Abstract
Preservation of ovarian function is important for the physical and psychosexual well-being of young patients with cancer. Patients with pelvic malignancies such as cervical or rectal cancer planned for radiotherapy may benefit from ovarian transposition with the aim of moving the ovaries outside the radiation field.1 Different surgical techniques have been reported previously.2,3 With the present video, we aim to standardize the surgical technique of laparoscopic ovarian transposition in ten steps. We present the case of a 30-year-old nulliparous woman diagnosed with grade 3 squamous cell cervical carcinoma having a largest tumor diameter of 41 mm on magnetic resonance imaging (MRI) scan. The tumor was staged as FIGO 2018 stage IIIC1r with a common iliac lymphadenopathy reported on both MRI and positron emission tomography (PET)/computed tomography (CT) scan. The multidisciplinary team recommended exclusive chemoradiation extended to paraaortic area. The patient underwent laparoscopic bilateral salpingectomy and bilateral ovarian transposition with extraperitonealization of the infundibulopelvic ligament. The procedure was divided into the following ten steps: division of uteroovarian ligament, incision of lateral pelvic peritoneum, identification of ureter, incision of medial pelvic peritoneum, skeletonization of the infundibulopelvic ligament, retroperitoneal tunnel in paracolic gutter, creating the window (as high as possible), mobilization of the ovary without torsion, intraperitonealization of the ovary, and fix ovary with clips (Fig. 1). Surgical time was 30 min, with minimal estimated blood loss. No intra- or postoperative complication was recorded. The patient started radiotherapy 14 days after the procedure. In conclusion, we showed that laparoscopic ovarian transposition in cervical cancer before radiotherapy can be standardized in ten steps with encouraging perioperative results, making it an easily reproducible procedure. Ovarian function is reported to be preserved in 62–65% of cases undergoing ovarian transposition and radiation therapy.4,5

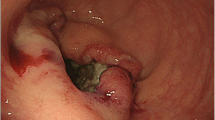
Laparoscopic view of right ovary transposed below the liver edge after extraperitonealization of the infudibulopelvic ligament
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Laios A, Duarte Portela S, Papadopoulou A, Gallos ID, Otify M, Ind T. Ovarian transposition and cervical cancer. Best Pract Res Clin Obstet Gynaecol. 2021;75:37–53. https://doi.org/10.1016/j.bpobgyn.2021.01.013.
Arian SE, Goodman L, Flyckt RL, Falcone T. Ovarian transposition: a surgical option for fertility preservation. Fertil Steril. 2017;107(4):e15. https://doi.org/10.1016/j.fertnstert.2017.01.010.
Marchocki Z, May T. High laparoscopic bilateral ovarian transposition to the upper abdomen prior to pelvic radiotherapy. Int J Gynecol Cancer. 2021;31(10):1384–5. https://doi.org/10.1136/ijgc-2021-002752.
Gubbala K, Laios A, Gallos I, Pathiraja P, Haldar K, Ind T. Outcomes of ovarian transposition in gynaecological cancers; a systematic review and meta-analysis. J Ovarian Res. 2014;7(69):2014. https://doi.org/10.1186/1757-2215-7-69.
Buonomo B, Multinu F, Casarin J, et al. Ovarian transposition in patients with cervical cancer prior to pelvic radiotherapy: a systematic review. Int J Gynecol Cancer. 2021;31(3):360–70. https://doi.org/10.1136/ijgc-2020-001774.
Acknowledgments
The authors thank the surgical team and scrub nurses at Policlinico Gemelli IRCCS, Rome, Italy.
Funding
Open access funding provided by Università Cattolica del Sacro Cuore within the CRUI-CARE Agreement.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Denis Querleu: consultant, Mimark Inc., Barcelona, Spain, since October 2021 and consultant, Arquers Diagnostics, Oxford, England, until October 2021, both related to diagnosis of endometrial cancer, outside the submitted work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: Missing Open Access funding information has been added in the Funding Note.
Supplementary Information
Below is the link to the electronic supplementary material.
Laparoscopic ovarian transposition with extraperitonealization of the infundibulopelvic ligament for cervical cancer in ten steps (MP4 265569 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s)␣and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bizzarri, N., Loverro, M., Angeles, M.A. et al. Laparoscopic Ovarian Transposition with Extraperitonealization of the Infundibulopelvic Ligament for Cervical Cancer in Ten Steps. Ann Surg Oncol 29, 5906–5907 (2022). https://doi.org/10.1245/s10434-022-11870-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-11870-0