA complex was the use of inactivated HVJ, which minimized the general safety concerns related with viral gene therapy protocols such as viral replication, aberrant expression of viral genes, and alterations of host genomic structure.
Put together, these studies endorse a clear advantage in using nonvirally modified cells as better and safer alternatives of naked DNA delivery or virally transduced cells. In addition to their angiogenic potential, cells may be effective after ex vivo transfection with angiogenic growth factor genes or with the genes encoding for myogenic and contractile function such as SERCA2a (59), parvalbumin (60), MyoD (61,62), or S100A1 (63) (Table 8).
Clinical Studies and Ex Vivo Gene Delivery
Angiogenic gene therapy has emerged as an alternative potential therapeutic strategy in no-option heart patients to achieve biological bypass surgery. However, during most of the reported clinical studies, the approach has been adopted as an adjunct to the routinely employed revascularization procedures (64,65). Multicenter clinical studies have been performed in Europe and the U.S. for the treatment of coronary artery disease in small number of patients. Most of these studies have used vascular endothelial growth factor (VEGF) and fibroblast growth factor-2 (FGF-2) in the form of protein or gene delivered either intramyocardially during bypass surgery or by intracoronary injection (66). The advantages of local delivery of angiogenic factors are to minimize unwanted systemic effects such as hypotension, tumor growth, retinopathy, and atherosclerotic plaque development and to permit precise and targeted angiogenic response.
Genetic therapy necessarily has a lag time between gene delivery and gene expression, making it less attractive as an acute-phase therapy for cardioprotection. Nonetheless, early delivery of gene products mitigates the ongoing molecular cascade responsible for cell death that occurs over a period of several days during myocardial ischemia. The necrotic myocardium is resistant to direct gene transfer (62). Therefore, donor cells with inherent ability to express angiogenic growth factors seem a logical choice for engraftment to achieve reperfusion of the infarcted myocardium (67). Patients with perfusion defects during acute phase of infarction may be the best candidates for this strategy. However, in patients with end-stage heart failure where improvement of left ventricular contractile function together with restoration of blood flow to the ischemic myocardium are the required clinical goals, cells with myogenic potential are a logical choice. Their ex vivo genetic manipulation for angiogenic growth factor expression before engraftment will help to achieve both angiogenesis and myogenesis. Theoretically, heart cells are the most ideal contractile cells, but a major barrier for clinical application is difficulty in availability. Skeletal myoblasts and bone marrow stem cells have been extensively assessed for their ability to serve as carriers of therapeutic transgenes (8,10,54,68). Multiple clinical studies achieved successful non-viral delivery of angiogenic growth factor genes to the heart to result in myocardial angiogenesis (Table 9). However, none of these studies have been combined with cell transplantation. Future clinical studies are therefore required to test this combinatorial approach for the best outcome.
In conclusion, combined gene and cell therapy have progressed toward large animal tests, and further human applications are predicted. The future of cell and gene therapy lies in the potential combination of gene therapy with cell therapy and tissue engineering and recently developed techniques for targeting genes to the myocardium, coupled with the use of powerful noninvasive assessment.
References
Lee MS, Lill M, Makkar RR (2004). Stem cell transplantation in myocardial infarction. Rev. Cardiovasc. Med. 5:82–98.
Redfield MM, Jacobsen SJ, Burnett JC Jr, Mahoney DW, Bailey KR, Rodeheffer RJ (2003). Burden of systolic and diastolic ventricular dysfunction in the community: appreciating the scope of the heart failure epidemic. JAMA 289:194–202.
Nordlie MA, Wold LE, Simkhovich BZ, Sesti C, Kloner RA (2006). Molecular aspects of ischemic heart disease: ischemia/reperfusion-induced genetic changes and potential applications of gene and RNA interference therapy. J. Cardiovasc. Pharmacol. Ther. 11:17–30.
Dib N, et al. (2005). Feasibility and safety of autologous myoblast transplantation in patients with ischemic cardiomyopathy. Cell Transplant. 14:11–9.
Smits PC (2004). Myocardial repair with autologous skeletal myoblasts: a review of the clinical studies and problems. Minerva Cardioangiol. 52:525–35.
Stamm C, et al. (2007). Intramyocardial delivery of CD133+ bone marrow cells and coronary artery bypass grafting for chronic ischemic heart disease: safety and efficacy studies. J. Thorac. Cardiovasc. Surg. 133:717–25.
Assmus B, et al. (2006). Transcoronary transplantation of progenitor cells after myocardial infarction. N. Engl. J. Med. 355:1222–32.
Haider H, et al. (2004). Angiomyogenesis for cardiac repair using human myoblasts as carriers of human vascular endothelial growth factor. J. Mol. Med. 82:539–49.
Yau TM, Kim C, Ng D, Li G, Zhang Y, Weisel RD, Li RK (2005). Increasing transplanted cell survival with cell-based angiogenic gene therapy. Ann. Thorac. Surg. 80:1779–86.
Ye L, Haider H, Jiang S, Ling LH, Ge R, Law PK, Sim EK (2005). Reversal of myocardial injury using genetically modulated human skeletal myoblasts in a rodent cryoinjured heart model. Eur. J. Heart Fail. 7:945–52.
Yla-Herttuala S, Martin JF (2000). Cardiovascular gene therapy. Lancet 355:213–22.
Nabel EG (1995). Gene therapy for cardiovascular disease. Circulation 91:541–8.
Ye L, et al. (2007). Angiopoietin-1 for myocardial angiogenesis: a comparison between delivery strategies. Eur. J. Heart Fail. 9:458–65.
Mangi AA, Noiseux N, Kong D, He H, Rezvani M, Ingwall JS, Dzau VJ (2003). Mesenchymal stem cells modified with Akt prevent remodeling and restore performance of infarcted hearts. Nat. Med. 9:1195–201.
Wang Y, Haider HK, Ahmad N, Xu M, Ge R, Ashraf M (2006). Combining pharmacological mobilization with intramyocardial delivery of bone marrow cells over-expressing VEGF is more effective for cardiac repair. J. Mol. Cell Cardiol. 40:736–45.
Jiang S, Haider H, Idris NM, Salim A, Ashraf M (2006). Supportive interaction between cell survival signaling and angiocompetent factors enhances donor cell survival and promotes angiomyogenesis for cardiac repair. Circ. Res. 99:776–84.
Clark PR, Hersh EM (1999). Cationic lipid-mediated gene transfer: current concepts. Curr. Opin. Mol. Ther. 1:158–76.
Dash PR, Read ML, Barrett LB, Wolfert MA, Seymour LW (1999). Factors affecting blood clearance and in vivo distribution of polyelectrolyte complexes for gene delivery. Gene Ther. 6:643–50.
da Cruz MT, Simoes S, Pires PP, Nir S, de Lima MC (2001). Kinetic analysis of the initial steps involved in lipoplex-cell interactions: effect of various factors that influence transfection activity. Biochim. Biophys. Acta 1510:136–51.
Kircheis R, Wightman L, Wagner E (2001). Design and gene delivery activity of modified polyethylenimines. Adv. Drug Deliv. Rev. 53:341–58.
Elmadbouh I, et al. (2004). Optimization of in vitro vascular cell transfection with non-viral vectors for in vivo applications. J. Gene Med. 6:1112–24.
Mehier-Humbert S, Bettinger T, Yan F, Guy RH (2005). Plasma membrane poration induced by ultrasound exposure: implication for drug delivery. J. Control. Release 104:213–22.
Andre F, Mir IM (2004). DNA electrotransfer: its principles and an updated review of its therapeutic applications. Gene Ther. 11(Suppl 1):S33–42.
Lawrie A, et al. (1999). Ultrasound enhances reporter gene expression after transfection of vascular cells in vitro. Circulation 99:2617–20.
Kondo I, et al. (2004). Treatment of acute myocardial infarction by hepatocyte growth factor gene transfer: the first demonstration of myocardial transfer of a “functional” gene using ultrasonic microbubble destruction. J. Am. Coll. Cardiol. 44:644–53.
Lawrie A, Brisken AF, Francis SE, Cumberland DC, Crossman DC, Newman CM (2000). Microbubble-enhanced ultrasound for vascular gene delivery. Gene Ther. 7:2023–7.
Zhigang W, et al. (2004). Ultrasound-mediated microbubble destruction enhances VEGF gene delivery to the infarcted myocardium in rats. Clin. Imaging 28:395–8.
Ohki S, Duax J (1986). Effects of cations and polyamines on the aggregation and fusion of phosphatidylserine membranes. Biochim. Biophys. Acta 861:177–86.
Binder H, Arnold K, Ulrich AS, Zschornig O (2001). Interaction of Zn2+ with phospholipid membranes. Biophys. Chem. 90:57–74.
Haberland A, Knaus T, Zaitsev SV, Stahn R, Mistry AR, Coutelle C, Haller H (1999). Calcium ions as efficient cofactor of polycation-mediated gene transfer. Biochim. Biophys. Acta 1445:21–30.
Pichon C, Guerin B, Refregiers M, Goncalves C, Vigny P, Midoux P (2002). Zinc improves gene transfer mediated by DNA/cationic polymer complexes. J. Gene Med. 4:548–59.
Fuchs O, Babusiak M, Vyoral D, Petrak J (2003). Role of zinc in eukaryotic cells, zinc transporters and zinc-containing proteins. Sb. Lek. 104:157–70.
Felgner PL, et al. (1997). Nomenclature for synthetic gene delivery systems. Hum. Gene Ther. 8:511–2.
Goncalves C, Pichon C, Guerin B, Midoux P (2002). Intracellular processing and stability of DNA complexed with histidylated polylysine conjugates. J. Gene Med. 4:271–81.
Pichon C, Goncalves C, Midoux P (2001). Histidinerich peptides and polymers for nucleic acids delivery. Adv. Drug Deliv. Rev. 53:75–94.
Breunig M, Lungwitz U, Liebl R, Fontanari C, Klar J, Kurtz A, Blunk T, Goepferich A (2005). Gene delivery with low molecular weight linear polyethylenimines. J. Gene Med. 7:1287–98.
Simoes S, Filipe A, Faneca H, Mano M, Penacho N, Duzgunes N, de Lima MP (2005). Cationic liposomes for gene delivery. Expert Opin. Drug Deliv. 2:237–54.
Karmali PP, Chaudhuri A (2007). Cationic liposomes as non-viral carriers of gene medicines: resolved issues, open questions, and future promises. Med. Res. Rev. 27:696–722.
Maitani Y, Igarashi S, Sato M, Hattori Y (2007). Cationic liposome (DC-Chol/DOPE = 1:2) and a modified ethanol injection method to prepare liposomes, increased gene expression. Int. J. Pharm. 342:33–9.
Boktov J, Hirsch-Lerner D, Barenholz Y (2007). Characterization of the interplay between the main factors contributing to lipoplex-mediated transfection in cell cultures. J. Gene Med. 99:884–93.
Nguyen LT, Atobe K, Barichello JM, Ishida T, Kiwada H (2007). Complex formation with plasmid DNA increases the cytotoxicity of cationic liposomes. Biol. Pharm. Bull. 30:751–7.
Hebert E (2003). Improvement of exogenous DNA nuclear importation by nuclear localization signal-bearing vectors: a promising way for non-viral gene therapy? Biol. Cell. 95:59–68.
Luton D, et al. (2004). Gene transfection into fetal sheep airways in utero using guanidinium-cholesterol cationic lipids. J. Gene Med. 6:328–36.
Tranchant I, Thompson B, Nicolazzi C, Mignet N, Scherman D (2004). Physicochemical optimisation of plasmid delivery by cationic lipids. J. Gene Med. 6(Suppl 1):S24–35.
Faneca H, Simoes S, de Lima MC (2002). Evaluation of lipid-based reagents to mediate intracellular gene delivery. Biochim. Biophys. Acta 1567:23–33.
Simonson OE, Svahn MG, Tornquist E, Lundin KE, Smith CI (2005). Bioplex technology: novel synthetic gene delivery pharmaceutical based on peptides anchored to nucleic acids. Curr. Pharm. Des. 11:3671–80.
Wiehe JM, et al. (2006). Efficient transient genetic labeling of human CD34+ progenitor cells for in vivo application. Regen. Med. 1:223–34.
Jacobsen F, et al. (2006). Nucleofection: a new method for cutaneous gene transfer? J. Biomed. Biotechnol. 2006:26060.
Hoshino K, et al. (2006). Three catheter-based strategies for cardiac delivery of therapeutic gelatin microspheres. Gene Ther. 13:1320–7.
Jo J, Nagaya N, Miyahara Y, Kataoka M, Harada-Shiba M, Kangawa K, Tabata Y (2007). Transplantation of genetically engineered mesenchymal stem cells improves cardiac function in rats with myocardial infarction: benefit of a novel nonviral vector, cationized dextran. Tissue Eng. 13:313–22.
Ye L, Haider H, Jiang S, Tan RS, Ge R, Law PK, Sim EK (2007). Improved angiogenic response in pig heart following ischaemic injury using human skeletal myoblast simultaneously expressing VEGF165 and angiopoietin-1. Eur. J. Heart Fail. 9:15–22.
Yau TM, Li G, Weisel RD, Reheman A, Jia ZQ, Mickle DA, Li RK (2004). Vascular endothelial growth factor transgene expression in cell-transplanted hearts. J. Thorac. Cardiovasc. Surg. 127:1180–7.
Askari AT, et al. (2003). Effect of stromal-cell-derived factor 1 on stem-cell homing and tissue regeneration in ischaemic cardiomyopathy. Lancet 362:697–703.
Zhang M, et al. (2007). SDF-1 expression by mesenchymal stem cells results in trophic support of cardiac myocytes after myocardial infarction. FASEB J. 21:3197–207.
Elmadbouh I, Haider H, Jiang S, Idris NM, Lu G, Ashraf M (2007). Ex vivo delivered stromal cell-derived factor-1alpha promotes stem cell homing and induces angiomyogenesis in the infarcted myocardium. J. Mol. Cell Cardiol. 42:792–803.
Elmadbouh I, Chen Y, Louedec L, Silberman S, Pouzet B, Meilhac O, Michel JB. (2005). Mesothelial cell transplantation in the infarct scar induces neovascularization and improves heart function. Cardiovasc. Res. 68:307–17.
Saeki Y, Matsumoto N, Nakano Y, Mori M, Awai K, Kaneda Y (1997). Development and characterization of cationic liposomes conjugated with HVJ (Sendai virus): reciprocal effect of cationic lipid for in vitro and in vivo gene transfer. Hum. Gene Ther. 8:2133–41.
Suzuki K, Murtuza B, Smolenski RT, Sammut IA, Suzuki N, Kaneda Y, Yacoub MH (2001). Cell transplantation for the treatment of acute myocardial infarction using vascular endothelial growth factor-expressing skeletal myoblasts. Circulation 104:I207–12.
Miyamoto MI, et al. (2000). Adenoviral gene transfer of SERCA2a improves left-ventricular function in aortic-banded rats in transition to heart failure. Proc. Natl. Acad. Sci. U. S. A. 97:793–8.
Huq F, Lebeche D, Iyer V, Liao R, Hajjar RJ (2004). Gene transfer of parvalbumin improves diastolic dysfunction in senescent myocytes. Circulation 109: 2780–5.
Etzion S, et al. (2002). Cellular cardiomyoplasty of cardiac fibroblasts by adenoviral delivery of MyoD ex vivo: an unlimited source of cells for myocardial repair. Circulation 106:I125–30.
Murry CE, Kay MA, Bartosek T, Hauschka SD, Schwartz SM (1996). Muscle differentiation during repair of myocardial necrosis in rats via gene transfer with MyoD. J. Clin. Invest. 98:2209–17.
Pleger ST, et al. (2005). S100A1 gene therapy preserves in vivo cardiac function after myocardial infarction. Mol. Ther. 12:1120–9.
Sayeed-Shah U, et al. (1998). Complete reversal of ischemic wall motion abnormalities by combined use of gene therapy with transmyocardial laser revascularization. J. Thorac. Cardiovasc. Surg. 116:763–9.
Rosengart TK, et al. (1999). Angiogenesis gene therapy: phase I assessment of direct intramyocardial administration of an adenovirus vector expressing VEGF121 cDNA to individuals with clinically significant severe coronary artery disease. Circulation 100:468–74.
Losordo DW, Dimmeler S (2004). Therapeutic angiogenesis and vasculogenesis for ischemic disease: part II: cell-based therapies. Circulation 109:2692–7.
Tse HF, Lau CP (2007). Therapeutic angiogenesis with bone marrow-derived stem cells. J. Cardiovasc. Pharmacol. Ther. 12:89–97.
Matsumoto R, et al. (2005). Vascular endothelial growth factor-expressing mesenchymal stem cell transplantation for the treatment of acute myocardial infarction. Arterioscler. Thromb. Vasc. Biol. 25:1168–73.
Tang GP, Yang Z, Zhou J (2006). Poly (ethylenimine)-grafted-poly [(aspartic acid)-co-lysine], a potential non-viral vector for DNA delivery. J. Biomater. Sci. Polym. Ed. 17:461–80.
Hattan N, Warltier D, Gu W, Kolz C, Chilian WM, Weihrauch D (2004). Autologous vascular smooth muscle cell-based myocardial gene therapy to induce coronary collateral growth. Am. J. Physiol. Heart Circ. Physiol. 287:H488–93.
Ye L, et al. (2007). Transplantation of nanoparticle transfected skeletal myoblasts overexpressing vascular endothelial growth factor-165 for cardiac repair. Circulation 116:I113–20.
Laitinen M, et al. (2000). Catheter-mediated vascular endothelial growth factor gene transfer to human coronary arteries after angioplasty. Hum. Gene Ther. 11:263–70.
Hedman M, et al. (2003). Safety and feasibility of catheter-based local intracoronary vascular endothelial growth factor gene transfer in the prevention of postangioplasty and in-stent restenosis and in the treatment of chronic myocardial ischemia: phase II results of the Kuopio Angiogenesis Trial (KAT). Circulation 107:2677–83.
Kutryk MJ, et al. (2002). Local intracoronary administration of antisense oligonucleotide against c-myc for the prevention of in-stent restenosis: results of the randomized investigation by the Thoraxcenter of antisense DNA using local delivery and IVUS after coronary stenting (ITALICS) trial. J. Am. Coll. Cardiol. 39:281–7.
Symes JF, Losordo DW, Vale PR, Lathi KG, Esakof DD, Mayskiy M, Isner JM (1999). Gene therapy with vascular endothelial growth factor for inoperable coronary artery disease. Ann. Thorac. Surg. 68:830–6.
Sarkar N, et al. (2001). Effects of intramyocardial injection of phVEGF-A165 as sole therapy in patients with refractory coronary artery disease: 12-month follow-up: angiogenic gene therapy. J. Intern. Med. 250:373–81.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is published under license to BioMed Central Ltd. This is an Open Access article is distributed under the terms of the Creative Commons Attribution License ( https://creativecommons.org/licenses/by/2.0 ), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Haider, H.K., Elmadbouh, I., Jean-Baptiste, M. et al. Nonviral Vector Gene Modification of Stem Cells for Myocardial Repair. Mol Med 14, 79–86 (2008). https://doi.org/10.2119/2007-00092.Haider
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.2119/2007-00092.Haider