Abstract
Introduction
Breast-conserving therapy (BCT) using oncoplastic surgery (OPS) allows for larger resections and improved aesthetics though volume redistribution and tissue rearrangement. Data regarding the impact of OPS on surveillance imaging and need for additional biopsies are limited.
Methods
This observational cohort underwent BCT at a single institution from 2009 to 2018; standard breast-conserving surgery (BCS) was the predominant approach until OPS was introduced in 2012. Rates of imaging beyond standard diagnostic views, as well as rates of biopsy following both approaches, are reported.
Results
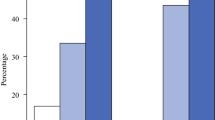
A total of 422 consecutive patients were identified. The OPS group comprised 205 patients and the BCS group included 217 patients. There was no difference in need for additional imaging between groups (BCS: 58 patients [26.7%] vs. OPS: 53 patients [25.9%]; p = 0.91). When additional imaging was required, it was on the ipsilateral side in 35 (60.3%) BCS patients compared with 24 (45.3%) OPS patients (p = 0.21). The need for biopsy was higher in the BCS group (BCS: 41 patients [18.9%] with 47 total biopsies vs. OPS: 20 patients [9.3%] with 22 total biopsies; p < 0.01). Benign findings on biopsy were similar between groups (BCS: 18 [38.3%] vs. OPS: 11 [50.0%]; p = 0.66).
Conclusions
OPS was not associated with an increased need for additional imaging compared with BCS. Concern regarding challenges with follow-up imaging should not impact the decision to offer OPS. Further study and longer-term follow-up is warranted to understand the trends in need for additional imaging, biopsy, and additional procedures following OPS.



Similar content being viewed by others
References
Chatterjee A, Gass J, Patel K, et al. A consensus definition and classification system of oncoplastic surgery developed by the American Society of Breast Surgeons. Ann Surg Oncol. 2019;26(11):3436–44.
Campbell EJ, Romics L. Oncological safety and cosmetic outcomes in oncoplastic breast conservation surgery, a review of the best level of evidence literature. Breast Cancer. 2017;9:521–30.
Crown A, Handy N, Rocha FG, Grumley JW. Oncoplastic reduction mammaplasty, an effective and safe method of breast conservation. Am J Surg. 2018;215(5):910–15.
Crown A, Laskin R, Rocha FG, Grumley J. Extreme oncoplasty: expanding indications for breast conservation. Am J Surg. 2019;217(5):851–6.
Crown A, Wechter DG, Grumley JW. Oncoplastic breast-conserving surgery reduces mastectomy and postoperative re-excision rates. Ann Surg Oncol. 2015;22(10):3363–8.
De La Cruz L, Blankenship SA, Chatterjee A, et al. Outcomes After Oncoplastic Breast-Conserving Surgery in Breast Cancer Patients: A Systematic Literature Review. Ann Surg Oncol. 2016;23(10):3247–58.
Santos G, Urban C, Edelweiss MI, et al. Long-term comparison of aesthetical outcomes after oncoplastic surgery and lumpectomy in breast cancer patients. Ann Surg Oncol. 2015;22(8):2500–508.
Yiannakopoulou EC, Mathelin C. Oncoplastic breast conserving surgery and oncological outcome: systematic review. Eur J Surg Oncol. 2016;42(5):625–30.
Crown A, Scovel LG, Rocha FG, Scott EJ, Wechter DG, Grumley JW. Oncoplastic breast conserving surgery is associated with a lower rate of surgical site complications compared to standard breast conserving surgery. Am J Surg. 2019;217(1):138–41.
Silverstein MJ, Savalia N, Khan S, Ryan J. Extreme oncoplasty: breast conservation for patients who need mastectomy. Breast J. 2015;21(1):52–9.
Henry NL, Hayes DF, Ramsey SD, Hortobagyi GN, Barlow WE, Gralow JR. Promoting quality and evidence-based care in early-stage breast cancer follow-up. J Natl Cancer Inst. 2014;106(4):dju034.
National Comprehenisve Cancer Network. Breast Cancer (Version 3.2019). Available at: https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf. Accessed 18 Feb 2020.
Khatcheressian JL, Hurley P, Bantug E, et al. Breast cancer follow-up and management after primary treatment: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol. 2013;31(7):961–5.
Margenthaler JA, Allam E, Chen L, et al. Surveillance of patients with breast cancer after curative-intent primary treatment: current practice patterns. J Oncol Pract. 2012;8(2):79–83.
American College of Radiology. ACR Appropriateness Criteria Breast Cancer Screening. Available at: https://acsearch.acr.org/docs/70910/Narrative/. Accessed 18 Feb 2020.
Dolan R, Patel M, Weiler-Mithoff E, et al. Imaging results following oncoplastic and standard breast conserving surgery. Breast Care (Basel). 2015;10(5):325–9.
Losken A, Schaefer TG, Newell M, Styblo TM. The impact of partial breast reconstruction using reduction techniques on postoperative cancer surveillance. Plast Reconstr Surg. 2009;124(1):9–17.
Muir TM, Tresham J, Fritschi L, Wylie E. Screening for breast cancer post reduction mammoplasty. Clin Radiol. 2010;65(3):198–205.
Roberts JM, Clark CJ, Campbell MJ, Paige KT. Incidence of abnormal mammograms after reduction mammoplasty: implications for oncoplastic closure. Am J Surg. 2011;201(5):611–4.
Clough KB, van la Parra RFD, Thygesen HH, et al. Long-term results after oncoplastic surgery for breast cancer: a 10-year follow-up. Ann Surg. 2018;268(1):165–71.
Jonczyk MM, Jean J, Graham R, Chatterjee A. Surgical trends in breast cancer: a rise in novel operative treatment options over a 12 year analysis. Breast Cancer Res Treat. 2019;173(2):267–74.
Silverstein MJ. Oncoplastic breast surgery: from oblivion to mainstream. Ann Surg Oncol. 2019;26(11):3409–12.
Barron M, Kuckelman J, Davison J, Mosier A, Sohn V. The role of early post-treatment mammography after breast conservation therapy. Am J Surg. 2016;211(5):850–3.
Hasan S, Abel S, Simpson-Camp L, et al. Short-term follow-up mammography in breast conservation therapy likely leads to unnecessary downstream workup: a longitudinal study. Int J Radiat Oncol Biol Phys. 2018;102(5):1489–95.
Neal CH, Yilmaz ZN, Noroozian M, et al. Imaging of breast cancer-related changes after surgical therapy. AJR Am J Roentgenol. 2014;202(2):262–72.
Miller CL, Feig SA, Fox JW. Mammographic changes after reduction mammoplasty. AJR Am J Roentgenol. 1987;149(1):35–8.
Moran MS, Schnitt SJ, Giuliano AE, et al. Society of Surgical Oncology-American Society for Radiation Oncology consensus guideline on margins for breast-conserving surgery with whole-breast irradiation in stages I and II invasive breast cancer. J Clin Oncol. 2014;32(14):1507–15.
Morrow M, Van Zee KJ, Solin LJ, et al. Society of Surgical Oncology-American Society for Radiation Oncology-American Society of Clinical Oncology Consensus Guideline on margins for breast-conserving surgery with whole-breast irradiation in ductal carcinoma in situ. J Clin Oncol. 2016;34(33):4040–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Angelena Crown, Ruby Laskin, Christina Weed, Flavio G. Rocha, and Janie Grumley declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Crown, A., Laskin, R., Weed, C. et al. Evaluating Need for Additional Imaging and Biopsy After Oncoplastic Breast-Conserving Surgery. Ann Surg Oncol 27, 3650–3656 (2020). https://doi.org/10.1245/s10434-020-08500-y
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-020-08500-y