Abstract
Background
The proportion of patients eligible for breast-conservation therapy (BCT) yet opting for mastectomy is increasing. This decision is often driven by the desire to eliminate future screening and/or biopsy of the remaining breast or breasts. This study investigated the incidence of post-mastectomy imaging and biopsy.
Methods
A retrospective review of all unilateral mastectomy (UM) and bilateral mastectomy (BM) cases managed at a single institution was undertaken. Post-mastectomy imaging and biopsy rates were determined.
Results
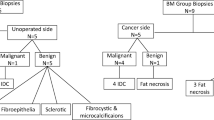
Between 2009 and 2015, 185 UM and 200 BM cases managed for breast cancer were identified. The mean follow-up period was 30 months (range 3–75 months). For the patients with UM, imaging studies and biopsies done on the contralateral side were excluded given the standard of care for continued surveillance of the contralateral breast. Of the 185 UM patients, 19 (10%) underwent ipsilateral imaging (all ultrasounds) for physical examination findings, 11 (6%) underwent biopsy, and 2 (1%) had malignant findings. Of the 200 BM patients, 31 (15.5%) required imaging (29 ultrasounds and 2 MRIs), with 76% of the ultrasounds performed on the side with previous cancer. Subsequently, 16 (8%) of the BM patients had biopsy, with 11 (69%) of the 16 biopsies performed on the ipsilateral side. Three (1.5%) of the biopsies done on ipsilateral side demonstrated malignancy, whereas all the contralateral biopsies were benign.
Conclusions
For 10–15.5% of patients who undergo mastectomy, either UM or BM, subsequent imaging is required, whereas 6–8% undergo biopsy. The yield of malignancy is low, approximately 1%. Thus, after mastectomy, the need for imaging and biopsy is not eliminated. This information is critical for patient understanding and expectation related to surgical decision making.
Similar content being viewed by others
References
Fisher B, Bauer M, Margolese R, et al. Five-year results of a randomized clinical trial comparing total mastectomy and segmental mastectomy with or without radiation in the treatment of breast cancer. N Engl J Med. 1985;312:665–73.
Fisher B, Anderson S, Bryant J, et al. Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N Engl J Med. 2002;347:1233–41.
van Dongen JA, Voogd AC, Fentiman IS, et al. Long-term results of a randomized trial comparing breast-conserving therapy with mastectomy: European Organization for Research and Treatment of Cancer 10801 trial. J Natl Cancer Inst 2000;92:1143–50.
NIH Consensus Conference. Treatment of early-stage breast cancer. JAMA 1991;265:391–5.
Dragun AE, Huang B, Tucker TC, et al. Increasing mastectomy rates among all age groups for early-stage breast cancer: a 10-year study of surgical choice. Breast J. 2012;18:318–25.
Kummerow KL, Du L, Penson DF, et al. Nationwide trends in mastectomy for early-stage breast cancer. JAMA Surg. 2015;10:9–16.
Valachis A, Nearchou AD, Lind P. Surgical management of breast cancer in BRCA-mutation carriers: a systematic review and meta-analysis. Breast Cancer Res Treat. 2014;144:443–55.
Molina-Montes E, Perez-Nevot B, Pollan M, et al. Cumulative risk of second primary contralateral breast cancer in BRCA1/BRCA2 mutation carriers with a first breast cancer: a systematic review and meta-analysis. Breast 2014;23:721–42.
Brennan MG, Houssami N, Lord S, et al. Magnetic resonance imaging screening of the contralateral breast in women with newly diagnosed breast cancer: systematic review and meta-analysis of incremental cancer detection and impact on surgical management. J Clin Oncol. 2009;27:5640–9.
Bilimoria KY, Cambic A, Hansen NM, et al. Evaluating the impact of preoperative breast magnetic resonance imaging on the surgical management of newly diagnosed breast cancers. Arch Surg. 2007;142:441–7.
Buchanan PJ, Abdulghani M, Waljee JF, et al. An analysis of the decisions made for contralateral prophylactic mastectomy and breast reconstruction. Plast Reconstr Surg. 2016;138:29–40.
Bellavance EC, Kesmodel SB. Decision-making in the surgical treatment of breast cancer: factors influencing women’s choices for mastectomy and breast conserving surgery. Front Oncol. 2016;6:1–7.
Steffens RF, Wright HR, Hester MY, et al. Clinical, demographic, and situational factors linked to distress associated with benign breast biopsy. J Psychosoc Oncol. 2011;29:35–50.
Virnig BA, Tuttle TM, Shamliyan T, et al. Ductal carcinoma in situ of the breast: a systematic review of incidence, treatment, and outcomes. J Natl Cancer Inst. 2010;102:170–8.
Iqbal J, Ginsburg O, Rochon PA, et al. Differences in breast cancer stage at diagnosis and cancer-specific survival by race and ethnicity in the united states. JAMA. 2015;313:165–73.
Mamounas EP. NSABP breast cancer clinical trials: recent results and future directions. Clin Med Res. 2003;1:309–26.
Adkisson CD, Bagaria SP, Parker AS, et al. Which eligible breast conservation patients choose mastectomy in the setting of newly diagnosed breast cancer? Ann Surg Oncol. 2012;19:1129–36.
Lautner M, Lin H, Shen Y, et al. Disparities in the use of breast-conserving therapy among patients with early-stage breast cancer. JAMA Surg. 2015;150:778–86.
Goyal S, Chandwani S, Haffty BG, et al. Effect of travel distance and time to radiotherapy on likelihood of receiving mastectomy. Ann Surg Oncol. 2015;22:1095–101.
Schroen AT, Brenin DR, Kelly MD, et al. Impact of patient distance to radiation therapy on mastectomy use in early-stage breast cancer patients. J Clin Oncol. 2005;23:7074–80.
Brett J, Bankhead C, Henderson B, et al. The psychological impact of mammographic screening: a systematic review. Psycho-oncology 2005;14:917–38.
Maxwell JR, Bugbee ME, Wellisch D, et al. Imaging-guided core needle biopsy of the breast: study of psychological outcomes. Breast J. 2000;6:53–61.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ahn, S., Elnekaveh, B., Schmidt, H. et al. Defining the Need for Imaging and Biopsy After Mastectomy. Ann Surg Oncol 25, 3843–3848 (2018). https://doi.org/10.1245/s10434-018-6735-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-018-6735-8