Abstract
Worldwide there has been a significant increase in the incidence of oropharyngeal squamous cell carcinoma (OPSCC) etiologically attributed to oncogenic human papillomavirus (HPV). Reliable and accurate identification and detection tools are important as the incidence of HPV-related cancer is on the rise. Several HPV detection methods for OPSCC have been developed and each has its own advantages and disadvantages in regard to sensitivity, specificity, and technical difficulty. This review summarizes our current knowledge of molecular methods for detecting HPV in OPSCC, including HPV DNA/RNA polymerase chain reaction (PCR), loop-mediated isothermal amplification (LAMP), p16 immunohistochemistry (IHC), and DNA/RNA in situ hybridization (ISH) assays. This summary may facilitate the selection of a suitable method for detecting HPV infection, and therefore may help in the early diagnosis of HPV-related carcinoma to reduce its mortality, incidence, and morbidity.
概要
在世界范围内,人乳头瘤病毒(HPV)的致癌性 导致口咽鳞状细胞癌(OPSCC)的发病率显著增 加。随着HPV 相关癌症发病率的上升,寻找可 靠且准确的识别和检测HPV 的工具变得非常重 要。目前,虽然在OPSCC 组织中检测HPV 的方 法已有多种,但是在灵敏度、特异性和技术难度 等方面各有优缺点。本文综述了近年来应用于 OPSCC 组织中检测HPV 的方法,包括HPV DNA/RNA 聚合酶链反应(PCR)、环介导等温扩 增(LAMP)、肿瘤蛋白16(p16)免疫组化(IHC) 和DNA/RNA 原位杂交分析(ISH),对选择合适 的HPV检测方法具有指导意义,从而有助于HPV 相关癌症的早期诊断,降低其死亡率和发病率。
Similar content being viewed by others
References
Abdullahi UF, Naim R, Wan Taib WR, et al., 2015. Loopmediated isothermal amplification (LAMP), an innovation in gene amplification: bridging the gap in molecular diagnostics; a review. Indian J Sci Technol, 8(17):1–12. https://doi.org/10.17485/ijst/2015/v8i17/55767
Abreu ALP, Souza RP, Gimenes F, et al., 2012. A review of methods for detect human Papillomavirus infection. Virol J, 9:262. https://doi.org/10.1186/1743-422X-9-262
Ahn SM, Chan JYK, Zhang Z, 2014. Saliva and plasma quantitative polymerase chain reaction-based detection and surveillance of human papillomavirus—related head and neck cancer. JAMA Otolaryngol Head Neck Surg, 140(9): 846–854. https://doi.org/10.1001/jamaoto.2014.1338
Akagi K, Li JF, Broutian TR, et al., 2014. Genome-wide analysis of HPV integration in human cancers reveals recurrent, focal genomic instability. Genome Res, 24(2): 185–199. https://doi.org/10.1101/gr.164806.113
Albano PM, Holzinger D, Salvador C, et al., 2017. Low prevalence of human papillomavirus in head and neck squamous cell carcinoma in the northwest region of the Philippines. PLoS ONE, 12(2):e0172240. https://doi.org/10.1371/journal.pone.0172240
Ang KK, Harris J, Wheeler R, et al., 2010. Human papillomavirus and survival of patients with oropharyngeal cancer. N Engl J Med, 363(1):24–35. https://doi.org/10.1056/NEJMoa0912217
Anneroth G, Batsakis J, Luna M, 1987. Review of the literature and a recommended system of malignancy grading in oral squamous cell carcinomas. Scand J Dent Res, 95(3):229–249. https://doi.org/10.1111/j.1600-0722.1987.tb01836.x
Antonsson A, Knight L, Panizza BJ, et al., 2018. HPV-16 viral load in oropharyngeal squamous cell carcinoma using digital PCR. Acta Oto-Laryngol, 138(9):843–847. https://doi.org/10.1080/00016489.2018.1461239
Arney A, Bennett KM, 2010. Molecular diagnostics of human papillomavirus. Lab Med, 41(9):523–530. https://doi.org/10.1309/lm75wgjsvmi7vvef
Babiker AY, Eltom FM, Abdalaziz MS, et al., 2013. Screening for high risk human papilloma virus (HR-HPV) subtypes, among Sudanese patients with oral lesions. Int J Clin Exp Med, 6(4):275–281.
Bhargava A, Saigal S, Chalishazar M, 2010. Histopathological grading systems in oral squamous cell carcinoma: a review. J Int Oral Health, 2(4):1–10.
Biron VL, Kostiuk M, Isaac A, et al., 2016. Detection of human papillomavirus type 16 in oropharyngeal squamous cell carcinoma using droplet digital polymerase chain reaction. Cancer, 122(10):1544–1551. https://doi.org/10.1002/cncr.29976
Bishop JA, Ma XJ, Wang HW, et al., 2012. Detection of transcriptionally active high-risk HPV in patients with head and neck squamous cell carcinoma as visualized by a novel E6/E7 mRNA in situ hybridization method. Am J Surg Pathol, 36(12):1874–1882. https://doi.org/10.1097/PAS.0b013e318265fb2b
Bishop JA, Lewis JS Jr, Rocco JW, et al., 2015. HPV-related squamous cell carcinoma of the head and neck: an update on testing in routine pathology practice. Semin Diagn Pathol, 32(5):344–351. https://doi.org/10.1053/j.semdp.2015.02.013
Bray F, Ferlay J, Soerjomataram I, et al., 2018. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin, 68(6):394–424. https://doi.org/10.3322/caac.21492
Candotto V, Lauritano D, Nardone M, et al., 2017. HPV infection in the oral cavity: epidemiology, clinical manifestations and relationship with oral cancer. Oral Implantol, 10(3):209–220. https://doi.org/10.11138/orl/2017.10.3.209
Carcopino X, Henry M, Mancini J, et al., 2012. Significance of HPV 16 and 18 viral load quantitation in women referred for colposcopy. J Med Virol, 84(2):306–313. https://doi.org/10.1002/jmv.23190
Chai RC, Lambie D, Verma M, et al., 2015. Current trends in the etiology and diagnosis of HPV-related head and neck cancers. Cancer Med, 4(4):596–607. https://doi.org/10.1002/cam4.424
Chai RC, Lim BH, Frazer I, et al., 2016. A pilot study to compare the detection of HPV-16 biomarkers in salivary oral rinses with tumour p16INK4a expression in head and neck squamous cell carcinoma patients. BMC Cancer, 16:178. https://doi.org/10.1186/s12885-016-2217-1
Chen HW, Weissenberger G, Atkins E, et al., 2015. Highly sensitive loop-mediated isothermal amplification for the detection of Leptospira. Int JBacteriol, 2015:147173. https://doi.org/10.1155/2015/147173
Coser J, da Rocha Boeira T, Fonseca ASK, et al., 2011. Human papillomavirus detection and typing using a nested-PCR-RFLP assay. Braz J Infect Dis, 15(5):467–472. https://doi.org/10.1016/S1413-8670(11)70229-X
Dang J, Feng QH, Eaton KD, et al., 2015. Detection of HPV in oral rinse samples from OPSCC and non-OPSCC patients. BMC Oral Health, 15:126. https://doi.org/10.1186/s12903-015-0111-x
Deng ZY, Hasegawa M, Kiyuna A, et al., 2013. Viral load, physical status, and E6/E7 mRNA expression of human papillomavirus in head and neck squamous cell carcinoma. Head Neck, 35(6):800–808. https://doi.org/10.1002/hed.23034
de Villiers EM, Fauquet C, Broker TR, et al., 2004. Classification of papillomaviruses. Virology, 324(1):17–27. https://doi.org/10.1016/j.virol.2004.03.033
Dhama K, Karthik K, Chakraborty S, et al., 2014. Loop-mediated isothermal amplification of DNA (LAMP): a new diagnostic tool lights the world of diagnosis of animal and human pathogens: a review. Pak J Biol Sci, 17(2):151–166. https://doi.org/10.3923/pjbs.2014.151.166
Duncan LD, Winkler M, Carlson ER, et al., 2013. p16 immunohistochemistry can be used to detect human papillomavirus in oral cavity squamous cell carcinoma. J Oral Maxillofac Surg, 71(8):1367–1375. https://doi.org/10.1016/j.joms.2013.02.019
El-Naggar AK, Chan JKC, Grandis JR, et al., 2017. WHO Classification of Head and Neck Tumours. World Health Organization Classification of Tumours. IARC Press, Lyon, France, p.136–138.
Fischer CA, Kampmann M, Zlobec I, et al., 2010. p16 expression in oropharyngeal cancer: its impact on staging and prognosis compared with the conventional clinical staging parameters. Ann Oncol, 21(10):1961–1966. https://doi.org/10.1093/annonc/mdq210
Fontaine V, Mascaux C, Weyn C, et al., 2007. Evaluation of combined general primer-mediated PCR sequencing and type-specific PCR strategies for determination of human papillomavirus genotypes in cervical cell specimens. J Clin Microbiol, 45(3):928–934. https://doi.org/10.1128/JCM.02098-06
Garibyan L, Avashia N, 2013. Research techniques made simple: polymerase chain reaction (PCR). J Invest Dermatol, 133(3): e6. https://doi.org/10.1038/jid.2013.1
Gillison ML, D’Souza G, Westra W, et al., 2008. Distinct risk factor profiles for human papillomavirus type 16-positive and human papillomavirus type 16-negative head and neck cancers. J Natl Cancer Inst, 100(6):407–420. https://doi.org/10.1093/jnci/djn025
Goot-Heah K, Kwai-Lin T, Froemming GRA, et al., 2012. Human papilloma virus 18 detection in oral squamous cell carcinoma and potentially malignant lesions using saliva samples. Asian Pac J Cancer Prev, 13(12):6109–6113. https://doi.org/10.7314/apjcp.2012.13.12.6109
Graham SV, 2010. Human papillomavirus: gene expression, regulation and prospects for novel diagnostic methods and antiviral therapies. Future Microbiol, 5(10):1493–1506. https://doi.org/10.2217/fmb.10.107
Gupta B, Johnson NW, 2014. Systematic review and meta-analysis of association of smokeless tobacco and of betel quid without tobacco with incidence of oral cancer in South Asia and the Pacific. PLoS ONE, 9(11):e113385. https://doi.org/10.1371/journal.pone.0113385
Gupta S, Gupta S, 2015. Role of human papillomavirus in oral squamous cell carcinoma and oral potentially malignant disorders: a review of the literature. Indian J Dent, 6(2): 91–98. https://doi.org/10.4103/0975-962X.155877
Hamzan NI, Fauzi FH, Taib H, et al., 2018. Simple and rapid detection of Porphyromonas gingivalis and Aggregatibacter actinomycetemcomitans by loop-mediated isothermal amplification assay. Bangladesh J Med Sci, 17(3): 402–410. https://doi.org/10.3329/bjms.v17i3.36995
Hewitt SM, Baskin DG, Frevert CW, et al., 2014. Controls for immunohistochemistry: the Histochemical Society’s standards of practice for validation of immunohistochemical assays. J Histochem Cytochem, 62(10):693–697. https://doi.org/10.1369/0022155414545224
Holzinger D, Schmitt A, Dyckhoff G, et al., 2012. Viral RNA patterns and high viral load reliably define oropharynx carcinomas with active HPV16 involvement. Cancer Res, 72(19):4993–5003. https://doi.org/10.1158/0008-5472.can-11-3934
Isaac A, Kostiuk M, Zhang H, et al., 2017. Ultrasensitive detection of oncogenic human papillomavirus in oropharyngeal tissue swabs. J Otolaryngol Head Neck Surg, 46:5. https://doi.org/10.1186/s40463-016-0177-8
Jalouli M, Jalouli J, Ibrahim SO, et al., 2015. Comparison between single PCR and nested PCR in detection of human papilloma viruses in paraffin-embedded OSCC and fresh oral mucosa. In Vivo, 29(1):65–70.
Khor GH, Froemming GRA, Zain RB, et al., 2013. DNA methylation profiling revealed promoter hypermethylation-induced silencing of p16, DDAH2 and DUSP1 in primary oral squamous cell carcinoma. Int J Med Sci, 10(12):1727–1739. https://doi.org/10.7150/ijms.6884
Kim KY, Lewis JS Jr, Chen Z, 2018. Current status of clinical testing for human papillomavirus in oropharyngeal squamous cell carcinoma. J Pathol Clin Res, 4(4):213–226. https://doi.org/10.1002/cjp2.111
Kouketsu A, Sato I, Abe S, et al., 2016. Detection of human papillomavirus infection in oral squamous cell carcinoma: a cohort study of Japanese patients. J Oral Pathol Med, 45(8):565–572. https://doi.org/10.1111/jop.12416
Lewis JS Jr, Chernock RD, Ma XJ, et al., 2012. Partial p16 staining in oropharyngeal squamous cell carcinoma: extent and pattern correlate with human papillomavirus RNA status. Mod Pathol, 25(9):1212–1220. https://doi.org/10.1038/modpathol.2012.79
Lewis JS Jr, Beadle B, Bishop JA, et al., 2018. Human papillomavirus testing in head and neck carcinomas: guideline from the College of American Pathologists. Arch Pathol Lab Med, 142(5):559–597. https://doi.org/10.5858/arpa.2017-0286-CP
Lin WJ, Jiang RS, Wu SH, et al., 2011. Smoking, alcohol, and betel quid and oral cancer: a prospective cohort study. J Oncol, 2011:525976. https://doi.org/10.1155/2011/525976
Livingstone DM, Rohatensky M, Mintchev P, et al., 2016. Loop mediated isothermal amplification (LAMP) for the detection and subtyping of human papillomaviruses (HPV) in oropharyngeal squamous cell carcinoma (OPSCC). J Clin Virol, 75:37–41. https://doi.org/10.1016/j.jcv.2016.01.002
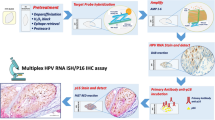
Marino FZ, Ronchi A, Stilo M, et al., 2020. Multiplex HPV RNA in situ hybridization/p16 immunohistochemistry: a novel approach to detect papillomavirus in HPV-related cancers. A novel multiplex ISH/IHC assay to detect HPV. Infect Agents Cancer, 15:46. https://doi.org/10.1186/s13027-020-00310-x
Mehanna H, Beech T, Nicholson T, et al., 2013. Prevalence of human papillomavirus in oropharyngeal and nonoropharyngeal head and neck cancer—systematic review and meta-analysis of trends by time and region. Head Neck, 35(5):747–755. https://doi.org/10.1002/hed.22015
Mellin H, Dahlgren L, Munck-Wikland E, et al., 2002. Human papillomavirus type 16 is episomal and a high viral load may be correlated to better prognosis in tonsillar cancer. Int J Cancer, 102(2):152–158. https://doi.org/10.1002/ijc.10669
Mirghani H, Moreau F, Lefèvre M, et al., 2011. Human papillomavirus type 16 oropharyngeal cancers in lymph nodes as a marker of metastases. Arch Otolaryngol Head Neck Surg, 137(9):910–914. https://doi.org/10.1001/archoto.2011.141
Mirghani H, Ferchiou F, Moreau F, et al., 2013. Oropharyngeal cancers: significance of HPV16 detection in neck lymph nodes. J Clin Virol, 57(2):120–124. https://doi.org/10.1016/j.jcv.2013.02.009
Mirghani H, Amen F, Moreau F, et al., 2014. Human papilloma virus testing in oropharyngeal squamous cell carcinoma: what the clinician should know. Oral Oncol, 50(1):1–9. https://doi.org/10.1016/j.oraloncology.2013.10.008
Mirghani H, Casiraghi O, Amen F, et al., 2015. Diagnosis of HPV-driven head and neck cancer with a single test in routine clinical practice. Mod Pathol, 28(12):1518–1527. https://doi.org/10.1038/modpathol.2015.113
Mirghani H, Casiraghi O, Guerlain J, et al., 2016. Diagnosis of HPV driven oropharyngeal cancers: comparing p16 based algorithms with the RNAscope HPV-test. Oral Oncol, 62:101–108. https://doi.org/10.1016/j.oraloncology.2016.10.009
Mori Y, Nagamine K, Tomita N, et al., 2001. Detection of loop-mediated isothermal amplification reaction by turbidity derived from magnesium pyrophosphate formation. Biochem Biophys Res Commun, 289(1):150–154. https://doi.org/10.1006/bbrc.2001.5921
Mori Y, Kitao M, Tomita N, et al., 2004. Real-time turbidimetry of LAMP reaction for quantifying template DNA. J Biochem BiophysMeth, 59(2):145–157. https://doi.org/10.1016/j.jbbm.2003.12.005
Mori Y, Kanda H, Notomi T, 2013. Loop-mediated isothermal amplification (LAMP): recent progress in research and development. J Infect Chemother, 19(3):404–411. https://doi.org/10.1007/s10156-013-0590-0
Muñoz N, Bosch FX, de Sanjosé S, et al., 2003. Epidemiologic classification of human papillomavirus types associated with cervical cancer. N Engl J Med, 348(6):518–527. https://doi.org/10.1056/NEJMoa021641
NCCN (National Comprehensive Cancer Network), 2020. Cancer of the oropharynx. Version 1.2021, Nov. 16. https://www.nccn.org/professionals/physician_gls/pdf/head-and-neck_blocks.pdf
Notomi T, Okayama H, Masubuchi H, et al., 2000. Loopmediated isothermal amplification of DNA. Nucleic Acids Res, 28(12):e63. https://doi.org/10.1093/nar/28.12.e63
Notomi T, Mori Y, Tomita N, et al., 2015. Loop-mediated isothermal amplification (LAMP): principle, features, and future prospects. J Microbiol, 53(1):1–5. https://doi.org/10.1007/s12275-015-4656-9
Oji C, Chukwuneke F, 2012. Poor oral hygiene may be the sole cause of oral cancer. J Maxillofac Oral Surg, 11(4):379–383. https://doi.org/10.1007/s12663-012-0359-5
Parida M, Sannarangaiah S, Dash PK, et al., 2008. Loop mediated isothermal amplification (LAMP): a new generation of innovative gene amplification technique; perspectives in clinical diagnosis of infectious diseases. Rev Med Virol, 18(6):407–421. https://doi.org/10.1002/rmv.593
Prigge ES, Arbyn M, von Knebel Doeberitz M, et al., 2017. Diagnostic accuracy of p16INK4a immunohistochemistry in oropharyngeal squamous cell carcinomas: a systematic review and meta-analysis. Int J Cancer, 140(5):1186–1198. https://doi.org/10.1002/ijc.30516
Qureishi A, Mawby T, Fraser L, et al., 2017. Current and future techniques for human papilloma virus (HPV) testing in oropharyngeal squamous cell carcinoma. Eur Arch Otorhinolaryngol, 274(7):2675–2683. https://doi.org/10.1007/s00405-017-4503-1
Randén-Brady R, Carpén T, Jouhi L, et al., 2019. In situ hybridization for high-risk HPV E6/E7 mRNA is a superior method for detecting transcriptionally active HPV in oropharyngeal cancer. Hum Pathol, 90:97–105. https://doi.org/10.1016/j.humpath.2019.05.006
Rietbergen MM, Snijders PJF, Beekzada D, et al., 2014. Molecular characterization of p16-immunopositive but HPV DNA-negative oropharyngeal carcinomas. Int J Cancer, 134(10):2366–2372. https://doi.org/10.1002/ijc.28580
Ritari J, Hultman J, Fingerroos R, et al., 2012. Detection of human papillomaviruses by polymerase chain reaction and ligation reaction on universal microarray. PLoS ONE, 7(3):e34211. https://doi.org/10.1371/journal.pone.0034211
Robinson M, Schache A, Sloan P, et al., 2012. HPV specific testing: a requirement for oropharyngeal squamous cell carcinoma patients. Head Neck Pathol, 6(S1):83–90. https://doi.org/10.1007/s12105-012-0370-7
Rohatensky MG, Livingstone DM, Mintchev P, et al., 2018. Assessing the performance of a loop mediated isothermal amplification (LAMP) assay for the detection and subtyping of high-risk suptypes of human papilloma virus (HPV) for oropharyngeal squamous cell carcinoma (OPSCC) without DNA purification. BMC Cancer, 18:166. https://doi.org/10.1186/s12885-018-4087-1
Rooper LM, Gandhi M, Bishop JA, et al., 2016. RNA in-situ hybridization is a practical and effective method for determining HPV status of oropharyngeal squamous cell carcinoma including discordant cases that are p16 positive by immunohistochemistry but HPV negative by DNA in-situ hybridization. Oral Oncol, 55:11–16. https://doi.org/10.1016/j.oraloncology.2016.02.008
Saetiew C, Limpaiboon T, Jearanaikoon P, et al., 2011. Rapid detection of the most common high-risk human papillomaviruses by loop-mediated isothermal amplification. J Virol Met, 178(1–2):22–30. https://doi.org/10.1016/j.jviromet.2011.08.007
Schache AG, Liloglou T, Risk JM, et al., 2011. Evaluation of human papilloma virus diagnostic testing in oropharyngeal squamous cell carcinoma: sensitivity, specificity, and prognostic discrimination. Clin Cancer Res, 17(19):6262–6271. https://doi.org/10.1158/1078-0432.CCR-11-0388
Schache AG, Liloglou T, Risk JM, et al., 2013. Validation of a novel diagnostic standard in HPV-positive oropharyngeal squamous cell carcinoma. Br J Cancer, 108(6):1332–1339. https://doi.org/10.1038/bjc.2013.63
Sigma-Aldrich, 2018. qPCR Technical Guide. https://www.gene-quantification.de/SIAL-qPCR-Technical-Guide.pdf
Singhi AD, Westra WH, 2010. Comparison of human papillomavirus in situ hybridization and p16 immunohisto-chemistry in the detection of human papillomavirus-associated head and neck cancer based on a prospective clinical experience. Cancer, 116(9):2166–2173. https://doi.org/10.1002/cncr.25033
Snijders PJ, Heideman DAM, Meijer CJLM, 2010. Methods for HPV detection in exfoliated cell and tissue specimens. APMIS, 118(6–7):520–528. https://doi.org/10.1111/j.1600-0463.2010.02621.x
Snow AN, Laudadio J, 2010. Human papillomavirus detection in head and neck squamous cell carcinomas. Adv Anat Pathol, 17(6):394–403. https://doi.org/10.1097/PAP.0b013e3181f895c1
Stevenson A, Wakeham K, Pan J, et al., 2020. Droplet digital PCR quantification suggests that higher viral load correlates with improved survival in HPV-positive oropharyngeal tumours. J Clin Virol, 129:104505. https://doi.org/10.1016/j.jcv.2020.104505
Suciu M, Morariu SH, Ormenisan A, et al., 2014. Oral squamous cell carcinoma of the maxilla, a second malignancy after a right ethmoido-maxillary chondrosarcoma. Rom J Morphol Embryol, 55(S3):1247–1251.
Suresh MJ, 2016. Detection of p16INK4a in Oropharyngeal and Upper Respiratory Tract Squamous Cell Carcinoma. Master Thesis, Chengalpattu Medical College, India. https://1library.net/document/oz1g1dvz-detection-oropharyngeal-upper-respiratory-tract-squamous-cell-carcinoma.html
Tawe L, Grover S, Narasimhamurthy M, et al., 2018. Molecular detection of human papillomavirus (HPV) in highly fragmented DNA from cervical cancer biopsies using double-nested PCR. MethodsX, 5:569–578. https://doi.org/10.1016/j.mex.2018.05.018
Veyer D, Wack M, Mandavit M, et al., 2020. HPV circulating tumoral DNA quantification by droplet-based digital PCR: a promising predictive and prognostic biomarker for HPV-associated oropharyngeal cancers. Int J Cancer, 147(4):1222–1227. https://doi.org/10.1002/ijc.32804
Volpi CC, Ciniselli CM, Gualeni AV, et al., 2018. In situ hybridization detection methods for HPV16 E6/E7 mRNA in identifying transcriptionally active HPV infection of oropharyngeal carcinoma: an updating. Hum Pathol, 74: 32–42. https://doi.org/10.1016/j.humpath.2017.09.011
Wang XY, Seo DJ, Lee MH, et al., 2014. Comparison of conventional PCR, multiplex PCR, and loop-mediated isothermal amplification assays for rapid detection of Arcobacter species. J Clin Microbiol, 52(2):557–563. https://doi.org/10.1128/JCM.02883-13
Wasserman JK, Rourke R, Purgina B, et al., 2017. HPV DNA in saliva from patients with SCC of the head and neck is specific for p16-positive oropharyngeal tumours. J Otolaryngol Head Neck Surg, 46:3. https://doi.org/10.1186/s40463-016-0179-6
Weiss D, Koopmann M, Basel T, et al., 2012. Cyclin A1 shows age-related expression in benign tonsils, HPV16-dependent overexpression in HNSCC and predicts lower recurrence rate in HNSCC independently of HPV16. BMC Cancer, 12:259. https://doi.org/10.1186/1471-2407-12-259
Yu DJ, Chen Y, Wu SH, et al., 2012. Simultaneous detection and differentiation of human papillomavirus genotypes 6, 11, 16 and 18 by AllGlo quadruplex quantitative PCR. PLoS ONE, 7(11):e48972. https://doi.org/10.1371/journal.pone.0048972
Zarei M, Moradie A, Hamkar R, et al., 2007. Detection of human papillomavirus DNA sequences in oral lesions using polymerase chain reaction. Acta Med Iran, 45(3): 177–182.
Zheng ZM, Baker CC, 2006. Papillomavirus genome structure, expression, and post-transcriptional regulation. Front Biosci, 11:2286–2302.
Zil-e-Rubab, Baig S, Zaman U, et al., 2018. Human papilloma virus 16/18: fabricator of trouble in oral squamous cell carcinoma. Int J Infect Dis, 69:115–119. https://doi.org/10.1016/j.ijid.2018.02.003
Acknowledgments
We thank Ms. Syaidatul Akmal SYAIFUDDIN from School of Dental Sciences, Universiti Sains Malaysia for her efforts in editing the figures.
Author information
Authors and Affiliations
Contributions
Fatin Hazwani FAUZI and Nural Izzati HAMZAN analyzed the literature and prepared the first draft of the manuscript. Nurhayu Ab RAHMAN and Siti SURAIYA edited and checked the final version. Suharni MOHAMAD designed, revised, edited, and checked the final version. All authors have read and approved the final manuscript and, therefore, have full access to all the data in the study and take responsibility for the integrity and security of the data.
Corresponding author
Additional information
Compliance with ethics guidelines
Fatin Hazwani FAUZI, Nurul Izzati HAMZAN, Nurhayu Ab RAHMAN, Siti SURAIYA, and Suharni MOHAMAD declare that they have no conflict of interest.
This article does not contain any studies with human or animal subjects performed by any of the authors.
Project supported by the Universiti Sains Malaysia Research University Grant (1001/PPSG/8012345)
Rights and permissions
About this article
Cite this article
Fauzi, F.H., Hamzan, N.I., Rahman, N.A. et al. Detection of human papillomavirus in oropharyngeal squamous cell carcinoma. J. Zhejiang Univ. Sci. B 21, 961–976 (2020). https://doi.org/10.1631/jzus.B2000161
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1631/jzus.B2000161