Abstract
Background
This study aimed to create a prognostic model to predict disease recurrence among patients with lymph node involvement but no prostate-specific antigen (PSA) persistence and to explore its clinical utility.
Methods
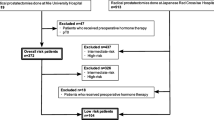
The study analyzed patients with lymph node involvement after pelvic lymph node dissection with radical prostatectomy in whom no PSA persistence was observed between 2006 and 2019 at 33 institutions. Prognostic factors for recurrence-free survival (RFS) were analyzed by the Cox proportional hazards model.
Results
Among 231 patients, 127 experienced disease recurrence. The factors prognostic for RFS were PSA level at diagnosis (≥ 20 vs. < 20 ng/mL: hazard ratio [HR], 1.66; 95% confidence interval [CI], 1.09–2.52; P = 0.017), International Society of Urological Pathology grade group at radical prostatectomy (RP) specimen (group ≥ 4 vs. ≤ 3: HR, 1.63; 95% CI 1.12–2.37; P = 0.010), pathologic T-stage (pT3b/4 vs. pT2/3a: HR, 1.70; 95% CI 1.20–2.42; P = 0.0031), and surgical margin status (positive vs. negative: HR, 1.60; 95% CI 1.13–2.28; P = 0.0086). The prognostic model using four parameters were associated with RFS and metastasis-free survival.
Conclusion
The prognostic model in combination with postoperative PSA value and number of lymph nodes is clinically useful for discussing treatment choice with patients.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Lestingi JFP, Guglielmetti GB, Trinh QD, Coelho RF, Pontes J Jr, Bastos DA, et al. Extended versus limited pelvic lymph node dissection during radical prostatectomy for intermediate- and high-risk prostate cancer: early oncological outcomes from a randomized phase 3 trial. Eur Urol. 2021;79:595–604.
Touijer KA, Sjoberg DD, Benfante N, Laudone VP, Ehdaie B, Eastham JA, et al. Limited versus extended pelvic lymph node dissection for prostate cancer: a randomized clinical trial. Eur Urol Oncol. 2021;4:532–9.
EAU guideline, Prostate cancer. Retrieved 30 Oct 2023 at https://uroweb.org/guidelines/prostate-cancer.
NCCN guidelines, Prostate cancer, version 4.2023. Retrieved 30 Oct 2023 at https://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf.
Blas L, Shiota M, Nagakawa S, Tsukahara S, Matsumoto T, Monji K, et al. Validation of models predicting lymph node involvement probability in patients with prostate cancer. Int J Urol. 2022;29:428–34.
Shiota M, Blas L, Eto M. Current status and future perspective on the management of lymph node-positive prostate cancer after radical prostatectomy. Cancers. 2022;14:2696.
Bianchi L, Nini A, Bianchi M, Gandaglia G, Fossati N, Suardi N, et al. The role of prostate-specific antigen persistence after radical prostatectomy for the prediction of clinical progression and cancer-specific mortality in node-positive prostate cancer patients. Eur Urol. 2016;69:1142–8.
Kim JK, Jeong CW, Ku JH, Kim HH, Kwak C. Prostate-specific antigen (PSA) persistence 6 weeks after radical prostatectomy and pelvic lymph node dissection as predictive factor of radiographic progression in node-positive prostate cancer patients. J Cancer. 2019;10:2237–42.
Ploussard G, Fossati N, Wiegel T, D’Amico A, Hofman MS, Gillessen S, et al. Management of persistently elevated prostate-specific antigen after radical prostatectomy: a systematic review of the literature. Eur Urol Oncol. 2021;4:150–69.
Shiota M, Takamatsu D, Kimura T, Tashiro K, Matsui Y, Tomida R, et al. Radiotherapy plus androgen-deprivation therapy for prostate-specific antigen persistence in lymph node-positive prostate cancer. Cancer Sci. 2022;113:2386–96.
Kirisawa T, Shiota M, Kimura T, Edamura K, Miyake M, Morizane S, et al. Comparison of therapeutic features and oncologic outcome in patients with pN1 prostate cancer among robot-assisted, laparoscopic, or open radical prostatectomy. Int J Clin Oncol. 2023;28:306–13.
Sobin LH, Gospodarowicz MK, Wittekind C. TNM Classification of Malignant Tumours. 7th edn. Hoboken: Wiley-Blackwell; 2009.
Epstein JI, Zelefsky MJ, Sjoberg DD, Nelson JB, Egevad L, Magi-Galluzzi C, et al. A contemporary prostate cancer grading system: a validated alternative to the Gleason score. Eur Urol. 2016;69:428–35.
Touijer KA, Mazzola CR, Sjoberg DD, Scardino PT, Eastham JA. Long-term outcomes of patients with lymph node metastasis treated with radical prostatectomy without adjuvant androgen-deprivation therapy. Eur Urol. 2014;65:20–5.
Pierorazio PM, Gorin MA, Ross AE, Feng Z, Trock BJ, Schaeffer EM, et al. Pathological and oncologic outcomes for men with positive lymph nodes at radical prostatectomy: the Johns Hopkins Hospital 30-year experience. Prostate. 2013;73:1673–80.
Abdollah F, Karnes RJ, Suardi N, Cozzarini C, Gandaglia G, Fossati N, et al. Predicting survival of patients with node-positive prostate cancer following multimodal treatment. Eur Urol. 2014;65:554–62.
Mandel P, Rosenbaum C, Pompe RS, Steuber T, Salomon G, Chun FK, et al. Long-term oncological outcomes in patients with limited nodal disease undergoing radical prostatectomy and pelvic lymph node dissection without adjuvant treatment. World J Urol. 2017;35:1833–9.
Passoni NM, Fajkovic H, Xylinas E, Kluth L, Seitz C, Robinson BD, et al. Prognosis of patients with pelvic lymph node (LN) metastasis after radical prostatectomy: value of extranodal extension and size of the largest LN metastasis. BJU Int. 2014;114:503–10.
Moschini M, Sharma V, Zattoni F, Boorjian SA, Frank I, Gettman MT, et al. Risk stratification of pN+ prostate cancer after radical prostatectomy from a large single-institutional series with long-term follow-up. J Urol. 2016;195:1773–8.
Mandel P, Kriegmair MC, Bogdan K, Boehm K, Budäus L, Graefen M, et al. Association between lymph node counts and oncological outcomes in lymph node-positive prostate cancer. Eur Urol Focus. 2017;3:248–55.
Moschini M, Sharma V, Gandaglia G, Dell’Oglio P, Fossati N, Zaffuto E, et al. Long-term utility of adjuvant hormonal and radiation therapy for patients with seminal vesicle invasion at radical prostatectomy. BJU Int. 2017;120:69–75.
Tilki D, Preisser F, Tennstedt P, Tober P, Mandel P, Schlomm T, et al. Adjuvant radiation therapy is associated with better oncological outcome compared with salvage radiation therapy in patients with pN1 prostate cancer treated with radical prostatectomy. BJU Int. 2017;119:717–23.
Abdollah F, Karnes RJ, Suardi N, Cozzarini C, Gandaglia G, Fossati N, et al. Impact of adjuvant radiotherapy on survival of patients with node-positive prostate cancer. J Clin Oncol. 2014;32:3939–47.
Marra G, Valerio M, Heidegger I, Tsaur I, Mathieu R, Ceci F, et al. Management of patients with node-positive prostate cancer at radical prostatectomy and pelvic lymph node dissection: a systematic review. Eur Urol Oncol. 2020;3:565–81.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Disclosure
Dr. Akira Yokomizo received lecture fees from Astellas, Bayer, and Janssen Pharma. The remaining authors have no conflicts of interest.
Ethics approval
The study protocol was approved by the institutional review board of each institute.
Consent to participate
All participants were provided with the opportunity to opt-out.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shiota, M., Takamatsu, D., Matsui, Y. et al. Prognostication in Lymph Node-Positive Prostate Cancer with No PSA Persistence After Radical Prostatectomy. Ann Surg Oncol (2024). https://doi.org/10.1245/s10434-024-14999-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1245/s10434-024-14999-2