Abstract
Background
Hepatic artery infusion pump (HAIP) with floxuridine/dexamethasone and systemic chemotherapy is an established treatment regimen, which had been reported about converting 47% of patients with stage 4 colorectal liver metastasis from unresectable to resectable.1,2 To this effect, HAIP chemotherapy contributes to prolonged survival of many patients, which otherwise may not have other treatment options. Biliary sclerosis, however, is a known complication of the HAIP treatment, which occurs in approximately 5.5% of patients receiving this modality as an adjuvant therapy after hepatectomy and in 2% of patients receiving HAIP treatment for unresectable disease.3 While biliary sclerosis diffusely affects the perihilar and intrahepatic biliary tree, a dominant stricture maybe found in select cases, which gives an opportunity for a local surgical treatment after failure of endoscopic stenting/dilations. While the use of minimally invasive approach to biliary surgery is gradually increasing,4 there have been no descriptions of its application in this scenario. In this video, we demonstrate the use of minimally invasive robotic technique for biliary stricturoplasty and Roux-en-Y (RY) hepaticojejunostomy to treat persistent right hepatic duct stricture after HAIP chemotherapy.
Patient
A 68-year-old woman with history of multifocal bilobar stage 4 colorectal liver metastasis presented to our office with obstructive jaundice and recurrent cholangitis that required nine endoscopic retrograde cholangiopancreatographies (ERCPs) and a placement of internal-external percutaneous transhepatic biliary drain (PTBD) by interventional radiology within the past 2 years. Her past surgical history was consistent with laparoscopic right hemicolectomy 3 years prior, followed by a left lateral sectorectomy with placement of an HAIP for adjuvant treatment. The patient had more than ten metastatic liver lesions within the right and left lobe, ranging from 2 to 3 cm in size at the time of HAIP placement. The patient had a histologically normal background liver parenchyma before the HAIP chemotherapy treatment. The patient did not have any history of alcohol use, diabetes mellitus, metabolic syndrome, nonalcoholic steatohepatitis, or other underlying intrinsic liver disorders, which are known to contribute to the development of hepatic fibrosis.
Despite a radiologically disease-free status, the patient started to have episodes of acute cholangitis 1 year after the placement of HAIP that required multiple admissions to a local hospital. The HAIP was subsequently removed once the diagnosis of biliary sclerosis was made despite dose reductions and treatment with intrahepatic dexamethasone for almost 1 year. In addition to this finding, the known liver metastases have shown complete radiological resolution. Therefore further treatment with HAIP was deemed unnecessary, and pump removal was undertaken.
Magnetic resonance imaging showed a dominant stricture at the junction of the right anterior and right posterior sectoral hepatic duct. The location of the dominant stricture was confirmed by an ERCP and cholangioscopy. Absence of neoplasia was confirmed with multiple cholangioscopic biopsies. Multiple endoscopic and percutaneous attempts with stent placement failed to dilate the area of stricture. Postprocedural cholangiographies showed a persistent significant narrowing, which led to multiple recurrent obstructive jaundice and severe cholangitis. While the use of surgical approach is rarely needed in the treatment of biliary sclerosis, a decision was made after extensive multidisciplinary discussions to perform a robotic stricturoplasty and RY hepaticojejunostomy with preservation of the native common bile duct.
Technique
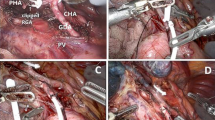
The operation began with a laparoscopic adhesiolysis to allow for identification of HAIP tubing (which was later removed) and placement of robotic ports. A peripheral liver biopsy was obtained to evaluate the degree of hepatic parenchymal fibrosis. Porta hepatic area was carefully exposed without causing an inadvertent injury to the surrounding hollow organs. Biopsy of perihepatic soft tissues was taken as appropriate to rule out any extrahepatic disease. The common bile duct and common hepatic duct with ERCP stents within it were identified with the use of ultrasonography. Anterior wall of the common hepatic duct was then opened, exposing the two plastic stents. Cephalad extension of the choledochotomy was made toward the biliary bifurcation and the right hepatic duct. The distal common bile duct was preserved for future endoscopic access to the biliary tree. After lowering the right-sided hilar plate, dense fibrosis around the right hepatic duct was divided sharply with robotic scissors, achieving a mechanical release of the dominant stricture. An intraoperative cholangioscopy was performed to confirm adequate openings of the right hepatic duct secondary and tertiary radicles, as well as patency of the left hepatic duct. A 4-Fr Fogarty catheter was used to sweep the potential biliary debris from within the right and left hepatic lobe. Finally, a confirmatory choledochoscopy was performed to ensure patency and clearance of the right-sided intrahepatic biliary ducts and the left hepatic duct before fashioning the hepaticojejunostomy.
A 40-cm antecolic roux limb was next prepared for the RY hepaticojejunostomy. A side-to-side double staple technique was utilized to create the jejunojejunostomy. The common enterotomy was closed in a running watertight fashion. Once the roux limb was transposed to the porta hepatic in a tension-free manner, a side-to-side hepaticojejunostomy was constructed in a running fashion by using absorbable barbed sutures. The index suture was placed at 9 o’clock location, and the posterior wall of the anastomosis was run toward 3 o’clock location. This stabilized the roux limb to the bile duct. The anterior wall of the anastomosis was next fashioned by using a running technique from both corners of the anastomosis toward the middle (12 o’clock), where both sutures were tied together. This completed a wide side-to-side hepaticojejunostomy anastomosis encompassing the upper common hepatic duct, biliary bifurcation, and the right hepatic duct. A closed suction drain was placed before closing.5
Results
The operative time was approximately 4 hr with 60 ml of blood loss. The postoperative course was uneventful. The patient was discharged home on postoperative Day 5 after removal of the closed suction drain, confirming the absence of bile leak. The patient had developed periportal/periductal fibrosis, cholestasis, and moderate-severe parenchymal fibrosis (F3–F4) based on liver biopsy, often seen in patients treated with a long course of floxuridine HAIP chemotherapy. The patient is clinically doing well at 1 year outpatient follow-up without any evidence of recurrent cholangitis at the time of this manuscript preparation.
Conclusions
Robotic biliary stricturoplasty with RY hepaticojejunostomy for treatment of biliary sclerosis after HAIP chemotherapy is safe and feasible. Appropriate experience in minimally invasive hepatobiliary surgery is necessary to achieve this goal.
Similar content being viewed by others
References
Kemeny N, Jarnagin W, Paty P, et al. Phase I trial of systemic oxaliplatin combination chemotherapy with hepatic arterial infusion in patients with unresectable liver metastases from colorectal cancer. J Clin Oncol. 2005;23(22):4888–96. https://doi.org/10.1200/JCO.2005.07.100.
Kemeny NE, Melendez FD, Capanu M, et al. Conversion to resectability using hepatic artery infusion plus systemic chemotherapy for the treatment of unresectable liver metastases from colorectal carcinoma. J Clin Oncol. 2009;27(21):3465–71. https://doi.org/10.1200/JCO.2008.20.1301.
Ito K, Ito H, Kemeny NE, et al. Biliary sclerosis after hepatic arterial infusion pump chemotherapy for patients with colorectal cancer liver metastasis: incidence, clinical features, and risk factors. Ann Surg Oncol. 2012;19(5):1609–17. https://doi.org/10.1245/s10434-011-2102-8.
Sucandy I, Younos A, Lim-Dy A, Lippert T. ASO Author Reflections—Robotic Klatskin type 3A resection with biliary reconstruction: can this emerging minimally invasive technique become an alternative approach to open surgery for perihilar cholangiocarcinoma? Ann Surg Oncol. 2023;30(13):8012–3. https://doi.org/10.1245/s10434-023-14298-2.
Sucandy I, Marques HP, Lippert T, et al. ASO Author Reflections—Clinical outcomes of robotic resection for perihilar cholangiocarcinoma: A first multicenter, trans-atlantic, expert-center collaborative study. Ann Surg Oncol. 2023. https://doi.org/10.1245/s10434-023-14362-x.
Acknowledgment
Alexander Rosemurgy, MD, for mentorship and consultation in treatment of hepatobiliary surgery diseases.
Funding
This research project did not receive any specific Grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Data collection and video editing: ES, IS; Manuscript writing/editing: IS, ES, SR.
Corresponding author
Ethics declarations
Disclosure
Sharona Ross is a consultant for Intuitive and Ethicon. Dr. Ross Receives educational grants for her Women In Surgery Career Symposium from Intuitive and Medtronic.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 292791 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shapera, E., Ross, S., Pattilachan, T. et al. Robotic Biliary Stricturoplasty and Roux-en-Y Hepaticojejunostomy After Hepatic Artery Infusion Pump Injury. Ann Surg Oncol (2024). https://doi.org/10.1245/s10434-024-15258-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1245/s10434-024-15258-0