Abstract
Background
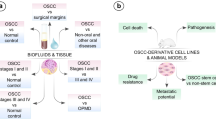
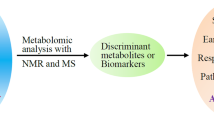
Metabolic disorders are significant in the occurrence and development of malignant tumors. Changes of specific metabolites and metabolic pathways are molecular therapeutic targets. This study aims to determine the metabolic differences between oral squamous cell carcinoma (OSCC) tissues and paired adjacent noncancerous tissues (ANT) through liquid chromatography-mass spectrometry (LC-MS). SPHK1 is a key enzyme in sphingolipid metabolism. This study also investigates the potential role of SPHK1 in OSCC.
Materials and Methods
This study used LC-MS to analyze metabolic differences between OSCC tissues and paired ANT. Principal component analysis (PCA) and partial least-squares discriminant analysis (PLS-DA) were applied to explain the significance of phospholipid metabolism pathways in the occurrence and development of OSCC. Through further experiments, we confirmed the oncogenic phenotypes of SPHK1 in vitro and in vivo, including proliferation, migration, and invasion.
Results
The sphingolipid metabolic pathway was significantly activated in OSCC, and the key enzyme SPHK1 was significantly upregulated in oral cancer tissues, predicting poor OSCC prognosis. In this study, SPHK1 overexpression was associated with high-grade malignancy and poor OSCC prognosis. SPHK1 targeted NF-κB by facilitating p65 expression to regulate OSCC tumor progression and promote metastasis.
Conclusions
This study identified metabolic differences between OSCC and paired ANT, explored the carcinogenic role of overexpressed SPHK1, and revealed the association of SPHK1 with poor OSCC prognosis. SPHK1 targets NF-κB signaling by facilitating p65 expression to regulate tumor progression and promote tumor metastasis, providing potential therapeutic targets for diagnosing and treating oral tumors.






Similar content being viewed by others
Availability of Data and Materials
All data generated or analyzed during this study are included in this published article.
References
Bloebaum M, Poort L, Böckmann R, et al. Survival after curative surgical treatment for primary oral squamous cell carcinoma. J Craniomaxillofac Surg. 2014;42(8):1572–6.
Gangopadhyay A, Bhatt S, Nandy K, et al. Survival impact of surgical resection in locally advanced T4b oral squamous cell carcinoma. Laryngoscope. 2021;131(7):E2266–74.
Flörke C, Gülses A, Altmann CR, et al. Clinicopathological risk factors for contralateral lymph node metastases in intraoral squamous cell carcinoma: a study of 331 cases. Curr Oncol. 2021;28(3):1886–98.
Panarese I, Aquino G, Ronchi A, et al. Oral and oropharyngeal squamous cell carcinoma: prognostic and predictive parameters in the etiopathogenetic route. Expert Rev Anticancer Ther. 2019;19(2):105–19.
Wolff KD, Follmann M, Nast A. The diagnosis and treatment of oral cavity cancer. Dtsch Arztebl Int. 2012;109(48):829–35.
Almangush A, Mäkitie AA, Triantafyllou A, et al. Staging and grading of oral squamous cell carcinoma: An update. Oral Oncol. 2020;107:104799.
Vitório JG, Duarte-Andrade FF, Dos Santos Fontes Pereira T, et al. Metabolic landscape of oral squamous cell carcinoma. Metabolomics. 2020;16(10):105.
Wang L, Wang X, Li Y, et al. Plasma lipid profiling and diagnostic biomarkers for oral squamous cell carcinoma. Oncotarget. 2017;8(54):92324–32.
Yonezawa K, Nishiumi S, Kitamoto-Matsuda J, et al. Serum and tissue metabolomics of head and neck. Cancer Genomics Proteomics. 2013;10(5):233–8.
Tsai CK, Lin CY, Kang CJ, et al. Nuclear magnetic resonance metabolomics biomarkers for identifying high risk patients with extranodal extension in oral squamous cell carcinoma. J Clin Med. 2020;9(4):951.
Wei J, Xie G, Zhou Z, et al. Salivary metabolite signatures of oral cancer and leukoplakia. Int J Cancer. 2011;129(9):2207–17.
Mikkonen JJ, Singh SP, Herrala M, et al. Salivary metabolomics in the diagnosis of oral cancer and periodontal diseases. J Periodontal Res. 2016;51(4):431–7.
Somashekar BS, Kamarajan P, Danciu T, et al. Magic angle spinning NMR-based metabolic profiling of head and neck squamous cell carcinoma tissues. J Proteome Res. 2011;10(11):5232–41.
Zheng X, Li W, Ren L, et al. The sphingosine kinase-1/sphingosine-1-phosphate axis in cancer: potential target for anticancer therapy. Pharmacol Ther. 2019;195:85–99.
Wollny T, Watek M, Durnas B, et al. Sphingosine-1-phosphate metabolism and its role in the development of inflammatory bowel disease. Int J Mol Sci. 2017;18(4):741.
Dai L, Wang W, Liu Y, et al. Inhibition of sphingosine kinase 2 down-regulates ERK/c-Myc pathway and reduces cell proliferation in human epithelial ovarian cancer. Ann Transl Med. 2021;9(8):645.
Song L, Xiong H, Li J, et al. Sphingosine kinase-1 enhances resistance to apoptosis through activation of PI3K/Akt/NF-kappaB pathway in human non-small cell lung cancer. Clin Cancer Res. 2011;17(7):1839–49.
Shida D, Fang X, Kordula T, et al. Cross-talk between LPA1 and epidermal growth factor receptors mediates up-regulation of sphingosine kinase 1 to promote gastric cancer cell motility and invasion. Cancer Res. 2008;68(16):6569–77.
Grbcic P, Tomljanovic I, Klobucar M, et al. Dual sphingosine kinase inhibitor SKI-II enhances sensitivity to 5-fluorouracil in hepatocellular carcinoma cells via suppression of osteopontin and FAK/IGF-1R signalling. Biochem Biophys Res Commun. 2017;487(4):782–8.
Uranbileg B, Ikeda H, Kurano M, et al. Increased mRNA levels of sphingosine kinases and s1p lyase and reduced levels of s1p were observed in hepatocellular carcinoma in association with poorer differentiation and earlier recurrence. PLoS One. 2016;11(2):e0149462.
Acharya S, Yao J, Li P, et al. Sphingosine kinase 1 signaling promotes metastasis of triple-negative breast cancer. Cancer Res. 2019;79(16):4211–26.
Bao Y, Guo Y, Zhang C, et al. Sphingosine kinase 1 and sphingosine-1-phosphate signaling in colorectal cancer. Int J Mol Sci. 2017;18(10):2109.
Shen Z, Feng X, Fang Y, et al. POTEE drives colorectal cancer development via regulating SPHK1/p65 signaling. Cell Death Dis. 2019;10(11):863.
Li S, Zheng X, Wu X, et al. Sphk1 promotes breast epithelial cell proliferation via NF-κB-p65-mediated cyclin D1 expression. Oncotarget. 2016;6(49):80579–85.
DeBerardinis RJ, Chandel NS. Fundamentals of cancer metabolism. Sci Adv. 2016;2(5):e1600200.
Xiao Q, Zhang F, Xu L, et al. High-throughput proteomics and AI for cancer biomarker discovery. Adv Drug Deliv Rev. 2021;176:113844.
Nassar AF, Wu T, Nassar SF, et al. UPLC-MS for metabolomics: a giant step forward in support of pharmaceutical research. Drug Discov Today. 2017;22(2):463–70.
Xie F, Liu T, Qian WJ, et al. Liquid chromatography-mass spectrometry-based quantitative proteomics. J Biol Chem. 2011;286(29):25443–9.
Chaleckis R, Meister I, Zhang P, Wheelock CE. Challenges, progress and promises of metabolite annotation for LC-MS-based metabolomics. Current Opin Biotechnol. 2019;55:44–50.
Duarte D, Castro B, Pereira JL, et al. Evaluation of saliva stability for NMR metabolomics: collection and handling protocols. Metabolites. 2020;10(12):515.
Faedo RR, Ushida TR, Lacchini R, et al. Sphingolipids signature in plasma and tissue as diagnostic and prognostic tools in oral squamous cell carcinoma. Biochim Biophys Acta Mol Cell Biol Lipids. 2022;1867(1):159057.
Kato K, Shimasaki M, Kato T, et al. Expression of sphingosine kinase-1 is associated with invasiveness and poor prognosis of oral squamous cell carcinoma. Anticancer Res. 2018;38(3):1361–8.
Gomez-Larrauri A, Presa N, Dominguez-Herrera A, et al. Role of bioactive sphingolipids in physiology and pathology. Essays Biochem. 2020;64(3):579–89.
Sukocheva OA, Furuya H, Friedemann M, et al. Sphingosine kinase and sphingosine-1-phosphate receptor signaling pathway in inflammatory gastrointestinal disease and cancers: a novel therapeutic target. Pharmacol Ther. 2020;207:107464.
Xu C, Zhang W, Liu S, et al. Activation of the SphK1/ERK/p-ERK pathway promotes autophagy in colon cancer cells. Oncol Lett. 2018;15(6):9719–24.
Imbert C, Montfort A, Fraisse M, et al. Resistance of melanoma to immune checkpoint inhibitors is overcome by targeting the sphingosine kinase-1. Nat Commun. 2020;11(1):437.
Hii LW, Chung FF, Mai CW, et al. Sphingosine kinase 1 regulates the survival of breast cancer stem cells and non-stem breast cancer cells by suppression of STAT1. Cells. 2020;9(4):886.
Giridharan S, Srinivasan M. Mechanisms of NF-kappaB p65 and strategies for therapeutic manipulation. J Inflamm Res. 2018;11:407–19.
Amaro-Leal Â, Shvachiy L, Pinto R, et al. Therapeutic effects of IkB kinase inhibitor during systemic inflammation. Int Immunopharmacol. 2020;84:106509.
Wang Y, Xu H, Jiao H, et al. STX2 promotes colorectal cancer metastasis through a positive feedback loop that activates the NF-kappaB pathway. Cell Death Dis. 2018;9(6):664.
Schmitz ML, Kracht M. Cyclin-dependent kinases as coregulators of inflammatory gene expression. Trends Pharmacol Sci. 2016;37(2):101–13.
Acknowledgement
The authors thank Dr. Wei Zhang and Prof. Xiao-Ling Song for their excellent pathological technical support. This research was funded by the Priority Academic Program Development of Jiangsu Higher Education Institutions: PAPD, 2018-87; Jiangsu Provincial Medical Key Talent Project: ZDRCA2016087; Southeast University-Nanjing Medical University Cooperative Research Project: 2017DN03.\
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosure
All the authors listed above declare that they have no conflicts of interest.
Ethics Approval
The study was approved by the Research Ethics Committee of Nanjing Medical University, China.
Patient Consent
Informed consent was obtained from the patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
10434_2022_12098_MOESM1_ESM.docx
Supplementary Fig. 1. (A) Statistics of SPHK1 positive areas in different clinical stages; (B, C) TUNEL staining for apoptosis analysis of cells (DOCX 17 KB)
10434_2022_12098_MOESM3_ESM.tif
Supplementary Fig. 3. (A) total and phosphorylated p65 levels in HN6 cells; (B, C) QNZ treatment significantly reduced the enhanced proliferation ability of cells caused by SPHK1 overexpressed; (D, E, F) QNZ significantly inhibited the migration and invasion in HN6 cells (TIF 10924 KB)
10434_2022_12098_MOESM4_ESM.tif
Supplementary Fig. 4. (A) Total and phosphorylated p65 levels in mouse xenograft specimens; (B–D) statistics of the invasion and migration ability of Cal 27 cells after QNZ intervention (TIF 5157 KB)
Rights and permissions
About this article
Cite this article
Hou, Cx., Mao, Gy., Sun, Qw. et al. Metabolomic Analysis Reveals that SPHK1 Promotes Oral Squamous Cell Carcinoma Progression through NF-κB Activation. Ann Surg Oncol 29, 7386–7399 (2022). https://doi.org/10.1245/s10434-022-12098-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-12098-8